How to simplify temporaries with Tuff-Temp Plus
A prosthetic reconstruction for oral rehabilitation requires a number of clinical and laboratory treatment stages. An interim restoration is necessary and this has a crucial influence on the patient’s well-being, the quality of the final restoration and the long-term success of the treatment. A prosthetic reconstruction for oral rehabilitation requires a number of clinical and laboratory treatment stages.
A prosthetic reconstruction for oral rehabilitation requires a number of clinical and laboratory treatment stages. An interim restoration is necessary and this has a crucial influence on the patient’s well-being, the quality of the final restoration and the long-term success of the treatment.
Essential factors for success in fabrication of fixed restorations include making anatomically correct and hygienic temporaries. Temporary fixed restorations serve to protect the underlying tooth preparation while the final restoration is being fabricated in the laboratory.
In recent years, many new materials have been marketed for temporary restoration of crowns, bridges, inlays, onlays and other fixed dental prostheses.
Materials for temporary restorations must meet various criteria: color stability, price, heat generation, smell, putty-phase, rubber-like nonstable phase, reparability, shrinkage, material stability, taste, processing, wear and surface quality. Until recent years, the different materials on the market could be divided into two main groups: traditional acrylics and bis-acryls.
Step-by-step technique: How to perform bioactive restorations using a "stamp" technique
Conventional materials
Traditional acrylic resins have been on the market a long time, mainly as PMMA (powder/liquid), but for years these have been more or less replaced by bis-acryl composites (cartridge systems, paste/paste). Both groups certainly have their merits. PMMAs are inexpensive, and when used correctly, the rubber-like phase that occurs during curing is a major advantage, especially when removing the rough temporary from the tooth stumps. The familiar disadvantages include relatively high heat generation, flammability, shrinkage, brittleness, odor and the need for experience in working with the material.These factors have led to the use of bis-acryl materials, which are now often preferred by practitioners for their aesthetics and ease of use.
A disadvantage of the conventional bis-acryl materials is the lack of flexibility after initial hardening, making them difficult to remove, especially from undercut preparation areas. They are also brittle. When removing them after they have been in place for some time, e.g., for a try-in, the brittleness often results in fractures, especially of temporary bridges, thus necessitating time-consuming repairs or re-makes.
Trending article: A close look at how Pulpdent's ACTIVA BioACTIVE material was created
New materials
Tuff-Temp Plus (Pulpdent), which is formulated on the basis of diurethane dimethacrylate, a new category of composite resin temporaries, has recently been available. This new temporary material is not a bis-acryl and is free from BPA (Bisphenol-A), bis-GMA, BPA derivatives, HEMA and TEGDMA.
The clinical technique for Tuff-Temp Plus is the same as for bis-acryls. The material is both self-cure and light cure (dual cure) and is dispensed through a mix tip from a double-barrel cartridge or syringe. The chemical composition, however, is different from bis-acryls. A patented synthetic rubber molecule is incorporated in the molecular chain of diurethane dimethacrylate base material, creating a rubberized-urethane that absorbs stress and shock and resists fracture and chipping. The physical properties of the material are greatly improved and, in particular, bending in mm before breaking was increased to 2.9 mm, which is significant when compared with conventional bis-acryl and methacrylates.
Tuff-Temp Plus has compressive strength of 205 MPa (±18 MPa) and flexural strength of 84 MPa (±4 MPa). Due to this flexural strength, the material is less brittle and more resistant to breaking, and the compressive strength with regard to occlusal function is increased compared with bis-acryl. Tuff-Temp Plus can therefore be used for long-span composite bridges as well as for one-piece temporary restorations. The optimised plastic matrix of the filler also contributes to reduced shrinkage and greater elasticity, aspects that are proved to lead to better retention. The Tuff-Temp Plus material is dual-curing and can therefore be light-cured as soon as the restoration is removed from the mouth.
Trending technique: How to easily perform quick, effective restoration with ACTIVA BioACTIVE
Clinical procedure
Tuff-Temp Plus is a dual-curing composite resin for temporaries that can therefore be used as self-curing or light-curing, if desired. Temporary restorations can be fabricated in the mouth or in the dental laboratory. As soon as the two pastes are combined in the double-barrel automatic mixing system, a polymerisation reaction takes place.
The paste is liquid in the first phase and can be worked for 45 seconds using a template. The paste adapts to the tooth preparation and becomes elastic within 120 seconds after application from the syringe (initial curing time). In the second phase of the polymerisation reaction, the material can either cure on its own for two minutes and 45 seconds or it can be light-cured to speed up the curing process.
After this final polymerisation phase, four minutes and 45 seconds after the start of mixing, the material has attained its final hardness, and the restoration can be adjusted.
Continue to page two to see the step-by-step procedure.

Case study
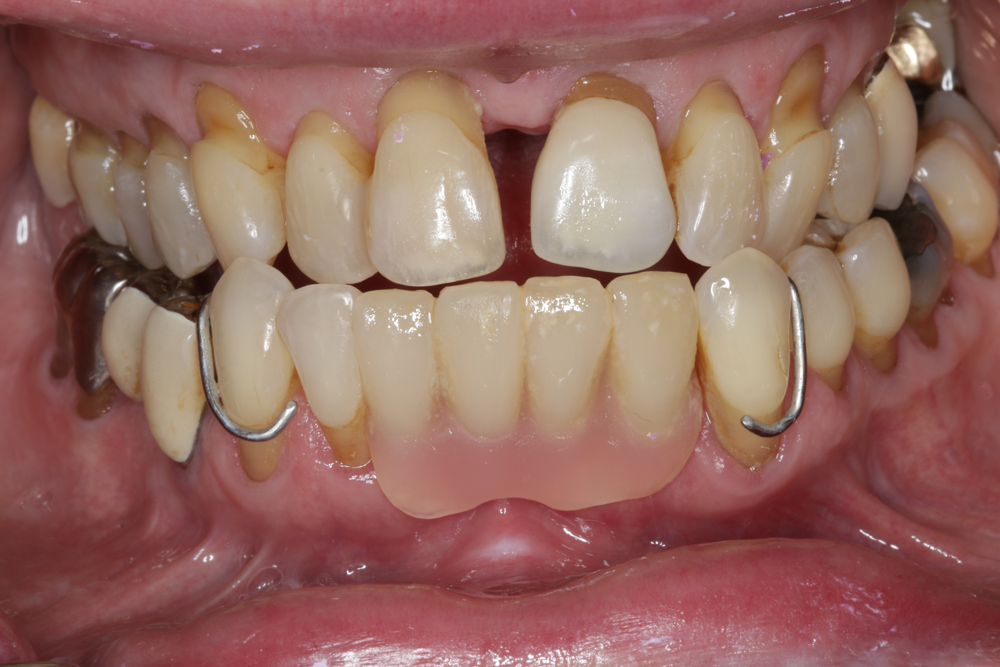
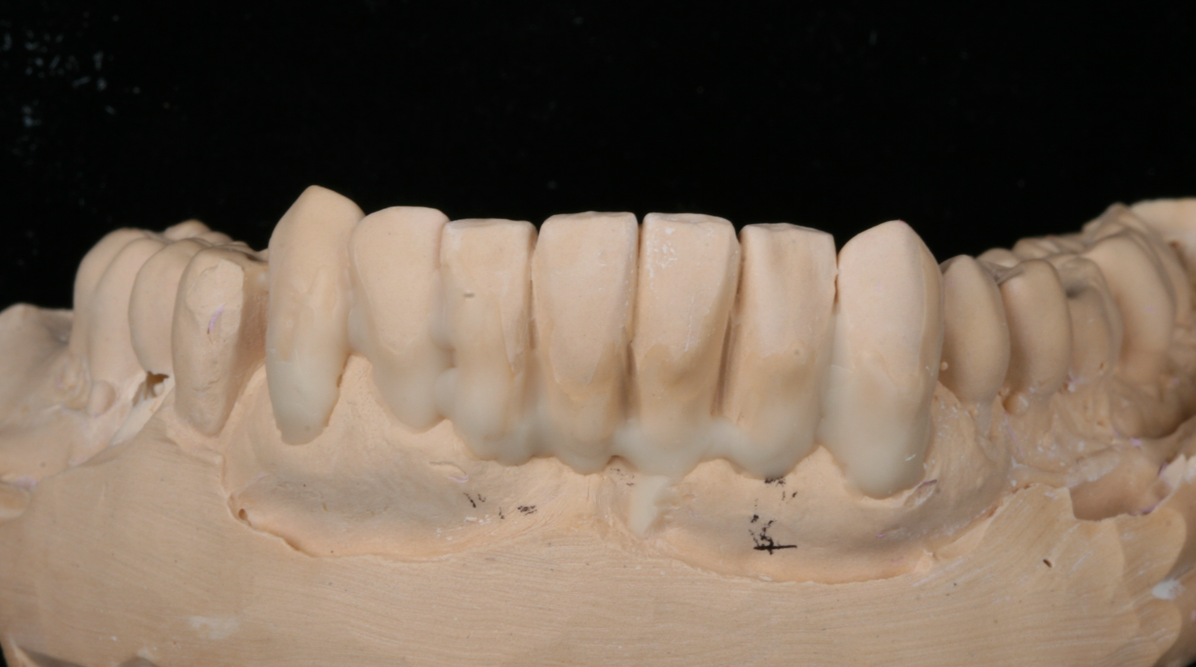
Fig. 1: Patient presented with lower anterior removable denture. Fig. 2: Stone model is poured and composite is added to the cervical area
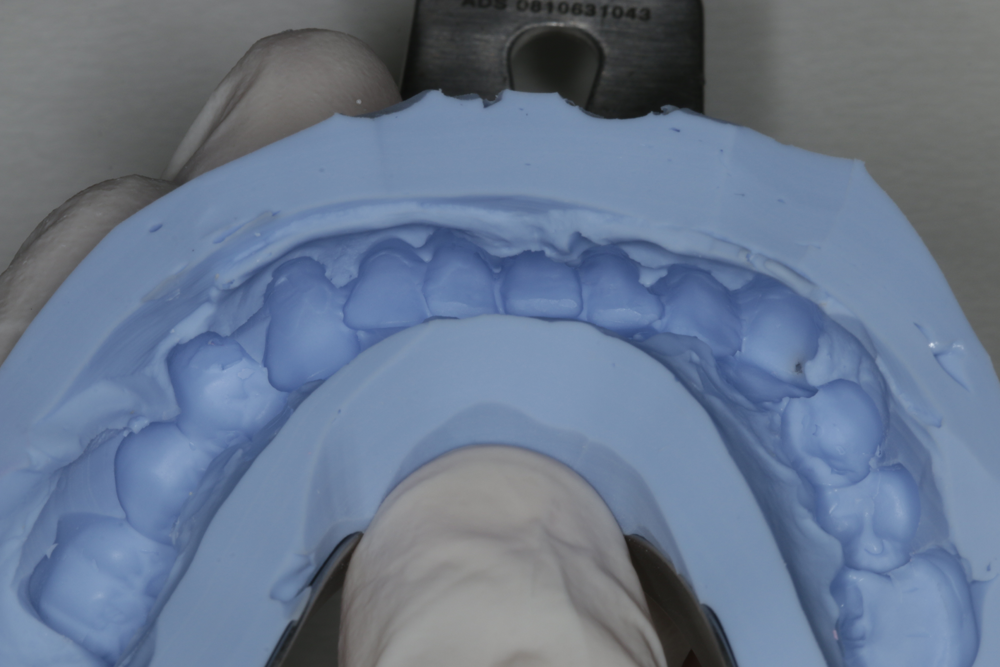
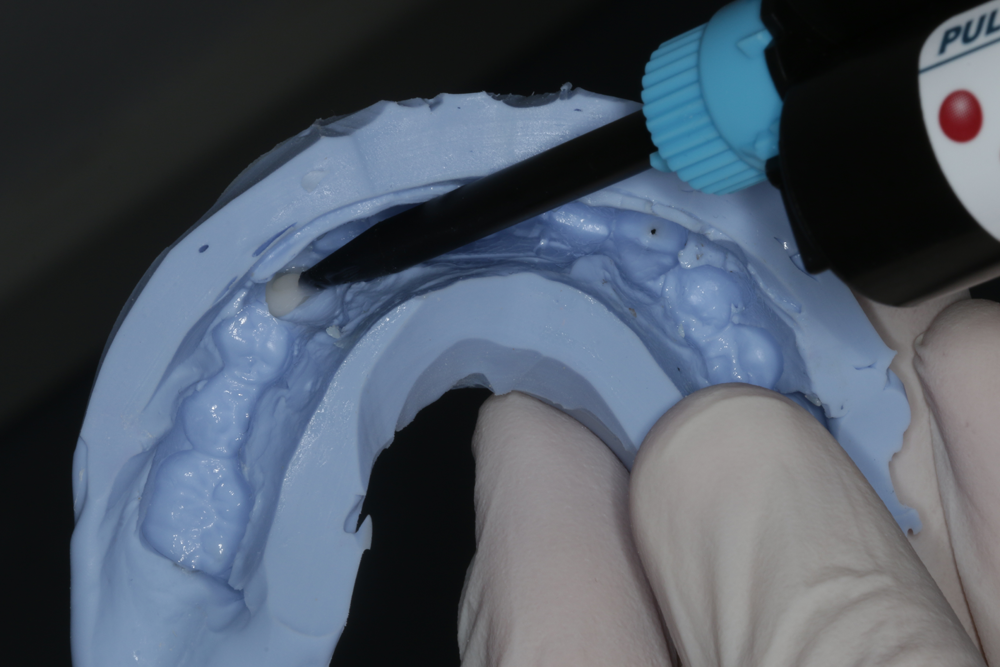
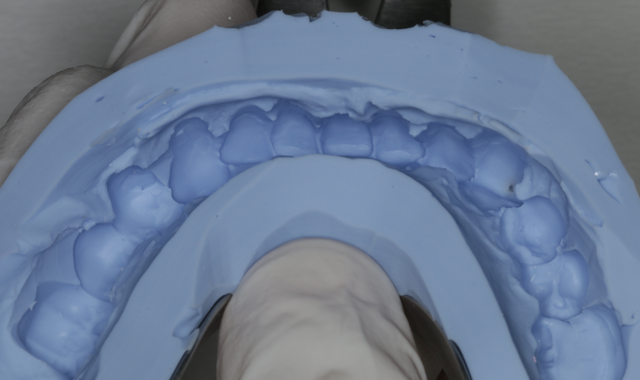
Fig. 3: A silicone dental mold is made over the prepared model. Fig. 4: Tuff-Temp Plus is carefully applied to the incisal edge of the matrix. By first dispensing a small amount of material into the entire incisal area before filling in the rest, bubbles and voids in the incisal area are prevented. Filling should be done quickly.
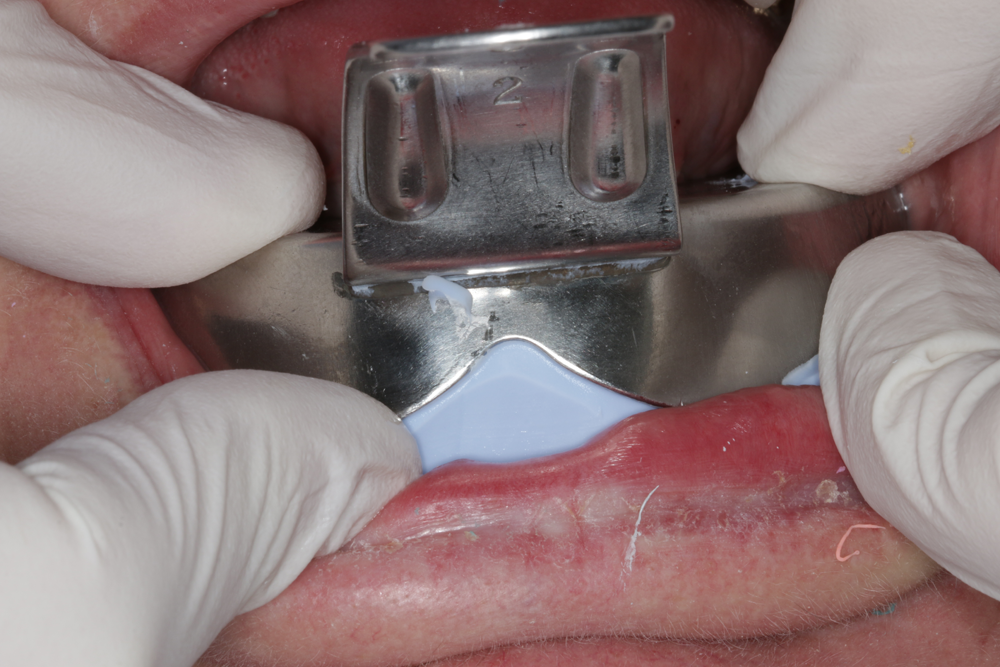
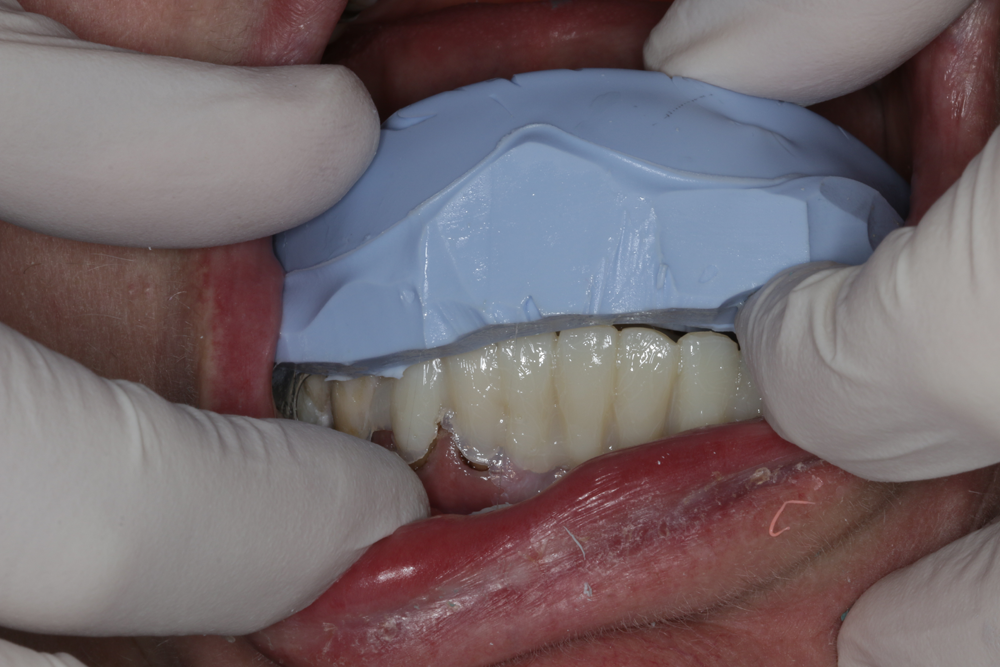
Fig. 5: The matrix is placed over the anterior arch and held in position for 90 seconds. Using an impression tray prevents distortion during the initial curing phase. Fig. 6: Remove the impression tray and gently lift the silicone mold upwards.
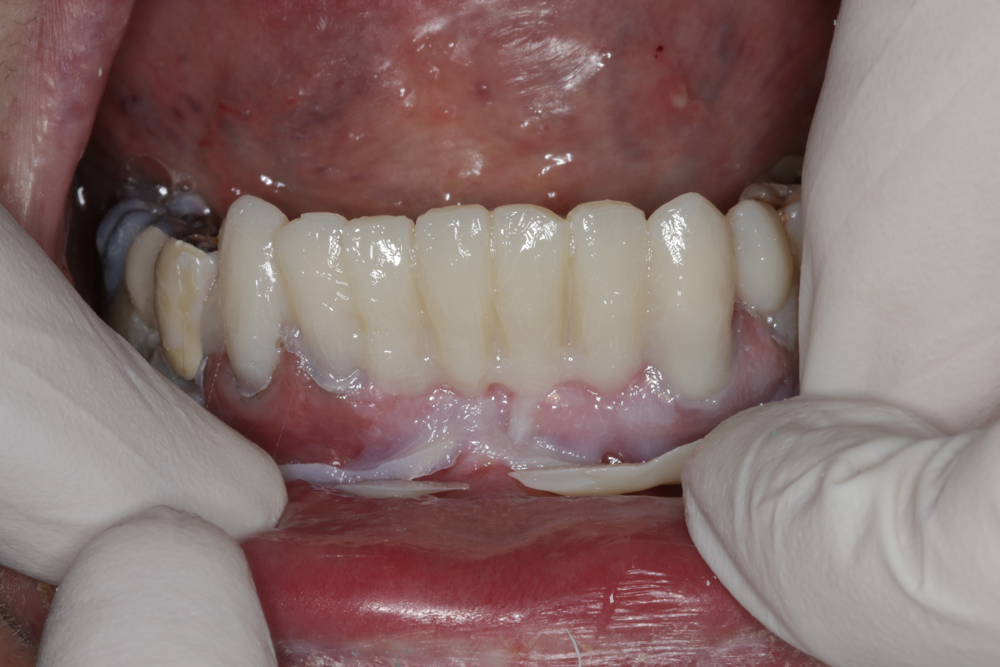
Fig. 7: The surface quality is already outstanding. Carefully remove the rough temporary prosthesis for shaping and finishing.
Next: The conclusion of the case.


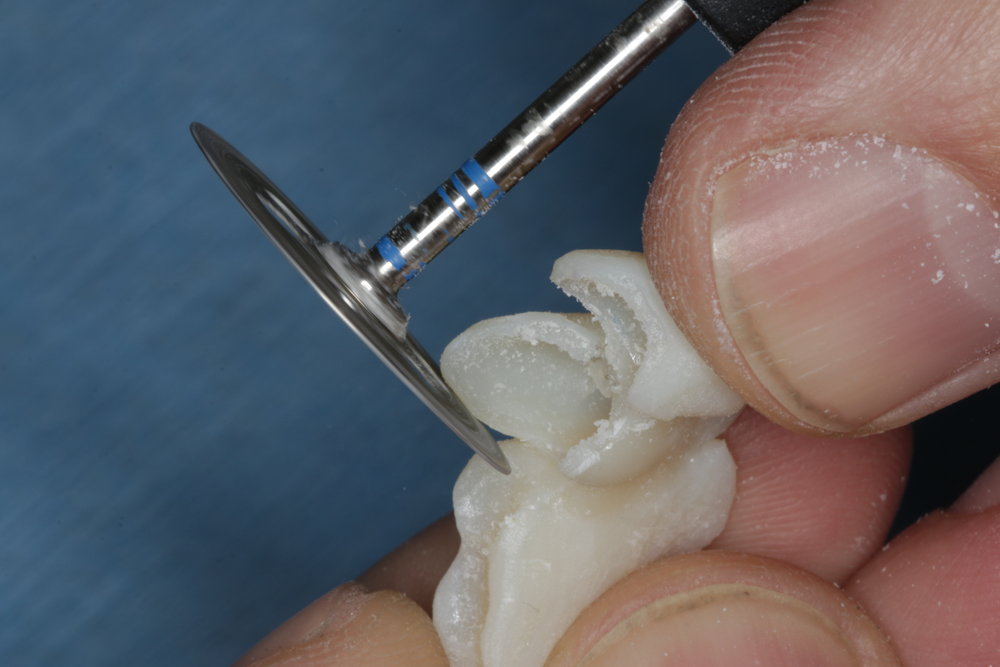
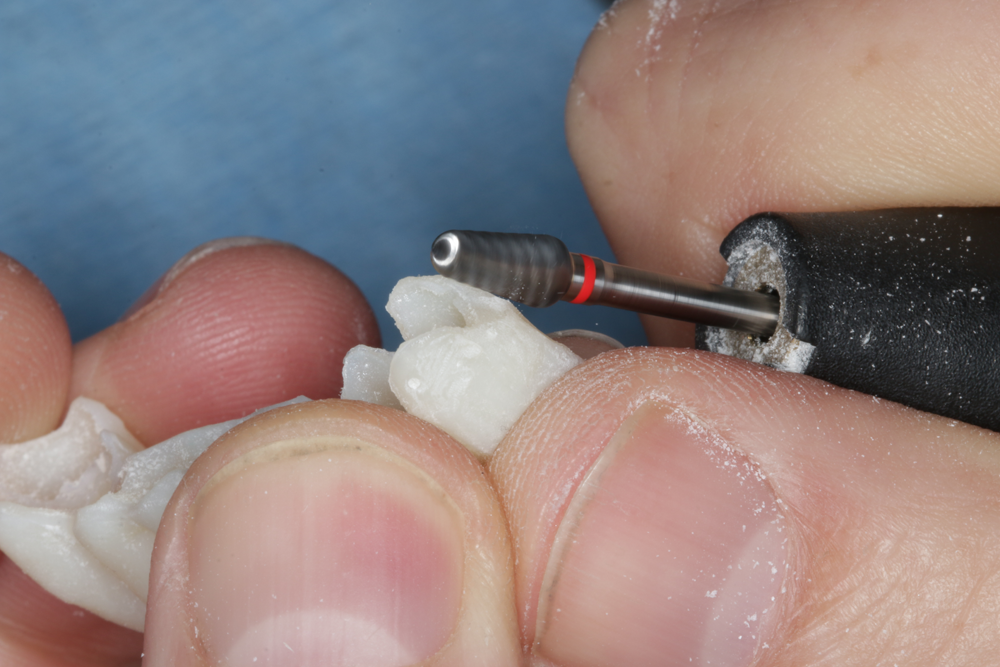
Figs. 8-9: Tuff-Temp Plus can be shaped and finished using conventional instruments. We recommend using carbide dental burs and diamond-impregnated disks.
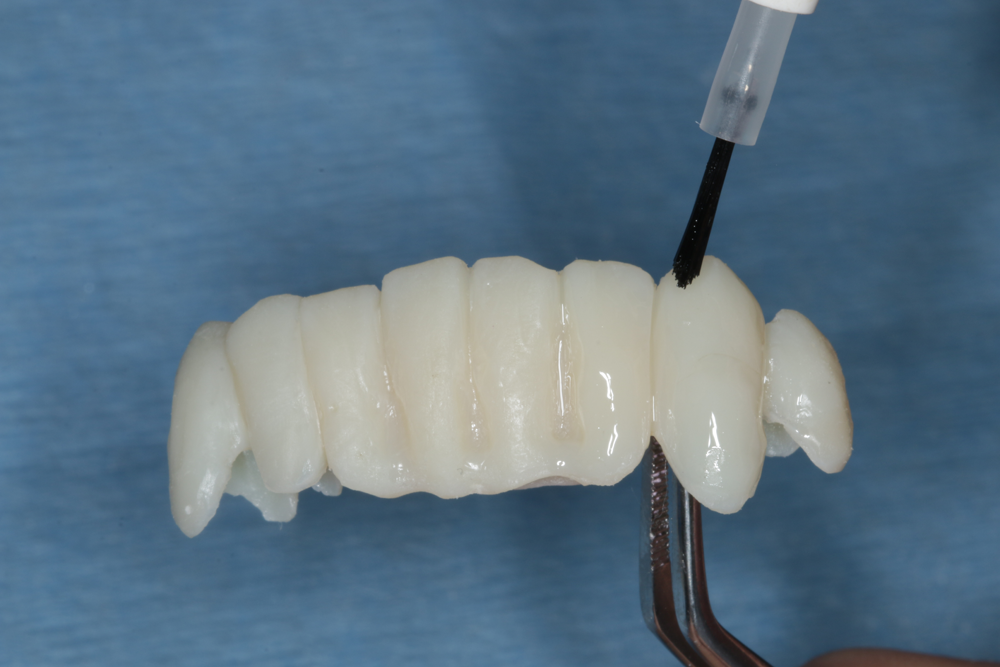
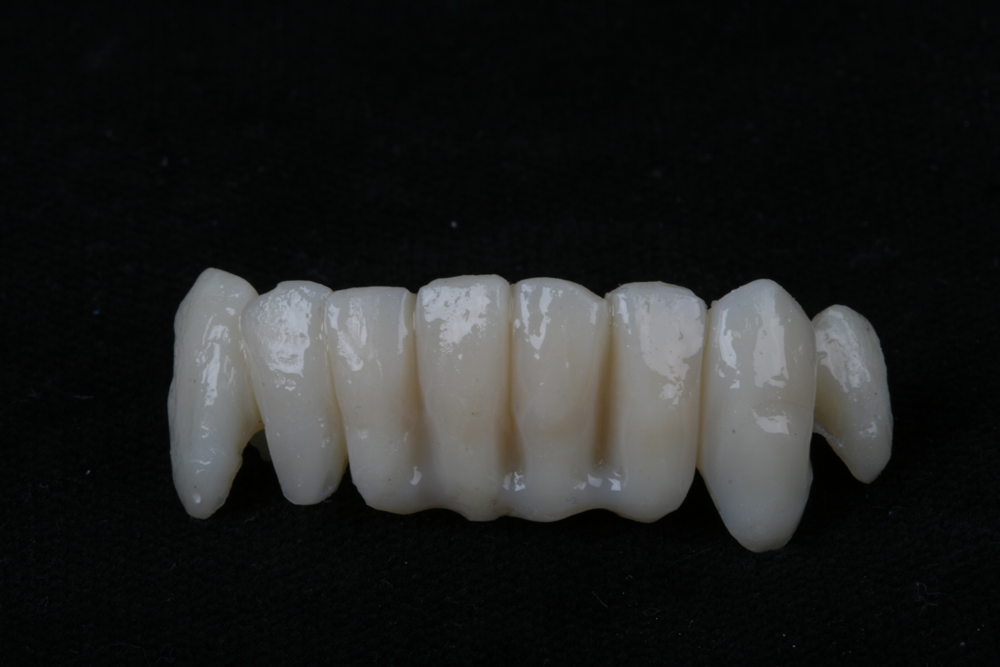
Figs. 10-11: After finishing, apply Tuff-Temp Glaze and light cure for a long-lasting high-gloss finish.
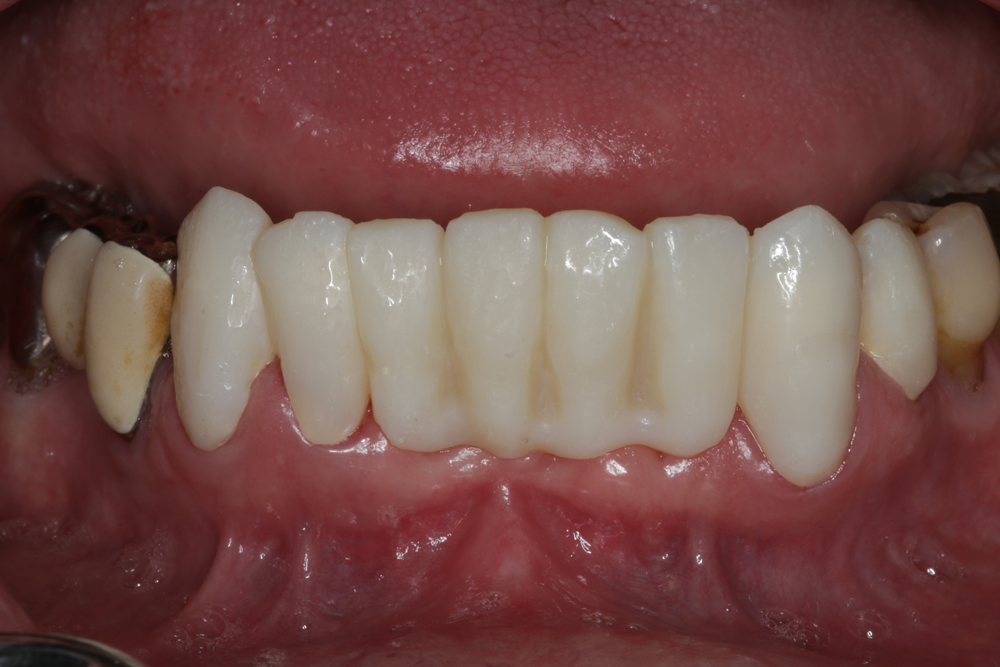
Fig. 12: The surface quality of the temporary prosthesis after several weeks. The tough provisional can be removed multiple times without fracturing, e.g., for trying on the final dental prosthesis.
Trending article: How and why to use ACTIVA BioACTIVE-CEMENT for crown cementation
Conclusion
With the techniques described in this article, a dentist can reduce the treatment time by nearly 30 minutes compared with the use of self-curing acrylic resin for temporary crowns and bridges. These techniques will offer dentists the possibility of fabricating high-quality, well-fitting, durable temporary restorations that are more esthetic than conventional acrylic resins.
Compared with the temporary materials on the dental market based on bis-acryl and methacrylates, Tuff-Temp Plus provides tight-fitting temporaries with high flexural strength and without brittleness. This is shown by the very good deflection at break test results in mm of the material before breaking, which is up to 100-percent higher than results obtained with bis-acrylates.
