How to restore dental decay with KaVo Kerr materials
How one dentist ensures success with one-step bulk fill composites.

Restorative dentistry and the removal of caries remain the essence of dentistry. The combat of caries disease in the posterior region is one aspect of dentistry that hasn’t changed much in theory - remove all the diseased tooth structure and replace it with a material comparable to that which was lost.
Modern advances in this field have helped us provide our patients with increasingly better results. While the preparation style of decay removal has become easier and more conservative - no more extension for retention or prevention - its concept hasn’t changed. One could argue that technology has made our life easier by aiding us in the process with caries visualization tools and dyes and more specialized burs and handpieces, yet the process remains the same. The restoration process has simplified and allows dental practitioners to restore missing tooth structure with ease and confidence. Placement ease has saved not only time and money but has also allowed us to confidently restore the tooth without fear of immediate or later failure.
Single component self-etch dental adhesives provide excellent adhesion for direct composite placement with an easy-to-follow and reproducible application technique, which in itself is generally more desirable than the multi-step systems we used to struggle with. No more complex step sequences with etching, rinsing, priming and bonding. That being said, no post-operative sensitivity or water residue issues - a problem that leads to delamination - have been reported, with the newest generation of these self-etching adhesives.
Trending article: 5 tips for infection control precatusions during flu season
One-step bulk fill composites available today1allow bulk placement without fear of missed adaptation, incomplete cure, inadequate polish, or esthetics. With the advent of these new composites, our task has yet again been simplified.
In order to be successful, it’s extremely important for clinicians to strictly abide by the manufacturer’s recommendations, adhere to the correct sequence of steps, and observe the proper application and placement steps. In my practice, I use materials from the same manufacturer’s line together, which have been tested together to achieve the best results.
Case study
A 25-year-old female presented to the office with complaints of staining on her posterior teeth and sensitivity to sweets. Upon clinical and radiographic exams, decay was diagnosed in the occlusal grooves of most of her posterior dentition.
The following treatment sequence depicts one quadrant of her restorations. The teeth addressed were teeth #18-21.
After local anesthetic was administered, all visible decay was removed (Fig. 1) and, following the latest Dental Caries 2018: New Insights recommendation, all “affected” dentin layers were also removed. The preparation was disinfected with 5 percent gluteraldehyde-35 percent hydroxylethyl methacrylate (HEMA) formulations applied with Ball-Point Applicators™by KaVo Kerr.
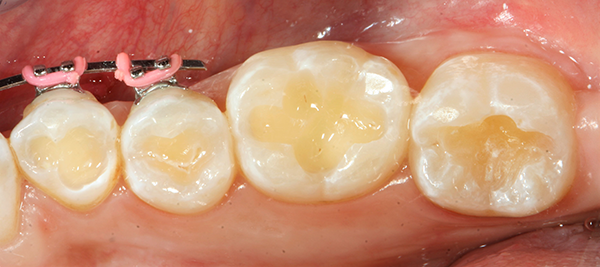
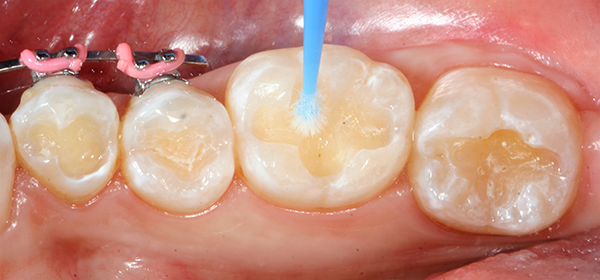
Fig. 1 Fig. 2
After the two separate one-minute applications of disinfectant, the restorations were suctioned to achieve a damp surface.2 This step was followed by the application of OptiBond™ All-In-One self-etching dental adhesive by KaVo Kerr with Ball-Point Applicators (Fig 2 ).
Read more: Tips and tricks for creating long-lasting restorations
I used OptiBond All-In-One self-etching adhesive because it combines the ingredients needed for etching, priming and bonding into a single adhesive solution, thereby eliminating separate etching and priming steps of the bonding process.3 It’s extremely easy to use and its bond strength is consistent. I’ve had no reports of post-operative sensitivity using this bonding method.
Using the Ball-Point Applicators, I applied a generous amount of OptiBond All-In-One adhesive to the enamel/dentin surface. I scrubbed the surface with a brushing motion for 20 seconds, and then applied a second application of OptiBond All-In-One adhesive with a brushing motion for 20 seconds. I then dried the adhesive with gentle air first and then medium air for five seconds with oil-free air, and then light cured for 10 seconds with the Kerr Demi™ Plus Curing Light (Fig. 3).
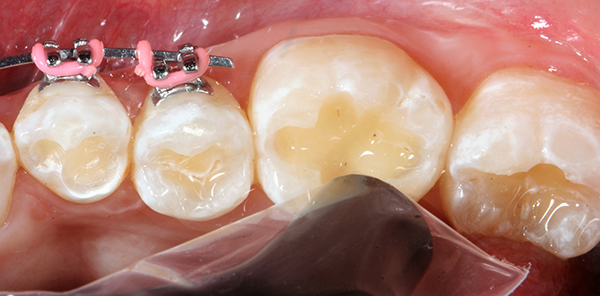
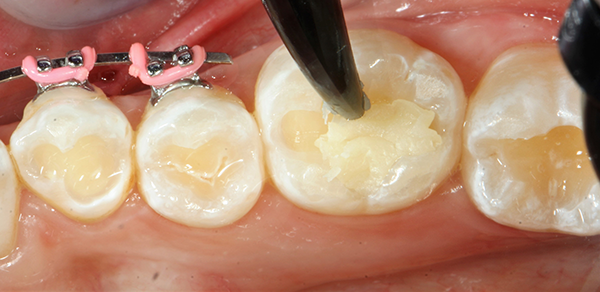
Fig. 3 Fig. 4
I then filled the preparation with bulk fill composite (Fig. 4). The composite of choice for this case was SonicFill™3 (Kerr), which is a sonic-activated bulk fill composite.
Continue reading on page 2...
SonicFill 3 replaces conventional time-consuming, multi-stage layering techniques used with other composites while providing improved adaptation. It’s easy to handle, sculpt and polish as well as simple to extrude with a specialized handpiece (SonicFill Handpiece, Kerr) during placement.
I chose this material because it provides better adaptation to margins and internal walls. SonicFill 3 contains rheological modifiers that react to the sonic energy applied during placement, reducing viscosity to increase flowability to all cavity surfaces. Most cavities are filled in seconds.
The low shrinkage stress this composite provides ensures lasting marginal integrity. Lower shrinkage stress can lead to void- and gap-free procedures and better outcomes.
Its optimized formula is slump-free. Once the sonic energy is removed, the composite reverts to a viscous, pliable state ideal for contouring and polishing. The nano-scale zirconsil (zirconium oxide + silica oxide) filler system allows the practitioner to achieve excellent gloss, wear resistance and reliability.
Related reading: 3 ways glass ionomers are changing restorative dentistry
SonicFill 3 also has a high depth of cure. Refractive index matching and an enhanced curing mechanism allow polymerization depths up to 5mm in a single step, while still retaining opacity for esthetically-pleasing finishes.4
Composite sculpting was achieved with a generic composite instrument (Fig. 5). All restorations were then cured with the Demi Plus curing light for 40 seconds each (Fig. 6).
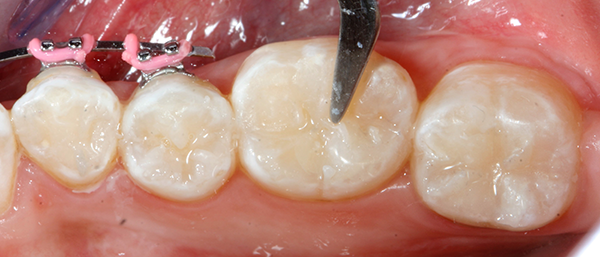
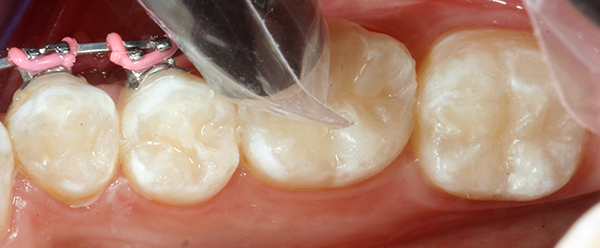
Fig. 5 Fig. 6
Occlusion was checked with articulating paper (AccuFilm®, Parkell) (Fig. 7) and adjusted as needed with a finishing bur (Fig. 8).
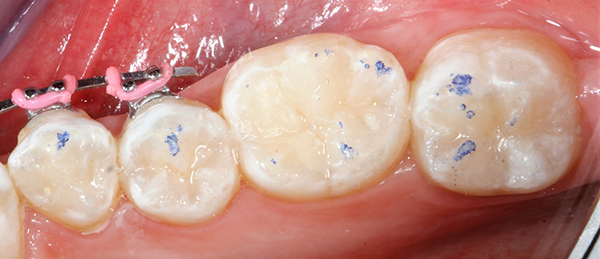
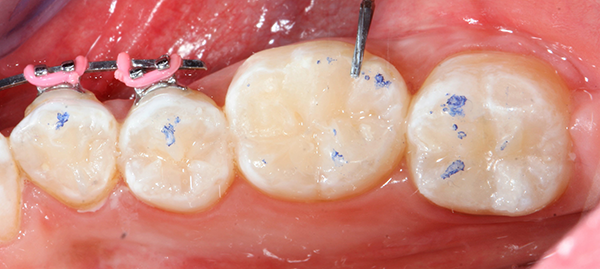
Fig. 7 Fig. 8
As one can observe from the pictures, when anatomy is closely followed in the reconstruction of the missing tooth structure, necessary occlusal adjustment is very minimal.
Final polish was achieved with a Kerr ProGloss™polisher (Fig. 9). ProGloss polishers are a one-step polishing system for all types of composite restorations. With the ProGloss polisher, one can achieve a faster, higher surface luster in one simple procedure, as seen in Figure 9.
The case was completed and the patient was very happy with the beautiful results, indistinguishable from her surrounding natural dentition, even with great magnification (Fig. 10).
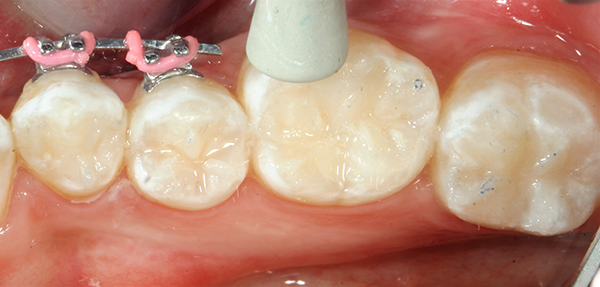
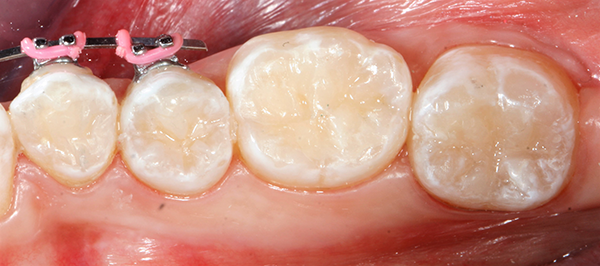
Fig. 9 Fig. 10
Conclusion
Restorative dentistry has become easier to achieve with the advancement in reliable self-etch bonding and composites that blend in seamlessly with the surrounding tooth structure.
As all of you surely do, I look forward to the new advances that modern technology and science will provide in dentistry to potentially further simplify this basic yet necessary dental treatment procedure.
