5 common mistakes that can ruin your infection control efforts
Paying attention to detail is key when it comes to avoiding mishaps.
When it comes to infection control, every dental practice operates with only the best of intentions. Nobody wants a patient or a dental team member acquiring an infection or getting injured, but despite good intentions, mistakes can occur. And as a result of those missteps, the risks for infection increase.
Trending article: 5 reasons to revisit lasers for your dental practice
Are you guilty of making some of these common infection control blunders?
Click through the slides to find out!


Develop an office-specific infection control program
The Centers for Disease Control and Prevention (CDC) recommends that each dental facility develops and maintains an infection prevention and occupational health program. Pre-planning and training are vital to the practice’s infection control program.
Related reading: 5 equipment considerations to improve infection control
“The number one problem practices have is an inadequate written plan,” Dr. Marie Fluent, DDS, an educational consultant for The Organization for Safety, Asepsis and Prevention (OSAP), says. “On occasion, when I go into a dental office, I find there is no written program. In these instances, one team member might train another on how to reprocess instruments, clean and disinfect environmental surfaces, or maintain dental unit waterlines according to the protocol that he or she had once learned, but the office-specific protocol is not written. Dental facilities may have an infection control manual that’s very thick and full of wonderful policies, protocol, resources, references and templates for documentation, but if it sits unwrapped on the shelf, it is of no use. Each dental facility should have a site-specific written manual that may be utilized on a day-to-day basis.”
Passing infection control policies and protocol to team members, informally, can and will lead to misunderstandings and errors. Dr. Fluent compares the effect to that of a children’s game.
“I call it, ‘The Game of Telephone,’” Dr. Fluent says. “As a child, we would sit in a circle and share a secret with one person who would share it with the next, who would share it with the next-around the circle. When the last person explained what they had heard, the story would be completely different than what the first person intended to pass along. If we look at instrument processing in the same manner, we can assume that instrument cleaning, wrapping, sterilization and storage would not be implemented as the trainer expected. This is one fashion in which instrument processing faux pas can occur. In these instances, perhaps the wrong product is utilized, inadequate or no PPE is worn, or the manufacturer’s instructions are not followed. There are many options for error and non-compliance- possibly without the team member’s awareness.”


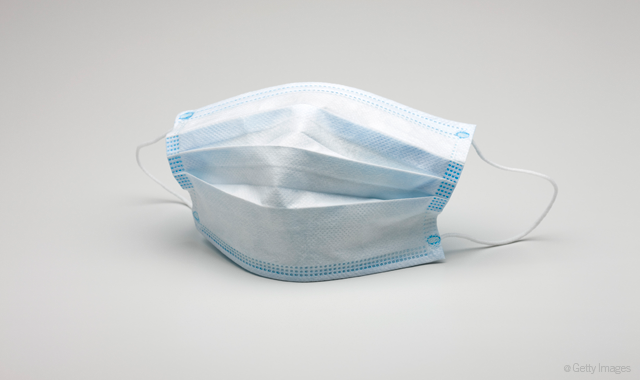
Improper personal protective equipment use
Personal protective equipment (PPE) is certainly necessary and something any practice would have on hand, but it’s not enough simply to have it-it must be worn correctly.
“During any patient treatment where there can be spray or spatter, they should leave that personal protective equipment at the site and not take it home to launder,” Mary Borg-Bartlett, president of SafeLink Consulting, says. “It should be changed between patients whenever there is spray or spatter. If a patient is there just having a hygiene appointment, that hygienist would need to wear PPE over their clothing and remove it after treatment of that patient and put on fresh PPE for the next patient. If the dentist is coming in just to do a quick look and exam of that patient after the hygiene appointment, they wouldn’t have to change it between patients, unless they were with another patient and had spray or spatter on their PPE. The key to it is spray or spatter and not to move the spray or spatter out of the operatory.”
PPE problems can involve things as unassuming as a face mask.
Trending article: The dangers of STDs in the dental practice
“I have seen clinical personnel in non-clinical areas (reception area, lunch room) wearing their mask pulled below their chin,” Dr. Fluent says. “When I see this, I don’t know if the mask is contaminated or not, nor if they’ve changed it in-between patients nor if they intend to perform a clinical function wearing the mask in this fashion. Masks are intended to cover the nose and mouth and form a complete seal. Masks are single-use and they should be removed and disposed of immediately after the dental procedure.”
While the process of wearing appropriate and non-contaminated PPE may seem cumbersome and difficult, it is necessary to avoid cross contamination.
“It is a challenge for the dentist,” Borg-Bartlett says. “But we do have dentists who use disposables and have become proficient in handling it when treating more than one patient at a time. They simply remove the PPE and leave it in that operatory before moving to the next operatory. In other words, they should not be moving between operatories with the same personal protective equipment when there is spray or spatter on the PPE. This is one of the major issues that we see involving cross contamination, plus one that I have seen OSHA issue citations for in dental practices.”


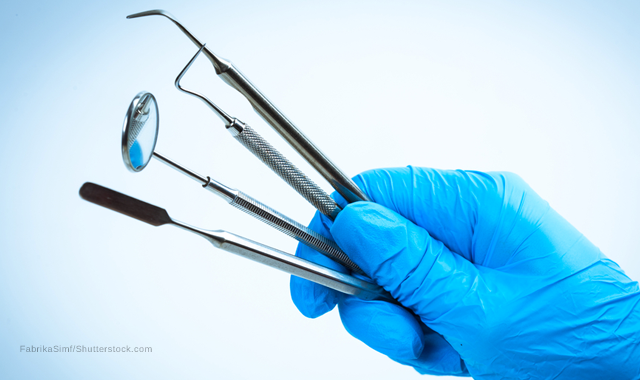
Segregate dirty instruments
Instruments should be segregated by patient or operatory during reprocessing. But it’s not just for the sake of proper cleaning, it’s in case the worst happens: a percutaneous stick.
“The reason they need to be able to identify instruments used on a specific patient is to be able to identify the patient in the event of a stick or cut by a dirty instrument,” Borg-Bartlett explains. “In other words, if they have three operatories going, then take all the dirty instruments on a tray from each one and place them into the sink to process for sterilization, and they get stuck by one of those instruments, OSHA’s ‘post-exposure evaluation and follow-up’ procedure outlined in the Bloodborne Pathogens standard must begin. The dentist then has to ask all three patients if they would consent to blood testing and offer the blood testing to the worker who got stuck.”
More from the author: 5 things you should be doing NOW to improve infection control
While the fact remains that if a team member has an occupational injury, instrument isolation makes it easier to determine whether the employee was exposed to a bloodborne pathogen.
“The point is to segregate by patient during the cleaning process so that if they get stuck while cleaning the instruments, they would know which patient, and the doctor would only have to ask that one patient,” Borg-Bartlett explains.
“I’ve had this happen where there were multiple patients’ instruments,” she continues. “The worker got stuck and they had to contact all of the patients. So if one of those patients tests positive for HIV or hepatitis, the employee is notified, but that may not even be the instrument from that patient’s mouth. So now this employee is going to be concerned until further testing is performed and it’s ruled out that none of the patients had a disease that could have been contracted. Not a pleasant situation for that employee.”



Improper sharps disposal
How sharps are handled is another easy way to avoid trouble. Borg-Bartlett recommends disposing of them at the point of use.
“It’s better to have a sharps container and have it easily accessible, not under a counter where they’re having to maneuver around to dispose of a needle,” Borg-Bartlett says. “Many practices will have a central, larger sharps container in Sterilization, so now you have the needles being transported to one area. So during transport there’s more potential for an accident.”
Like a cut or a stick during instrument reprocessing, getting stuck while handling a needle has its own protocols to follow once an incident occurs.
Read more: 6 overlooked areas in your office that can improve infection control
“It is an OSHA requirement that every office has a copy of the Bloodborne Pathogens standard on file,” Dr. Fluent says. “And part of this standard is an exposure control plan. What happens if an injury should occur? Where do you go? What do you do? What forms need to be filled out?”
Since the transporting of sharps and needles poses a greater risk of injury, why would a dental facility utilize a centralized sharps container?
“It could be economics,” Borg-Bartlett observes. “They can get more in a larger container, as opposed to the smaller ones in the operatories, so disposal costs may be less.”
Easily accessible sharps containers are not a mandate, just a good idea.
“It’s not a requirement, but the Centers for Disease Control recommends it,” Borg-Bartlett says. “We’ve just seen having sharps containers at point of use work better to prevent needlesticks.”



Improper sterilization protocol
Following correct policies and protocols during instrument reprocessing and sterilization is a common place for errors. Blunders can occur in seemingly innocuous locations.
“During the packaging of dirty instruments for sterilization, they don’t always fold them right on the perforation,” Borg-Bartlett observes. “They may have a packet that is 6 inches tall, but the instrument is only 3 inches tall. They will fold it all the way down to make a 3-inch packet. Well, those packets are designed to be folded on the perforation. What happens is, when you fold it below the perforation, it creates a pocket on either side and is not completely sealed. Therefore, after sterilization, and they’re placed on a counter or in a drawer, they shouldn’t be considered properly sealed and sterile.”
Trending article: The latest hourly and annual salary numbers for dentists and dental assistants
Another mistake is overloading the packets with instruments.
“If you have a very busy office, a number of people performing packaging and only one sterilizer, it opens the risk for overloading the packets and compromised sterilization,” Borg-Bartlett says. “The packaging needs to permit free circulation of the sterilizing agent. So don’t overload packets and don’t overload the sterilizer. You don’t want multiple layers of instruments in the packets because you want proper circulation.”
Once instruments come out of the sterilizer, the packets must still be handled correctly.
“Don’t take them out wet. They need to dry,” Borg-Bartlett advises. “If they are removed from the sterilizer wet, something called ‘wicking’ can occur. If you set them on a dirty counter, for instance, that wet packet can absorb whatever’s on that counter or on someone’s hands, so now they’re not sterile.
“Also, we see practices unwrapping sterilized instruments and tools,” she continues. “Mainly, it happens with handpieces and putting them in a drawer until they’re needed. They should not be unwrapped until you’re ready to use them.”
Infection control is something everyone should take seriously, but even when one thinks he or she is following the rules, mistakes can still be made. Fortunately, those mistakes can be easily avoided by paying attention to detail.

