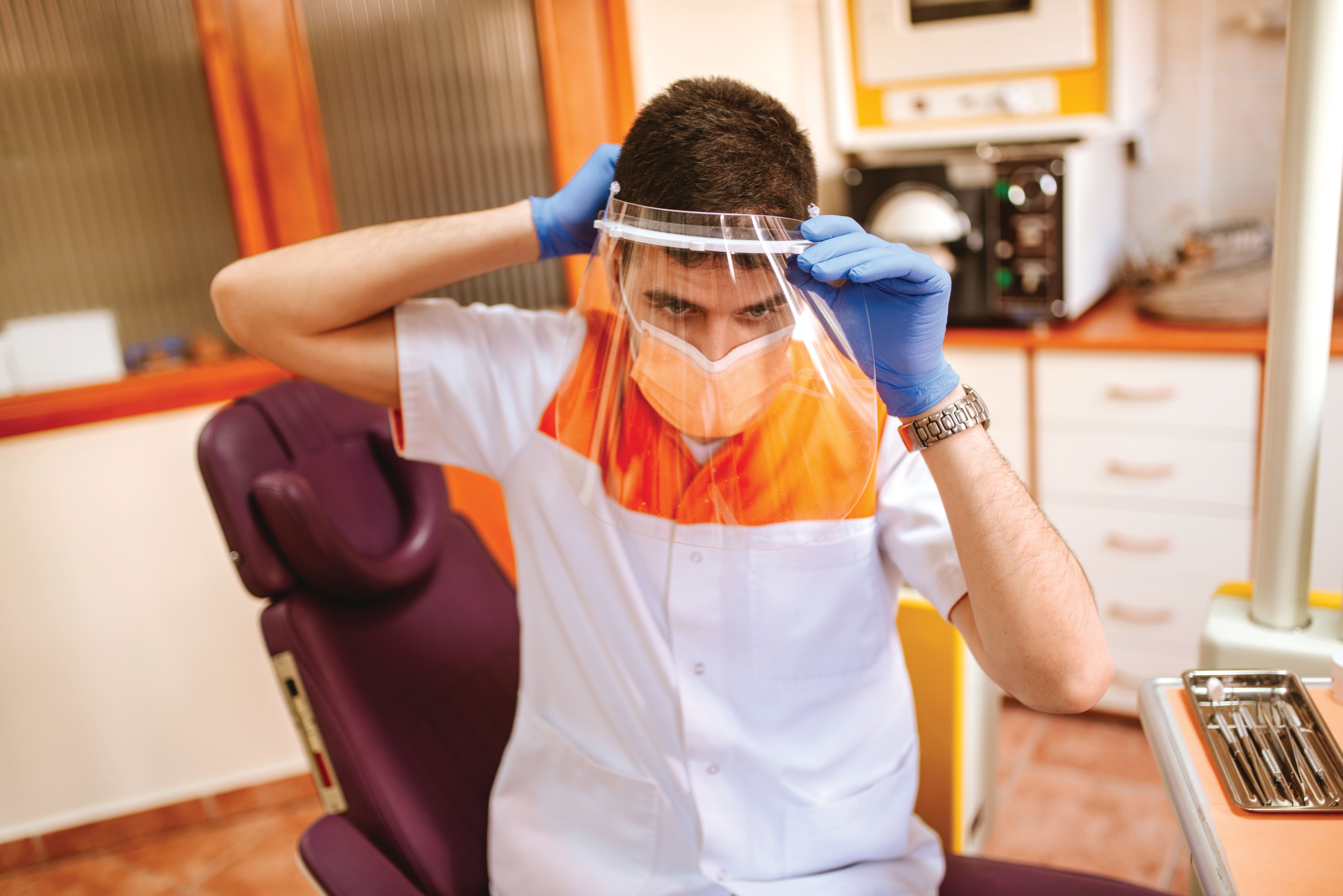
During the first weeks of the coronavirus disease 2019 pandemic, most dental practices closed their doors to patients, although many remained open for emergencies. Since reopening in May and June, practices are running under a new standard operating procedure.
Practice owners may have feared patients wouldn’t return, but most are seeing the opposite. Patients are so eager to return to their dentist’s office that many practices are booked well into October.
“I was shut down between March 18 and May 18,” says John Flucke, DDS, who practices in Kansas City, Missouri and is Chief Dental Editor for Dental Products Report. “Since we’ve reopened on May 18, I can barely sit down. It’s a good thing, but it just doesn’t make any sense to me. Everyone was saying that nobody was going to go out or spend money for fear of the economy, but life has been crazy busy.”
Additional Resources for Healthcare Professionals
Centers for Disease Control and Prevention: Interim Guidance for Businesses and Employers Responding to Coronavirus Disease 2019 (COVID-19)
bit.ly/CDCBusinessEmployers
Centers for Disease Control and Prevention: Interim U.S. Guidance for Risk Assessment and Work Restrictions for Healthcare Personnel with Potential Exposure to COVID-19
bit.ly/CDCWorkRestrictions
Centers for Disease Control and Prevention: Criteria for Return to Work for Healthcare Personnel with Suspected or Confirmed COVID-19 (Interim Guidance)
bit.ly/CDCReturntoWork
Centers for Disease Control and Prevention: If You Are Sick or Caring for Someone
bit.ly/IfYouAreSickCDC
Centers for Disease Control and Prevention: How COVID-19 Spreads
bit.ly/HowCovidSpreads
Despite the nation getting back to normal, the number of COVID-19 cases is still rising. Since reopening more public spaces, every day in July saw record numbers. Several states set record highs for daily new coronavirus cases as of mid-July, including Alaska, California, Florida, Texas, and North Carolina.
Despite the ever-present danger of the pandemic, dental professionals believe it is their duty to continue to provide care to patients.
“In March, we all thought this was just a virus, so we treated it as such,” says Katrina Sanders, RDH, a member of the Modern Hygienist editorial advisory board. “But we’re now learning that not only does this virus replicate in the host, which is done through inflammatory pathways, it also has systemic complications.”
Sanders says individuals with high levels of inflammation are experiencing the worst symptoms of the virus. Because periodontal disease is the second-most frequent modifiable inflammatory condition in the U.S., she believes dental professionals play a critical role in mitigating the effects of this illness on the most vulnerable population. For that reason, it’s unlikely that her practice in central Arizona will see another closure.
“We opened fully on May 1, but we’ve recently seen an incredible spike in COVID-19 cases in Arizona, so we take it day by day,” Sanders says. “However, I don’t suspect we’ll go back to just treating emergency cases.”
Many practices reopened to help keep their dental patients out of emergency departments. “We felt strongly about our obligation to see patients when they had dental issues so we could keep them out of the ER,” says Jeffrey Rohde, DDS, who practices in Santa Barbara, California. “The ER isn’t as equipped to handle dental issues. Plus, they’re using up time and resources on dental patients, and dental patients are potentially being exposed to illnesses.”
While there are some exceptions, most dental professionals feel safe returning to work. There have been changes in infection control protocol in every practice in the U.S., but many of them are subtle, because they were already doing what they could to limit the transmission of airborne infections before the pandemic.
“I [am in] surgeries in the operatory with our periodontists,” Sanders says. “When I would go into a surgical operatory, I would wear a hair bonnet, a gown, and a level-3 ASTM mask. Our patients were using pre-procedural mouth rinses, and my assistant was using a high-volume evacuation system.”
For Sanders, the only differences now are that she never removes her mask and she wears a face shield over it. The difference for patients is that they wear a mask when they come into the practice. These aren’t major changes.
“Our office had been doing a lot of these things before coronavirus came to the U.S.,” she says. “Our practice might look a little different, but it’s not dramatically different, and our patients appreciate that. They recognize that we were doing the things that were necessary before this pandemic.”
One area where practices are seeing significant changes is the patient experience. Waiting rooms have become obsolete. Patients wait in their cars in the practice’s parking lot, only entering the practice after they’ve received a text from the front desk telling them it’s their turn to check-in.
They are screened as they walk in, which includes taking their temperature and asking them questions about any symptoms and their potential risk. Paperwork has been completed online in advance, or patients fill out forms with a sanitized pen, which they then keep or throw into a container for disinfection. Patients wear masks before entering the facility and only take them off once they are in the dental chair. After the procedure, the mask goes back on and the patient leaves the facility, likely without encountering another patient on the way.
The risk of contracting COVID-19 increases whenever someone leaves their home, and the dental practice is no exception. However, seeing the new procedures in place in dental practices alleviates the fear many patients have. “All you have to do is walk into a dental office to know that we are doing things differently,” says Kim Miller, RDH, BSDH, a consultant and coach for Inspired Hygiene, and a member of the Modern Hygienist editorial advisory board. “We are dressed differently, taking temperatures, asking different questions, and asking patients to sanitize their hands. And because we’re doing things differently, patients are feeling safe.”
While some practices already had most of the recommended personal protection equipment (PPE) on hand during this pandemic, many delayed reopening because of a delay in getting PPE. Some previously donated the PPE they had to hospitals, which were more in need in those first few weeks.
“We were concerned hospitals weren’t going to have enough gear to handle the number of patients,” Rohde says. “We were seeing nurses in New York wearing trash bags, so we donated our own stuff. And then in early May when it looked like we were going to be able to open up again, we tried to reorder stuff and we couldn’t get it. PPE was either being requisitioned by the state of California to be used for health care workers, or people were hoarding what they had.”
To work around the PPE shortage, Rohde’s staff found old lab coats in their closets, which they would use once before placing in bags until they were deemed safe to wash and use again. For masks, they were wearing 3M N95 masks from the hardware store under level-2 and level-3 masks, which served as barrier protection.
"Thankfully, we were on a limited schedule, so we didn’t need a lot of equipment,” Rohde says. “But that’s how we saw people for a week or two until our orders came in.”
Other practices near him were using daily racks for their medical supplies, cycling the supplies weekly so that any contamination would dissipate before the next use.
Donning proper PPE for aerosol-generating procedures (AGP) is not new in dentistry, but that doesn’t mean the newest recommendations have been easy to meet. The industry is seeing a shortage of dental hygienists and assistants, some of whom fear returning to work because their practice isn’t following the CDC’s recommendations.
“The CDC has guidelines, but ultimately, they leave most of these guidelines to the interpretation of the employer who is providing the equipment,” Sanders says. “There are a lot of dental professionals in a situation in which they don’t have the recommended equipment. Many of them are trapped in an ethical dilemma in which they must consider how to effectively treat their patients with a level-2 or level-1 mask or without proper high-volume evacuation or are expected to return to work even though the equipment they need is on back order.”
She adds that because the guidelines are left open to interpretation, some practices require their staff to work even if they test positive for the virus. While this is a highly questionable decision, practices will start seeing more staff members test positive in the next few weeks and months, and they’ll need to have a protocol in place.
“This is going to happen in every dental practice in the country at some point,” Rohde says. “One of their staff members will test positive, not because they got it at work, but because they’re living their lives. People are still going to restaurants and birthday parties.”
One of Rohde’s staff members has already tested positive for the virus. The staff member didn’t have any symptoms and was tested as a precaution before seeing an elderly family member. When Rohde told his staff the next day, he says there was a collective panic.
“The whole worry was that doctors’ offices were going to suffer economic ruin from having to shut down for two weeks every time someone tests positive, but the CDC is saying not to panic and shut down,” he says. “They say that if a health care provider works with someone who has tested positive, but they’ve been wearing their mask around them, they don’t have to run out and get tested. If they weren’t wearing a mask around the person and were closer than six feet for more than 15 minutes, that’s considered high-risk exposure—in which case that person should quarantine and get tested.”
Rohde then came up with a clear set of guidelines, which he calls a decision tree.
“This isn’t going away any time soon, so you need to have those protocols,” he says. “Even if you think the steps on your plan are over the top, just have a plan. And know that the second you hear something new, you can update it.”
He advises answering questions such as, what do you do when a staff member or a patient tests positive? What do you do when a patient says they feel OK, but they have a sore throat? It takes some pressure off the staff to know how the practice will deal with these situations before they arise.
Flucke seconds that opinion. “One of my mentors told me that if I prepare for an emergency, then it ceases to be one,” he says. “So, when things like this happen, I plan for the worst-case scenario. I feel like I can plan around most of this and we’ll be just fine.”
Overall, the patient response has been positive. Some practices are seeing patients get defensive after being told they have to wear masks in the practice, but those are rare cases.
“I’ve had about five patients refuse to wear masks in the office and have instead elected to wait until masks aren’t required,” Flucke says. “I don’t think the sky is falling, but you do have to analyze what is safest, and cutting infections by wearing masks and washing your hands is the safest. I don’t know how it went from ‘masks prevent infection’ to ‘don’t oppress me.’”
For practices that weren’t very cautious about AGP before, these recommendations will bring lasting changes. After all, infection control standards and policies have been built on previous epidemics, Sanders says.
“Nobody was wearing gloves and masks in dentistry until the HIV/AIDS epidemic,” she says. “The industry was very cavalier when it came to bloodborne pathogens prior to that. Here we are on the other side of the spectrum with airborne pathogens, recognizing that perhaps we haven’t been cognizant of what the research was recommending, and that’s a problem.”
Sanders adds that it has been normal to show up to work sick and to treat patients who are sick in order to keep a productive schedule. Sick days for many are rare, and we may save them for vacation or childcare leave. But calling in with a fever and body ache now is taken much more seriously.
“These are things that we have needed to change in the culture of dentistry for a long time,” she adds. “The dental practices that are going to take this opportunity to pivot and do the right thing are going to rise to the top. We saw this with the HIV/AIDS epidemic: the offices that did not align with what was required of them in that moment, who had doctors reusing needles or improperly sterilizing equipment, had to send letters to their entire dental populations explaining that they were likely exposed to HIV and Hepatitis C. We’re going to see the same thing for the practices that force positive-testing employees to come in or who go back to doing things the way they were before.
“This is a big wakeup call for the dental community,” Sanders continues. “This is an opportunity for us to define ourselves as essential workers, given the work we do with inflammation to mitigate the risk of infections. This is our chance to pull up a seat at the table with all of the other medical providers who are truly doing integrative work for comprehensive patient care. Now is the time to elevate our standards and permit patients to expect better of us.”