How to simplify composite decisions [VIDEO]
The first resin-based light cured dental composites were introduced in the 1970s. Since that time significant advancements have been realized in resin and filler technology, and today more than 70 different brands of composite exist on the market.
The first resin-based light cured dental composites were introduced in the 1970s. Since that time significant advancements have been realized in resin and filler technology, and today more than 70 different brands of composite exist on the market.
Practitioners are faced with ever-increasing composite choices that are designed to give better results during placement and over the lifespan of the restoration.
Today’s clinicians may be easily confused about the subtle differences between the many available composite materials and some find it more difficult to make the correct decision about which material is best for each clinical situation.1
Choosing which composite material to purchase can be a difficult decision. Ideally, practitioners should rely on published reports and a careful review of a product’s physical properties when selecting a material, however, this level of review is generally not realistic for everyday providers.
Dentists’ purchasing decisions may be based on cost, brand preference, and the “works best in my hands” argument, rather than a strict review of each product’s fracture toughness, volumetric shrinkage, or other properties.
Clinicians become more confident in their procedures and materials through repetition of use and clinical observations. This is especially true when considering material choices: exacting use of poorly selected materials will not offer better clinical results than use of ideally chosen materials.2
To simplify decision-making and to offer a composite that can ensure excellent performance in all clinical situations, DENTSPLY Caulk has introduced TPH Spectra Universal Composite.
This new composite is based on the resin technology of TPH3 and contains nanohybrid- and micro-filler components. The result is a composite that has the potential to perform well in either the anterior or posterior, and should have tooth-like translucency, improved polishability and color stability, and good wear resistance.3,4,5
TPH Spectra also comes in two handling choices: a creamy light-viscosity formulation, and a packable high-viscosity formulation. For both viscosities the physical properties are similar. Because handling preference is subjective and highly individualized, practitioners are now able to select the right viscosity for all clinical situations.
To make shade selection simpler, TPH Spectra is available in the seven most popular shades: B1, A1, A2, A3, A3.5, A4, and C2. According to DENTSPLY’s internal data, the seven shades of TPH Spectra represent more than 80% of total sales from the previous TPH3 formulation.6
The TPH Spectra shade guide was condensed for several reasons. First, some practitioners may be overwhelmed with the number of current shades; the Vita Classic (Vident) shade guide has 16 shades, and the TPH3 shade guide has 26. Because only seven of the current TPH3 shades are regularly purchased, the color difference (i.e., Delta-E value) between shades was calculated to determine if a top-seven shade could be used in place of another shade not offered.
TPH Spectra also offers excellent color blending between restorative materials and natural tooth, often called “the chameleon effect.” Again, building and improving from the previous TPH3 composite formulation,
TPH Spectra has a refractive index that falls directly between enamel (1.63) and dentin (1.54).8,9 Because of TPH Spectra’s excellent translucent properties and an appropriate refractive index similar to natural tooth structure, it will have an excellent chameleon effect and create undetectable restorations.
Case 1
Intraoral exam reveals a cavitated lesion on the disto-facial surface of tooth No. 8 (Figs. 1-2). The patient was experiencing no pain but was displeased with the esthetics of the tooth. After verifying the medical history and reviewing the radiographs, a direct composite resin restoration of the disto-lingual-facial surfaces was treatment planned.
Anesthesia was achieved with one carpule of 2% Xylocaine© with 1:100,000 epinephrine via buccal infiltration. Caries excavation was completed using a 330 carbide bur on a highspeed handpiece and a #4 round bur on a lowspeed handpiece.
The preparation was verified caries-free with Snoop caries detector (Pulpdent Corp.) (Figs. 3-4 ). A facial bevel was placed with a football shaped diamond bur to increase retention and facilitate shade matching and blending.
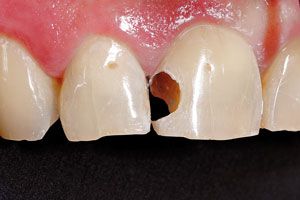
Fig. 3 // After caries excavation (frontal view)
Because of the depth and size of the final preparation, a selective etch technique with DENTSPLY Caulk’s Prime and Bond Elect was used. This technique was chosen to maximize enamel bonding while minimizing the potential for post-operative sensitivity.10,11
The enamel was etched with 34% phosphoric acid for 20 seconds and then rinsed (Fig. 5). Prime and Bond Elect was scrubbed into the preparation for 20 seconds followed by a 5-second air drying to remove the solvent. The adhesive was light cured for 20 seconds.
Isolation was accomplished with a mylar strip and Wizard wedge (Waterpik) (Fig. 6). The patient’s shade was judged to be between A3.5 and A4 according to the Vita Classic (Vident) shade guide. TPH Spectra Low-Viscosity shade A3.5 was selected because of its creamy handling and placed in 2 mm increments.
The final restoration was finished with fluted composite finishing burs and Sof-Lex discs (3M ESPE) to achieve proper shape and contour. After occlusal adjustment, the composite was polished with Caulk’s Enhance and PoGo (Figs. 7-8).
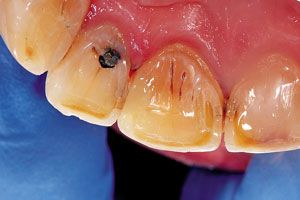
Fig. 8 // Final restoration of tooth No. 8 (lingual view)
Case 2
After the clinical exam, the patient agreed to a treatment plan that included root canal therapy on tooth No. 4 followed by a core-build using direct composite. Because of financial constraints the definitive restoration of tooth No. 4 using full-coverage needed to be postponed (Fig. 9).
After local anesthesia with one carpule of 4% Articadent© with 1:100,000 epinephrine (DENTSPLY Pharmaceutical), root canal therapy was completed conventionally and without complication (Fig. 10).
Because of the large amount of dentin present in the preparation, a selective-etch technique was again chosen. The exposed enamel surfaces were etched with 34% phosphoric acid for 20 seconds and then thoroughly rinsed with water. Isolation of the preparation was achieved using Caulk’s Palodent Plus (Fig. 11).
Prime and Bond Elect was scrubbed into the preparation for 20 seconds followed by a 5-second air drying to remove the solvent. The bonding agent was light cured for 20 seconds. An initial layer of Surefil SDR Flow was placed into the preparation, followed by a 20-second light cure (Figs. 12-13).
TPH Spectra High-Viscosity shade A2 was packed into the preparation and cured in 2 mm increments (Figs. 14-15).
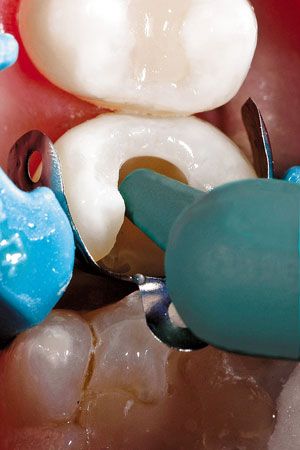
Fig. 14 // Placement of TPH Spectra HV, shade A2
The final restoration was finished with fluted composite burs and polished with Caulk’s Enhance and PoGo (Figs. 16-17).
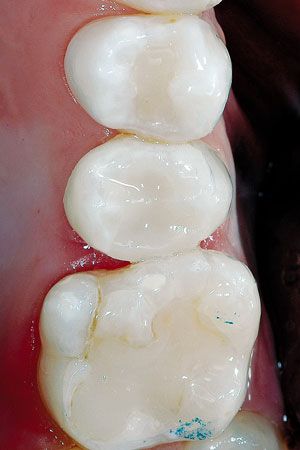
Fig. 16 // The final restoration after finishing and polishing
Closing thought
With the introduction of TPH Spectra by DENTSPLY Caulk, dentists now have one material that can be used for all situations. As a result, no longer do practitioners need to struggle with decisions of shading or selecting the material with the most appropriate physical properties. TPH Spectra’s characteristics and excellent chameleon effect will provide the dentist and patient with predictable results not only during placement at chairside but for years to come.
REFERENCES
1. Devoto W. Saraceinelli M, Manauta J. Composites in everyday practice: how to choose the right material and simplify application techniques in the anterior teeth. Eur J Esthet Dent 2010;5(1):102-24.
2. Jacob RF, Carr AB. Hierarchy of research design used to categorize the “strength of evidence” in answering clinical dental questions.” J Prosthet Dent 2000;83(2):137-52.
3. Garg N, Garg A. Tooth preparation for composite restorations. In: Textbook of Operative Dentistry. 2010. New Delhi: Jaypee Brothers Medical Publishing, pp. 260.
4. LeBlanc BJ. Nanohybrid composite restorations: dentistry’s most versatile solution. Dental Economics. Available at: http://www.dentaleconomics.com/articles/print/volume-99/issue-5/features/nanohybrid-composite-restorations-dentistry39s-most-versatile-solution.html. (Accessed January 17, 2013)
5. Vargas M. Nanomicrohybrid composites make posterior placement easier. Dent Today 2012; 31(5):128,130-1.
6. Internal DENTSPLY Caulk data on file, 2012.
7. Jaju RA, Nagai S, Karimbux N, Da Silva JD. Evaluating tooth color matching ability of dental students. J Dent Educ 2010;74(9):1002-10.
8. TPH Spectra, DENTSPLY Caulk. Using TPH Spectra. Available at: http://tphspectra.com/using-tph-spectra. (Accessed March 6, 2013).
9. Meng Z, Yao XS, Yao H, Liang Y, Liu T, Li Y, Wang G, Lan S. Measurement of the refractive index of human teeth by optical coherence tomography. J Biomed Opt 2009; 14(3):034010.
10. Ritter R. Using the selective etch technique for esthetic restorations. Inside Dentistry 2011;7(3). Available at: http://www.dentalaegis.com/id/2011/03/using-the-selective-etch-technique-for-esthetic-restorations. (Accessed January 23, 2013).
11. Perdigão J. New developments in dental adhesion. Dent Clin N Am 2007;51:333–357.
