Do You Have a Xerostomia Strategy?
Dealing better with dry mouth patients starts with a screening, diagnosis, and management protocol.
©Andrey Popov / stock.adobe.com
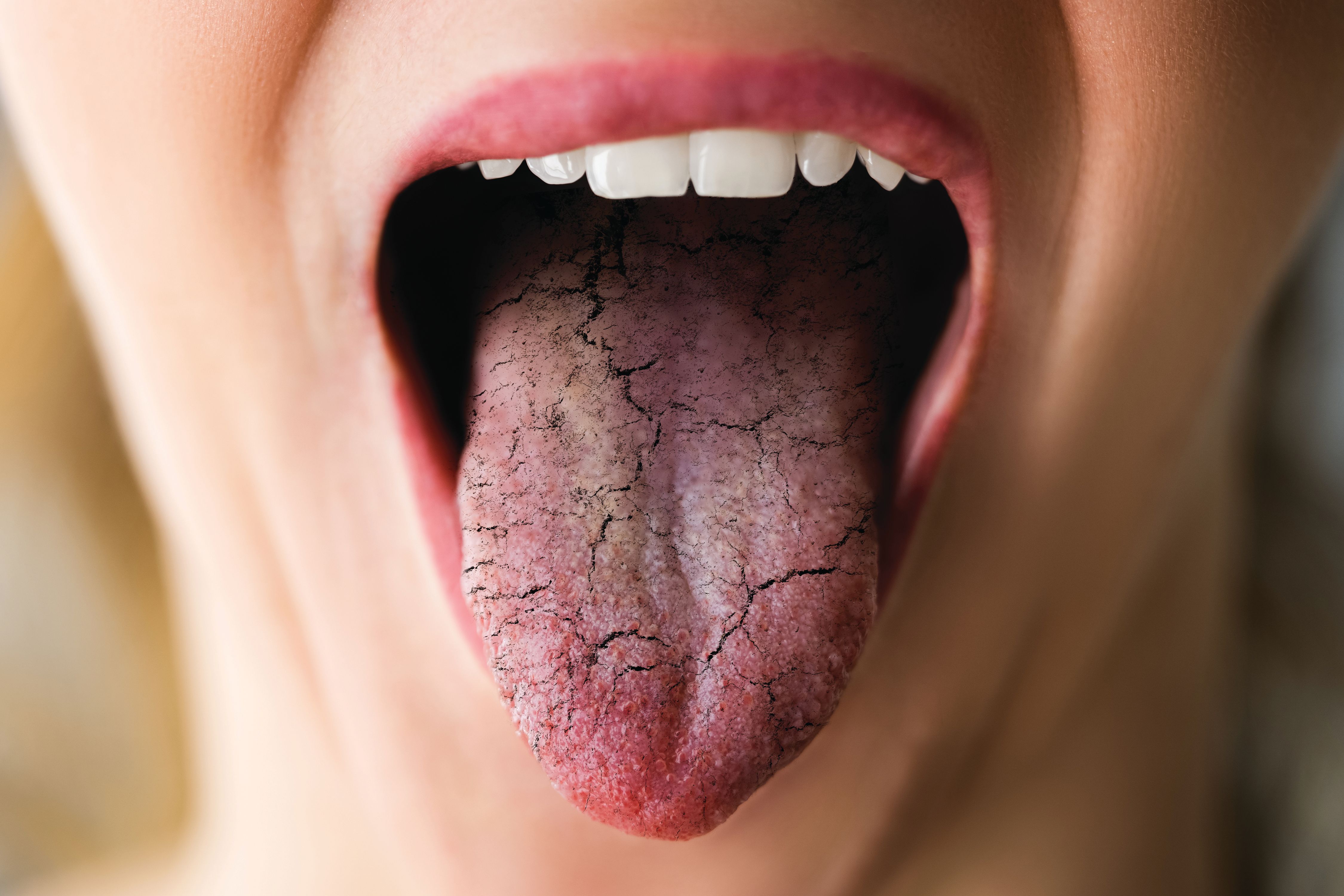
According to the Cleveland Clinic, an estimated 4 million Americans have Sjögren's Syndrome, an autoimmune disease that affects the entire body. Characterized by extensive dryness in the mouth and around the eyes, Sjögren's includes other complications, such as profound fatigue, chronic pain, major organ involvement, neuropathies, and lymphomas. But do we know how to support and manage it?
Sjögren's—pronounced “SHOW-grins”—can increase a patient’s risk of caries and other oral complications, but for Brooke Crouch, RDH, her dental office was not the resource she hoped for or needed when she received her diagnosis of the disease.
Through her own research and self-advocacy, she has become a trusted voice helping dental professionals translate Sjögren's symptoms into dental office strategies. I was excited to sit down with her to learn more about her experience and the clinical options and technology that are changing the standard of oral care as we work to manage this disease.
Lou Shuman: When you and I first spoke about the limitations many practices face when addressing xerostomia (dry mouth), I saw a number of similarities to the gaps related to screening for sleep apnea. The dental community needs a protocol for screening, diagnosing, and equipping patients to manage conditions that are increasingly common. I’d love for you to help readers better understand the part they can play.
Brooke Crouch: I was diagnosed with Sjögren's by an endocrinologist a little over 5 years ago. He tested me based on constant dry eye complaints; it took almost 2 years before I started dealing with the oral complications.
Before that point, I never had a cavity; I was a very low-risk patient. That low risk changed overnight, and I became desperate for answers. I’m a hygienist, and I could do research and reach out to companies to ask for things to be sent to me, but it felt like I was doing all the research and basically creating my own treatment plan and interventions.
When I asked my own dentist for her recommendation, all the office offered me was 1 brand of prescription toothpaste. There weren’t options.
LS: Why did that fall short as an intervention?
BC: At 5000 parts per million, toothpaste focuses on getting more fluoride into the oral cavity, which is good for many patients, but not in severe cases. Is it something we can throw at xerostomia? Yes, but it’s not enough. Sjögren's patients need more. Through my research, I was learning how recurrent decay is an issue for Sjögren's patients, and I didn’t want to go down the road of restoration after restoration. I didn’t want restorations. I wanted a treatment regimen.
Because Sjögren's syndrome is an autoimmune disease, I was primarily seeing a rheumatologist. However, when I started to have eye issues, he sent me to the eye doctor, and when I started to have dental side effects, they told me I needed to see a dentist. Patients end up with all these different people telling them what they should do, and although some dental offices are innovative, many are doing the bare minimum— some don’t even stock a prescription toothpaste as an option for their patients. There’s no standardized training in our profession for addressing xerostomia.
LS: It’s very upsetting to hear what you went through. We as a profession should be able to respond better to a patient who presents with this. If a practice wanted to create a tool kit for addressing xerostomia, what might it include?
BC: It is important for practices to know that you can’t judge dry mouth based only on salivary flow. Sometimes I’ll go into an office, and I’ll have saliva, so they think I’m fine. The truth is, adequate salivary flow doesn’t mean quality saliva, so practices should carry pH and buffering capacity strips—they go under the tongue—to test. If a patient has low pH (less than 6.5), you want to recommend products that help raise it, such as xylitol. OraCoat makes XyliMelts, which help lubricate the oral cavity and keep the pH raised.
I mentioned earlier that my office offered 1 brand of prescription toothpaste, but there is also a 5000 parts-per-million toothpaste called FluoriMax from Elevate Oral Care that has xylitol. Xylitol being added to the toothpaste is something our Sjögren’s and xerostomia patients need. I recommend pairing that with an electric toothbrush and water flosser, such as Waterpik Sonic Fusion. Without salivary flow, it is much harder for a patient to clear food debris from the mouth, so food sits longer on surfaces in an acidic environment. I also use GC America’s MI Paste, which uses salivary proteins to deliver bioavailable calcium and phosphate to the tooth surface during the demineralization and remineralization processes.
LS: Where does technology fit in terms of creating value and offering relief to the patient? Is the Voutia device for people who experience chronic dry mouth considered more of a supplement or a replacement for the “tool kit” you described?
BC: Voutia can be used 24 hours a day, even while sleeping, but I still use it as a supplement. It has a huge impact on my quality of life. It is brilliantly engineered—not uncomfortable or scary—and a good option for moderate and severe cases.
LS:Just as important as having the right equipment is having the right information. With so many issues presenting in the dental office, how do we put something like xerostomia generally or Sjögren's specifically on the dental team’s educational radar?
BC: My first goal is to create a course that can be offered to offices that need the training. It would provide critical information to the dental team and also offer guidance on how best to educate patients who are suffering.
I also think there is room for improvement in how dental practices screen for xerostomia. Developing a xerostomia risk assessment—similar to the caries or periodontal risk assessment—to help dental professionals be proactive in supporting their patients is important. Hopefully, dental insurance providers will also be able to catch up in how they cover care for patients with dry mouth, who require more frequent cleanings and should be on a shorter recall, every 3 months instead of every 6. All these things should be part of a dry mouth treatment protocol.
About the interviewee
Brooke Crouch, RDH, is a remote supervision dental hygienist, outreach coordinator, advocate, educator, oral health champion, consultant, and volunteer. She is vice president of the American Mobile Dentistry Alliance and chairs and sits on several clinical advisory, oral health action, and community-based boards and committees. She can be reached at brookecrouchdentalconsulting@gmail.com.