5 steps to a pain-free dental career
These essential steps can be invaluable to preventing pain and ensuring career longevity.
Pain is not a necessary by-product of dentistry - you can reduce or eliminate your pain with evidence-based interventions.

Effectively resolving work-related pain in dentistry requires correctly identifying the risk factors and then targeting those risk factors with specific, evidence-based interventions. Due to the multi-factorial nature of work-related pain, rarely does a single intervention (i.e. purchasing a new set of loupes, strength training, etc.) permanently resolve pain issues.
Related reading: 5 ergonomics tips that could save your career
It is also important to know the proper sequence in which to implement the interventions. Here are my five steps to wellness in dentistry to help you work with less pain, improve your quality of life and extend your career.
Continue to the next page to check out the five steps.

Fig. 1
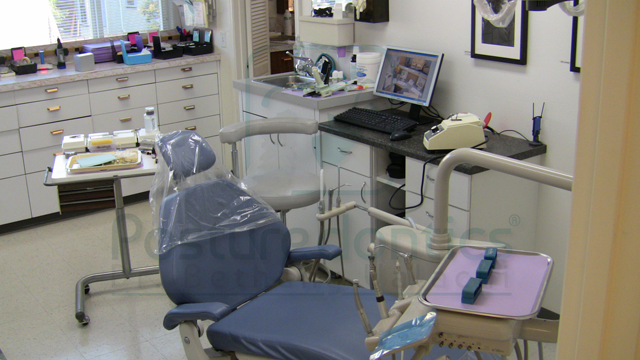
1. ‘Ergonomize’ your operatory
It is all too common to observe dental professionals spending money on chiropractic adjustments, personal trainers or expensive gadgets, only to return to the operatory environment that likely caused the pain problem in the first place. It is no surprise that the pain syndrome usually returns, and round and round it goes …
Related reading: Delivery systems-is yours delivering pain?
So, first and foremost, you need to resolve ergonomic problems in your operatory. Some important questions to ask include:
• How can I easily and economically “ergonomize” my operatory layout? (Fig. 1)
• How should I adjust the levers on my operator stool to optimize my spinal health?
• Is my loupe declination angle improving or hurting the health of my neck?
• Is the occlusal plane properly oriented for treating the upper arch?
• What style of stool is best for preventing back pain?
• Do my gloves fit properly?
• What is the best clock position to treat my patients?
Related reading: How better dental office design can prolong your career
For example, one of the most common ergonomic mistakes I observe is through-the-lens loupes with a poor declination angle that force the dentist into an unsafe forward head posture, which causes neck pain. I have found that there is only one style of loupe on the market that consistently keeps all operators in a safe head posture - the vertically adjustable flip-up-style loupe. However, before you invest in ergonomic equipment, it is helpful to know which stools, loupes, instruments, gloves and chairs will benefit your health and not make it worse. In my Equipment Recommendations Portal, you’ll find my “go-to” list of ergonomic equipment I use in consultations (http://bit.ly/ErgoEquipment).



2. Pick the right healthcare professional
If you have had persistent chronic pain for longer than six to eight weeks, you should probably consult a healthcare professional. So, who is the “right” healthcare professional? The first person most of us turn to when we are in pain is our primary care medical physicians. While physicians receive a tremendous amount of training in medical school, their schooling in therapeutic rehabilitation is quite limited.
Trending article: 5 ways to counteract neck pain in the dental practice
However, many PCPs are making treatment decisions that can profoundly (and often negatively) impact your musculoskeletal health and career longevity. Consider requesting a referral to a specialist that specifically addresses the key etiologies of work-related pain in dentistry. For example, keep in mind that because one of the primary causes of pain in dentistry is muscle imbalance and tension, a chiropractic adjustment alone rarely permanently resolve neck pain. Look to the research, which shows that dry needling is the most effective therapy for neck pain!


Fig. 2
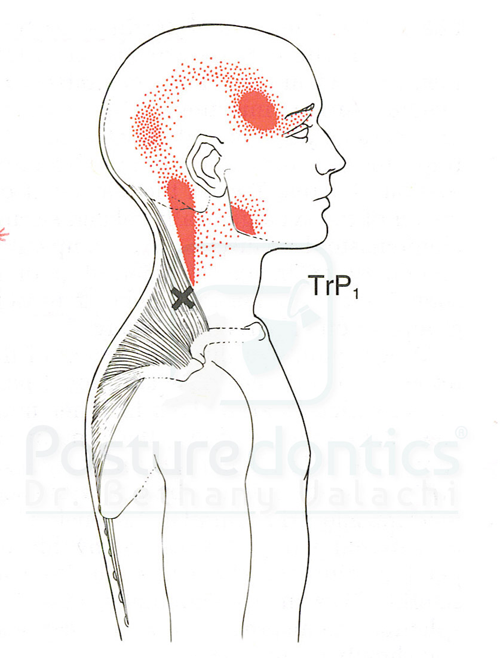
3. Resolve your trigger points
Major trigger points should be resolved before any strengthening exercise is attempted. Painful trigger points are common among dental operators due to poor postures, improper body mechanics, repetitive movement, sustained muscle contraction and mental stress. Unfortunately, trigger points are often overlooked in traditional Western medicine and patients are sent from specialist to specialist with no resolution to their pain.
Trending article: Backrests and your health: What does the research say?
Among dentists, trigger points occur in numerous muscles (Fig. 2). In the operatory, trigger points can develop from improper positioning, poorly adjusted scopes and a myriad of other ergonomic pitfalls, and require special operatory modifications. If allowed to persist untreated, trigger points can cause a myriad of musculoskeletal pain and dysfunctions.
Trending article: The top exercises that can worsen dental professionals' health
It is important to relieve trigger points as soon as possible to restore nutrient flow to the muscle, prevent muscle imbalances and prevent compression on nerves. There are various methods to treat trigger points; however, due to costs, time constraints or convenience, self-treatment is often the most practical and economical consideration.


Fig. 3

4. Develop good flexibility
Chairside stretching will help you regain full range of motion and prepare you for strengthening (Fig. 3). Overstretching muscles with active trigger points may cause micro-tearing of muscle, which is why stretching is recommended after trigger point treatment.
Trending article: Are dental loupes worsening or improving your neck health?
Since dental professionals are prone to muscle imbalances, it is important to ensure you are targeting the correct muscles with your stretching. Rather than stretching muscles that are already elongated, focus on the muscles that tend to become short, tight and ischemic.
Trending article: Demystifying pain among women in dentistry
Chairside stretching is an important strategy to perform throughout the workday to prevent microtrauma and muscle imbalances, especially for men, who are more prone to musculoskeletal injury due to poorer flexibility than women. Stretching is especially important after prolonged static postures, and even more so if awkward positions were assumed.


5. Strengthen specific stabilizing muscles
Fig. 4

Studies show that dentists with better endurance of the back and shoulder girdle muscles have less musculoskeletal pain (Fig. 4).
However, if you over-strengthen muscles with trigger points, your pain may worsen, which if why this is the fifth step in our sequence. Consider waiting until the area is pain-free to begin strengthening.
Related reading: Why all exercise is not necessarily good exercise for dental professionals
Because of their vulnerability to muscle imbalances, all strengthening exercise is not necessarily good exercise for dental professionals. Some of the worst pain problems I have seen resulted from a dentist who followed a generic exercise program designed by a personal trainer at their gym. The exercise needs of dentists are very specific, and while certain key muscle groups should be targeted, others should be very cautiously approached or eliminated altogether in an exercise regimen.
Numerous studies support endurance exercise over strength training for dentists. In dentistry, it is imperative to have proximal stability - when these postural “stabilizer” muscles become fatigued, not only can the operator slump into less than optimal posture, but the “mover” muscles are called upon to perform a stabilizing task for which they are not designed, (e.g., muscle substitution). Muscle imbalances can develop that cause painful trigger points and muscle spasms to develop in the inappropriately used muscle. Also, joints may not move normally due to the abnormal muscular tension, causing premature degeneration of joint surfaces and inflammation of the muscles or tendons. Over time, weak postural stabilizing muscles in dental professionals may ultimately lead to a musculoskeletal disorder.
Related reading: Two exercises that can help keep dental professionals pain-free
Ensuring a pain-free career involves addressing numerous risk factors. Take the time to further educate yourself on each step of the above sequences with evidence-based resources developed specifically for dentistry. You’ll find yourself feeling less pain, more energy, less fatigued, and increasing your productivity!
To help dentists effectively implement the five steps to wellness in this article, Dr. Valachi developed the Wellness System for Dental Professionals. This evidence-based kit addresses all the risk factors that contribute to work-related pain in dentistry to ensure a long and healthy career in a stepwise, easy-to-implement format. DPR readers receive a special discount using the code WELLNESSDISC. For more information, go to http://bit.ly/PosturedonticsWellness.
