Review Your Cement Inventory to Increase Flexibility, Decrease Costs
Here’s how to decide which cements to stock and what to keep in mind when choosing systems.
ANATOLIY GLEB / STOCK.ADOBE.COM
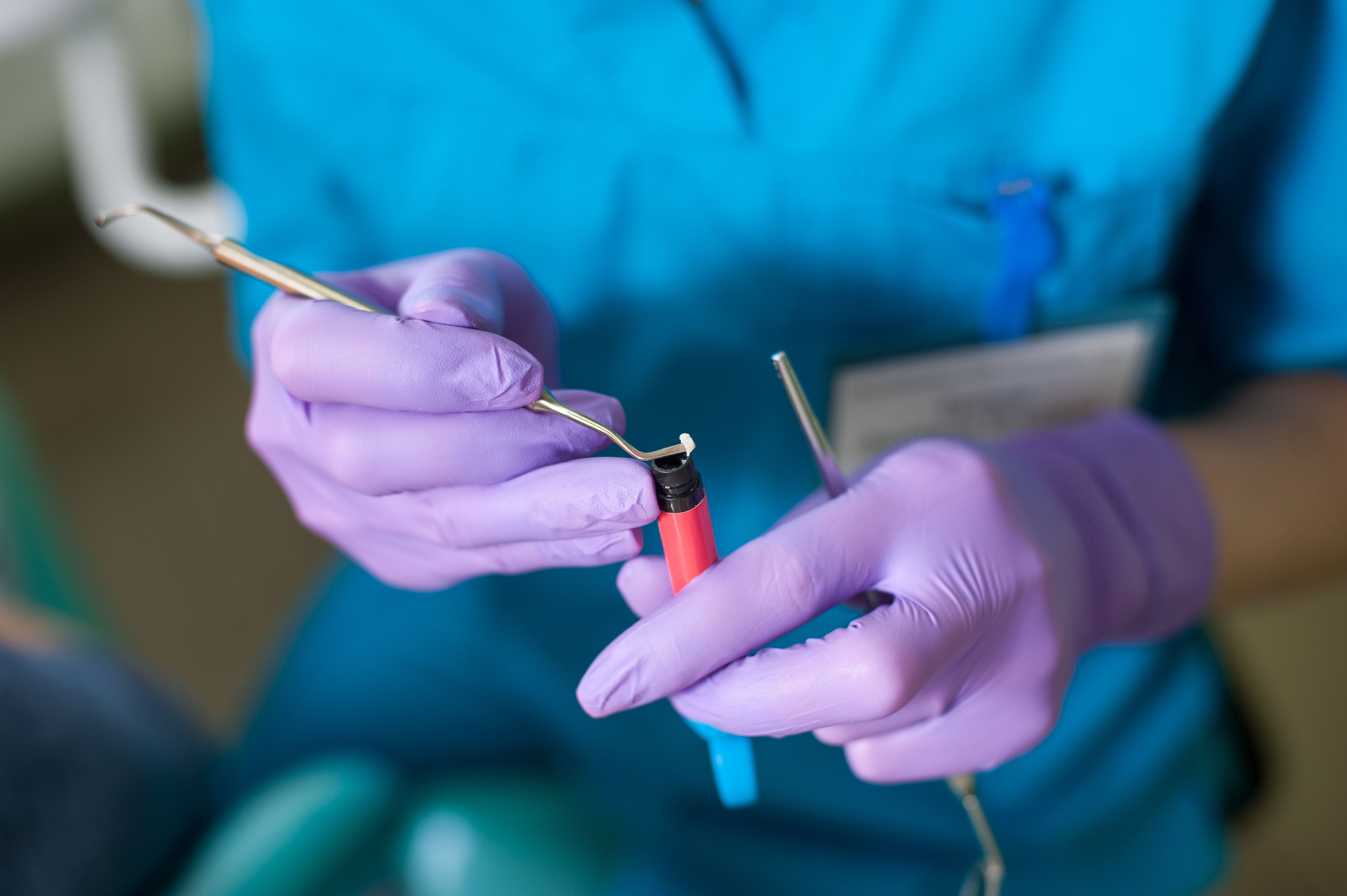
We all like having options. But too many options can be detrimental. Imagine standing in front of the ice cream cooler in the grocery store and choosing from 100 flavors. While the variety is impressive and surely provides the perfect selection for everyone, you’re stuck trying to decide—or end up leaving with a dozen different flavors. Being presented with fewer options makes the decision a lot simpler, and you’ll most likely still walk away satisfied.
The same goes for dental cements. Providing yourself with a variety of choices is critical for restoration success, but there’s no need to stock hundreds of cement systems. Keeping numerous systems in-house increases inventory costs and the likelihood that the cements will expire before you need to use them.
So, how do you know which cements to stock? While there isn’t a 1-size-fits-all cement for every indication, there are several important considerations to help you figure out how many cements you need while also reducing your inventory to a manageable amount.
Considerations for use
There are myriad indications to take into account when choosing a cement system.
“When bonding cosmetic cases, we have 1 system,” explains John Flucke, DDS, Dental Product Report®’s technology editor, who practices in Lee’s Summit, Missouri. “We have another for cementing implant crowns, etc. And different indications also affect cement choice. For example, in addition to restoration material and location of the restoration, the available retentive properties of the prep, prep sensitivity, and cosmetics all come into play.”
Restoration location
The restoration’s location can help you determine which cement to use. Anterior restorations will require a cement with higher esthetic properties. While esthetics aren’t as critical to posterior cases, these hard-to-reach cases may require a cement that is more moisture tolerant, since isolation will be a larger challenge. This means turning to a conventional cement that can accept some moisture.
For example, glass ionomer cements are extremely tolerant to moisture, and resin-modified glass ionomer (RGMI) cements are ideal for situations where maintaining a dry operating field may be difficult or impossible. Conversely, total-etch resin cements require precise isolation from contamination, and they should be avoided in cases where maintaining isolation is difficult.
Restoration material
Cementing will be a waste of time if the cement can’t bond with the substrate in indirect restorations. It’s critical to choose a cement that is compatible with the restoration material. Resin cements are an ideal choice for glass-ceramic restorations, thanks to their superior bond strength. RGMI cements are indicated for metallic, PFM, lithium-disilicate CAD/CAM inlays and onlays, and also for alumina- and zirconia-based ceramics. This all comes back to the golden rule of following the instructions: By reviewing manufacturers’ guidelines and recommendations for use, you can ensure you’re stocking a product that will work with a designated restoration material.
Esthetics
Just because a cement can bond to a material doesn’t mean it’s the only choice. Esthetics play a major role in cement selection, as varying opacity and even viscosity can affect the end result. In general, light-cured cements provide better color stability (necessary to mimic the color of natural dentition) and are available in a wide range of VITA and chromatic shades.
For example, say you’re doing a thin-walled restoration, such as a veneer. You’ll want to reach for a low-viscosity material to ensure the restoration will seat easily and postseating drifting will be minimized. Thanks to their thin film thickness and high translucency, this makes resin cements an optimal choice—provided they are light-cure and total-etch. While self-adhesive cements may be simpler to use, they should be avoided for this type of restoration as they are prone to color change over time, which can adversely affect the appearance of the veneer over time.
Prep design
Not every case will present with easy prep. In situations where prep may be compromised, cement strength becomes paramount. Retentive crown or bridge preps don’t require extra bond strength, so a conventional cement, such as a glass ionomer or RGMI cement, can be used (though self-adhesive resin cements can be considered in cases where the restoration material (such as glass ionomer) is weaker.
Self-adhesive resin cements should also be the choice for nonretentive preps, or preps with a smaller surface area. The strong bond strength of resin cements can help give extra support to the restoration, and their esthetic properties make them adaptable for both anterior and posterior restorations. These cements are also ideal for partial preps (particularly on enamel), though generally indicated for use with a separate bonding system and enamel etch.
Ease of use
Choosing the correct cement will be a moot point if it can’t be properly dispensed easily, or has a narrow window for removing excess cement. Additionally, introducing extra steps such as mixing into the process greatens the likelihood of user error. “I prefer systems that are self-mixing, because I know that when it exits the dispenser it will be mixed exactly according to the manufacturer’s specifications,” Flucke says.
Using self-mixing, all-in-1 universal systems is an efficient way to cut down on the cumbersome steps that increase opportunities for mistakes. Since universal 1-bottle systems combine the etching, priming and bonding steps into 1, it eliminates the need for mixing, while also reducing the need to use multiple products for 1 procedure. Additionally, the range of protocols they allow for (self-etch to total-etch, light-, dual- or self-cure composites) mean that dentists can implement their preferred methods.
How many does it take?
So, what’s the right number of cements to stock? Dentists are going to need at least 2—a resin cement and a conventional cement. This gives practitioners flexibility for situations where moisture may be an issue, or where esthetics is paramount.
For Flucke, personally, the answer is 4.
“We currently keep 4 different systems in my practice,” he says. “Which one we use depends on the case.”
By stocking 4 unique systems, Flucke can cover a range of needs. In his practice he always makes sure to have Maxcem Elite Chroma (Kerr), PermaShade LC (Ultradent Products), TheraCem (BISCO) and Variolink (Ivoclar Vivadent) on hand.
Each system brings different strengths to the table for different indications. Maxcem Elite Chroma has an automix delivery system, and its Color Cleanup Indicator makes cement cleanup easy. PermaShade LC, designed for use with porcelain, composite and zirconia veneers, has excellent color stability. Variolink is ideal for glass-ceramic, lithium disilicate glass-ceramic, and composite restorations. Universal adhesive TheraCem, which contains methacryloyloxydecyl dihydrogen phosphate (MDP) to promote a strong bond to zirconia, metal, and alumina substrates without a primer, has the added bonus of releasing calcium and fluoride.
While some clinicians may find they need a wider variety to cover a range of indications, there’s no need to stock a cement for every imaginable scenario. By limiting your selection—while still making sure you’ve covered your bases—you can cut down on inventory costs but still provide superb, long-lasting cementation.