Photobiomodulation for Dental Patients Undergoing Cancer Treatment
Laser therapy can prevent and treat adverse effects, helping patients avoid the interruption of treatment and maintain better quality of life.
Today the greatest fight of humanity is against cancer. Patients need to be very strong to face the diagnosis, the treatment, the uncertainty of what will happen, and the adverse effects (AEs) of the treatment, which are so debilitating that they may become worse than the disease itself.1
The management and control of AEs are fundamental to not only ensuring the patient’s comfort but also allowing the cancer treatment to continue. AEs occur once the cancer treatment goes beyond destroying altered cells and begins affecting the healthy ones. Chemotherapy attacks cells that multiply fast. In addition to the tumor, it attacks and destroys oral and gastrointestinal cells, nails and hair, and cells produced by the bone marrow (blood cells, defense cells, and platelets).2
In radiation therapy, cells that are near the tumor, in the irradiation range, are injured. Thus, several tissues are affected by radiation such as salivary glands, muscles, nervous tissue, teeth, bones, skin, and oropharyngeal mucosa.
A common and debilitating AE that occurs in the entire gastrointestinal tract mucosa is known as mucositis. It is an inflammatory, erosive, and ulcerative lesion that, in addition to causing pain, compromises food, speech, and oral hygiene and ends up being the gateway to a systemic infection.
In an attempt to alleviate the symptoms, some products are recommended, such as mouthwash with bicarbonated water, vitamin E oil, and topical anesthetics. However, what is most effective for both treating and preventing oral mucositis is photobiomodulation.
Scientific evidence includes Cochrane reviews and Multinational Association of Supportive Care in Cancer/International Society of Oral Oncology clinical recommendations that list photobiomodulation as the best choice to manage oral mucositis.
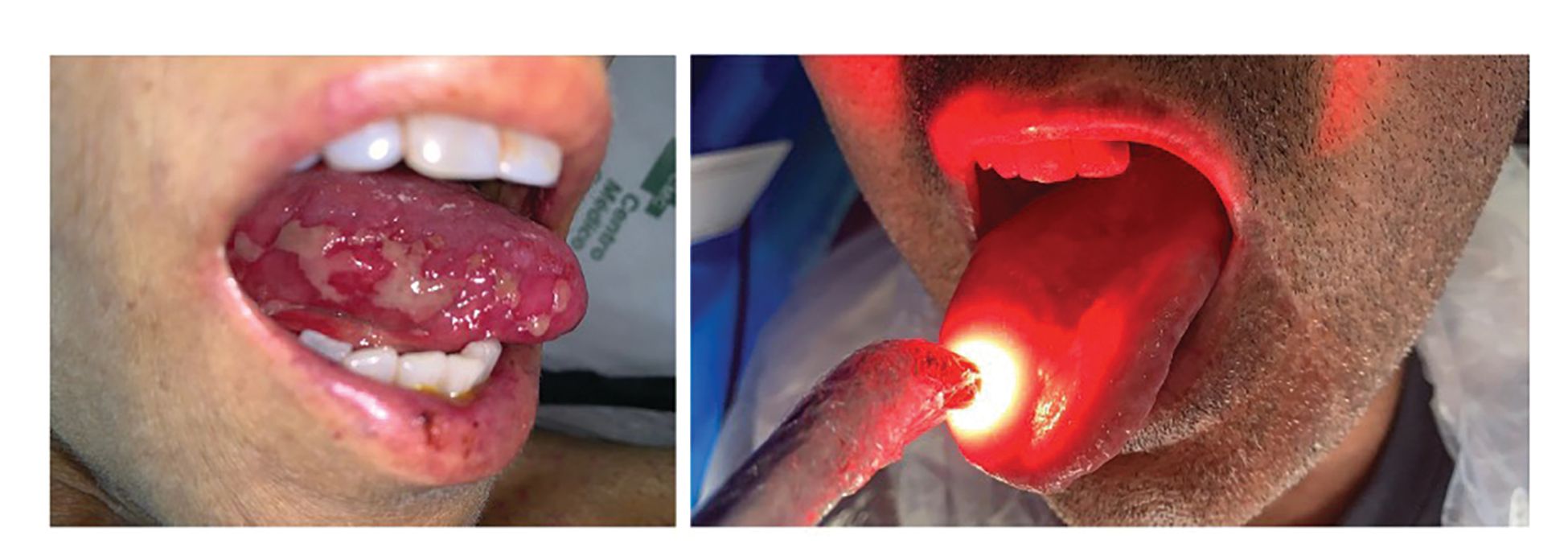
Laser therapy can either prevent or treat oral mucositi (Figures 1 and 2). Mucositis can be prevented by applying the laser after injury to the mucosa has occurred—that is, after chemotherapy or head and neck radiation therapy. At this time, the inflammation started by the treatment toxicity can be modulated by laser therapy, avoiding cell apoptosis that leads to mucosal ulceration and, thus, avoiding ulcers and bacterial colonization and minimizing the systemic infection that can happen in immunocompromised patients.
Oral mucositis treatment by laser therapy can be performed after the lesion occurs, and laser therapy will promote energetic and functional homeostasis, which leads to pain reduction and accelerates tissue regeneration. With the Horizon Laser System from Summus Medical Laser, you would select the size of the lesion so the software will automatically deliver the correct dosage and proper time frame for application.
The Horizon Laser System from Summus Medical Laser.

The effectiveness of the treatment is related to the right light intensity in the target tissue. This can be done with any laser device, but recent technologies have improved laser capabilities.
Multiple wavelengths affect penetration and stimulation of multiple chromophores within the metabolic process. Pulsing and superpulsing laser modes can better enhance different physiologic mechanisms and even different cell types. Higher power gives more energy in less time, and larger probes guarantee low intensity.3 This results in efficient and effective photobiomodulation distribution over the entire tissue.
Based on the type of treatment—chemotherapy, radiotherapy, or hematopoietic stem cell transplant (HSCT)—the risk to develop mucositis increases respectively. Other risk factors such as dose, type of chemotherapy, type of radiation therapy, type of transplant (autologous or halogen), the patient’s immune status, age, and oral hygiene should also be considered.
It is very common, especially for cultural reasons, that patients prioritize the health of the body over oral health. But what needs to be said, reinforced, and taught in the general population is that oral health is closely related to the health of the body. In addition to cardiac, diabetic, kidney transplant, and older patients, patients with cancer must be aware of the influence that inflammation and oral infections have on their treatment outcome and evolution of the disease.
Patients undergoing chemotherapy, whose immunity is affected by the medication, must be informed that any oral infection can trigger a generalized infection. Radiation decay or even osteonecrosis (bone necrosis that may be irreversible and progressive) can happen if patients have an infected area in the mouth and receive radiation. And finally, patients undergoing HSCT are at the greatest risk of death if they have an oral infection. In these patients, the immune system needs a reset to enable transplantation, and any small infection can be fatal.
What to Expect
- By modulating inflammation, the laser can save cells from apoptosis, preventing oral lesions (oral mucositis).
- The laser can reduce symptoms and pain in established mucositis lesions.
- The laser promotes the regeneration of salivary glands and adjacent tissues affected by the treatment.
- The treatment time is fast (using Class IV lasers), and the patient does not experience any discomfort during therapy.4
In addition to oral mucositis, other AEs including xerostomy, pain, dysphagia, dysgeusia, opportunistic infections, dental hypersensitivity, trismus, edema, neurotoxicity, ototoxicity, and radiodermatitis can be managed with laser therapy.
Dental follow-up before and throughout cancer treatment is very important. In addition to maintaining the oral health of patients, using available laser therapy, the dentist now can help prevent and treat the AEs associated with cancer treatment. This is essential to avoid the interruption of treatment and ensure a better quality of life for patients during and after cancer treatment. ●
