How to repair porcelain restorations instead of replacing them
Using composite resin, this case illustrates an efficient, reliable intraoral repair of fractured porcelain. These elements of esthetic dentistry can be very frustrating for both patient and practitioner especially in the case of an anterior tooth, yet most of these inherent problems with porcelain can be immediately and predictably repaired chairside with the use of composite resin.
Using composite resin, this case illustrates an efficient, reliable intraoral repair of fractured porcelain.
These elements of esthetic dentistry can be very frustrating for both patient and practitioner especially in the case of an anterior tooth, yet most of these inherent problems with porcelain can be immediately and predictably repaired chairside with the use of composite resin.
However, a study released in 2004 illustrated that of 87 porcelain veneers placed on 25 patients, 92 percent remained clinically acceptable (i.e. not needing repair or replacement) after 5 years, but only 64 percent remained clinically acceptable after 10 years.¹ Even under ideal circumstances, long-term function in the oral cavity (mastication), and such problems as diurnal/nocturnal bruxism, or an impact accident, can lead to porcelain fractures.
More how-to techniques: How to choose the most suitable temporization approach
Composite resin is frequently indicated for bonding, filling cavities, repairing fractures in crowns, onlays, bridges, and in the case presented here, repairing fractured porcelain veneers. It is important in the anterior region to match natural dentition in color and anatomic form, which composite resin easily achieves.² This is because available composite materials offer a variety of opaque and translucent shades, are extremely pliable, very resilient, and capable of being shaped or thinned using only a stream of air. Composite resin also possesses beneficial caries-inhibiting properties and increases the overall durability of restorations.
In the past, the problem has been how to provide an adequate adhesive bond between the existing porcelain and the new composite. The preferred method of creating this bond is micromechanically (e.g. sandblasting with 5 mm aluminum dioxide), micromechanically (e.g. acid etching the porcelain with 9% hydrofluoric acid), and applying coupling agents and resins for better chemical retention that clinically translates into a more predictable porcelain bonding system.
More how-to techniques: How to improve Class II composite restorations
Silanating porcelain restorations prior to adhesively bonding composite materials is extremely important because of the nature of the bond it creates between the porcelain and the composite repair material. This bond is both mechanical and chemical.³ Silane coupling agents function partly by forming “chemical bridges” between two materials (i.e., composite and porcelain), and partly by altering the surface of porcelain with the formation of microporosities.
Microporosities allow bonding agents to infiltrate the internal structure of porcelain restorations to provide maximal adhesion. The longevity and strength of the bonds created depends on the silane coupling agent applied, and the method of application.
Continue to page two for a clinical case...
Clinical case
A 20-year-old female patient presented with eight porcelain restorations that had been placed two years prior. The incisal edge of the veneer on the central fractured during an accident (She was trying to fix the time on her watch). This created an immediate dilemma for the patient, as she was in college far away and didn’t have time to travel back and forth for a replacement. Because of the age of the patient and restorations, the patient decided to do a composite repair to the fractured veneer intraorally.
Procedure
The pre-operative full retracted view of the patient’s fractured restoration (Fig. 1).
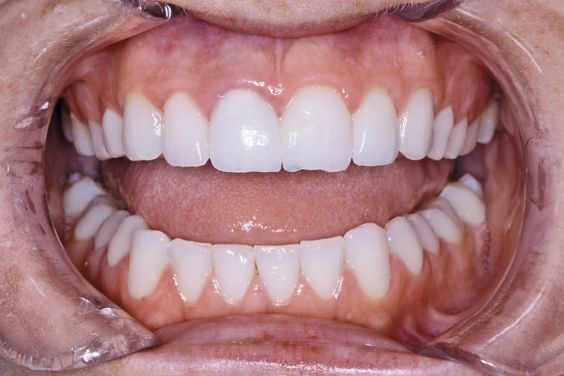
Figure 1
1. The fractured porcelain veneer is air-abraded using aluminum oxide to increase micromechanical retention with the abrasion unit. Restoration was rinsed and dried (Figs. 2 and 3a).
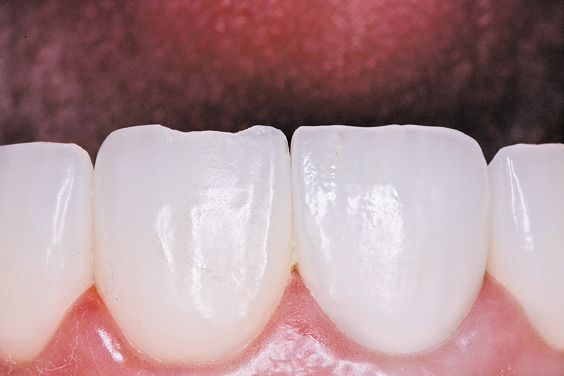
Figure 2
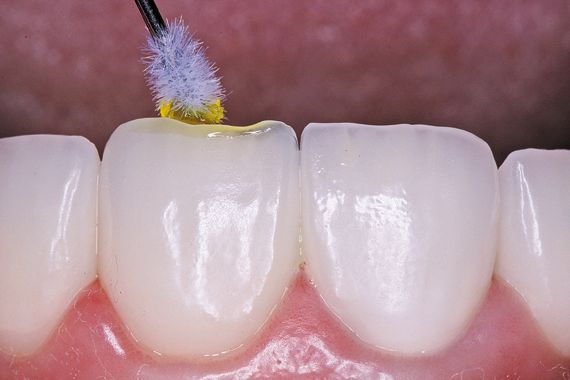
Figure 3a
2. A 9% hydrofluoric acid porcelain etchant (Ultradent Porcelain Etch) is applied to the porcelain veneer (Fig. 3b).
After 90 seconds, the porcelain etchant is rinsed off with a simultaneous mixture of air and water, which is directed toward the porcelain in an incisal direction, away from the tooth and gingival margin. Porcelain Etch is designed for intraoral or extraoral porcelain etching. Use it to etch porcelain or old macro-filled composites prior to bonding and repair.

Figure 3b
3. Ultradent’s Silane is placed on the restoration and allowed to dry (Figs. 4-4a).
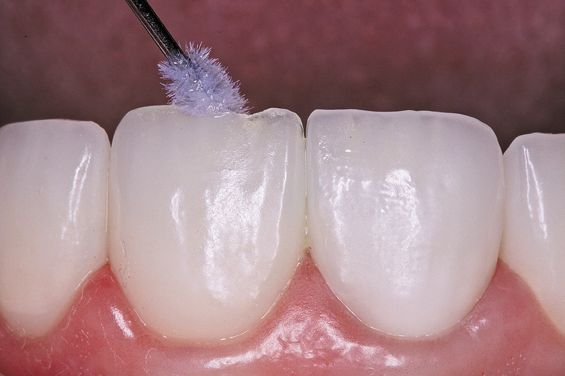
Figure 4

Figure 4a
4. Bonding resin is placed on the restoration iBond (Heraeus), lightly air dried and cured (Fig. 5). Venus Diamond composite B1 body shade from Heraeus was used.
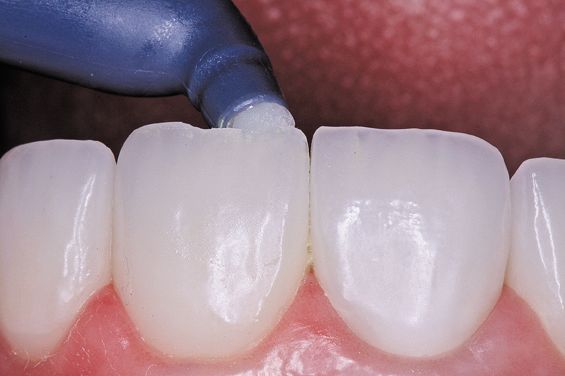
Figure 5
Continue to page three for more...
5. Composite material is manipulated with Ultradent’s Wetting Resin (Fig. 6). Composite Wetting Resin may be placed on the composite surface if it has become dry while contouring the composite. Use Composite Wetting Resin on an instrument or brush to enhance glide. This greatly facilitates adaptation of the composite restoration and preparation.
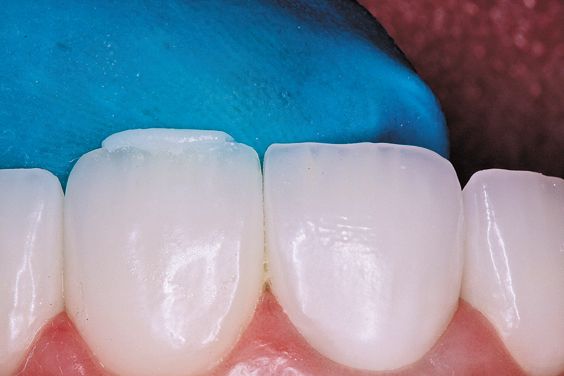
Figure 6
6. The final layer of composite Venus Diamond Clear from Heraeus is added to incisal edge repair (Fig. 7).
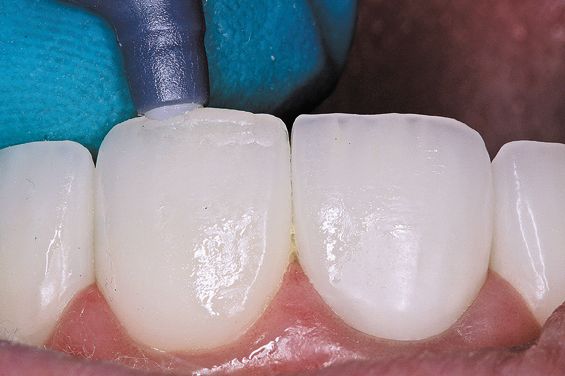
Figure 7
7. The completed restoration was polished with Ultradent’s Jiffy polishing system.
Each bur is used to achieve a high gloss finish (green course, yellow medium, white fine) (Figs. 8a-c).
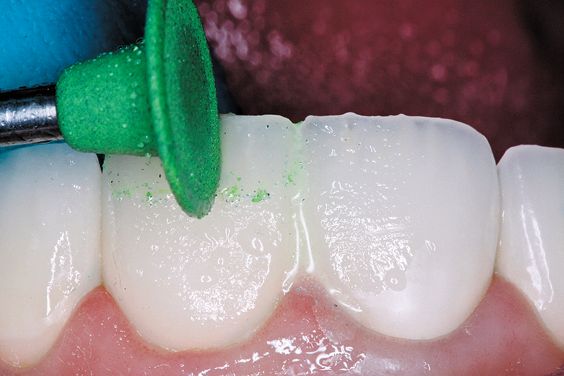
Figure 8a
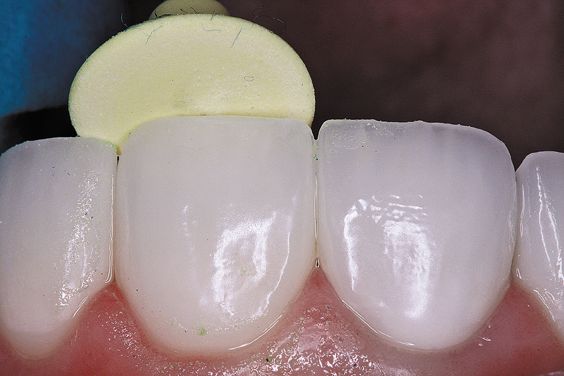
Figure 8b
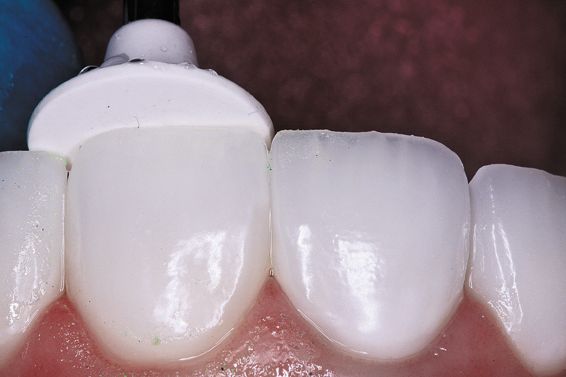
Figure 8c
8. Final polish with Jiffy composite polishing brushes (Fig. 9).
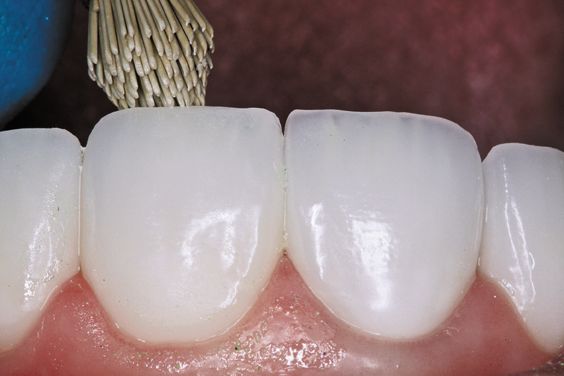
Figure 9
Fig. 10 shows the patient’s final smile after repair.
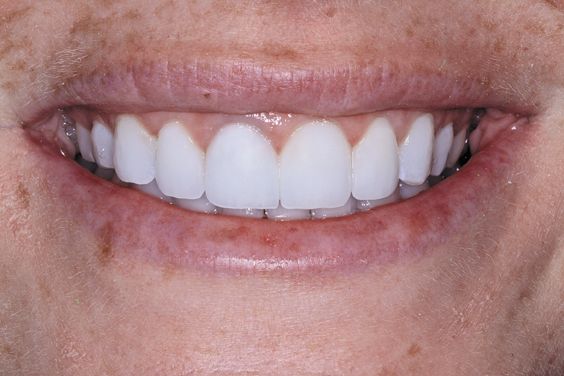
Figure 10
Conclusion
As the number of all-porcelain restorations increases, so too will the need for efficient, reliable intraoral repairs of fractured porcelain. Every time a restoration is removed more tooth structure is sacrificed. This restoration was repaired 3 years ago and still looks like it was placed yesterday.
1.Peumans M, De Munck J, Fiews S, Lambrechts P, Vanherle G, Van Meerbeek B. A Prospective Ten-year Clinical Trial of Porcelain Veneers. Journal of Adhesive Dentistry 2004;6(1):65-762.Fahl N Jr. A Solution for Everyday Direct Restorative Challenges. Journal of Cosmetic Dentistry 2010;26(3):573.Calmia JR, Simonsen RJ. Effect of coupling agents on bond strength of etched porcelain. [Abstract] J Dent Res 1984;163:179.4.Antonucci JM, Dickens SH, Fowler BO, et al. Chemistry of silanes: interfaces in dental polymers and composites. J Res Natl Inst Stand Technol 2005;110(5):541-558.5.Barghi N. To silanate or not silanate: making a clinical decision. Compend Contin Educ Dent. 2000;21(8)659-62,664;quiz