Using Dental Technology to Troubleshoot
Technology can’t eliminate problems or miscalculations, but it can make rectifying those situations easier and help improve clinical outcomes.
Technology can make rectifying obstacles easier and less stressful on both the patient and the team while also improving clinical outcomes. Photo: VISIVASNC / STOCK.ADOBE.COM

Let’s face it, there is no perfect system. As I’ve said many times, striving for perfection is admirable.
It’s what we as health care specialists are challenged to do on a daily basis. However, expecting or demanding perfection is the definition of insanity. No matter how good the systems, the Second Law of Thermodynamics states that things naturally tend to go from order to disorder.
You may think that improvements in our processes and workflows naturally have the ability to eliminate problems we’ve dealt with in the past. But you cannot routinely count on technologies to solve problems that we cannot solve on our own. For example, I’ve had people tell me they were investing in a digital impression system because they “wanted their preps to be better.” While seeing your preps magnified x30 on the screen can help you identify areas that need improvement before milling or sending the scan to a laboratory, simply thinking a digital scan will improve things with no effort on your part is a fallacy.
Don’t get me wrong. Technology can do incredible things for your practice. It can make you a much better operator. However, it will not fix your mistakes. It will just help you make mistakes faster.
As Technology Evangelist, my mission is to push the envelope, find what is possible, and then report to you my discoveries. There are so many amazing technological advancements available to the profession today that it can be daunting to keep up with them. For this month’s article, let’s explore ways we can use technologies currently on the market to improve clinical outcomes for our patients.
Digital Impression Systems
Since we first used CEREC in the 1980s, digital impression systems have come a long way. It’s incredible to me when I think back and consider what progress has been made.
I started my journey into digital impressions in the late 1990s with CEREC 2, which booted the machine…wait for it…with a floppy disk! The images were shown on the monochrome screen in 1 dimension. The mill used a diamond cylinder and diamond wheel to fabricate the restoration. The camera took individual pictures that were captured by pressing a foot switch. When you consider where we are today, it’s a wonder that it was ever considered “state of the art,” but it was.
At that point in time, the acquisition unit and the mill were both contained within the same unit. While sometimes it was good for marketing for patients to watch the machine working, separating the units in the next generation, CEREC 3, was a better idea.
I remember discussing with engineers at Sirona Dental Systems the possibility of sending data to a lab for fabrication of the restorations. I knew there would be some doctors who didn’t want to learn how to design, and there would be cases better off in the hands of a human being. Unfortunately, the technology of the late 1990s and very early 2000s wouldn’t support that dream. There simply wasn’t a readily available high-speed data connection that could send files of the size the machine generated. Sending a crown would have taken hours, if it could have been sent at all.
Today, scans can be delivered to a lab so quickly that the doctor can call the lab and discuss complicated cases while the patient is still in the chair. Photo: Dentsply Sirona.
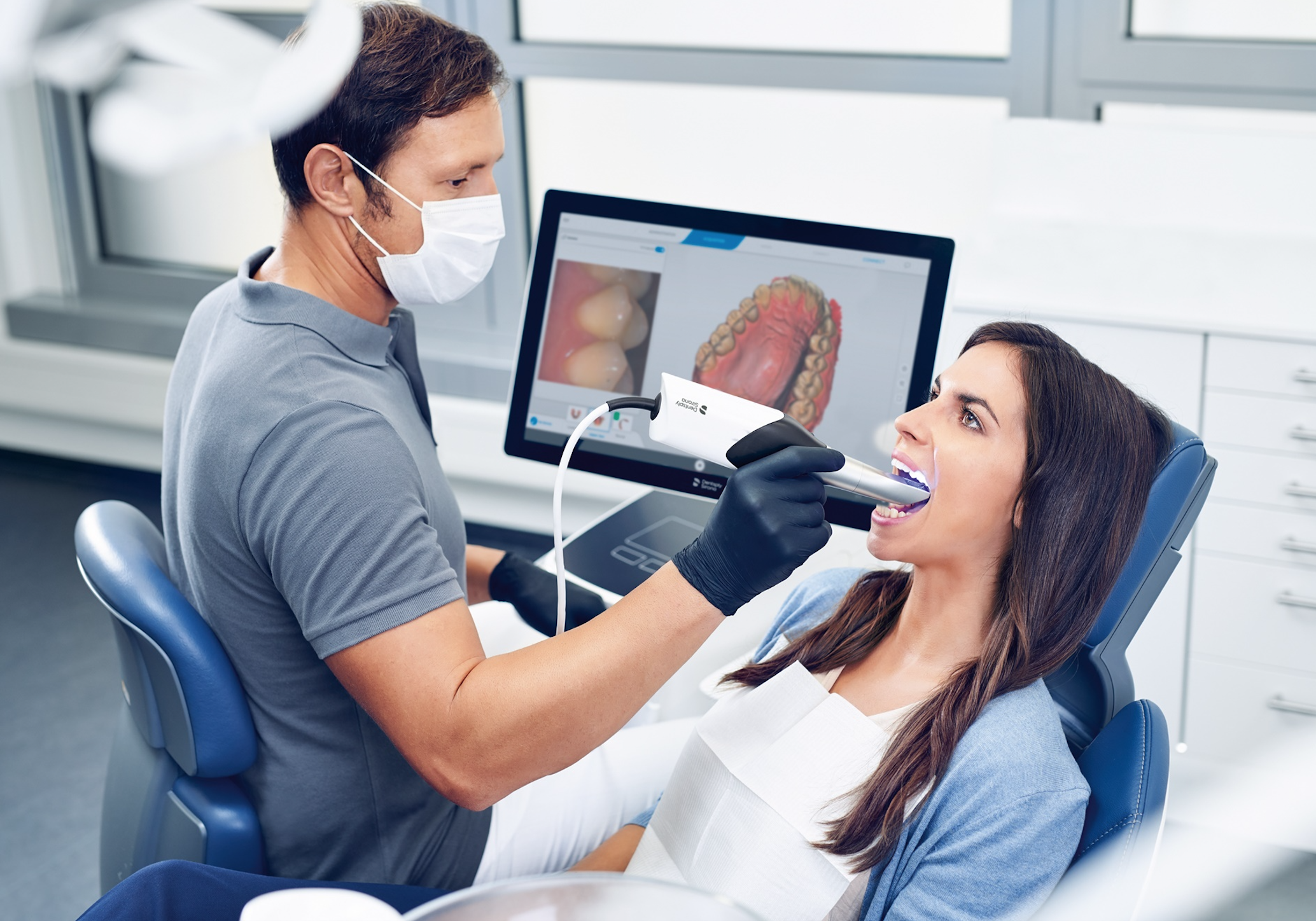
Now with the proliferation of high-speed data connections, almost every office can send a digital scan in just a few minutes. This has several advantages over analog impression systems. Scans can be delivered to a lab so quickly that the doctor can call the lab and discuss complicated cases while the patient is still in the chair. This results in better communication with the lab techs, and then better results for the patients. It also allows preparation refinements recommended by the lab tech to be made and sent out during the same appointment, which means that patients don’t have to return to have the prep refined. It’s a tremendous time saver for the practice and the patient.
Seating appointments also are much less stressful. Current digital impression systems are so accurate that it is rare to spend a lot of time adjusting. In fact, in my office we have come to expect that the actual adjustment time (if any is needed) to be 5 minutes or less. This helps keep the schedule running smoothly and patients happy.
Diode Lasers
For anyone who owns a digital impression system or is thinking of purchasing one, I highly recommend a diode laser. While retraction cord is still a viable option in fixed prosthetics, diode lasers are faster, easier, kinder to the tissue, and more reliable when it comes to eliminating problems with retraction.
One of the problems with retraction cord is that the moment you pull the cord, the tissue naturally begins to rebound to its original state. This always throws the team into a game of “Beat the Clock” to either fill the void with impression material or scan the area before the tissue rebounds sufficiently to close off the margin. This can especially be problematic in multiple unit cases. If you are using traditional analog impression techniques, 1 bubble on the margin means you are right back to square 1, packing cord, wasting time, and then playing round 2 of “Beat the Clock.” Some operators choose to use a 2-cord technique to help prevent the above scenario, but that is more time, more effort, and still not guaranteed to rectify the situation.
Because a diode laser ablates the tissue, there is no rebound. That means there is no clock running in your head on how long you have before the potential for problems sets in. Multiple units are simple because once exposed, the margins stay exposed until the body rebuilds the tissues that were ablated.
The margins are quickly and easily exposed, usually taking about 1 minute per tooth. The tip on these lasers is between 300 to 400 microns, so they are minimally invasive while still allowing room for impression materials or allowing the digital scanner to see well past the margin. Some doctors feel that deep margins cannot be read by digital scanners, but that isn’t true. Deeper margins are more difficult for the camera to see, due to the need for the camera to have straight line access visually to the margin. Because light travels in a straight line, a laser does a phenomenal job of dealing with these situations. I have yet to come across a margin that our iTero Element scanner cannot read, if properly exposed.
Using lasers leads to almost no post-operative pain for the patient, meaning that even very deep margins that require greater ablation than normal heal uneventfully. Lasers have so many unique ways of solving everyday problems in fixed prosthetics that there is no way I could practice without them.
One negative I sometimes hear about lasers is their cost. However, time savings and quality of treatment are just two of the benefits that come from diode laser usage in everyday dentistry. Lasers have become quite affordable in the last few years. The Picasso diode lasers from AMD (amdlasers.com) are used by many doctors who understand the value of lasers but are not enamored of units with a high price tag. AMD has created a market of high-value hardware for a very reasonable price.
Composite Curing
Bonded restorations frequently require troubleshooting. While there are many factors that can contribute to postoperative problems, one of the most common is the curing light.
In an attempt to get better depth of cure and greater procedural efficiency, many companies have increased the power of their lights. This creates the problem of the “double-edged sword.” While the increased power does provide better penetration of the photons, which gives better depth of cure, the increase in power also creates increased heat.
While you cannot overcure a composite, multiple curing cycles with an intense light can cause pulpal tissue to be thermally affected. Many operators, attempting to get the best cure possible, use multiple curing cycles. However, by doing this, the tooth becomes a heatsink, and the pulp absorbs the excess energy. An increase of 5° C can result in pulpal inflammation, which can cause the dreaded post-op sensitivity we all try to avoid.
The best way to avoid this with high-intensity lights is to slow down between curing cycles and give the tooth a chance to cool. However, there are a couple of lights coming to the market that may provide better depth of cure than multiple curing cycles.
PinkWave from Apex Dental Materials (apexdentalmaterials.com/pinkwave) uses an array of multiple LEDs that emit light in four different wavelengths. This gives the PinkWave the ability to cure all photoinitiated materials but with less heat. The device utilizes two types of LEDs to create the standard blue wavelengths needed for light curing, but also uses a pink wavelength and a near-infrared wavelength to provide better depth of cure and less volumetric shrinkage. In addition to lower heat output, less volumetric shrinkage can also decrease cuspal flexure during curing, thus minimizing postop sensitivity.
The device has a white LED so that, in addition to a curing light, the PinkWave also becomes a highly efficient transilluminator. This helps with diagnosing problems such as “cracked tooth syndrome,” as well as recurrent caries and other clinical problems that can be a bit difficult to visualize without transillumination. Having a curing light that doubles as a transilluminator gives doctors a 2-in-1 device that makes practicing more efficient.
Another curing light coming on the market is the Monet from AMD. The Monet is the industry’s first handheld curing laser. Lasers kickstarted the concept of high-speed curing back in the 1990s. Unfortunately, those lasers were huge boxes that required a cart, were noisy, and were incredibly expensive (I paid $8,000 for mine). However, the smart folks at AMD have turned those large boxes into a standard handheld curing footprint…amazing!
Because the Monet is a true laser, the beam is collimated, so it stays focused in a straight line. This allows all the photons generated to be applied to the target. Lasers also are incredibly bright, meaning it better penetrates into the composite. The device provides a depth of cure of 5 to 8 mm, depending on composite shade, with a 3-second cure cycle. Applying the high energy beam for short cycles allows for tremendous curing with minimal heat generation. Restorations can be built up with fewer incremental layers, speeding up procedures. The Monet provides stronger composites and ensures less sensitivity.
Wrapping Up
Throughout my career, I’ve learned that technology provides incredible tools, along with better and more choices. It is rare for me to find a new device that completely eliminates the need for its older sibling. I may not use the older device very often, but I still find that the toolbox keeps growing. I don’t throw tools away; I just don’t use the older tools as often.
Everything we do in life and in dentistry carries inherent risks. Those risks can be linked to problems, and those problems can be studied and evaluated, then those problems linked to solutions. Technology has allowed us to do incredible things in dentistry, but it will never eliminate problems or miscalculations. However, technology can make rectifying those situations easier and less stressful on both the patient and the team while also improving clinical outcomes. And at the end of the road, that’s what we’re all striving for, right? See you next time!
