Although composite resins have been used successfully in restorative dentistry for decades, these materials still pose some clinical problems. Microleakage continues to be an issue, particularly at the interface between dentin and the composite resin. Chemical adhesion between glass ionomer cement and dentin has been shown to promote a better “seal” to dentin than that of adhesive resins alone.1-3 This fact led to the development of the so-called sandwich technique, in which glass ionomer cement is used as a lining under composite resin restorations, particularly where the cavosurface margin is in contact with dentin.4 The weak link has always been the composite portion of the “sandwich” restoration.
The biological assault on composite materials can vary due to the individual’s oral environment (pH), quality and quantity of saliva, and acidic challenge to natural tooth structures and restorative materials, as well as the patient’s ability to keep tooth surfaces plaque-free. However, some of today’s resin-based restorative materials actively release and recharge mineral ions, a significant improvement over traditional passive materials that merely fill the prepared cavity after caries removal. This case report will demonstrate the use of bioactive and other mineral-enriched materials that may be an improvement over the use of glass ionomer materials as dentin replacements capped with a conventional passive composite resin.
Bioactivity in Modern Dental Materials
Bioactivity is only possible in the presence of water. According to McCabe et al, “the potential for dynamic behavior exists with materials that are partly water-based, transport water, or have phases or zones with significant water content, and for which the water within the material can react to changes in the ambient conditions. Such materials have the potential for ‘smart’ behavior.”5 The availability of calcium, phosphate, and fluoride ions can facilitate conditions that stimulate mineralization and the formation of chemical bonds that help seal the tooth and prevent microleakage at the cavosurface margins of a restoration.
Activa Presto
- A universal, stackable, light cure composite that is strong, durable, wear and fracture-resistant, releases and recharges calcium, phosphate and fluoride, and is indicated for all classes of cavities
- The white dental filling material is said to mimic the properties of natural teeth
- The material is esthetic, high-strength, and contains no Bis-GMA, Bisphenol A, or BPA derivatives
- Its chemistry is designed to penetrate and integrate with tooth structure for margin-free adaptation
Pulpdent Corporation
800-343-4342 pulpdent.com
Activa BioActive-Restorative from Pulpdent Corporation is a moisture-friendly bioactive material that supports natural remineralization by releasing calcium, phosphate, and fluoride and contains a rubberized resin component that acts as a shock absorber, much like natural dentin. Activa Presto is the first light cure, mineral-enriched composite that mimics the properties of natural tooth structure. This material also has the esthetic quality to match nano and microhybrid composite materials and can be used for all anterior and posterior applications.
The following case demonstrates the sandwich technique using Activa BioActive-Restorative as a dentin replacement and Activa Presto as an enamel replacement.
Clinical Technique
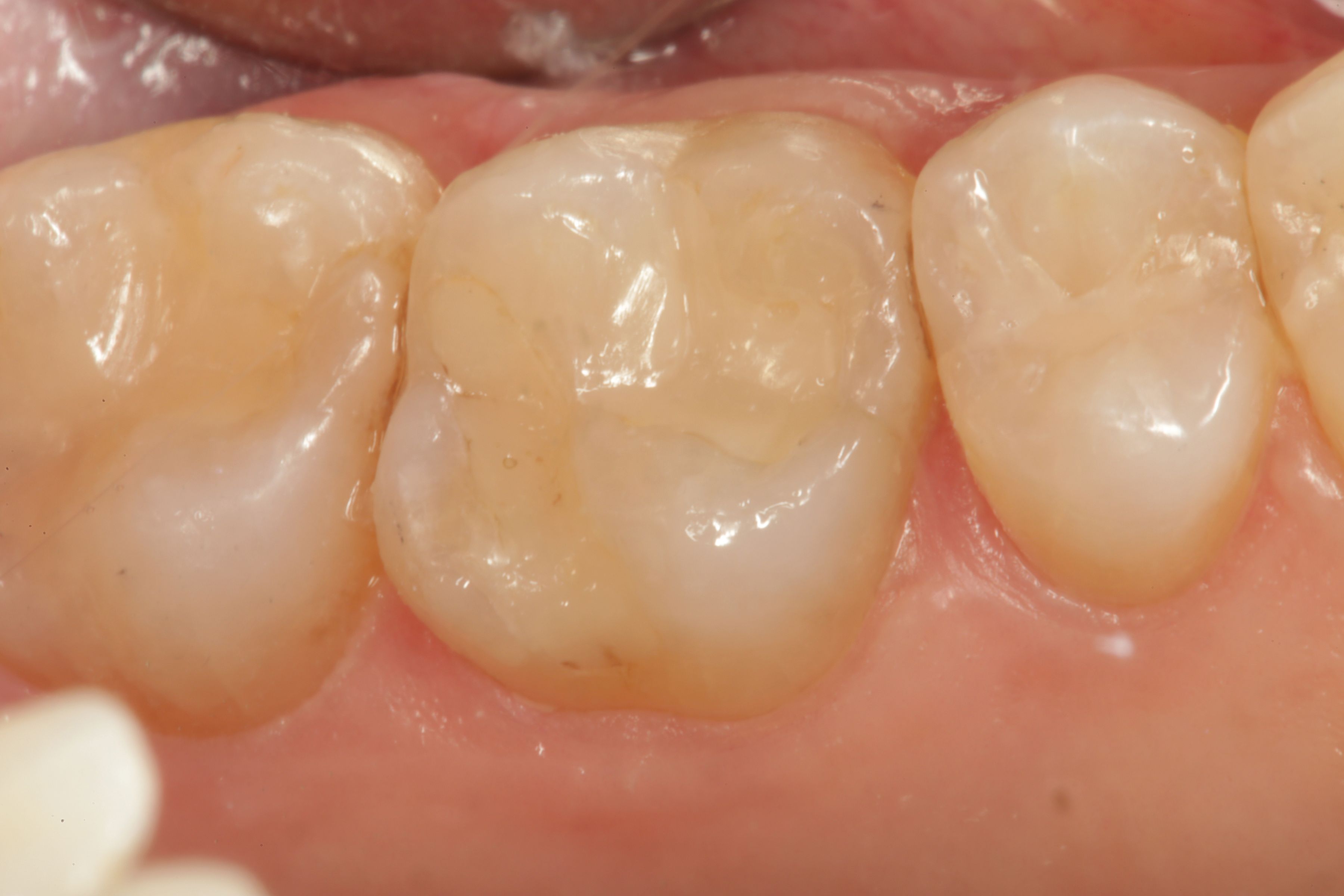
In the following case, a patient who is unable to afford a crown receives a direct restoration using bioactive materials. Figure 1 is a preoperative occlusal view of tooth No. 3 showing marginal failure in the area of the existing restoration near the mesial marginal ridge. A portion of the mesial margin has been compromised due to fracture, and recurrent decay was diagnosed using quantitative laser fluorescence and verified clinically.
Caries detection with SoproCare from Acteon shows active caries lesion around a defective restorative margin on tooth No. 3 (Figure 2). Decay is visible upon removal of the defective restoration (Figure 3), and a Smart Burs II from SS White Dental is used to remove infected dentin only. Affected dentin (ie, demineralized dentin) can be restored with the calcium and phosphate made available by using Activa BioActive-Restorative as the dentin replacement.
Once infected dentin removal is complete, the preparation is etched with Etch-Rite 38% phosphoric acid from Pulpdent Corporation for 15 seconds and rinsed well. Excess moisture is removed using high-volume suction so the etched dentin is not overdried and desiccated.
An adhesive resin is applied to the dentin surface, air thinned, and light cured. It is important to note that the presence of an adhesive resin does not affect the ability of ions to diffuse from Activa BioActive-Restorative to the demineralized tooth (dentin) surface. Studies by Sauro et al6 and others show that calcium, phosphate, and fluoride ions pass through the bonding agent and deposit apatite crystals, which help prevent the degradation of the adhesive bond.
Next, Activa BioActive-Restorative is placed in the cavity and light cured, leaving approximately 1 to 1.5 mm for the final layer of restorative material (Figure 4). Activa Presto was chosen for the enamel replacement because it is a mineral-enriched universal composite material with a stackable viscosity that holds its shape. Its calcium-and-phosphate component and shock-absorbing ability mimic the properties of natural teeth.
The moisture-friendly resin facilitates the release and recharge of these essential tooth-building ions and creates nucleation sites and an environment favorable for both apatite formation and marginal seal. After light curing, Activa Presto is highly polishable and maintains its luster. Figure 5 is an occlusal view of the completed restoration on the occlusal surface of tooth No. 3.
Conclusion
An updated version of the sandwich technique has been demonstrated using materials that can help support the natural rebuilding process of diseased tooth structure. Although they provide fluoride to convert heathy apatite to fluorapatite, glass ionomers do not have calcium and phosphate availability to restore affected dentin back to a healthy, remineralized condition.
References
1. McLean JW, Wilson AD. Fissure sealing and filling with an adhesive glass-ionomer cement. Br Dent J. 1974;136(7):269-276. doi:10.1038/sj.bdj.4803174
2. McLean JW. Evolution of glass-ionomer cements: a personal view. J Esthet Dent. 1994;6(5):195-206. doi:10.1111/j.1708-8240.1994.tb00860.x
3. Ngo HG, Mount GJ, Peters MC. A study of glass-ionomer cement and its interface with enamel and dentin using a low-temperature, high-resolution scanning electron microscopic technique. Quintessence Int. 1997;28(1):63-69.
4. Mount GJ. Clinical requirements for successful “sandwich”—dentine to glass ionomer cement to composites resin. Aust Dent J. 1989;34(3):259-265. doi:10.1111/j.1834-7819.1989.tb00680.x
5. McCabe JF, Yan Z, AI Naimi OT, Mahmoud G, Rolland SL. Smart materials in dentistry. Aust Dent J. 2011;56(suppl 1):3-10. Doi:10.1111/j.1834-7819.2010.01291.x
6. Sauro S, Makeeva I, Faus-Matoses V, et al. Effects of ions-releasing restorative materials on the dentine bonding longevity of modern universal adhesives after load-cycle and prolonged artificial saliva aging. Materials (Basel). 2019;12(5):722. doi:10.3390/ma12050722