Technique: Why GC Initial™ is a simple choice for complicated esthetics
GC Initial™ from GC America Inc. is used as part of this comprehensive treatment plan to transform a patient’s smile.
GC Initial™ from GC America Inc. is used as part of this comprehensive treatment plan to transform a patient’s smile.
Since the early 1990s, general dentistry and prosthodontic practices have witnessed a steady increase in the number of patients wanting to make an elective change to their smile. This influx of cosmetically driven patients has demonstrated an interesting point.
Modern patients are in the habit of self-educating and will often come to their dental professionals not only with a clear idea of what outcome they would like to achieve, but a list of procedures and products they would like us to use.1
With steadily more knowledgeable patients and a continued rise in demand for esthetics, dental professionals have seen a congruent rise in educational programs designed to provide the restorative dentistry team with the requisite knowledge to deliver beautiful, predictable, and durable results. 2
This high demand also has necessitated the chemists and engineers who make restorative dental materials to provide increasingly durable and esthetic compounds with more efficient processing capabilities and lower rates of failure.
These requirements are met by current dental ceramics,3 however a talented restorative team is still needed to properly perform a smile improvement.
As the esthetics market grows in the dental practice, the entire team must be able to perform accurate and efficient procedures and send a patient to the next step in treatment without fear of complications. This requires the dental assistant to keep accurate, clear records, impressions, and x-rays. It requires the hygienist to perform high-quality cleaning, whitening and patient education services.
The laboratory must continually produce anatomically correct and well-fitting restorations.
It requires the dentist to perform general dentistry well and place restorations artfully, and the entire team needs to communicate accurately and perform as a cohesive unit.4
It also is of paramount importance to include the restorative team, laboratory and patient in the treatment planning process because, ultimately, this will determine not only the course of treatment, but preparation and material guidelines.5
Case presentation

A 55-year-old male patient presented with the desire to enhance his smile’s appearance with in-office whitening (Figs. 1-4).
The desired effect was a more youthful smile, as the patient was about to embark on a new employment venture. After the whitening consult, a comprehensive records examination including a TMJ/occlusal evaluation, restorative charting, full periodontal probing, and oral cancer screening was performed.
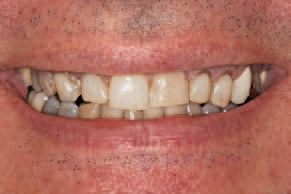
The patient had old crowns, bonding, and broken fillings with decay present, so the dentist developed a restorative component to the patient’s treatment plan to fully realize the desired youthful appearance. However, in-office whitening could be conducted.
Initial treatment
The patient’s discolored dentition made him a good candidate for whitening, but the
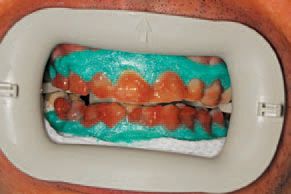
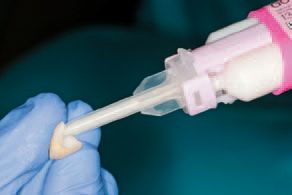
effectiveness of the whitening procedure is based on the concentrate of hydrogen peroxide/carbamide peroxide solution and how long it is left on the teeth. The clinical team decided upon an in-office whitening procedure (Ultradent Opalescence® Boost 40%) in combination with a nightguard vital bleaching procedure (Ultradent Opalescence ®) that consists of viscous 10% carbamide peroxide material in a syringe delivery system.
After the in-office treatment, the patient was instructed to continue the night whitening procedure for three weeks, then return for a follow-up visit to check his progression.
Follow-up, planning
During the follow-up visit, the patient was highly satisfied with the whitening results, but it was agreed that restorative procedures were necessary to accomplish his esthetic goals. Diagnostic models were taken and mounted with the Slidematic facebow in centric relation on a Denar® combination articulator (Whip Mix Corp.).
The esthetic goals were waxed into position by the laboratory ceramist (Walt Richardson of Bay View Dental Laboratory). This model was used to fabricate provisional matrices.
Treatment plan
Discussion led to agreement on a treatment plan consisting of restoring tooth Nos. 4-12 using GC Initial (GC America). The patient did not want any tissue adjustments. The goal was to add 1.25 mm vertical length, while positioning the restorations slightly more lingually to allow for a more harmonious lip closure path.
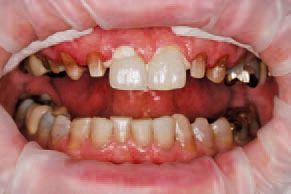
Provisional restorations
Tooth Nos. 4-12 were prepared for GC Initial bonded restorations (Figs. 5-6). The dentition was equilibrated to centric relation. After final impressions and jaw relation records, the teeth were provisionally restored with Structure 3 Provisional Material (VOCO America) and cemented with GC Fuji TEMP™ LT (GC America).
The provisional restorations were then systematically contoured to provide all the requirements of stable occlusion and satisfy the patient’s esthetic needs.
The patient was seen for a 48-hour follow-up appointment to evaluate esthetics and envelope of function. When all parameters were met to satisfy doctor and patient, an impression was made of the provisional restorations, digital photographs were taken of the patient’s face, and a Crossref bite record was made to aid in the cross mounting with the die model in the laboratory.
The photographs, impression and bite record served as blueprints, communicating to the laboratory what the final restorations should look like.
More Step-By-Steps on the Next Page ...
Laboratory fabrication
The dentist wanted a universal all-ceramic system containing zirconia, and he and Matt Shafer, CDT, of Bay View Dental Lab decided on GC Initial because of its high strength, incredible esthetic properties, and ease of processing.
Steps to fabricate the restorations
Using the impressions of the patient’s teeth before the provisional restorations were placed and a provisional model, zirconia copings for the restorations were designed and milled. A porcelain layering technique was then used to create an optimal esthetic appearance with a process that is easily learned, efficient, cost-effective, and not very technique-sensitive.
GC Initial™ IQ- Lustre Paste NF was applied to the restorations prior to beginning the build-up to shade the copings. A combination of Opacious Dentin Modifier, Inside, and Fluorescent Dentine powders are applied to the copings to establish proper color saturation and reflective zones.
Standard dentin mixes and a proper lingual/incisal edge matrix were used to layer functional lingual contours. With the working side established, all attention can be focused on a true-to-nature build-up process to meet the patient’s specific needs and desires.
The incisal was contoured with enamel or transparent mixtures, and by means of a “cut- back” technique, the area was reduced to internal dentin levels. The reduced area was reconstructed with reflective dentins and transparent enamels in the desired anatomic structure.
This was a very important point for color synchronization. One does not wish to wash out, or allow excessive show through of the internal structures of your crowns. The final contouring was built from a mixture of Enamel Opalescence (EOP) standard Enamel (E) and CL-F.
The restorations were checked on both trimmed and untrimmed models ensuring proper proximal contacts, margin accuracy, function, and occlusion. The final GC Initial restorations were then sent to the dentist for placement.
Delivery appointment
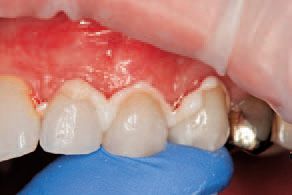
The final restorations were evaluated and inspected for marginal fit on the master dies. The patient was anesthetized, and the provisionals were carefully cut away in sections so the underlying tooth structure would not be damaged. The exposed preparations were cleaned with chlorhexadine scrub (Consepsis, Ultradent), and each individual restoration was tried in with water to check the marginal fit, occlusion, esthetics, and final color.
The patient approved delivery of the restorations. After patient approval, each restoration was thoroughly rinsed and dried, etched with 37 percent phosphoric acid, and silanated with Ultradent’s Porcelain Etch and Silane. The definitive restorations were then bonded into place using GC FujiCEM™ 2 Automix resin modified glass ionomer luting cement dispensed directly into the restorations with its syringe delivery system (Figs. 7-9).
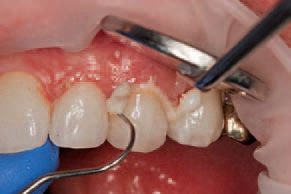
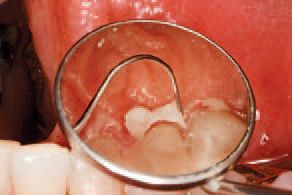
Excess cement was removed from interproximal areas by careful flossing, and final
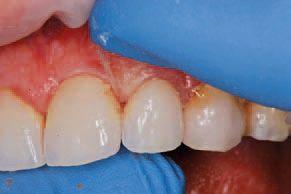
cement cleanup and occlusal adjustments under water were then completed (Figs. 10-11).
When viewing the finished restoration, the optimum incisal placement was noted from a vertical and horizontal perspective, and precise placement toward the inner vermillion border of the lip established the desired lip closure.
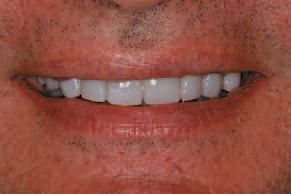
Closing thought
This patient presented with a discolored, aged smile and wanted to look more youthful for his new employment venture. Through careful treatment planning, excellent hygienist work, outstanding laboratory communication, and talented restorative dentistry, the entire dental team helped him achieve his esthetic goal (Fig. 12).
As demonstrated by this case, it is imperative to have appropriate and predictable restorative materials like GC Initial for esthetic dental treatments, as well as a talented, well-communicating restorative team to perform them.
See References on the Next Page ...
References
1. Frost & Sullivan. Market insight. The rise
of Cosmetic Dentistry. http://www.frost.
com/sublib/display-market-insight-top.
do?id=221252128. Accessed February 11,
2013.
2. PB Osborne, J Skelton. Survey of
Undergraduate esthetic courses in U.S. and
Canadian dental schools. http://www.jdentaled.
org/content/66/3/421.short. Accessed
February 11, 2013.
3. Vagkopoulov T, Koutayas SO, Koisdis P,
et al. Zirconia in dentistry: Part 1. Discovering
the nature of an upcoming bioceramic.
The European Journal of Esthetic Dentistry.
2009;4(2):4.
4. Ruiz, JL. Achieving predictable, beautiful
smiles using a dento-facial esthetic diagnosis
system. Compend Contin Educ Dent.
2007;28(1):50-55.
5. Rosenthal, L. Preparation guidelines for
less invasive cosmetic restorations. Gen
Dent. 2007;55(7):624-30