Implant surgery and surgical guides: How hard can it be?
Surgical guides help, but training is key to implant success.
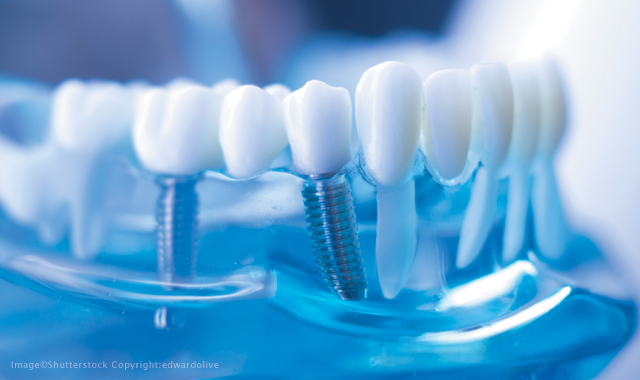
When I was in dental school 20 years ago, dental implants were a bit “taboo,” if you will. They weren’t the most sought-after procedure, but they were being placed in our periodontal and oral surgery clinics from time to time. In fact, implant dentistry got its start here in the United States when implant courses were available to surgeons only - they weren’t even offered to general practitioners. Today, there are implant courses for all levels of practitioners and these vary from courses that are a few days long to ones that last a year or more.
Years ago when implants were being placed, a “surgical” guide or template was fabricated to help “guide” the placement of the implant/implants. This was used to place radiographic markers such as lead foil and metal marking balls, and then a panoramic 2D X-ray was taken, or, if you were really high-tech or had it available, you could get a tomogram done to look at the bone in a new dimension.
This was then taken to the patient’s mouth where we would anesthetize the patient, make a nice incision and expose the bony ridge, hoping to find enough bone where we were going to place the implant. We’d use the “guide” for the initial osteotomy, and then overlay the surgical guide over guide pins to help “verify” the placement of the implant.
My journey in implant dentistry started right after school by working with surgeons who were placing them on a regular basis, and then I simply restored the patient. After a few years, I took the plunge and completed a nine-month-long surgical implant course. Over the years, I went from placing implants with panoramic X-rays like I described earlier to now having a CBCT in my office with guided implant software and having milled guides made where I place the implants without a flap.
Trending article: IoMT and the future of dentistry
If we look at how implant placement and surgeries have evolved over the past 20 years, the advent of technologies such as CBCT 3D scans and the ability to mill or print surgical guides have revolutionized and streamlined the process. So much so that everything from placing the implant virtually in the bone to the final restoration design can be completely “worked” out before we even do the surgery and with “safe” guides that help overpreparing implant sites. I mean, how hard can it be to place an implant? After placing implants as a GP for more than 10 years, it’s like the old saying goes, “It depends.”

So, what have I learned over the years of placing implants as a GP? Here are some words of wisdom that I’ve gained if you want to surgically place implants:
Proper education is key, like everything else we do in dentistry. Like the old saying goes, “You only know what you know, and you only see what you know.” In my opinion, a quick two-day course can’t help you “know” everything you need to “see” in implant surgery. So, find a respected course that allows you ample time to learn the principles of proper implant placement.
As Clint Eastwood wisely said once, “A man has to know his limitations.” The same is true in all of dentistry whether it’s root canals or implants. In order to know your limitations, you have to “know” and “see” things at a level to be able to do this.
Surgical principles don’t change whether it’s a guided surgery or not. In other words, you have to be comfortable with doing the surgery, know the ins and outs of anatomy, bone and tissue support that’s required, and all of the steps involved. You also have to be able to manage the potential complications that arise during and after the surgery. If not, then you should reconsider doing the surgery or get training to help you be more competent and comfortable.
3D scans and proper presurgical treatment planning are standard of care, period. Surgical guides aren’t “foolproof!” Remember, even if you have a lab or company fabricate the guide, ultimately, you’re responsible for the end result.
Start out simple and find a specialist who you can refer more difficult cases to and work alongside him or her. It’s amazing to me how many general dentists will send out difficult cases to their specialists, but they will not approach the same specialist for help and guidance, fearing that he or she will be chastised for doing the surgery.
I’ve found most, if not all, specialists who I’ve worked with are more than happy to help you when it comes to the surgical aspect of things. This relationship that’s built upon discussing challenges and difficulties among general dentists and specialists leads to a better understanding and growth between both parties and, ultimately, leads to better patient care.
