How To Create the perfect emergence profile for dental implant restorations
The Gingival Cuff Link System is a simple, predictable, and time-efficient methodology that benefits both dental professionals and patients.
Adam McCormick, D.D.S., FACS

Dental implants rank among dentistry’s most successful procedures. With many more practitioners placing implants around the world, this type of dentistry has grown incrementally every year.
Given implant therapy’s rather high out-of-pocket cost to the patient, combined with consumers’ increasing knowledge of this treatment modality, patients have high expectations for outcomes. Patients expect their implant restoration to be esthetically pleasing and mimic the natural dentition. Because time is a premium for all stakeholders, patients want their treatment completed in as few appointments as possible, an objective the clinical team shares.
One area that is critical to the esthetic and functional outcome yet sometimes receives less attention is the formation of the gingival tissue, or emergence profile, created during the healing phase. Most implant manufacturers provide circular titanium or titanium alloy healing abutments, so the gingival tissue forms a circular channel to receive the final crown/restoration.
Which natural teeth emerge from the bone and through the soft tissue in a completely spherical manner? None, of course-each tooth has a unique geometry and emergence profile appropriate for its location in the arch. Some implant companies have created flared healing abutments to improve the emergence profile, but once again, the soft tissue channel that is created is uniform circumferentially and not ideally matched to the tooth being replaced. These healing abutments also do not lend themselves to chair side customization, which is necessary in a high percentage of cases to produce an optimal emergence profile.
An absence of proper emergence profile can have clinical implications. First is the risk that the dental laboratory creates a restoration that matches the spherical geometry created in the soft tissue. This can result in the “popsicle on a stick” crown form, which creates undercuts and food traps for the patient.
If the lab does produce a more natural emergence, the restoration is unlikely to passively fit in the tissue geometry that was formed. This can impinge tissue or require a secondary soft tissue procedure, increasing chair time and patient inconvenience. Ultimately, there is the risk of the restoration not properly seating on the implant. Secondly, a lack of matched emergence profile between the restoration and soft tissue may result in tissue recession over time and deterioration of the esthetic result.
Although it is possible for the clinician to create an anatomically correct custom healing abutment for the site using temporary abutments and restorative materials, this is time-consuming and lacks predictability. One innovative solution involves off-the-shelf custom healing abutments, Gingival Cuff Links from GCL Systems. The brainchild of an oral and maxillofacial surgeon and a general dentist who wanted to improve soft tissue management in implant dentistry, Gingival Cuff Links have changed how I practice.
This product not only addresses the soft tissue but also helps maintain the bone graft, especially in immediate implant placement. Anecdotally, this technology has reduced pain for my patients undergoing a procedure that before required some sort of narcotic, but now involves just a few OTC acetaminophen or ibuprofen tablets.
In my practice, when a molar tooth requires extraction and there is an ability for an immediate implant placement, this technique offers a predictable way to obtain ideal bone and soft tissue healing and decrease bone loss and pain.
I have also noted the practice-building potential as patients discuss with friends and neighbors how they had just one appointment for a tooth extraction and implant placement, with little to no pain. For practitioners who are specialists, it helps general dental colleagues create the ideal emergence profile for a customized abutment and crown. The following example illustrates the technique.
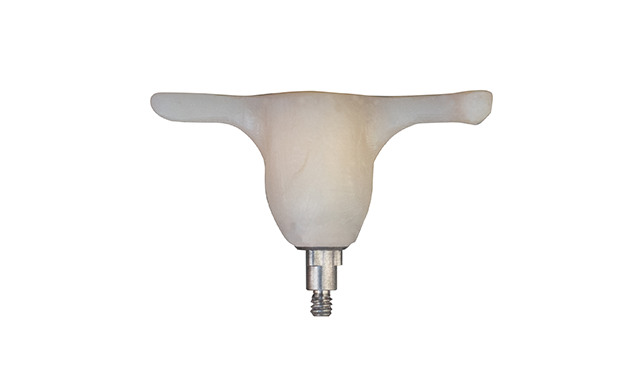
Gingival Cuff Links™
- Fully customizable healing cuffs
- Maintains and sculpts gingival soft tissue
- T-handle design assists doctors in aligning the implant in the correct position
- Compatible with most implant systems
GCL Systems833-425-4346 | gclsystems.com
