Dental Composites Continue to Transform Clinical Dentistry
For the past 60 years, dental composites have revolutionized restorative dentistry. Here are ways these versatile materials have changed the practice - and a look at promising techniques coming down the pike.
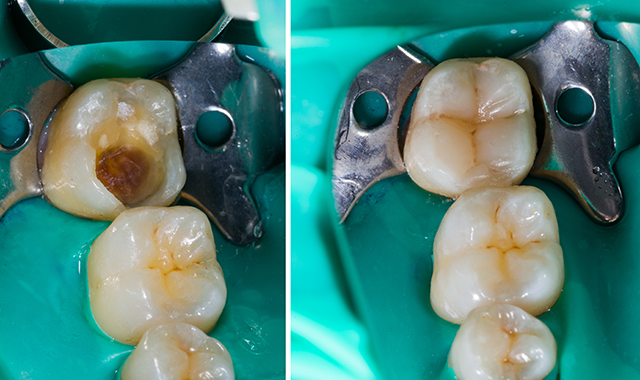
Dental composites first hit the industry in the mid-20th century. Since then, they have changed the way dental professionals approach restorative dentistry.
In 1955, Michael Buonocore, DDS, developed the acid etch technique for acrylic fillings. His simple method of applying phosphoric acid to enamel addressed concerns that the materials could not create a satisfactory mechanical bonding with natural teeth.1 The Journal of the History of Dentistry suggested that Dr. Buonocore’s discovery led to “a vast world of bonding of resins and cosmetic dentistry to unfold over the next fifty years."1
Other discoveries also contributed to the rise of resin composites’ popularity. The introduction of the DentalEZ fully reclining dental chair in 1958 and the increasing use of four-handed dentistry, which improved productivity and efficiency in the operatory by 1960, also influenced its use.2
Resin composite materials’ popularity further increased when Rafael Bowen introduced the thermoset resin bisphenol A-glycidyl methacrylate (Bis-GMA) in 1962; today’s composite resin restorative materials often use Bis-GMA.2 Over the following 30 years, dentistry saw many innovations in composite resins, from the introduction of light-cured materials to decreases in filler particles to enhancements in bonding systems.3
Related content: How dental composites have changed over time
Based on these modifications and the proper placement technique, the Swiss journal Schweizer Monatsschrift für Zahnmedizin described composite resin as “a reliable restorative material for nearly all applications.”4 Here are a few ways dental composites have changed clinical dentistry.
They changed the way many dentists treat cosmetic cases in the anterior and improved esthetics in the posterior. By the 1990s, tooth-colored restorative materials had helped usher in a new era of esthetic dentistry.5 Composite resins have improved their polishability over the years. Many of today’s composite materials have proved to have the mechanical and wear properties restorative dentistry seeks while providing the look of a natural tooth that patients demand. Dentists now use composite resins in a range of cosmetic procedures, including anterior veneers, diastema closings and small class III and extensive class IV restorations.6 Moreover, all classes of posterior restorations use composite resin restorative materials.6
They allow for more conservative preparations than previous materials. For many years, dentists had to remove what was otherwise healthy tooth structure to ensure retention of the filling material or to prevent recurrent decay. However, the ability to adhere the material to enamel and dentin eliminates the need to remove additional healthy tooth structure to create retentive features. Adhesive methods, not prep design, retain dental composites.7
They made isolation critical. Resin composites require excellent isolation because saliva, blood and other contaminants interfere with the adhesion of the materials with patients’ natural tooth structure. With past restorative materials, such as amalgam, isolation was not as vital. However, as the Annals of Biomedical Engineering pointed out, contamination of the restoration with bacteria, bacterial enzymes or oral fluids that get between the tooth and the restoration leads to premature failure and recurrent decay.8 Ensuring a pristine field for the bonding is crucial. Ideally, dentists should use a rubber dam,9 but other methods for isolation work too. However, if dentists choose not to use a rubber dam, they must retract the patient’s tongue during bonding. Also, dentists should ensure that if bleeding occurs, they can control it with either a hemostatic agent or use of a soft tissue laser to cauterize the area.
They also require a delicate balance between being too wet or too dry. While isolation is critical to the success of placing dental composite restorations, dentists must be careful to not over-dry the tooth. When the tooth is too dry, potential exists for postoperative sensitivity. Dental professionals must find the balance between the two to facilitate bonding with isolation while preventing postoperative sensitivity by keeping the tooth moist enough during the procedure.10
They mandate reading the manufacturer’s instructions. Dental composites are technique sensitive, and techniques often vary by brand. When working with a dental composite material, dentists must follow many steps for placing them correctly specific to their system. Following the instructions is essential to ensuring the best possible result from the material dentists are using for composite restorations - and for avoiding a compromised result. Moreover, many experts agree that being familiar with a system can boost productivity and efficiency when placing composite restorative materials.
They are pursuing bioactive and biorestorative properties for restorations. Since the introduction of glass ionomer cement in the 1960s, restorative materials have had the potential to affect the natural tissue around them. Today’s manufacturers are attempting to take bioactivity to the next level by developing materials with biorestorative properties. Marketers of biorestorative materials say they can help the tooth structure repair itself by releasing essential building blocks like calcium, phosphate and fluoride. While the validity of these claims is unclear,11 the promise of materials that can help prevent recurrent decay and help patients heal themselves is exciting.
Since Dr. Buonocore developed the acid etch technique to increase the adhesion of acrylic materials to enamel, composite resins have been a popular restorative material for dental practices the world over. Little did Buonocore know that his discovery would change clinical dentistry in many ways. More dental composite materials and more choices are available now than ever before for restorative dentistry. With the innovation in the material, it will be exciting to see what changes in clinical dentistry are in store for tomorrow.
References
1. Schulein, DDS, MS, Thomas M. “Significant Events in the History of Operative Dentistry.” Journal of the History of Dentistry (2005) 53:2, pp. 63-72. From Web. www.facuchard.org. 9 April 2019: < https://www.fauchard.org/system/publications/attachments/000/000/027/original/The-History-of-Operative-Dentistry.pdf>.
2. “History of Dentistry Timeline.” www.ada.org. Web. 9 April 2019. < https://www.ada.org/en/about-the-ada/ada-history-and-presidents-of-the-ada/ada-history-of-dentistry-timeline>.
3. Schulein, DDS, MS, Thomas M. “Significant Events in the History of Operative Dentistry.” Journal of the History of Dentistry (2005) 53:2, pp. 63-72. From Web. www.facuchard.org. 9 April 2019: < https://www.fauchard.org/system/publications/attachments/000/000/027/original/The-History-of-Operative-Dentistry.pdf>.
4. Zimmerli, Brigitte et al. "Composite Materials: Composition, Properties And Clinical Applications A Literature Review". Sso.Ch, 2010, https://www.sso.ch/fileadmin/upload_sso/2_Zahnaerzte/2_SDJ/SMfZ_2010/SMfZ_11_2010/smfz_11_2010_research1.pdf. Accessed 19 Mar 2020.
5. “History of Dentistry Timeline.” www.ada.org. Web. 9 April 2019. < https://www.ada.org/en/about-the-ada/ada-history-and-presidents-of-the-ada/ada-history-of-dentistry-timeline>.
6. Schulein, DDS, MS, Thomas M. “Significant Events in the History of Operative Dentistry.” Journal of the History of Dentistry (2005) 53:2, pp. 63-72. From Web. www.facuchard.org. 9 April 2019: < https://www.fauchard.org/system/publications/attachments/000/000/027/original/The-History-of-Operative-Dentistry.pdf>.
7. Hervás-García A, Martínez-Lozano MA, Cabanes-Vila J, Barjau-Escribano A, Fos-Galve P. Composite resins. A review of the materials and clinical indications. Med Oral Patol Oral Cir Bucal 2006;11:E215-20. Accessed via Web. 10 March 2020. <http://scielo.isciii.es/pdf/medicorpa/v11n2/en_23.pdf>.
8. Spencer, Paulette et al. “Adhesive/Dentin interface: the weak link in the composite restoration.” Annals of biomedical engineering vol. 38,6 (2010): 1989-2003. doi:10.1007/s10439-010-9969-6. Accessed via web. 19 March 2020. <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2871971/>
9. Wang, Yan et al. “Rubber dam isolation for restorative treatment in dental patients.” The Cochrane database of systematic reviews vol. 9,9 CD009858. 20 Sep. 2016, doi:10.1002/14651858.CD009858.pub2 Accessed via web. 19 March 2020. <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6457832/>.
10. Porto, Isabel. (2012). Post-operative sensitivity on direct resin composite restorations: clinical practice guidelines. Indian Journal of Restorative Dentistry. 1. 1-12. Accessed via web. 19 March 2020. <https://www.researchgate.net/publication/235977564_Post-operative_sensitivity_on_direct_resin_composite_restorations_clinical_practice_guidelines>.
11. Lawson, DMD, PhD, Nathaniel. “Examining Bioactive Restorative Materials.” Decisionindentistry.com. 11 April 2018. Web. 20 March 2020. < https://decisionsindentistry.com/article/bioactive-restorative-materials/>.
