Mapping the Root: The Latest in Endodontic Diagnostic and Treatment Planning Technology
Clinicians today can use CBCT, surgical microscopes, and more to provide predictable endodontic care, as well as plan treatment and communicate better with their patients.
ALEX MIT / STOCK.ADOBE.COM
For years, patients associated root canals with 2 very negative things. One, the pain was going to be great. And two, years ago the end results could be unpredictable, so some patients have choosen to skip the endodontic treatment rather than risk failure and possibly suffer plenty of pain with no gain.
But those days are behind us. Advancements in technology, materials, and techniques have changed endodontic care dramatically. Diagnostic tools like CBCT and surgical microscopes have had a tremendous impact on improving care for patients and making the lives of clinicians a whole lot better.
These tools provide much more information than was previously available, enabling today’s clinicians to tackle endodontic cases with extensive knowledge and precise details. But another factor is knowing when certain cases just can’t be successfully performed. These diagnostic developments—especially CBCT—can guide clinicians away from taking on a case that’s most likely going to fail. The result is better treatment for the patients and fewer poor outcomes.
“Root canals get such a bad rap. Patients often report, ‘Oh, nothing [endodontic] works on me.’ I think this is further perpetuated by word of mouth [from] friends and family members, and it really bums me out because the actuality of what I see in my practice is that some patients present with a failing root canal often because they were looking for the fastest or lowest-cost root canal the first time around,” says Judy McIntyre, DMD, MS, an endodontist at Hopkinton Endodontics outside Boston, Massachusetts. “Unfortunately, doing quality work—in any field—is an investment.”
Dr McIntyre has long since invested in CBCT and surgical microscopes and uses both technologies all the time in her practice.
“I have both in my office, and, thankfully, I was trained with both,” she says. “I employ both on a daily basis, on almost every patient. My goal is to save teeth. But that’s not always possible. Diagnosis and treatment planning [are] seeing what exists and then planning what is actually possible and has the best/good prognosis, and going from there.
“Sometimes, sadly, it may mean turning patients toward an implant or extraction. I’m not just talking about unideal retreatments because the roots are too thin or there’s resorption or a large post,” Dr McIntyre adds. “I’m even thinking about some virgin teeth [that are] unrestorable due to cracks or resorption, etc.”
Brooke Blicher, DMD, an endodontist in private practice in Vermont and a member of the Dental Products Report® Editorial Advisory Board, can’t say enough good things about the value of a cone beam unit in dentistry. The information provided from CBCT scans allows her practice to perform better endodontic care with increased confidence brought on by improved diagnostics.
“In endo, the answer [to diagnostics and treatment planning] is really simple; it’s CBCTs,” says Dr Blicher, who also teaches at Harvard School of Dental Medicine and Tufts University School of Dental Medicine in Boston, Massachusetts. “We bought a machine in 2013. Up until that point we sent a few patients out here and there because we know that CBCTs pick pathology up earlier so we can see infections and inflammation in an earlier stage as compared to traditional, periapical films. We’d also use it when we were planning for surgery and wanted to know if there was important anatomy close by—were we close to the sinus or the mandibular nerve. Eventually we sent enough out that we could justify buying a machine in our office.”
Once CBCT was in her office, Dr Blicher and her staff were amazed at how much information they consistently got and how often these new details were dramatically changing the diagnosis and treatment planning for the patients.
“Initially, we were fairly limited in our use of the CBCT,” Dr Blicher explains. “But as we used the machine more and more, we found an explosion in the amount of incidental findings. As a result, we now take an image on almost every diagnostic patient because of the number of cases where we find things that we don’t expect that dramatically change our diagnosis and our treatment plan.
“The classic example is resorption. When present, it can dramatically change our treatment planning. CBCT has revolutionized the accuracy of our diagnosis, the selective nature of our treated cases. Ultimately, our success rates are going to be better because we’re not getting into cases that aren’t going to work.”
Dr McIntyre says using CBCT, such as with the DEXIS Orthopantomograph™ OP 3D™, provides her with essential information—the additional details allow her to not only provide better care to her patients, but also to know when not to take on a case that’s likely to fail.
This complete 3D x-ray imaging platform from DEXIS provides easy-to-use features throughout the entire workflow. With its versatile imaging programs, intuitive user interface, and different configurations, the DEXIS OP 3D offers optimal imaging to any practice.

Her confidence increases when using CBCT and a microscope for diagnosis and for treatment planning. With versatile imaging programs, an intuitive user interface, and different configurations, the DEXIS OP 3D is designed to offer imaging excellence to any practice to support all clinician needs and help focus on delivering better patient care.
A number of companies have made big strides in CBCT units recently, including Carestream, Dentsply Sirona, J. Morita, Planmeca, and PreXion.
J. Morita developed one of the first 3D units in the dental sector worldwide, the 3D Accuitomo, which was introduced in 2001 at the International Dental Show. Improved clarity and dose reduction for improved patient protection are at the core of the company’s research and development. J. Morita’s x-ray units show even the most delicate structures, allowing for the evaluation of root fractures, fourth canals, apical lesions, resorption, and much more. Today, its fourth-generation unit is the 3D Accuitomo 170, while the company’s newest unit is the Veraview X800. Additionally, J. Morita manufactures Root ZX II, a popular apex locator.
“My focus and emphasis is high-quality endodontics. My goal is to perform the endodontic treatment correctly so that the patient will have complete restorative success and a pain-free tooth for their lifetime,” says Dr McIntyre, adding that this is why she has invested in CBCT and surgical microscopes.
Recently, the 3D technology enabled her to explain to a friend that performing endodontic treatment in their particular case was not the best option under the present conditions.
“Last week I told a friend, ‘Your tooth is actually kissing the adjacent tooth. So, if I go into it, I potentially could destroy the perfect tooth behind the one in question.’ Imagine [if I performed the root canal and it didn’t work out]? Or, if then, the patient became symptomatic on the adjacent tooth,” Dr McIntyre says. “These scenarios are why I rely so heavily on my cone beam—it is truly changing my treatment planning.
“In this example, because of what is visualized in 3D [vs 2D and cannot be appreciated fully], we realize that we must think beyond my specialty: Let’s discuss orthodontically moving the tooth [that’s] behind away from the tooth in question/adjacent so we don’t destroy both,” Dr McIntyre continues. “This is just 1 example, but I see cases like this weekly where I am so grateful for the 3D information. Explaining it to the patients when I review scans with them—‘You [the patient] are 3D, so of course it makes the most sense to have this information,’ they’re really blown away by it and really get it when they see the images/scan. I also explain that it provides me with the information to guide me where to go and to get everything right. I have no excuses because of this essential tool. The microscope is similarly valuable, as it illuminates things clearly so that I can do my best to clean inside the tooth.”
Dr Blicher adds that the improved diagnostics provided by CBCT changes the way clinicians plan treatment and steers them away from cases where an implant or extraction is a better option than endodontics.
“We used to do what we called exploratory treatment, where we’d say I’m not sure what’s happening, but let’s try it. Let’s see what happens in here,” Dr Blicher says. “Now, because of CBCT, we’re not doing exploratory treatment because we know ahead of time about a fracture or resorption where the tooth has to come out instead.”
She notes that a published study had clinicians look at periapical images and make a diagnosis and create a treatment plan based on those images. When these same clinicians were given CBCT images for the same cases, their diagnosis and treatment plans changed 60% of the time.1 That “totally applies” in her practice, so the very first thing she does when walking into a patient room is look at her cone beam scans.
“I don’t even want to do an exam before I’ve seen that image,” Dr Blicher says. “If you don’t have that information and it’s out there, you’re missing something.”
Further, CBCT imaging allows clinicians to be more efficient with treatment based on its abilities to identify root anatomy. “If I’m doing the treatment, I have my road map. I tell my patients, this is my GPS,” Dr Blicher says. “It allows me to be extremely efficient with treatment itself.”
The information provided to endodontists from the use of cone beam can really have an impact on both the treatment and on case selections.
“Reception-wise, we can inform retreatment patients,” Dr McIntyre says. “We want to figure out why it failed the first time—there may be a missed canal or a fracture. We explain that they may be able to save their money and put it elsewhere if [redoing the] root canal is not possible. But, with 2D only, that’s not discernible and can end up wasting patients’ resources. That’s really the priceless value in having that information. And when I perform a retreatment, I can say confidently that I did my best. I cleaned everything out. I didn’t leave anything behind.”
Dr McIntyre has used DEXIS CBCT since opening Hopkinton Endodontics in 2016. She shares her cases on Instagram and has been surprised by the compliments—not just from the dental community, but from other endodontists. She’s proud that her colleagues find her images clear and are impressed by DEXIS’ clarity. “They can recognize that DEXIS’ technology is better than what they may be viewing,” she says. “I get many compliments from peers, and that says a lot. I’m honored.”
Patient Communication and Case Acceptance
Clinicians not only now have access to more information and better scans to perform endodontic care, but they can show these detailed scans to patients to educate them and to illustrate just what is going on with their teeth.
For Rebekah Lucier Pryles, DMD, who practices with Dr Blicher in Vermont, having the information provided by CBCT scans is a big deal for both the clinicians and the patients ahead of treatment planning and performing care.
“Cone beams have really caused a huge paradigm shift in endodontic diagnosis and treatment planning,” says Dr Pryles, who, together with Dr Blicher, cofounded Pulp Nonfiction Endodontics, a continuing education collaborative. “When we’re treatment planning for our patients with this technology, we’re not getting into cases where there are fractures or that have other comorbid conditions that could lead to failure. We know so much more from the beginning with a cone beam that we’re saving our patients a lot of time and heartache and treatment time as well, and that’s been wonderful.”
Once you take advantage of what CBCT has to offer, it’s difficult to practice without it on any cases, Drs Pryles and Blicher state.
CBCT systems, such as the 3D Accuitomo 170 from J. Morita, provide details not previously available to clinicians, which is having a big impact on diagnosis and treatment planning today.
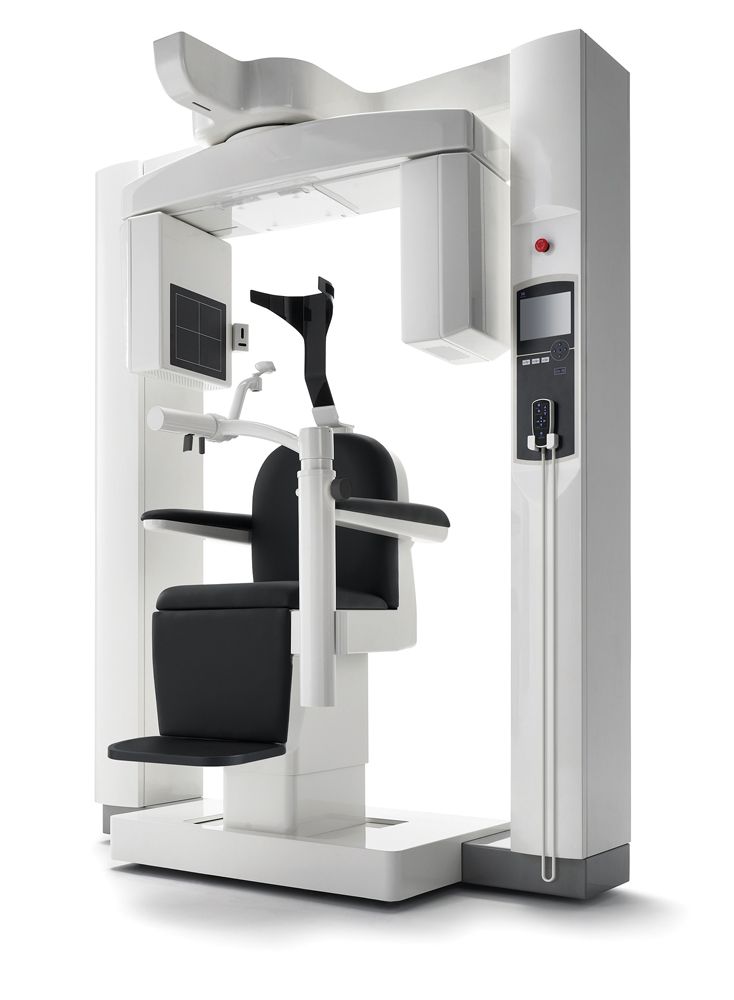
“I review each scan with every patient,” Dr McIntyre explains. “Some people are referred to me [who] don’t have any pain. So, this can be tricky. When I show them, ‘Look at this, this is your infection,’ [it often makes an impact]. It’s been eye-opening. [Dentists have] been pointing to x-rays with patients for almost 20 years, [but] I don’t think patients realize what we’ve been trying to show them on 2D films—I can’t help but wonder if they’ve kindly been nodding in the past. But with CBCT imaging, clinicians can show their patients exactly what is going on inside their mouths and with their root canals, when present.
“I’ve noticed that some patients really are impacted when I share their volume rendering and show them different views; they’re like, ‘Oh, that totally looks like me, and l get it.’ When I show them their periapical lucency, they can appreciate it much better than on 2D and, again, they’re really impacted; they see the infection in their skull/jawbone,” says Dr McIntyre. “Back to my friend, I could show the teeth touching and explain why I’m hesitant to proceed. The volume rendering really clearly points out what I’m trying to convey to them in 3D—they get it.”
Everyone Benefits
As advances in care continue to evolve, patients and clinicians reap the benefits. Patients are getting better, less painful endodontic treatments, clinicians are more confident and successful, and the success stories are rewarding.
“Over the past 10-plus years, cone beam CT has skyrocketed in popularity in the dental industry. It has revolutionized how dentists treatment plan, diagnose, and acquire patient data,” says Ryan M. Walsh, DDS, MS, a member of Catapult Education. “This point-of-service imaging is comparable with imaging modalities that used to be limited to hospitals and imaging centers. With the prices for these machines dropping as the technology becomes more affordable, CBCTs are becoming an integral part of many [clinicians’] everyday practice.”
Dr Walsh, a diplomate of the American Board of Endodontics and endodontist/owner of Advanced Endodontics of Texas, also points out how safe today’s CBCT units are. With the low-dose radiation, often equivalent to a few hours spent in the sunlight or on a short regional flight within the US, he is now able to acquire high-resolution imaging.
“The days of digging around to find an MB2 are gone, and the new frontier of pretreatment CBCT to identify canal anatomy is here,” he says. “The CBCTs of today are critical for diagnosing cracks and fractures and other common pathologies. Manufacturers like Carestream, J. Morita, and PreXion offer CBCT units that also have a variety of field of view [FOV] choices. As an endodontist, I can use the 5 x 5-cm FOV to home in on a particular tooth of interest, but I can also expand to 8 x 8-cm to scan multiple teeth for a detailed and extensive exam without the need to stitch images together. One machine can truly serve all of my needs without needing to compromise.
“Outside the endodontic perspective and locating individual canals, clinicians are able to more accurately implant plan,” Dr Walsh adds. “It’s now possible to utilize integrated software to plan an implant with the patient in the chair. I can send a copy of the scan—either digitally or via CD/thumb drive—to a referring [general practitioner] or specialist to aid the patient in planning their next restoration,” he says. “Ten years ago, this just wasn’t possible. That same CBCT I initially made to aid endodontic diagnosis can be used for implant planning and can be translated, through 3D printing software, to make a surgical guide…all from the same low-dose scan. This type of technological revolution is amazing and only continues to improve.”
Dr McIntyre is equally wowed by the wealth of information CBCT can provide. “In the past, some patients might return to the dentist or endodontist reporting that a root canal may still be bothering them, or a tooth without any endodontic treatment. Historically, we’re looking at an x-ray, or you’re looking under the microscope, and you just don’t know and/or cannot see anything that could possibly still be bothersome,” she says. “You tell the patient, ‘Sorry, I don’t see anything.’ But with cone beam, I can factually share with them, this is all of you. It’s the only version. Other than bacteria or hairline fractures, you’re confidently sharing with them that something is there or is not. It provides more confidence.”
Dr Blicher is glad she practices in a time where CBCT, surgical microscopes, advanced rotary instrumentation, and other developments make providing root canals far less scary and far more predictable than in the past.
“The cone beam is huge for treatment planning as far as case selection goes. I love that I practice in a time and in a community where I have great surgeons doing really nice implant work, as well. We don’t have to get into heroics—cases where you know this isn’t going to work. It’s nice to know that there’s other options out there besides endodontics,” she says.
Dr Pryles is glad that all of the newer technologies available are helping change the way many patients feel about the “dreaded” root canal. Her practice has used Carestream CBCT for years now and loves the resolution of the scans.
“I would also argue that most of the fun of being an endodontist is getting to change patients’ misperceptions about endodontics,” she adds. “With the technology, and with the anesthetics that we have these days, the care can be painless and efficient, and providers are really kind. So it’s not unusual for us every day in the office to hear patients say what I worked on has been terrible previously, but that this was one of the better dental experiences they’ve ever had. That’s really gratifying to hear. It was so often maligned.”
Again, the information is invaluable, especially when it comes to determining which cases to take on and then figuring out the best treatment plan.
“Knowing which cases might be hopeless from the beginning is going to save your patients and you a lot of time and a lot of heartbreak,” Dr Pryles adds. “Cone beams, especially, can help us do that. It’s a really illustrative tool. And for us to have it up on the screen and be able to walk a patient through exactly what we’re seeing and why it’s going to impact their care…you can just enhance a patient understanding and make sure everybody’s on the same page.”
Reference
1. Ee J, Fayad MI, Johnson BR. Comparison of endodontic diagnosis and treatment planning decisions using cone-beam volumetric tomography versus periapical radiography. J Endod. 2014;40:910-6. doi:10.1016/j.joen.2014.03.002
