A mysterious upper-back pain syndrome in dental professionals
Scalene trigger points often fly under the radar of clinical treatment, but they can have serious consequences for dental professionals.
You’ve tried massage, acupuncture and physical therapy for that aching pain on the medial border of your shoulder blade, but to no avail!
Fig. 1: Pain at the medial border of the scapula is often of trigger-point origin.
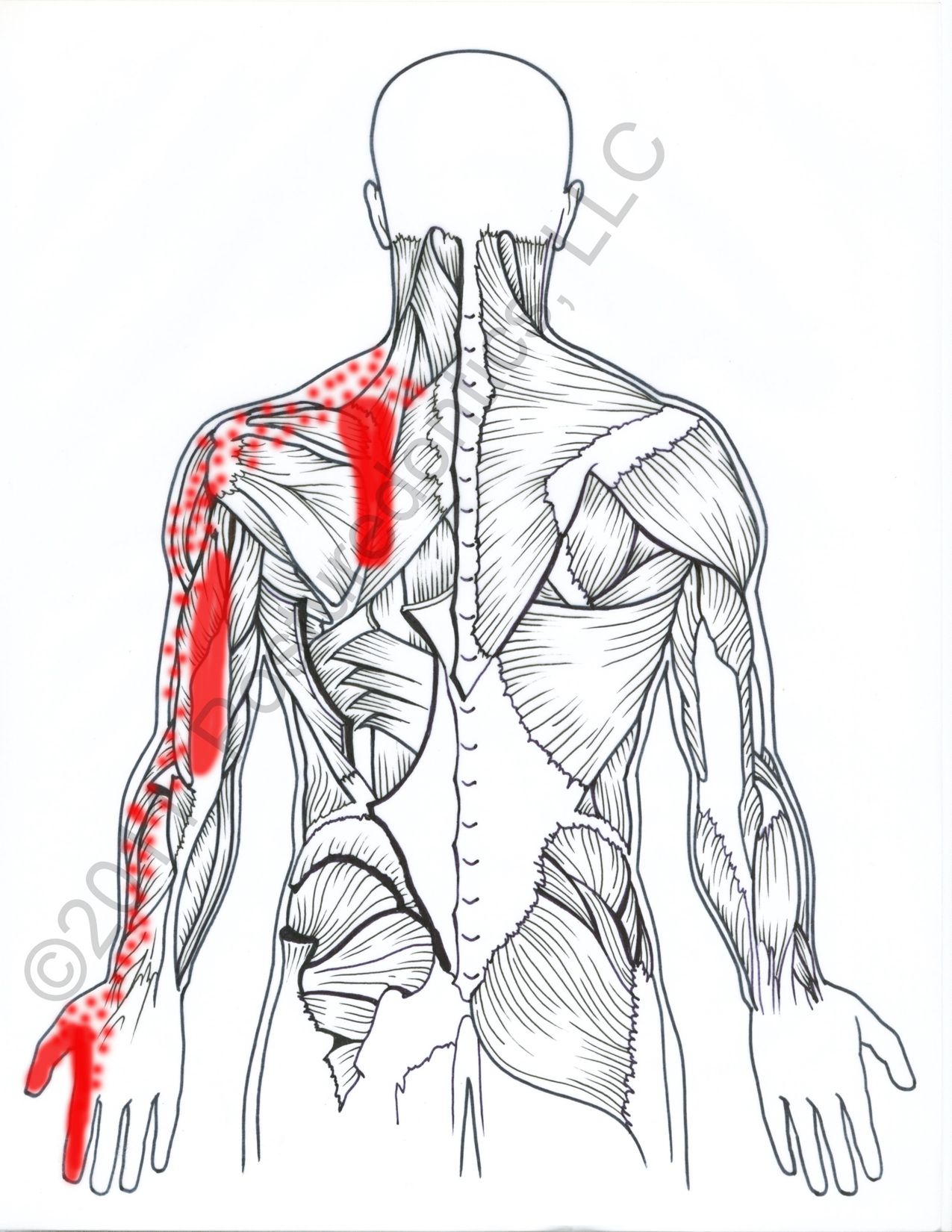
When treating pain in this area (Fig. 1), most bodywork therapists address the local muscles (i.e. rhomboids, middle traps). However, in dentistry, one of the most common causes of pain along the medial border of the scapula is scalene trigger points.
A trigger point (TP) is a sustained contracted knot in a tight band of muscle that neither allows the muscle to contract nor relax. Typically, trigger points refer pain to a distant area, which is one reason they are frequently overlooked in Western medicine. They are also not currently recognized as a valid diagnosis in the United States, so easily fly under the radar of effective clinical treatment.
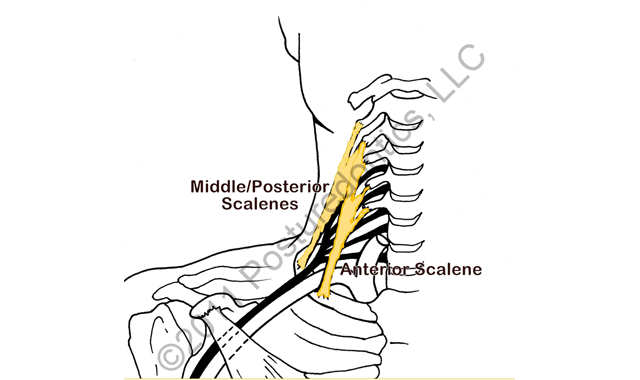
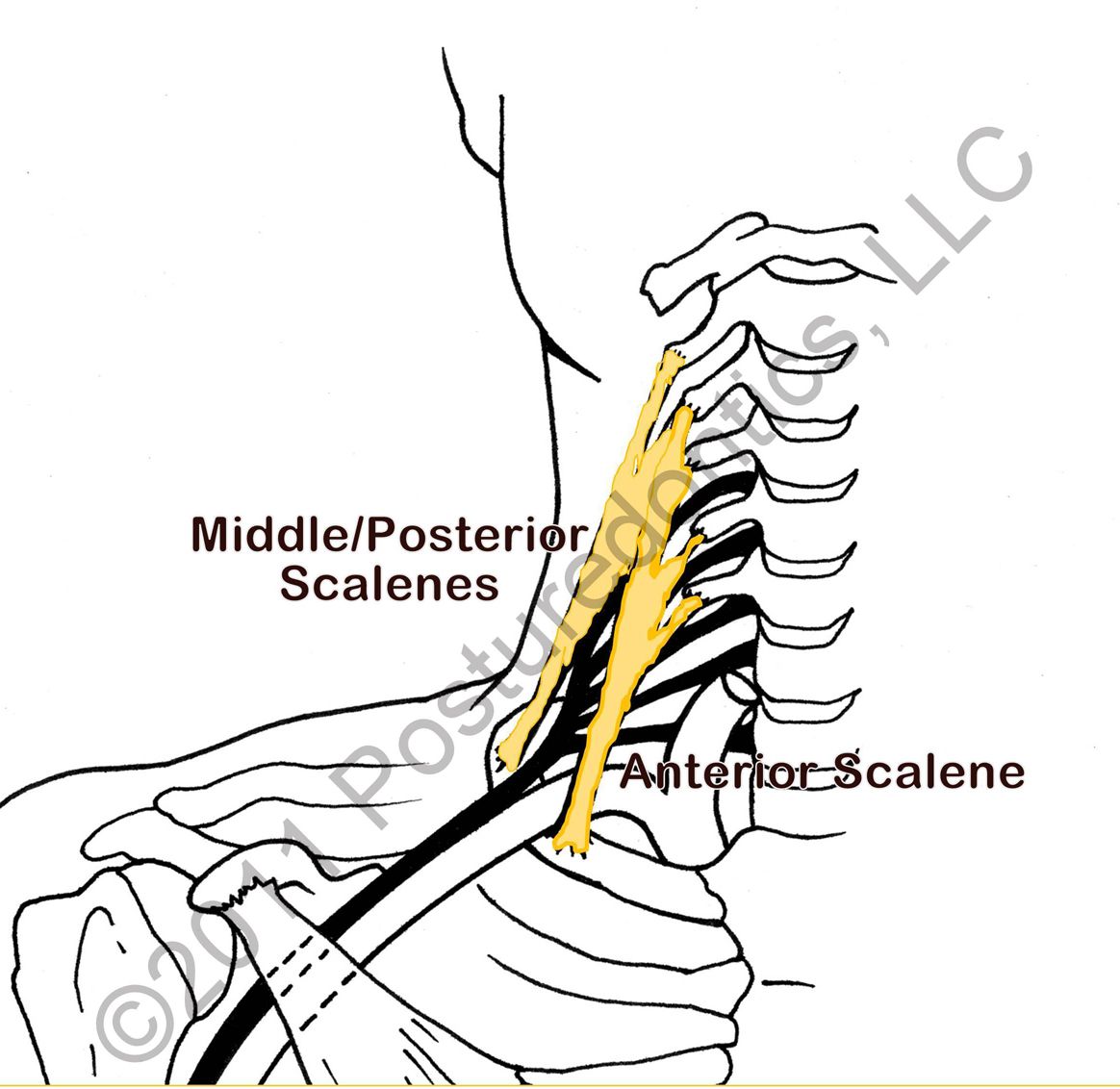
Located at the sides of the neck, the scalene muscles actively sidebend the neck and stabilize the neck against sideways movement (Fig. 2). Thus, it is easy to see why dental professionals are so vulnerable to developing trigger points in these muscles. The scalene muscles are frequently misdiagnosed by health care professionals as rhomboid trigger points, since pain is rarely felt in the scalene muscles themselves. Trigger points in these muscles are also a common cause of thoracic outlet syndrome. Scalene trigger point symptoms include:
• pain in the medial border of the scapula and interscapular pain
• aching pain in the chest area (often mistaken for angina pectoris)
• pain and weakness in the front/back of the arms and thumb side of the hand and index finger
• dropping of objects
• moving the arm and neck restlessly, to apparently relieve the discomfort
Related reading: 3 ergonomic mistakes that could end your dental career
Fig. 2: Trigger points in these neck muscles refer pain to distant areas of the body.
Victims of motor vehicle accidents (MVAs) are especially prone to developing severe trigger points in the scalenes, so team members who have been in MVAs should be familiar with all scalene T.P. referral patterns and highly vigilant with preventive strategies.
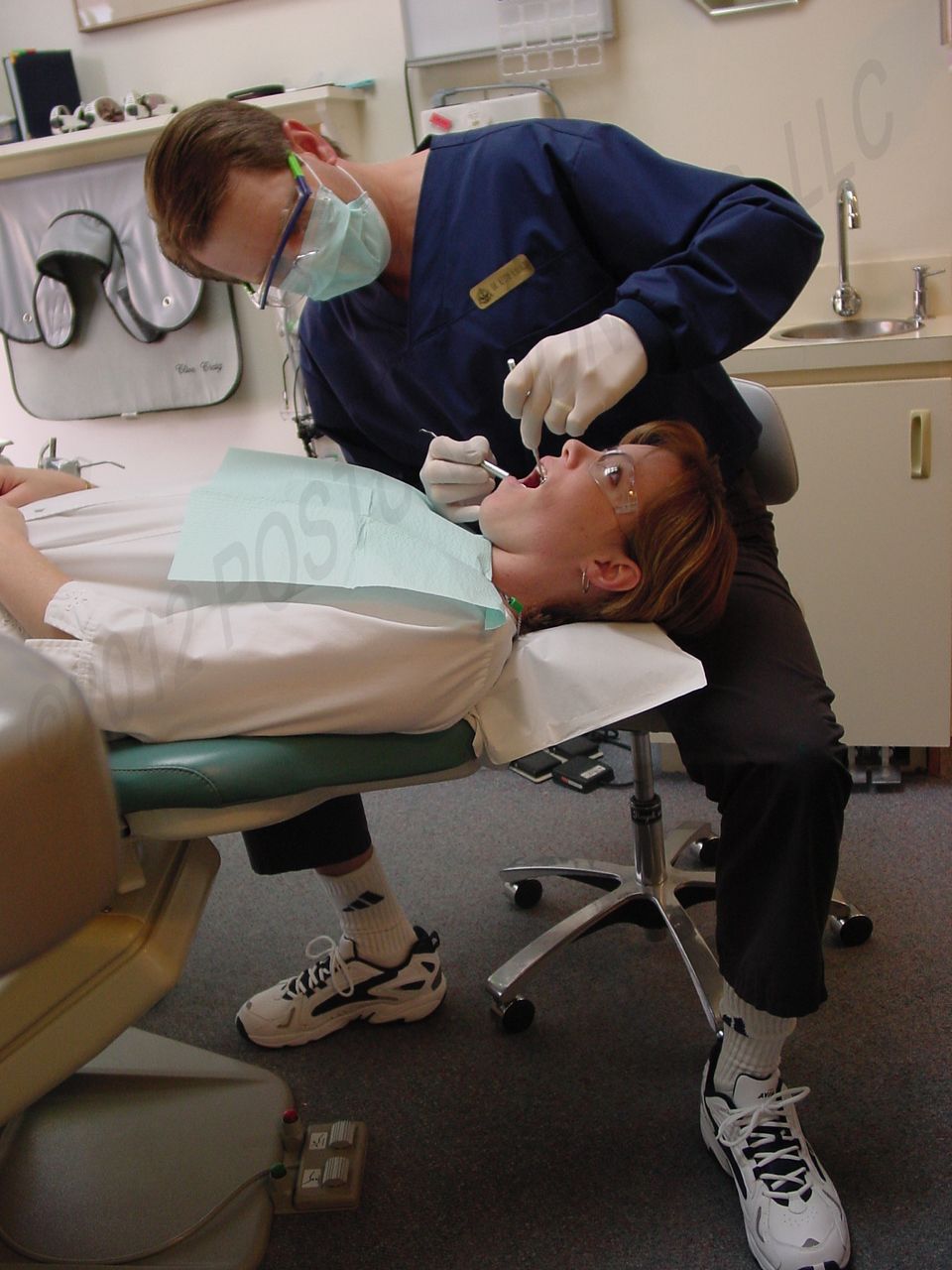
Activities in the operatory that can cause and perpetuate scalene TPs include: working with the shoulders on a tilted axis, leaning the neck to one side to view the treatment area, forward head posture, extended reaching forward with the arms, poor lighting that causes shadowing and chest-breathing (instead of diaphragmatic breathing) (Fig. 3).
Ergonomic interventions
1. Proper patient positioning: Team members who persistently lean the head to one side to view the treatment area or infrequently use their mirror will have a difficult time resolving their scalene TPs. Special patient positioning guidelines must be observed to maintain level shoulder posture during all treatment. Watch excerpts from the “Positioning for Success” DVD at www.posturedontics.com/patient-positioning-sequences.php.
2. Overhead light angle: Contrary to what most dental professionals were taught in school, shadowing is most effectively reduced when the overhead light parallels your line of sight as closely as possible. Therefore, the light should be positioned slightly behind and to one side of your head. Of course, the lighting that most closely parallels your line of sight is headmounted lighting!
3. Armrests: Simply taking the weight of the arm off these muscles will help reduce perpetuation of trigger points.
4. Good declination angle: Since forward head posture is a contributing factor to scalene trigger points, make sure your scopes have an excellent declination angle. For more information on this, see Dr. Valachi’s article “Are loupes improving or worsening your neck health?”
5. Chest breathing: Shallow chest breathing, which commonly occurs in the operatory, can easily cause scalene TPs. Make a concerted effort to use diaphragmatic breathing (stomach goes out when inhaling, not in!) whenever possible.
Trending article: Why all exercise is not necessarily good exercise for dentists
Risk factors outside the operatory
Scalene trigger points are often found in people who ‘suck in their gut’ to improve their appearance, since this causes chest breathing. These individuals often find they run out of breath when speaking or on the phone
Foam pillows that have a ‘springy’ property to them can worsen scalene trigger points.
Fig. 3: Scalene trigger points are worsened with side-leaning posture.
Cold temperatures can also increase hyper irritability of the scalene muscles. An air conditioner that blows on the neck can be especially problematic.
Team members who are highly prone to emotional stress are especially susceptible to scalene trigger points.
Pilates exercises that require lifting the head off the floor for prolonged periods of time can worsen scalene (and sternocleidomastoid) trigger points. Since they are prone to tightness in these muscles, most dental professionals should leave their head on the floor during these Pilates moves.
Sit-up techniques that curl the head forward can cause and worsen scalene trigger points.
Preventing and managing work-related pain in dentistry requires addressing multiple risk factors. Oftentimes, pain syndromes may walk like a duck and look like a duck, but they are not, in fact, a duck!