Periodontal Priorities: The Diagnostics and Treatment Changing Perio Care
How diagnostics and preventive measures are fueling periodontal treatment acceptance among patients.
©Alexandr Mitiuc/Shutterstock.com
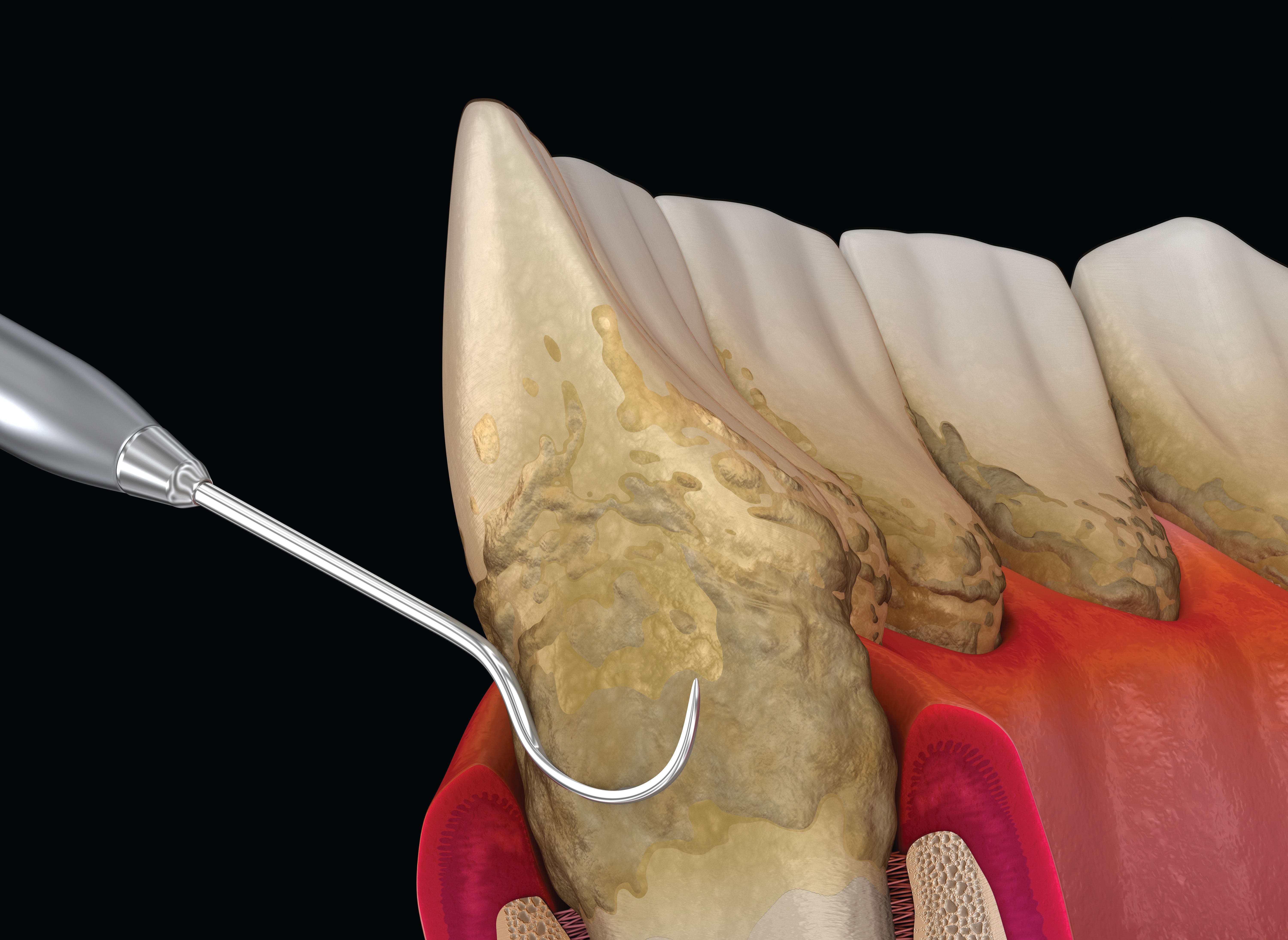
When it comes to education about periodontal disease, patient acceptance and adherence have been inconsistent. Perhaps the biggest challenge in treating periodontal disease is convincing patients that they have a disease. The Centers for Disease Control and Prevention (CDC) reports that 47.2% of adults have some form of periodontal disease.1 However, many of these patients do not believe they have a problem.
With so many individuals disregarding oral health—and emerging research on the links between periodontal disease and serious systemic health issues—periodontal disease is becoming a national health crisis. If only, practitioners mused, there was something that created national awareness about an asymptomatic disease that could easily enter your body without you knowing it but cause life-threatening problems. If only the breaking story of the year involved such a potentially fatal disease that could present without pain or symptoms. If only there were identified risk factors that could predict whether someone had a higher possibility of contracting the asymptomatic disease. Enter coronavirus disease 2019 (COVID-19).
Perio Care in a Pandemic
The past year has thrust just such a disease into the spotlight. Although periodontal disease and COVID-19 differ immensely, the parallels can be valuable educational tools.
“This is our opportunity to utilize this as an educational piece for our patients,” says Katrina Sanders, MEd, BSDH, RDH, RF. “I’m not saying let’s lean into the fear our patients have about this disease process—that’s not it at all. But let’s draw parallels to help them understand how periodontal disease can have serious repercussions even if it doesn’t hurt.”
Education is critical because periodontal care during the pandemic presents numerous challenges. Patients who delayed dental care during shutdowns or because of concern about the virus are returning to practices and often presenting with increased calculus following the interruption in care. As a result, the risk of inflammation is elevated. Add habits instituted by pandemic life (such as increased alcohol and tobacco use or poor dietary considerations) and high levels of stress (an etiologic factor that increases cortisol and inflammatory conditions), and the perfect environment for oral health issues has been created.
“Oral hygiene status has been poor,” says Sanders. “In addition, ‘mask mouth’ dries out the mouth and makes people more prone to periodontal disease. And a lot of patients are working from home now—they wake up, hop on a Zoom call, and they aren’t going to really be seen by anyone, so maybe they skip brushing their teeth. So, we’re starting to see these patients come in and they are a challenge.”
In addition to educating patients, practitioners need to be aware of their own focus on perio treatment. As practices reopen, dentists are focused on setting up schedules and resuming business. Hygienists must spend time comforting patients who are nervous about COVID-19 risks in the practice and becoming acquainted with new personal protective equipment and tools such as high-speed evacuation systems. But dedication to perio cannot be neglected, particularly because periodontal disease could be linked to COVID-19.
The Oral-Systemic Link
A recent study found enough evidence to suggest that periodontal disease is a risk factor for COVID-19, because diseases such as diabetes, obesity, and cardiac conditions, all of which are linked to periodontal problems, are comorbidities that are common risk factors for COVID-19.2
“During the time when periodontal disease is ongoing, there is a huge inflammatory burden on the rest of the body,” says Mia Geisinger, DDS, MS, associate professor and predoctoral periodontal program director at the University of Alabama at Birmingham School of Dentistry, and a diplomate in the American Board of Periodontology (ABP). “We have a unique opportunity right now to reach our patients and to talk about the important work that we do to manage and address chronic inflammatory disease that can create similar inflammatory burden, cardiovascular disease, diabetes, and obesity.”
As a result of these comorbidities, Sanders says, evaluating, managing, and optimizing patients’ immune response is critical in the current health crisis.
“There’s so much research coming out about how if we have inflammation in our body associated with oral disease, it can elevate our risk for SARS-CoV-2,” says Sanders. “Periodontal disease is one of the only bacterial diseases in the body that we’re really leaning on to the host response to be able to fight this inflammatory condition. By rendering patients healthier, we can reduce the burden on the immune system or the amount of inflammatory condition my patient has. This could be a huge key to help control how this disease is spreading.”
Although research has linked periodontal disease to numerous conditions in addition to COVID-19 (including heart disease, cancer, respiratory disease, and osteoporosis), it was believed until recently that only bacteria were to blame. According to the ABP, however, inflammation is a critical factor. Perhaps one of the silver linings of the pandemic has been a refocusing of attention on low-grade chronic inflammatory conditions that are endemic to the adult population, such as diabetes, prediabetes, dysglycemia, obesity, and, critically, periodontal disease.
“Inflammation is the big keyword, and there’s quite a bit of inflammation when someone has periodontal disease,” says Robert Levine, DDS, a board-certified periodontist and diplomate of the ABP practicing in Philadelphia, Pennsylvania. “As a profession, we need to take very seriously that the mouth is connected to the body and the systemic links.”
With such close links to other inflammatory conditions, periodontal disease and the resulting inflammation are nothing to dismiss, considering they affect nearly half the US adult population. “One of the learnings that we can take away from the COVID-19 pandemic is that individuals who had inflammation associated with periodontal diseases tended to have higher rates of hospitalization and higher morbidity and mortality rates when compared to other individuals that were matched for other morbidities,” Dr Geisinger says. “It really hammers home that point that oral health is so tied to overall health and even in our body’s ability to respond to these exogenous infections.”
This correlation between oral and overall health has not always been acknowledged. For many years, the focus of periodontal care was on removing biofilm, root planing, and scaling, with little regard for soft tissue involvement, inflammation, or potential bacterial contamination. The growing understanding of oral-systemic health, Sanders believes, caused the dental community to reevaluate.
“We began to see a paradigm shift. It wasn’t simply how well you could root plane or smooth the tooth surface, but how you are treating the soft tissue,” says Sanders. “What does that treatment look like? Is it laser therapy? Is it some type of air polishing or air abrasion? Is it an antibiotic, an antimicrobial? Essentially, what are we doing from a holistic standpoint?”
Deborah Durako, director of StellaLife, Inc., agrees that oral-systemic health is critical and says the time to act is now. “It’s time for us to really understand how bacteria and inflammation are affecting more than just the mouth. We understand so much more now but we need to continue that big shift toward a total body wellness approach and using our new technology to be able to understand it better.”
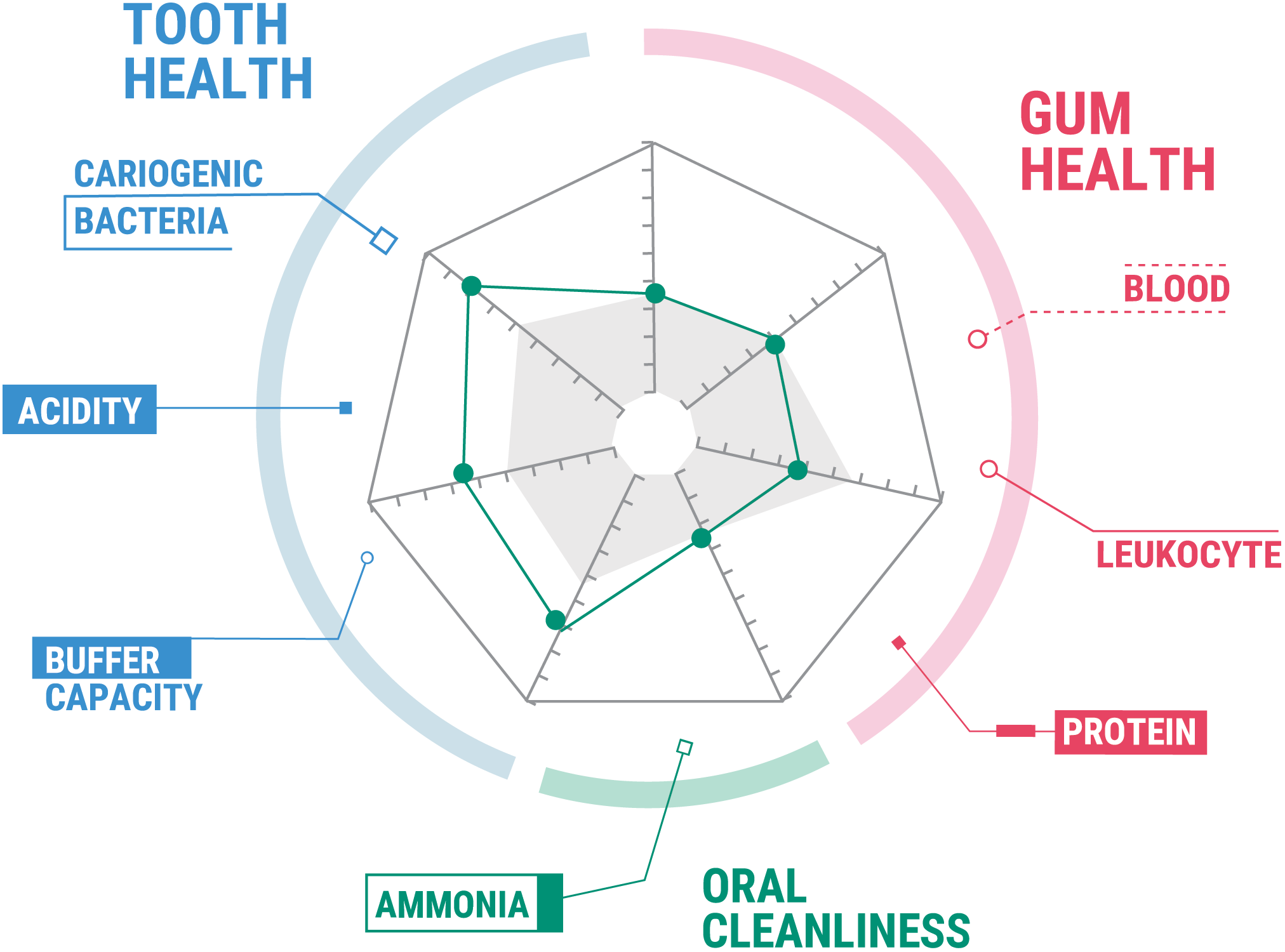
With a small saliva sample, the SillHa Oral Wellness system measures the reactivity on a test strip from the sample and offers insight to activity clinicians cannot see, such as bacteria activity, acidity, and the presence of inflammatory markers. This activity may indicate that the patient is at an increased risk for caries or gum inflammation.
This information has prompted some clinicians to reevaluate how they practice. Barbara McClatchie, DDS, partnered with her husband’s cardiology practice 4 years ago to found Complete Health Dentistry of Columbus in Worthington, Ohio. The combined practices formed the first medical center in the United States with a dentist and a cardiologist under 1 roof practicing the Bale/Doneen Method of care and testing.
In her practice, Dr McClatchie works collaboratively with cardiologist Eric Goulder, MD, to treat the correlations between cardiovascular and periodontal diseases and bring inflammation under control. They instituted full-mouth periodontal charting for all cardiology patients and determined that almost all also suffer from periodontal disease.
“We’re realizing that the mouth is having a significant impact on the overall inflammation of the body, and how it affects the lining of the arteries,” says Dr McClatchie. “We started really seeing the correlations [between] their inflammation of their body and active perio, and it was really consistent. So we have really started referring our dental patients over for screening for cardiovascular disease when we see these high-risk anaerobes.”
Salivary Diagnostics
To detect these anaerobes, Dr McClatchie and her team have turned to diagnostic saliva testing. Saliva testing can help identify the specific underlying pathogenic cause of periodontal issues and even detect periodontal disease in its preclinical phase. Saliva contains antibodies, antimicrobials, enzymes, hormones, and other biomarkers, many of which are also found in blood. This makes saliva a great monitoring device for not only oral health but overall systemic health.
By evaluating bacterial, genetic, microbial, and protein biomarkers, clinicians can make treatment decisions based on facts.3 Evaluating biomarkers can help identify specific problematic bacteria, serve as an early predictor for disease, and help assess potential future health risks.
“What’s really exciting is where dentistry is going with the saliva testing,” says Dr McClatchie. “That’s really one of the first objective tests that dentistry really has. How people treat and chart has always [been] very subjective and can differ from office to office. There’s no real standard of care. But when you have saliva testing you can actually get a starting point and it serves as a record of how well we did.”
The more objective information you have, the better equipped you are, says Dorothy Prahl, product marketing manager at ARKRAY USA.
“The more a practitioner knows about the situation at hand, the better they can treatment-plan for the patient,” Prahl says. “Recent developments in salivary diagnostics, including chairside and in-office units, have improved the quality and validity of screening results, providing critical information to plan the best course of action. Although certain forms of diagnostics tools have been around for many years, the new products utilize advances in technology that help deliver better screening results.”
The development of in-office units has made salivary testing more accessible to practices and can provide results within minutes, eliminating the need to send samples to labs and wait for results. This helps clinicians identify potential problem areas while the patient is in the chair and allows them to provide helpful take-home instructions and immediate feedback, reducing delays and increasing patient participation on the path to better oral health.
One such unit is ARKRAY USA’s saliva analysis tool, SillHa™ Oral Wellness System. This system analyzes saliva for inflammatory markers of blood, leukocyte, and protein (3 things that can indicate increased risk of developing caries and periodontal disease) and provides numerical assessments of each component in a report called mySaliva™. This allows dentists to measure tooth and gum health and oral cleanliness and potentially identify what is happening even before there is evidence of the initial signs of disease.
“Salivary diagnostics have made great strides from the days of just having a test strip to compare against a test grid,” says Prahl. “Screening solutions such as SillHa provide much greater detail in a straightforward, objective format, providing practitioner and patient the pathway to better oral health.”
MyPerioPath from OralDNA Labs is a salivary testing kit that tests for 11 different pathogens that can cause periodontal issues and other systemic health issues. Patients simply swish with the provided sterile saline for 30 seconds and clinicians collect the sample with the provided collection tube.

There are other screening options. Dr McClatchie primarily uses OralDNA® for salivary testing, because she finds it intuitive and easy to use. OralDNA’s MyPerioPath® tests for 11 pathogens that can cause periodontal issues and place patients at increased risk for cardiovascular disease, stroke, diabetes, and other conditions. It can provide early warning of these pathogens so that periodontal treatment can be personalized to the patient.
Although OralDNA does not test for fungal infections, staph, or as wide a range of bacteria as some other salivary testing options, Dr McClatchie finds that its user-friendliness and simple reports are a big help in identifying bacteria and the antibiotics recommended to treat them, particularly for clinicians new to salivary testing.
There is still a lot of room for development in these technologies, and Dr Geisinger is optimistic about where it will go and how it will expand into deeper diagnostics. “I’m very excited about a lot of these diagnostic technologies,” she says. “Particularly the ability to not only look at individual pathogens or individual salivary biomarkers but the ability to look at the way that those factors interact with the hosts and in particular the specific genetic profile of the hosts themselves. I think that’s really exciting. Are we there yet? No. I think we’ll get there, hopefully in my practice lifetime but certainly in the practice lifetime of the students that I teach.”
Treatment Options and Acceptance
As diagnostics expand and noninvasive methods offer more appealing treatment options, the goal is to get patient acceptance and adherence to follow. Providing patients with quantitative results (like those from a saliva test) can help increase patient engagement and encourage best practices. When a case progresses past preventive measures, offering treatment options patients will accept becomes critical.
• Bacterial Management
With COVID-19 creating risks in the dental practice, more dentists have been using antimicrobial and antibacterial products to stem viral transmission. Although the debate rages about the efficacy of povidone-iodine (PVP-I) and chlorhexidine gluconate rinses as an antiviral, their efficacy against bacteria is proven.
A disadvantage of these types of rinses is that they are not selective about whether they kill beneficial or harmful bacteria.
“What we know about iodine and chlorhexidine and other types of antibacterial products is that there’s another side to all of that, which is that they do in fact wipe everything out,” says Durako. “But we don’t want to destroy the good flora. And yet that’s what we’re doing because we’re trying to combat COVID-19, so you want to try to reinstate that good back into the oral cavity as quickly as possible.”
Antimicrobial products such as the all-natural VEGA Oral Care Recovery Kit (StellaLife) specifically targets the anaerobic bacteria that cause periodontal disease and tooth decay. Research performed by StellaLife found that use of VEGA Oral Rinse reduced anaerobic bacterial loads by approximately 50% for up to 3 hours.4
“Imagine if you’re a perio patient and you rinse 3 times a day, long term,” says Durako. “Theoretically, you would have at least 9 hours out of your day that production of those anaerobic bacteria loads is prevented. It’s going to keep the levels low in your system so your immune system can work on the disease process by itself.”
The critical piece is that the product does not destroy good bacteria but instead promotes a more symbiotic oral microbiome versus a dysbiotic oral microbiome, Dr Geisinger agrees.
“In identifying and utilizing mouth rinses—particularly if they’re going to be utilized for a longer period of time, like postoperatively—we need to look at ones that don’t completely eliminate or significantly reduce the overall bacterial load, but ones that target the bad guy bacteria in particular, which are generally facultative or strict anaerobic bacteria,” she says.
When it comes to combating bacteria below the gumline, options such as Perio Protect Perio Trays offer noninvasive solutions. The only periodontal medicine delivery product with clearance from the Food and Drug Administration (FDA), Perio Trays deliver 1.7% hydrogen peroxide gel (a broad-spectrum antimicrobial) into the pockets, allowing healthy bacteria to flourish while destroying pathogenic bacteria. One study found that use of the peroxide gel provided a significant decrease in bleeding on probing for patients who used the trays at least once a day.5
• Intervention Acceptance
Although nonsurgical approaches to periodontal therapy are the first line of defense, sometimes deeper intervention is necessary. But that does not always mean surgery, which patients will often decline. Laser therapy is rapidly becoming a popular alternative.
The PerioLase MVP-7 from Millennium Dental Technologies is a 6-watt free-running variable pulsed Nd:YAG dental laser that offers clinicians the ability to perform less invasive procedures.

Through procedures like the laser-assisted new attachment procedure (LANAP) protocol pioneered by Millennium Dental Technologies, dentists can offer patients less painful, and quicker, healing alternatives to invasive surgery, with no cutting or sewing.
“The buzz term of noninvasive or nonsurgical is really an impactful 1 because, now more than ever, patients don’t want to spend a lot of time in the dental operatory,” explains Sanders. “Clients are very aware and educated about the fact that lasers can make something easier and noninvasive. So, it creates patient acceptance and I think that makes lasers very important and impactful.”
With fast healing times, less pain and more successful treatment, the LANAP protocol has become popular with clinicians and patients. The LANAP=LAR FDA-cleared laser treatment is the only research-proven, evidence-based method of achieving periodontal regeneration, gum tissue reattachment, and new bone growth.
“If someone has the choice between coming in for a surgical flap treatment or having a laser treatment when they’ll be out in an hour, that’s a no-brainer,” says Dr Levine. “I’m so excited to see the changes with using LANAP. We’ve had really good patient-reported outcomes. We’re able to do the entire mouth when they come in, and 90% of our patients had little to no discomfort immediately after the Novocain wore off, which is incredible; you couldn’t do that with periodontal surgery.”
In addition to at-ease patients and reduced postoperative discomfort, LANAP clinicians reported satisfaction with overall treatment success in a 2020 survey co-authored by Dr Levine. The surveyed clinicians said they found that LANAP treatments were cost-effective, had a high patient acceptance rate, yielded consistent tissue regeneration and better tissue response, and took less time than traditional osseous or guided tissue regeneration surgery.6
Other techniques such as the BIOLASE REPAIR Perio protocol are also seeing success, with significantly better patient-reported outcomes. A recent study found that the REPAIR protocol laser procedures were comparable to Minimally Invasive Surgical Technique (MIST) treatment and as effective as such open flap procedures within clinical parameters.7
• How Numbers Can Help Acceptance
The numbers game can be a real motivator. Whether tracking weight loss or cholesterol points, people like having a starting point and being able to monitor their progress. That mentality extends to oral health.
“I think having data helps patients own their problem,” says Dr McClatchie. “For example, when you’re taking an actual saliva sample and showing them their results, then it becomes like a game because you start chasing your numbers as you see your markers go down.”
Prahl has also seen that patients react well to data they can understand, rather than just recommendations of ways to reduce inflammation. “Only so much can be done while the patient is in the dental chair,” says Prahl. “Adherence to the home care treatment plan is vitally important to improvement of the patient’s condition. The patient needs to better understand what is happening in their mouth and how they can positively affect their own oral health. With mySaliva™ reports, the practitioner can customize comments and insights to make the home care instructions meaningful for each patient, as well as print a copy of the report to take home for reminder and motivation. Results can be compared over time in this report, which can be a powerful motivator for adherence.”
In 2014, Preston Miller, DDS, and Mark McEntire, DMD, spearheaded the Miller-McEntire Periodontal Prognosis Index (MMPPI). Their research found that the periodontal prognosis of molars could be calculated using an evidence-based scoring index.8
“The patient can better understand the long-term prognosis of 15 and 30 years,” says Dr Levine, who uses the MMPPI. “Where the MMPPI strength really lies is at translating clinical outcomes, because we have this report card of patient values we can share with them so they understand.”
The MMPPI evaluates the most periodontally involved molar and scores 7 factors (age, smoking, diabetes, molar type, probing depth, furcation, and mobility). These scores are then converted into percentages to determine how successful treatment can be over 15 and 30 years. For example, Dr Levine says, a score of 4 means a patient has a 95% chance of keeping their teeth for 15 years and an 85% chance for 30 years. The goal is for all patients to have a score of 5 or less.
“We’ll take the worst molar—usually it’s an upper second molar because that score is usually the highest—and the score of that molar reflects the whole mouth,” explains Dr Levine. “We can do this in a minute. And then we can go over it with the patient, where they are with their MMPI, steps on how they can bring it down, etc.”
In addition to assessing periodontal health status, the MMPI can present the patient with tips for making lifestyle changes that will improve overall health, as well as the recommended preventive periodontal maintenance.
“In addition to giving the clinician information about gum recession, it’s a very motivational way that we can get patients to accept treatment, which is obviously a win-win situation,” says Dr Levine. “I use it for all patients, not just perio patients. It gives the patients a number to keep in mind. It helps the patient become part of their own therapy; they’ve got to buy into it for it to succeed.”
Perio Improvements
Diagnostics are improving rapidly, but there is still much to come. Advances in salivary testing will provide significant benefits and push forward the development of new treatments. “The ability to screen for additional detail and specific pathogens at chairside will be a benefit to all,” says Prahl. “These future screenings may also look for oral cancer markers and other bacteria that relate to systemic conditions.”
Dr Geisinger sees current diagnostic techniques as just the beginning. “I think we’re still in the nascent stages for some of these more advanced diagnostic techniques,” says Dr Geisinger. “I think, for routine dental care, most of the advanced things that we can do in research really aren’t practical or feasible currently for garden variety treatment. But I think it’s coming.”
As research trickles down into practical application in the dental practice, big advances will be made. “Maybe this is the biggest limitation of perio right now—the fact that we don’t have enough tools in our arsenal,” says Sanders. “And so, we’ve really just been kind of throwing spaghetti against the wall and seeing what sticks. I think there’s opportunity for new technology, and I very much believe in it. I think we need to start moving into that model.”
With advances in diagnostics and technology come advances in treatment and biologic materials. Dr Geisinger says one of the big ones is the burgeoning use of platelet concentrates. In particular, she sees great benefits in altered platelet concentrates that provide particular handling or biologic capabilities that are specific to the individual treatment. Additionally, the use of mesenchymal stem cells for grafting to create true periodontal regeneration offers many opportunities. “Being able to take stem cells from 1 donor and use them in another individual in a clinically relevant way that ensures the grafts that we’re using have live osteoblast progenitor cells—live cells that are capable of regeneration—in them is a really interesting technique,” Dr Geisinger says.
And although advances continue in biologic materials (soft tissue substitutes that can be used for root coverage procedures, growth factors to improve regenerative outcomes, and other regenerative therapies), perhaps the biggest benefit to periodontal and oral health care will be the embracing of oral-systemic health.
“Our mission is to get medicine and dentistry to collaborate together to be better advocates for patients—to not be in their own lanes, but working together and collaborating for our patients,” says Dr McClatchie. “So, I’m hoping that people [who] are interested in oral-systemic connections will start partnering with like-minded medical professionals so we can endorse the work of each other and be true patient advocates.”
References
- Eke PI, Dye BA, Wei L, Thornton-Evans GO, Genco RJ; CDC Periodontal Disease Surveillance workgroup. Prevalence of periodontitis in adults in the United States: 2009 and 2010. J Dent Res. 2012;91(10):914-920. doi:10.1177/0022034512457373
- Pitones-Rubio V, Chávez-Cortez EG, Hurtado-Camarena A, González-Rascón A, Serafín-Higuera N. Is periodontal disease a risk factor for severe COVID-19 illness? Med Hypotheses. 2020;144:109969. doi:10.1016/j.mehy.2020.109969
- Giannobile WV. Salivary diagnostics for periodontal diseases. J Am Dent Assoc. 2012;143(suppl 10):6S-11S. doi:10.14219/jada.archive.2012.0341
- StellaLife. Reduction of Anaerobic Bacteria Case Report Using StellaLife VEGA Oral Rinse. November 21, 2016. Accessed January 2021. https://cdn.shopify.com/s/files/1/0870/0750/files/Reduction_of_Anaerobic_Bacteria_Case_Report___FINAL.pdf?5285783413516810810
- Cochrane RB, Sindelar B. Case series report of 66 refractory maintenance patients evaluating the effectiveness of topical oxidizing agents. J Clin Dent. 2015;26(4):109-114.
- Richman C, Levine RA, Sullivan A, Jiang S, Farber A, Zalewsky J. Perceptions of the LANAP protocol. Decisions in Dentistry. 2020;6(10):18, 21-23.
- Clem D, Heard R, McGuire M, et al. Comparison of Er,Cr:YSGG laser to minimally invasive surgical technique in the treatment of intrabony defects: six month results of a multicenter, randomized, controlled study. J Periodontol. Published online July 2, 2020. doi:10.1002/JPER.20-0028
- Miller PD Jr, McEntire ML, Marlow NM, Gellin RG. An evidenced-based scoring index to determine the periodontal prognosis on molars. J Periodontol. 2014;85(2):214-225. doi:10.1902/jop.2013.120675
