Closer Look: Let Your Patients Try Before They Buy
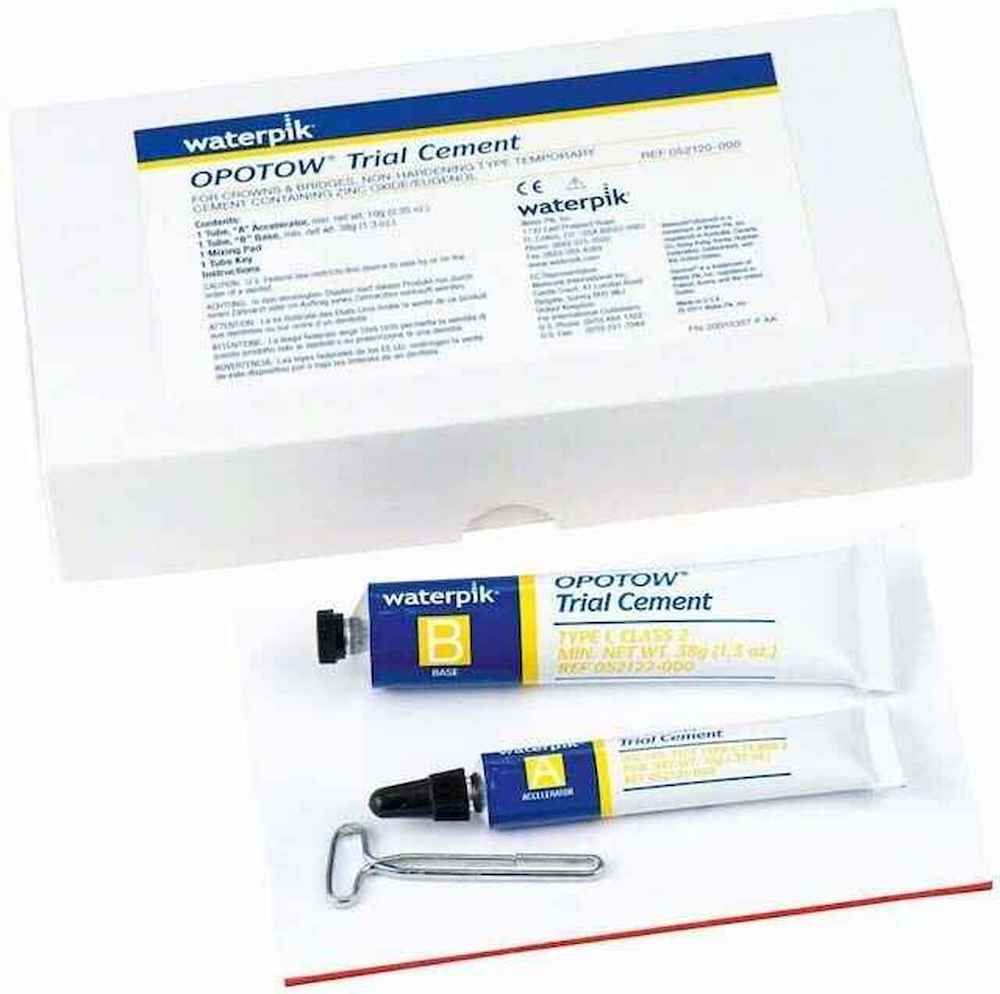
Why one clinician uses Opotow Trial Cement from Waterpik to let every crown and bridge patient test the restoration’s fit before permanent placement.
The adage “Try before you buy” is very applicable to dentistry, especially with crown and bridge restorations. I find that after insertion of a crown or fixed bridge with Waterpik Opotow Trial Cement, 100% of my patients report their restorations seat, and are more comfortable after a few days or a week.
The occlusion, which at first may seem high, settles in and is self-adjusted. Tight crowns fit comfortably with good contact points after a few days with the restoration. However, I find these outcomes only when using Opotow Trial Cement, a nonsetting adhesive with a rubbery consistency.
Inserting a fixed prosthesis with rubbery trial cement gives patients an opportunity to be certain they are comfortable and satisfied with the prosthesis before final cementation. In doing this you give the patient an opportunity to complain about any aspect of the restoration. Once they return for final cementation, and say they are happy, you have fulfilled your obligation to allow the patient to try the prosthesis before final cementation.
Often a crown does not fully seat when first inserted, and the dentist reduces the occlusal. This is wrong unless you gave the lab an inaccurate bite. It’s better to take a new bite and return the case to the lab.
Designed to provide temporary adhesion during try in of bridges, splints, and porcelain-fused-to-metal crowns and bridges, Opotow Trial Cement is a nonhardening material that can easily be removed after the try in is completed. The temporary material kit includes accelerator, base, mixing pad, and tube key. The material is suited for use with temporary restorations from veneers to multiunit bridges.
I realize temporary cementation with Opotow Trial Cement involves an additional visit; it is well worth the extra time. You don’t want a patient to return with a complaint after permanent cementation.
This approach works because the rubbery consistency of the cement allows for easy, nontraumatic removal prior to final placement. Comparatively, regular temporary cement will harden. You must have faith in your lab, and confidence in your bite. The slight tooth movement during the time between the impression and insertion often is responsible for any difficulty in seating the restoration, and that will correct with trial cementation.
It is easier to remove a prosthesis seated with a rubbery trial cement than a prosthesis without any cement at all. There is no point to using a hard setting temporary cement, as that will not permit crown movement. It is best to use a rubbery cement that allows the prosthesis to seat in function. When you remove the prosthesis prior to permanent cementation, Opotow Trial Cement usually peels cleanly out of the crown.
A word of caution: It is best to use a thin viscosity permanent cement that will permit full seating of the prosthesis. Also, watch your setting time. The permanent cement is thinner than the trial cement, so the prosthesis will actually feel even more comfortable to the patient after permanent cementation.
Allowing a patient to wear a fixed prosthesis for a period of time before final cementation offers benefits from a patient/dentist relationship, as well as a legal relationship. The prosthesis will be more comfortable if you let the case fully seat for a few days in function. Tell the patient to bite on it, chew on it, and use it (but avoid chewing gum or sticky foods). Wearing the prosthesis for a few days also helps detect unseen defects prior to permanent placement.
The patients will be very appreciative if you tell them they will have an opportunity to wear the prosthesis before final cementation. A fixed prosthesis might not seat for 1 or more of several reasons, such as bad fit due to a poor impression, bad bite impression, tight contacts from excessive contact reduction, or too thick cement from being either improperly dispensed or mixed, or set too quickly. Such a crown is not fully seated, and will have open margins filled with cement that could be a future source of decay and gum recession.
If you were careful with your bite and impression technique, you should hardly ever have to adjust the occlusion. Our 21st-century impression and bite materials, along with excellent laboratory techniques, should make occlusal adjustments a memory from the 20th century.
“Try before you buy” is ever more pertinent when inserting crowns and fixed bridges. It lets the patient try the new prosthesis before permanent cementation. Doubting patients will become your biggest fans.