Approaches to Aerosol Reduction
Updates on the technology and the science behind reducing aerosol risks in a dental practice.
©Blickfang / stock.adobe.com
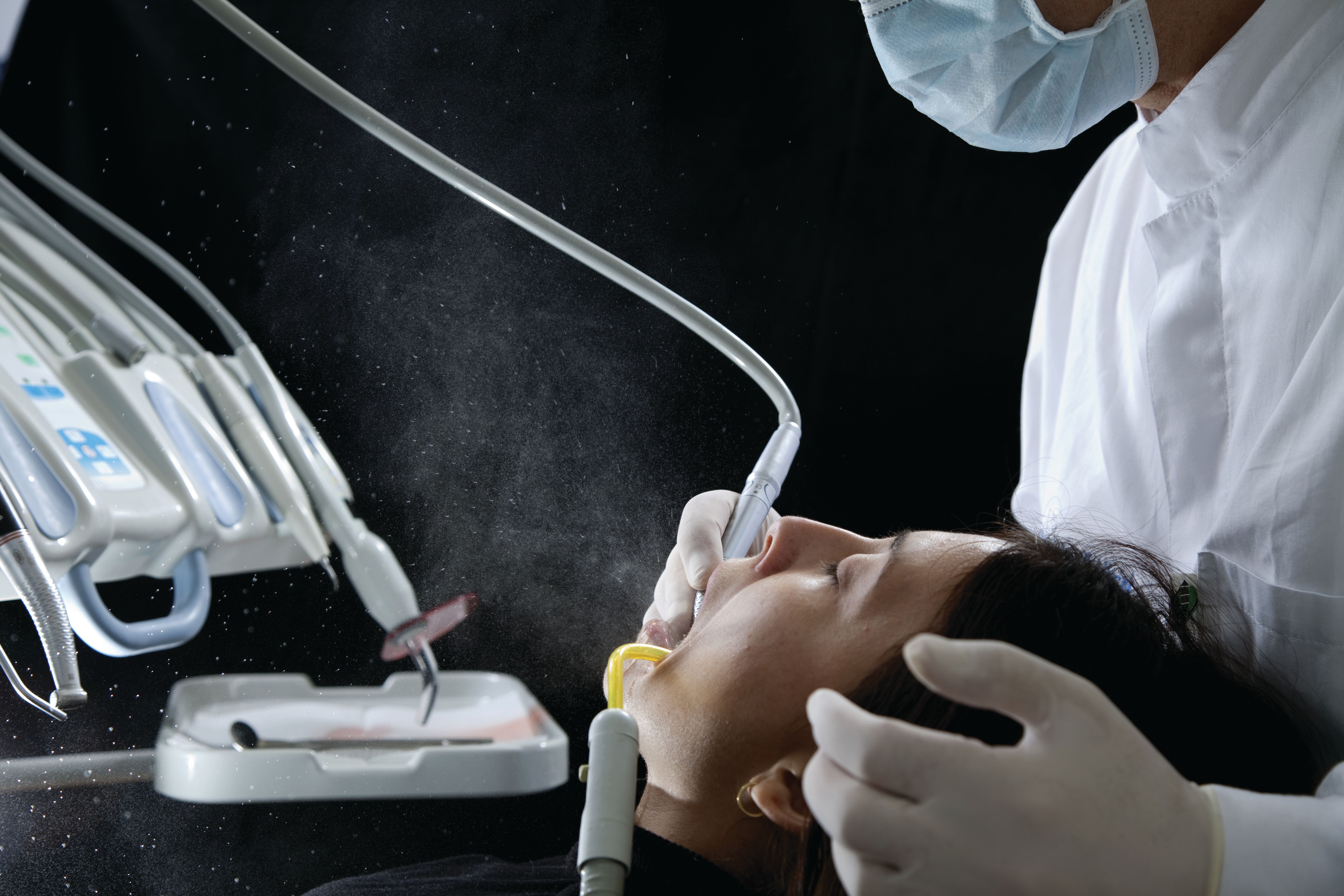
If there were a defining word for the dental industry over the past year, it would be aerosols. As masks are donned and surfaces are compulsively disinfected in the face of the coronavirus disease 2019 (COVID-19) pandemic, aerosols have been front and center.
“I think that at the moment the COVID-19 pandemic has increased everybody’s awareness of aerosols,” says V. Kim Kutsch, DMD, a private practitioner and CEO of Dental Safety First. “Suddenly, we’re looking at aerosols because there’s pretty good evidence that COVID-19 is transmitted that way. So that puts us at obvious risk in the profession since we deal with so many of them on a daily basis. We need to reexamine our attitude toward the aerosol and what we can do to protect ourselves and be able to practice safely.”
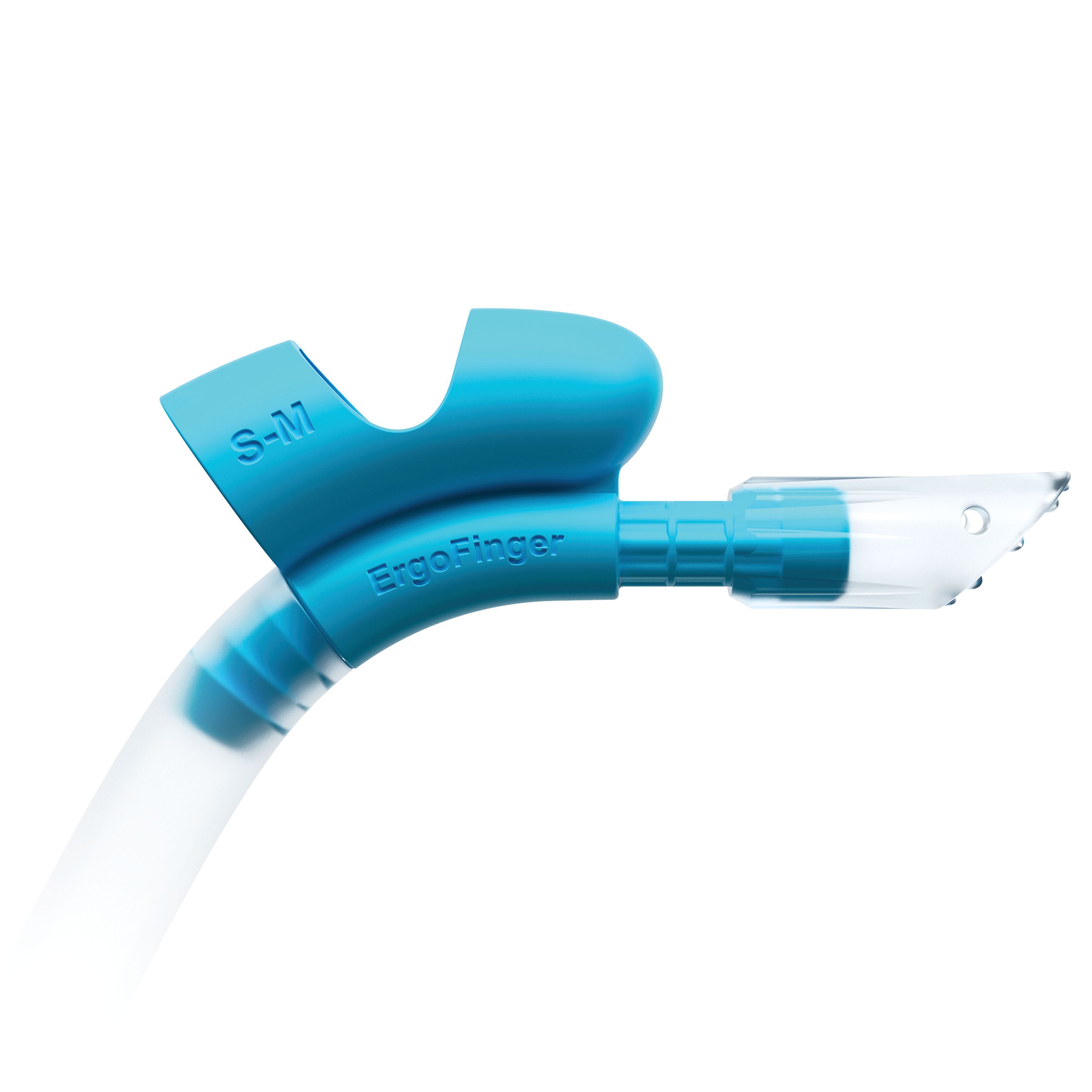
The ErgoFinger HVE attaches to a clinician’s finger, which allows suction to be placed right at the point of aerosol origination.
Mounting evidence has proved that the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) virus is indeed airborne and carried through aerosols. In October, the Centers for Disease Control and Prevention (CDC) launched How COVID-19 Spreads, which outlines how a person with COVID-19 can infect others who are over 6 feet away, or even after the infected person has left the area.
The CDC found that cases of airborne transmission largely occurred in “poorly ventilated and enclosed spaces that involved activities that caused heavier breathing” or other activities that resulted in more airborne virus-carrying particles.1 In regard to health care settings specifically, the agency noted that aerosol-generating procedures required extra engineering controls to prevent occupational transmission of contagious pathogens.2
This puts dentists performing lengthy procedures with high-powered instruments in small, poorly ventilated operatories—essentially a typical day in the dental practice—at great risk.
“You can’t avoid these aerosols in dentistry’s aerosol-generating procedures [AGPs],” says Martin Koch, PhD, head of the technical academy at Air Techniques and Dürr Dental. “You produce these whenever you use a drill, turbine, handpiece, etc. To reduce the risk [involves] a combination of mitigation methods. You can’t avoid it, but you can mitigate the procedures.”
Mitigating the Risks
Since the AIDS epidemic in the 1980s, dentists have relied on standard infection-control procedures including wearing personal protective equipment (PPE) such as gloves and gowns, practicing good hand hygiene, and implementing sharps safety protocols to protect themselves and their patients. In addition, since the arrival of SARS-CoV-2, they have added transmission-based precautions to address airborne aerosols.
“Nobody wore gloves before the AIDS epidemic,” says David Roholt, DDS, the inventor of AeroSol Away. “It changed dentistry forever and standardized PPE across the entire field. Going forward, I think OSHA [Occupational Safety and Health Administration] will mandate transmission-based precautions like aerosol-reduction devices; it’s going to be standard of care for staff safety, and patients are going to look for it too.”
So, what are the best ways to implement transmission-based precautions to mitigate the increased risks created by SARS-CoV-2? A multitiered strategy is the best approach. The CDC and National Institute for Occupational Safety and Health (NIOSH) released the Hierarchy of Controls, a chart in the shape of an inverted pyramid that ranks the level of hazard controls from least to most effective, with the most effective at the top.3
At the bottom of the chart and therefore considered least effective is PPE. Although PPE is undeniably important, it offers the lowest level of protection, according to the CDC and NIOSH.
“Since the onset of COVID-19, dental teams have worn enhanced PPE mainly consisting of N-95 respirators, disposable gowns, face shields, and head coverings,” explains Michele Lash, BS, RDH, a clinical instructor for Dentsply Sirona. “While PPE is a valuable piece in protecting the clinician from hazards, it is most beneficial when the levels above, administrative and engineering controls, are incorporated into procedures.”
The goal of engineering controls is to isolate people from the hazard. This means managing aerosols to limit the dental professional’s risk of exposure. In the dental practice, this could mean the use of a rubber dam or high-volume evacuator (HVE). The combined use of intraoral tools, HVEs, and extraoral aerosol-reduction techniques can greatly mitigate aerosol transmission.
“HVE carries a higher ‘ranking’ than PPE, is crucial to the management of aerosols, and should be a focus of a layered approach,” Lash says.
Intraoral Evacuation
As the first step of engineering controls, intraoral evacuation is an opportunity to remove aerosols before they spread through the air. Using an HVE allows practitioners to capture particles at the source, immediately isolating the hazard. Study results have shown that using an HVE can actually remove 90% to 98% of aerosols arising from the operatory site.4
“The best mitigation strategy is intraoral evacuation,” Dr Koch notes. “Intraoral evacuation with a high flow rate and a sufficient vacuum is the gold standard in mitigation because you remove the aerosol at the source—again, you can’t avoid it, but you can remove it at the source—and if you can remove it then it is a noncontamination strategy,” he says.
When evaluating vacuum systems, Dr Koch recommends the use of oil-free technology. Although most dental air compressors are now oil-free, many vacuums still use outdated technology that can push oil vapor into the compressor air intake, sending it directly into the patient’s mouth and potentially damaging expensive handpieces. One oil-free option is the Mojave, a dry-vacuum system from Air Techniques. Mojave produces high-suction power, key to managing aerosols in the practice.
“For vacuums, make sure the technology is robust and produces not only high negative pressure but also high flow rates,” Dr Koch recommends. “Often, vacuum technologies are only able to provide high value of one or the other. The Mojave has high flow rates that, along with proper HVE techniques, capture more aerosols when performing dental procedures, thereby reducing the amount of aerosols that can escape the oral cavity.”
The Mojave V5 vacuum system from Air Techniques has a high flow rate that supports up to 5 simultaneous users.

Koch is right to be concerned about flow rates. A high flow rate and sufficient suction are critical to the efficacy of intraoral evacuation. If a low-volume standard saliva ejector is used or HVE doesn’t have sufficient suction, it won’t be effective. Results of a pilot study from Dr Koch found that from a flow rate of 300 l/min {10.6 SCFM}, the particle emission can be reduced below the detection limit during preparation with a turbine.5 Additionally, results of studies conducted prior to the emergence of SARS-CoV-2 found that using an HVE with a bore opening of 8 mm or larger during AGPs resulted in a 90% reduction compared with low-volume counterpart.6
“Before COVID-19, most dental hygienists used low-volume suction options such as a standard saliva ejector when performing an AGP,” Lash says. “Many clinicians have not used HVEs routinely since dental school, so there’s been a learning curve in adopting aerosol-reduction devices.”
According to Lash, many clinicians may be struggling to adjust to HVE protocols, including the management or weight of the hose, proper placement, or establishing a grip with their nondominant hand. As proper protocol is critical to HVE success in reducing aerosols, newly reintroduced HVE users should look for products featuring lighter-weight hoses, a mirror, or ergonomic angles.
For practitioners who are particularly concerned about ergonomics, there are now alternatives to the traditional HVE. Tools such as the finger-mounted ErgoFinger are available and help reduce unnecessary twisting of the wrist or bending of the neck. Because the HVE tip is attached to the clinician’s finger, it allows suction to easily be placed right at the point of aerosol origination. The nozzle bore size of 11 mm reduces the amount of aerosol arising from the operatory site and simplifies 2-handed dentistry, eliminating added craning or reaching.
“The main reason we developed this product was that we clearly needed something ergonomically better than the normal solutions,” says Becki Cole, RDH, CEO of ErgoFinger USA. “The tip moves 360 degrees, so you can easily change the position and keep really close aerosol control. It also has a lightweight hose, so there’s little to no drag.”
Extraoral Aerosol Reduction
Although HVE and intraoral aerosol reduction are critical, some aerosols will inevitably escape the area immediately around the patient’s mouth. A second line of defense is needed.
“Current protocols like PPE, HVE, and increased ventilation just aren’t enough,” Dr Kutsch says. “We need to add another layer of protection in conjunction with these.”
This can come in the form of a high-efficiency particulate air (HEPA) vacuum positioned in front of or next to the patient to catch any expelled aerosols missed by the HVE. Chairside extraoral vacuum HEPA filters suck in air and push it through a dense HEPA filter, removing aerosolized particles such as viruses, bacteria, dust, and other pollutants. Testing on the efficacy of HEPA filters against SARS-CoV-2 is still under some debate, but results from a NASA study showed that HEPA filters are most efficient at capturing ultrafine particles as small as 0.01 μm.7 As the SARS-CoV-2 virus is approximately 0.0125 μm, it falls within the particle range of HEPA filters.
This technology has been integrated into devices such as the Dental Aerosol Extractor (DAX) from Dental Safety First. A chairside unit, the vacuum is positioned in front of the patient’s face. High air speed through the nozzle helps catch pollutants, before being slowed through the HEPA filter for a maximum filtration of particles from 100.0 to 0.01 μm. These speeds are critical, as the vacuum must have enough velocity at the opening to catch the aerosols leaving the patient’s mouth at a high speed—potentially, Dr Kutsch says, up to 28 to 45 mph.
The DAX captures pollutants through its high–air speed nozzle and filters them through a HEPA Filter.

“This means your vacuum has to be at least 50 mph to catch that aerosol,” he explains. “But you want to slow the air over the filter to catch the virus particles. So you have to slow the air down to 0.06 mph over the filter, otherwise they are pushed through. That’s obviously a challenge, but DAX is a NASA-based optimized system, so it’s very effective at it.”
One criticism of extraoral vacuums is that they are just one more noisy thing taking up space in a patient’s view, which can make them nervous or claustrophobic. During his practice’s shutdown at the beginning of the pandemic in 2020, Dr Roholt decided he needed to come up with a less obtrusive version of extraoral aerosol reduction that could also be placed closer to the source for increased efficacy.
“The farther from the source you are, the more the effectiveness of the vacuum decreases with the square of the distance,” he explains. “If you’re 1 inch away, you need 100 CFM [cubic feet per minute], but 10 inches away, you’ll need 1,000 CFM in order to have the same effect. By positioning a vacuum cone on either side of a patient’s face, you can be just 2 inches away.”
This sparked the invention of AeroSol Away, a mounted vacuum positioned on either side of the head of the dental chair. By having the vacuum immediately surrounding the patient’s face, it can be on at a lower rate, reducing the noise it produces. Eventually, Dr Roholt says, he sees all dental chairs having AeroSol Away or a similar device built in as an extra line of defense against the aerosols generated during treatment.
“We still use all of the intraoral devices that we’ve always used—rubber dams, high-volume suction, drives—everything that we did before, we are still using it,” he explains. “We’ve just added AeroSol Away, because it doesn’t interfere with us using anything else but helps us protect ourselves further. I think it’s critical to get options like this in an affordable manner so every dentist can have one and make it safer for their staff and themselves.”
The Future of Aerosols
The combined strategy of intra- and extraoral aerosol mitigation seems to be the best bet for increasing safety in the dental practice. The expanding market of HVEs and vacuums—and increased demand—in the past year has been a testament to practitioners’ dedication to keeping their team and their patients safe. The technology will continue to improve, lowering transmission rates and upping peace of mind. Research and development of aerosol-management technologies will continue well into the future, Lash believes, with companies focusing on capturing aerosols at the point of contact, ergonomic enhancements, and improved ease of use.
“Returning to old habits such as using low-volume evacuation out of convenience is not an option,” Lash says. “Rather, we need to find a balance between providing the evidence-based therapies we know are beneficial for our patients to receive while integrating a multilayered strategy to address aerosol containment. We should not practice in fear of risks but be mindful of the hazard control systems that have always been in place to minimize our risks.”
Dr Roholt and Dr Kutsch agree that aerosol containment and the use of aerosol-reducing technology isn’t going anywhere anytime soon, even when the pandemic dies down.
“I think this is going to be standard practice,” Dr Roholt says. “I think we just have to [accept that we’ll] have to have some type of aerosol-reduction device in place and utilize it all the time.”
Where things stand now, further adoption of these technologies must continue, and more research into the efficacy of various aerosol-reducing systems needs to take place. But Dr Kutsch thinks the dental industry is on the right path.
“I’m really proud of our profession and the steps we’ve taken to up our game against aerosol transmission,” he says. “You see that there haven’t been any outbreaks traced to a dental practice in the United States. I think it speaks to the fact that we’ve taken the extra steps to prevent that and to the measures to protect ourselves and our patients as much as possible.”
References
- How COVID-19 spreads. CDC. Accessed January 4, 2021. https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/how-covid-spreads.html
- Scientific brief: SARS-CoV-2 and potential airborne transmission. CDC. Accessed January 6, 2021. https://www.cdc.gov/coronavirus/2019-ncov/more/scientific-brief-sars-cov-2.html
- NIOSH. Hierarchy of controls. CDC. Accessed January 3, 2021. https://www.cdc.gov/niosh/topics/hierarchy/default.html
- Harrel SK, Molinari J. Aerosols and splatter in dentistry: a brief review of the literature and infection control implications. J Am Dent Assoc. 2004;135(4):429-437. doi:10.14219/jada.archive.2004.020
- Koch M. Aerosol reduction by means of an intraoral spray mist suction—the first findings from an experimental pilot study." https://www.airtechniques.com/en/aerosols-protection/
- King TB, Muzzin KB, Berry CW, Anders LM. The effectiveness of an aerosol reduction device for ultrasonic scalers. J Periodontol. 1997;68(1):45-49. doi:10.1902/jop.1997.68.1.45
- Perry JL, Agui JH, Vijayakimar R. Submicron and nanoparticulate matter removal by HEPA-rated media filters and packed beds of granular materials. NASA Technical Reports Server. Accessed January 6, 2021. https://ntrs.nasa.gov/search.jsp?R=20170005166
