Infection control technologies keep dental teams, patients safe
With the COVID-19 pandemic’s spotlight on infection control, it’s vital to know what products offer the best protection. Here’s how to incorporate infection control technologies into your dental practice’s workflow.
OSORIOARTIST / STOCK.ADOBE.COM

Fears of spreading coronavirus disease 2019 kept dental practices across the country closed for months. As offices begin to reopen, everyone is exploring how best to protect team members and patients from this disease.
While infection control (IC) has always been a priority, the COVID-19 pandemic has brought it to center stage. Dentistry is one of the occupations at highest risk for spreading the virus, and clinicians must take extra precautions, according to Sharon Ward-Fore, an infection prevention consultant. COVID-19 is transmitted through aerosol droplets, which can be plentiful during many dental procedures, and social distancing isn’t an option when treating patients chairside.
There are many infection control technologies that help limit exposure to coronavirus, but it can be difficult to keep track of all the options. How do you know what will work best for your practice, and how will you communicate the changes to your team members and patients?
First, stay up to date on guidance from the Centers for Disease Control and Prevention (CDC), the American Dental Association, and other national and state authorities. Recommendations shift as more is learned about the virus, so make it a priority to stay informed and adjust IC protocols as needed.
Aerosol prevention and reduction, air filtration, surface disinfection, personal protective equipment (PPE), and instrument sterilization are all IC areas that need extra attention these days, requiring updated procedures and protocols that will likely be with dental practices for years to come.
“We’re not out of the woods at all,” Ward-Fore says. “It’s not like this is over and it’s back to normal. We’re in the maintenance phase, and this is where we can’t get complacent. We need to be at the top of our game.”
Preventing and Reducing Aerosol Droplets
While many dental procedures produce aerosol droplets, there are steps that can be taken to prevent and reduce them. One of the best ways is to use a rubber dam, Ward-Fore says. This underused, old-school IC method can be quite effective in protecting you and your team members from COVID-19.
Ward-Fore suggests using disposable rubber dams rather than those with reusable frames. There are some available that cover part of the nose, fully protecting dental professionals from exposure to respiratory droplets and aerosols.
“This is a super simple technology that should be embraced by all,” Ward-Fore says. “It goes in the patient’s mouth and kind of seals it off so the practitioner is working only in a protected field. Just the teeth that need to be worked on are exposed.”
The Mr. Thirsty isolation and suction device from Zirc is designed to make isolation easier.

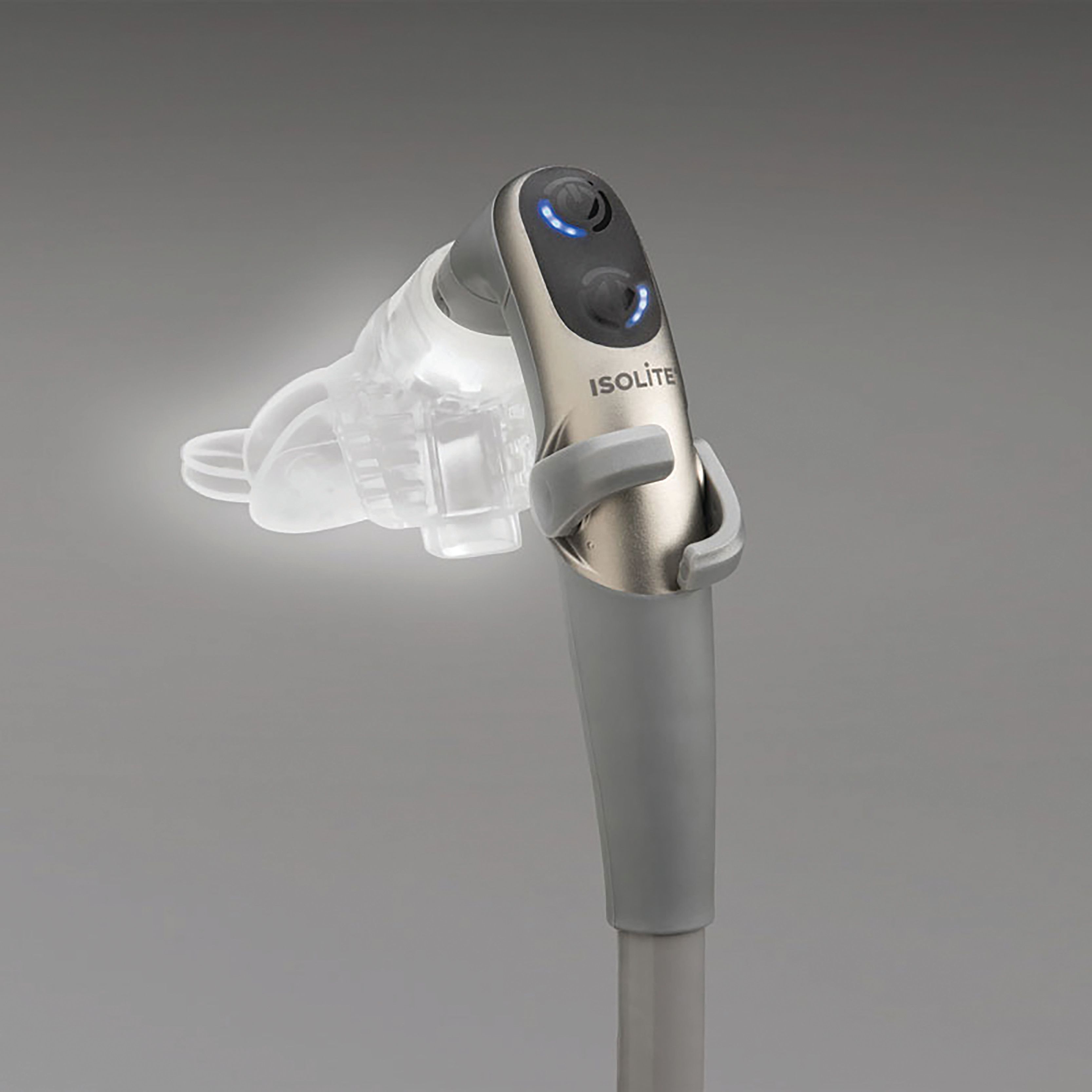
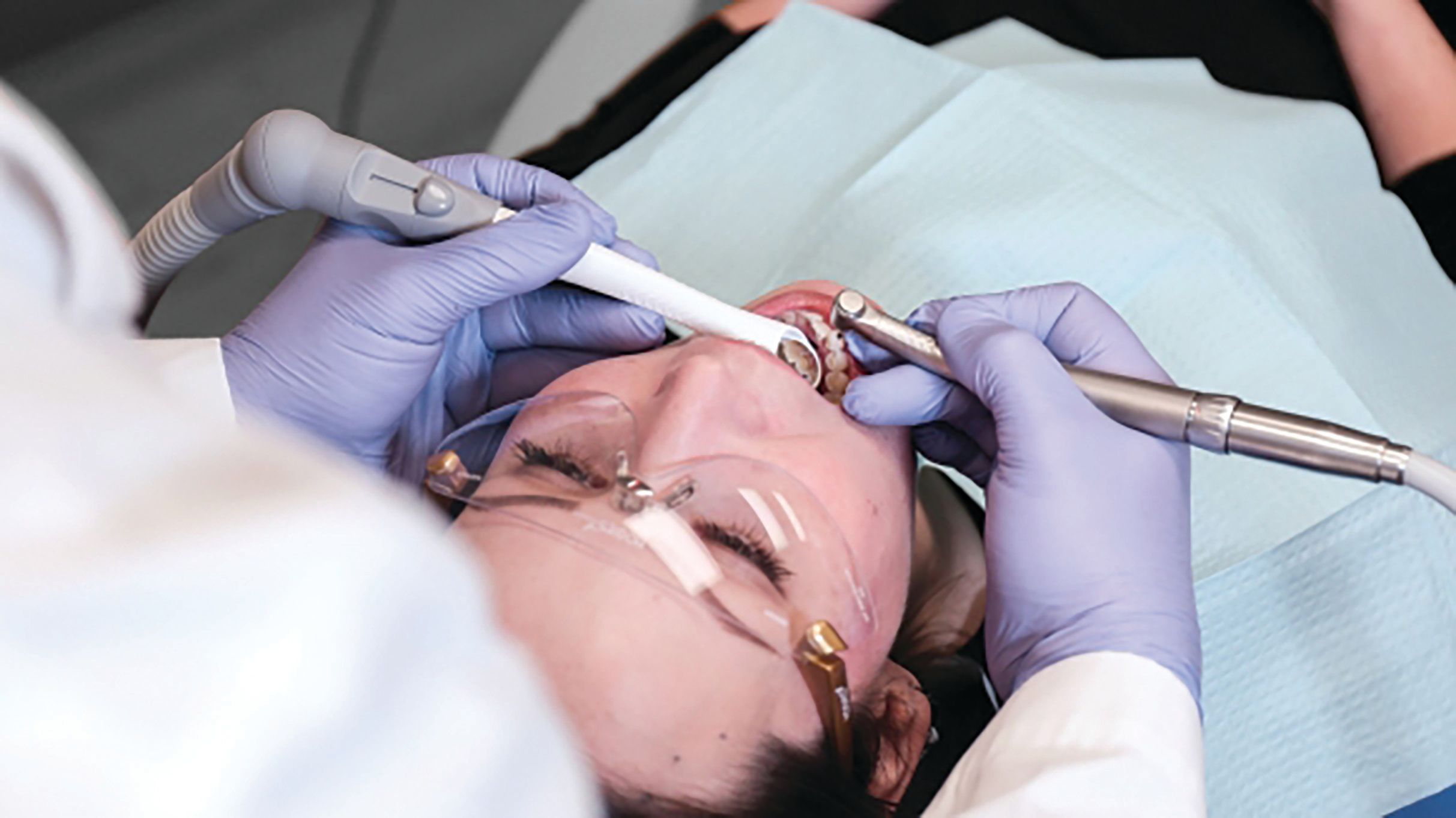
Isolation devices such as the Isolite from Zyris are also effective at aerosol reduction. Ward-Fore described the Isolite, which combines light, suction, and retraction, as a “rubber dam on steroids.” The Isolite features a fitted mouthpiece that protects soft tissue and the airway while also providing retraction. Its suction capabilities make it possible to continuously evacuate saliva and debris, while the LED provides proper visibility into the field. The Mr. Thirsty isolation and suction device from Zirc and the Isovac dental isolation adapter from Zyris are other products that make isolation easier.
A high volume evacuation (HVE) system also is critical, Ward-Fore says. HVE devices, such as the Purevac HVE system from Dentsply Sirona, essentially remove aerosols before they even leave a patient’s mouth.
HVE is common in procedures the doctor and assistant complete, but hygiene generally uses saliva ejectors, says Mary Govoni of Mary Govoni & Associates, a Kansas-based company that coaches dental practices on safety. Since the pandemic, she has started advising practices to use HVE for hygiene patients as well.
“The hygienist needs something that has more volume to it than a saliva ejector,” Govoni says. “If the hygienist is scaling or polishing and using an ultrasonic scaler, the saliva ejector will remove fluids but it’s not controlling the aerosols.”
There are extraoral suction devices that can be used to control aerosols, and there are also portable units, Govoni says. The Extra Oral Suction System from ADS, for example, features an arm that can be placed near a patient’s mouth to remove aerosols. A similar product, the A~flexX HVE Arm, attaches to the back of a dental chair and holds the HVE hose with a suction tip or funnel placed outside the patient’s mouth.
Another way to reduce aerosols is to put the ultrasonic scaler away and instead hand scale, at least for now.
“I recommend going back to more manual practices and using four-handed dentistry,” Ward-Fore says, “so there’s someone there who can manually help you and keep the level of aerosols down.”
Selecting Air Filtration
Many dentists are investing in high-efficiency particulate air (HEPA) filtration units to minimize the risk of coronavirus exposure. Standalone units are available, or a professional can come in and install an in-duct system that creates the ideal number of air exchanges.
An air filtration system traps particulate, with its effectiveness measured by how many times it can cycle the air, says Buzz Thompson, IC expert and founder of GermFree MD. HEPA filters offer a greater degree of filtration for trapping particulate. The more air that goes through these devices, the more particulate the devices trap.
Newer technologies not only trap the particulate, but they “trap and zap,” Thompson says. Ultraviolet (UV-C) light is an example of a “zap” technology. With UV-C systems, air is drawn into the handling unit and the UV-C light is applied to the trapped pathogen to render it inert. The challenge is that UV-C light is very effective, but only if it has enough contact time.
UV-C light can be distributed in-duct or via standalone units. Rooms still need to be cleaned prior to disinfection when this type of technology is used, Ward-Fore says, and standalone units can run only when the room is not occupied. It should be noted that UV-C has not been proven effective against COVID-19.
Cranberry USA’s Smart Dam can help reduce aerosols.

A newer technology to consider is air scrubbing. ActivePure, an air and surface scrubbing technology created in cooperation with NASA, can zap the air quickly without having to trap, Thompson says. The device turns humidity into hydrogen peroxide molecules that are safely distributed to clean and disinfect the air and any surfaces contacted, such as door handles, countertops, and surgical equipment. Thompson recommends placing the units in reception areas and operatories. They can be used to purify the air 24/7.
“Now we have a mechanism for occupied space infection control that’s effortless and highly effective,” Thompson says, noting that different types of air filtration can be complementary. “The ideal solution is something that’s proven, cost effective and requires little to no behavior modification. Combining air scrubbing devices in addition to an in-duct HEPA system, possibly with UV-C light in the duct work, provides a really nice package for a practice.”
UV-C wands are another option, but using them can be time consuming and tedious because you have to slowly go over the areas you want to disinfect, Thompson says. There are also aerosol sprays, but most tend to be toxic and don’t provide 100% saturation. Many dentists are turning to foggers, which are stronger than aerosol sprays. These devices can be effective, but fogging after every patient takes time and isn’t realistic for most practices.
Another challenge with foggers is the room must be cleaned before use, Ward-Fore says. Cleaning must occur prior to disinfection to allow the disinfectant to touch the cleaned surface for the manufacturers’ stated contact or dwell time. And the hypochlorous acid mist that foggers release has an odor that may bother patients or team members with respiratory conditions.
Govoni urges caution because studies validating fogging’s effectiveness are still being completed. While the mist released is nontoxic, she’s concerned with the potential for the particles to cause problems with technologies in the treatment rooms, especially if the solution isn’t at the ideal concentration.
Using Surface Disinfectants and Barriers
Treatment rooms should be disinfected after every patient using hospital-grade products with a kill claim for mycobacterium tuberculosis. That’s been the standard for years, Govoni says. Mycobacterium form spores and are difficult to kill, so if a product is effective against that, it will be effective against COVID-19. Any disinfectant you buy should have the mycobacterium tuberculosis kill claim; if it only protects against coronavirus, it may not be strong enough to take out other harmful pathogens.
On the Environmental Protection Agency (EPA) website, (epa.gov), you can find List N, a list of disinfectants that can be used to kill the coronavirus. All products on the list meet EPA’s criteria for use against SARS-CoV-2, the virus that causes COVID-19.
Isolation devices such as Isolite from Zyris are effective at aerosol reduction.
When cleaning operatories, Govoni recommends using disinfecting wipes instead of sprays. Sprays can be taken up in the air conditioning/heating system and circulated, possibly causing respiratory issues for team members, even if they’re wearing proper PPE. AdvantaClear, CaviWipes, or similar products are great options, or you can make your own. To do so, saturate 4x4 gauze in disinfectant, but don’t leave the gauze to soak, as that can deactivate the ingredients.
Putting plastic barriers on equipment and changing them between patients can reduce the amount of disinfecting necessary and save time, Govoni says. Barriers are something that will likely be more common in operatories. The biggest change in treatment rooms may be the removal of unnecessary items, such as pictures or patient brochures, because they can become contaminated with aerosols or droplets and potentially spread the virus.
CaviWipes from Metrex are ideal for operating rooms and dental operatories.

“Don’t have equipment sitting out on the counter for the next patient,” Ward-Fore says. “Make sure everything is tucked away in cabinets and drawers and don’t have any paperwork in the room. It’s a common-sense approach of limiting the amount of items that can be contaminated and making it easier to clean.”
Choosing PPE
PPE is key to keeping your team members and yourself safe. Not only do you need to wear more PPE now, you also must know how to properly put it on and take it off to avoid contamination.
For face masks, N95 respirators offer the best protection and should be worn during aerosol-generating procedures, Govoni says. While these were difficult to obtain early on in the pandemic, they should now be available. Try multiple vendors to secure these masks for your team.
If you can’t find N95s, then KN95s are the next best option, Govoni says. Both filter out at least 95% of airborne particles and must be fit tested. The N95 respirators allow you to breathe in and out of the device, and have 2 straps, 1 that goes on the top of the head and 1 behind the neck. KN95s and regular masks, which don’t offer the same protection, only have ear loops.
Whether you’re purchasing N95s or KN95s, work with a reputable vendor that isn’t trying to sell you counterfeits. The CDC and FDA offer resources to ensure sure you’re buying the real thing.
If neither the N95s nor the KN95s are available, a surgical mask can be used, Govoni says, but avoid performing aerosol-generating procedures on anyone suspected of having or diagnosed with COVID-19. These patients should be sent to a hospital that has the proper protections in place for treatment.
Per the CDC, dental professionals also should wear gloves, full face shields instead of goggles or safety glasses for eye protection and single-use, disposable gowns that are changed and disposed of after every patient. Gowns, which may be covered with droplets or splatter, should be taken off in the treatment room, Govoni says. The CDC also recommends wearing hair coverings because droplets or aerosols may settle in hair during procedures. Shoe coverings also are recommended.
While it has been recommended by some to put gloves on in front of patients so they know you’re taking the safety protocols seriously and not walking from op to op with the same PPE on, the CDC states in its interim guidance to put on clean, non-sterile gloves prior to entering the patient room.
“You also need to be diligent on how you wear your mask. It needs to cover your mouth and your nose,” Ward-Fore says. “You have to be all-in and wear everything appropriately. And if you touch your PPE and you’re wearing gloves, it’s time to strip those gloves off, do hand hygiene and put on a new pair of gloves.”
Sterilizing Instruments
Ward-Fore recommends using disposable products as much as possible, but for reusable instruments, it’s important to follow the manufacturer’s guidance on how to properly clean and sterilize them. The foam or gel pre-cleaner is used to prevent blood or tissue from drying on the instruments, which makes them harder to clean. The pre-cleaner keeps the debris soft, making it easier to clean prior to placing them in an autoclave or sterilizer for disinfection. Perform the necessary quality control on your sterilizer to ensure it’s working properly, and make sure instruments are clean and dry before they’re packaged, Govoni says. If packages are put away wet, they could tear, compromising sterility. Conduct spore tests weekly on sterilization equipment, and follow manufacturer instructions for proper maintenance and use.
HVE devices, such as the PureVac from Denstply Sirona, essentially remove aerosols before they even leave a patient’s mouth.
An instrument management system (IMS), such as the one from HuFriedyGroup, can help ensure instruments stay organized and clean, says Jessica Wilson, business development manager for HuFriedyGroup. When ready to be sterilized, the instruments are placed into a cassette that keeps them separated during reprocessing, maximizing the number of instruments that can be put into equipment at once while also ensuring they don’t get tangled and damaged. Placing instruments into a cassette also ensures they’re loaded properly in the sterilizer to achieve proper sterilization between patients. The cassettes feature color-coded labels to make it easy to match instruments to procedures.
“With this system, they have everything they need to sit down and finish that procedure,” Wilson says. “If the instruments aren’t organized, they have dental team members getting up in the middle of the procedure when PPE preservation is at an all-time focus for practices. They need to be organized when they sit down to avoid having to leave the room for anything until the treatment is completed.”
Investing in such a system shows your team and patients you’re serious about keeping them safe, Wilson says. Team members are protected from sharps injuries, the practice improves efficiencies, and the patients receive visible safety measures by having cassettes unwrapped in front of patients.
Implementing Changes
It’s important to get team members involved in the changes you’re making and for them to understand why they’re vital to protecting everyone in the practice. Offer training, which might include how to properly don and doff PPE and consider putting a team member in charge of your IC efforts.
Think of this team member as the voice of safety, Wilson says, and the person who communicates with patients about new precautions the practice is taking. The IC coordinator can research the various IC technologies to help decide what would work best for the practice, and they should stay informed on the latest guidance.
Make it clear to team members that everyone needs to follow the same protocols, Govoni says, and explain the rationale behind them. The GreenLight Dental Compliance Center by HuFriedyGroup can help with that. The website’s
tools (greenlightcompliancecenter.com) enables dental practices to create written documentation and protocols for all areas included in the CDC infection control guidelines. Each protocol includes specific, customizable steps for practices to follow. The information reflects what is actually being done in the practice and fulfills a need for documentation that many practices overlook. This helps promote consistency with how IC tasks are performed. The comprehensive online tools also include auditing so practices can ensure they’re following proper protocols.
Focusing on the Future
There’s no doubt coronavirus has changed dentistry. The products and procedures you’re implementing now will be part of your practice for the foreseeable future, making it critical to choose the IC technologies that will work best for your practice while keeping everyone safe from exposure to coronavirus.
“This is for the long haul,” Ward-Fore says. “It may be how dentistry and health care functions from now on. Maybe if we build these changes into our day-to-day practices now, we’ll be better prepared for the next big thing we didn’t know was coming. We’ll be more protected.”
