Two common reasons your wrist hurts — and how to treat it
Many dentists complain of pain in the hands and wrist, but aren't sure what's causing it or how they can take care of it.
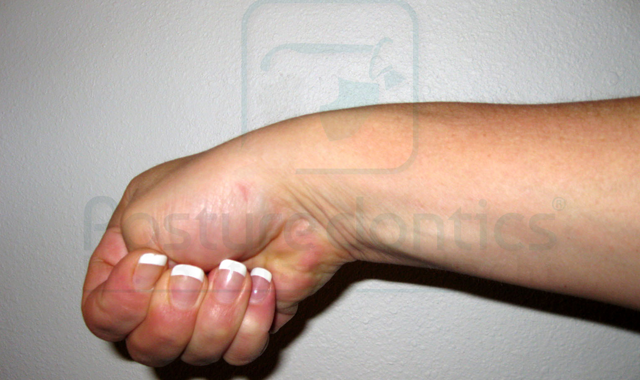
In dentistry, two of the most commonly reported pain syndromes of the wrist occur in nearly the same area.
Easily confused, but of entirely different origin, de Quervain’s disease is a painful inflammation of the tendons in the thumb, whereas osteoarthritis (OA) of the thumb is a degenerative joint process. Both appear frequently among dental professionals, since a primary risk factor is repetitive thumb use.
These syndromes can be debilitating, and OA of the thumb can force early retirement, especially among female dentists and hygienists. Therefore, it is a good investment in your health to implement early ergonomic prevention strategies.
Fig 1
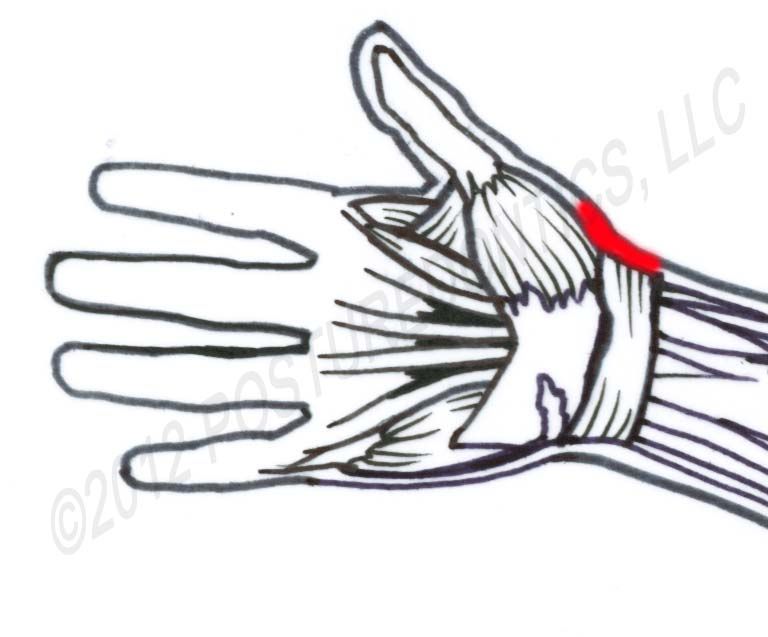
de Quervain’s disease (also known as de Quervain’s Tenosynovitis) affects two thumb tendons that move the thumb forward and away from the hand at the CMC joint, between the base of the thumb and the wrist. Symptoms include pain, tenderness and swelling on the thumb side of the wrist (Fig. 1). Oftentimes gripping is difficult, and movement of the thumb worsens the pain. While the name implies a tendonitis, the newest research reveals that it is more likely a thickening and degeneration of the tendon synovial membrane.
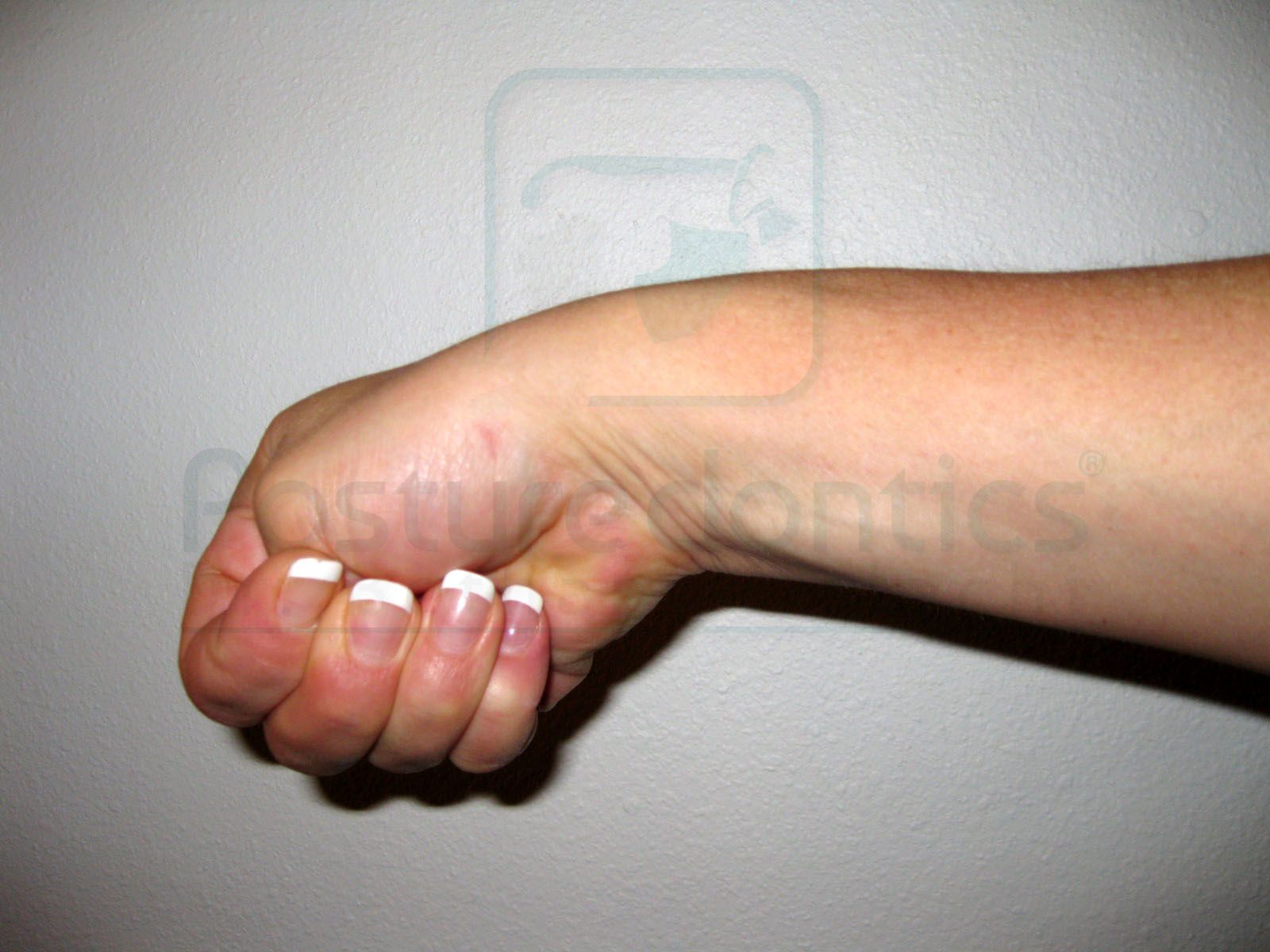
In dentistry, this is most often due to forceful, sustained or repetitive thumb abduction (flexed forward, out of the plane of the hand) combined with angling the hand sharply to one side. Scaling, extractions or suctioning with a palmar grip are a few examples of tasks in dentistry that can lead to the problem. Women are four times more prone to develop this problem than men, and frequency is highest in team members 35-55 years of age. The test for de Quervain’s is quite simple: with the thumb held in a fist, angle your wrist toward the little finger, or “pinky” side (Fig. 2). It is normal to experience discomfort; however, if it produces pain, you may have de Quervain’s disease.
Related article: 5 ergonomics tips that could save your career
Interventions include ergonomic modification, cortisone injections, splinting, ice, anti-inflammatory meds, frequent breaks, gentle stretching and surgery. Regardless of the intervention, ergonomics in the operatory should always be addressed to prevent recurrence or worsening of symptoms. Most importantly, avoid a forceful pinch combined with angling the wrist sharply to one side.
Fig. 2
Hygienists should consider the following motion when scaling: grip the instrument in a straight, or neutral, wrist posture, use a finger fulcrum and lock the wrist as you roll the forearm from side to side. To decrease pinch force, consider larger diameter handles (10 mm+), using ultrasound and ensuring sharpness of hand instruments.
A certified hand therapist (CHT) may be a good referral to request from your doctor for conservative therapy before considering surgery. You should also know that the muscles of the same tendons that cause de Quervain’s disease may develop trigger points that can also refer wrist pain and mimic this syndrome. A good resource for troubleshooting and differentiation is “The Trigger Point Therapy Workbook” by Clair Davies.
If considering surgery, the success rate is quite higher than carpal tunnel surgery and provides relief in many cases.
Osteoarthritis of the CMC joint of the thumb
Osteoarthritis (OA) is the most common joint disease and a major cause of disability in the U.S. Similar to muscles and spinal discs, your joints also require movement to receive nourishment and remain healthy. Whereas medium to high levels of activity do not cause OA, studies show that abnormal static loading and immobilization leads to the syndrome.
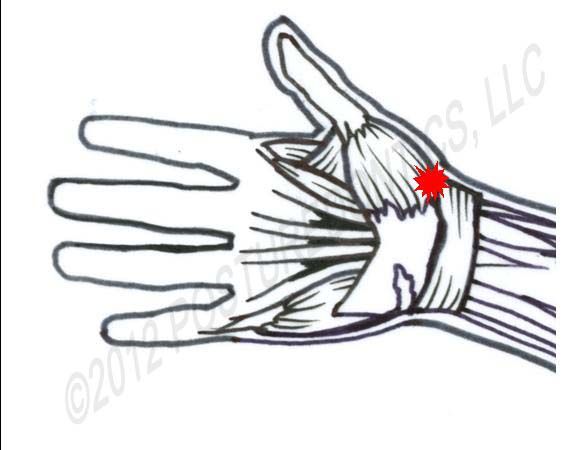
Fig. 3
Joint forces are greatest in the hands during precision handgrip. It is easy to see why dental hygienists are most prone to disability due to this syndrome.
Symptoms include pain and aching at the base of the thumb (Fig. 3), which worsens with pinch grip. The area is tender when pressed upon and can be stiff in the morning. These symptoms are worsened with pinching and twisting. At the thumb CMC joint, the primary stabilizing ligament (the beak ligament) becomes tight when you pronate your forearm (palms-down) and assume a lateral pinch grip. When this ligament becomes weakened, the CMC joint moves improperly and joint damage can occur. The syndrome is most prevalent in women over 40 years old. Excessive thumb pain can limit hand function up to nearly 50 percent.
The symptoms are very similar to de Quervain’s disease, but intervention is quite different. Therefore, it is imperative that specific diagnostic tests be performed. In addition to the Finkelstein’s test above, the “grind test” should be performed by a trained professional (CHT or orthopedic surgeon) to test for cartilage damage at the CMC joint. If positive, a primary ergonomic intervention is to maintain a flexed CMC joint during activity and avoid a collapsed or flattened joint.
To see what a flexed CMC joint looks like, make an “O” with your thumb and second finger. Notice the bend at the base of your thumb? Try to maintain this angle while working in the operatory. Also, frequently moving the thumb into extension and abduction is an important prevention strategy (Figs. 4a and 4b). Other interventions are large diameter instruments and ultrasonic usage.
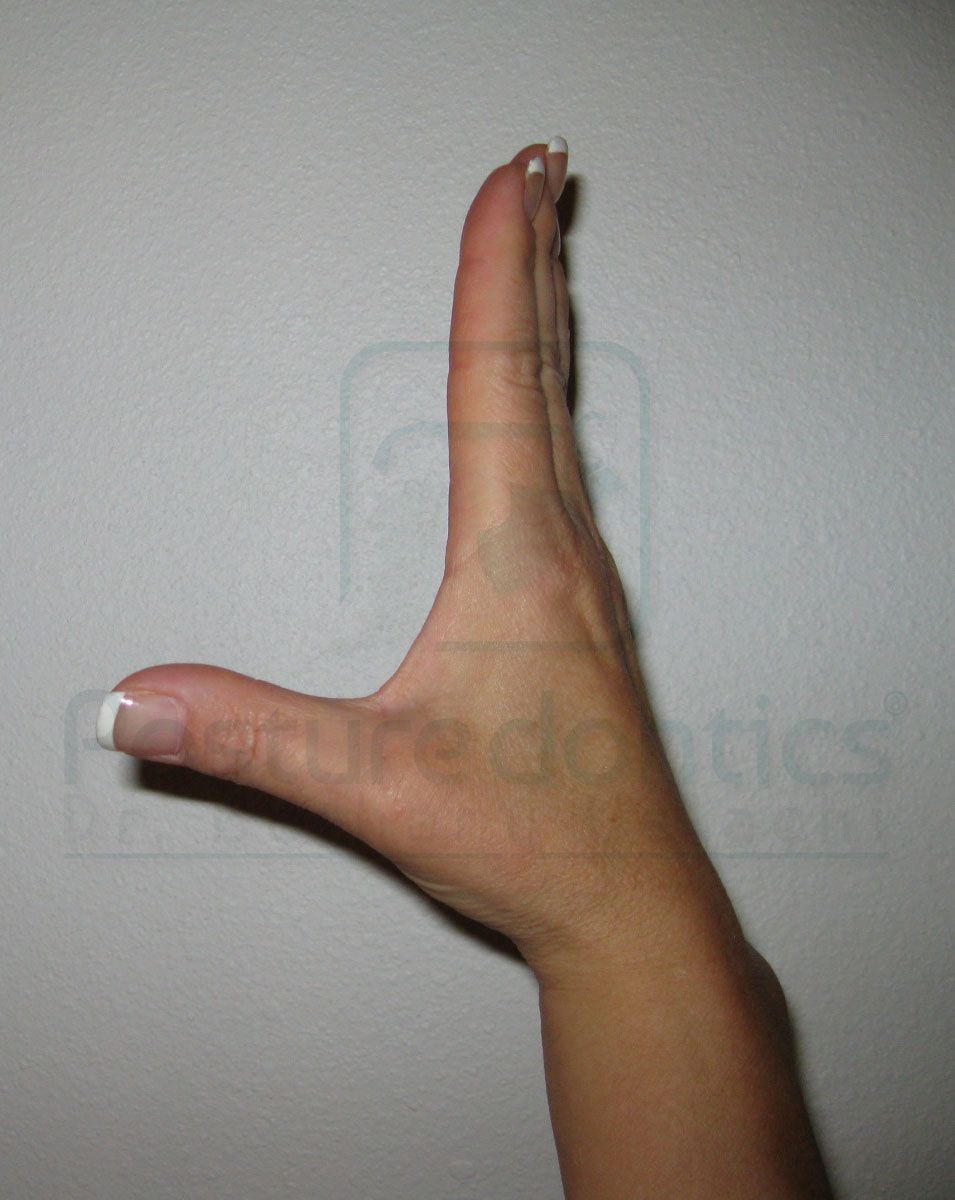
Fig. 4b
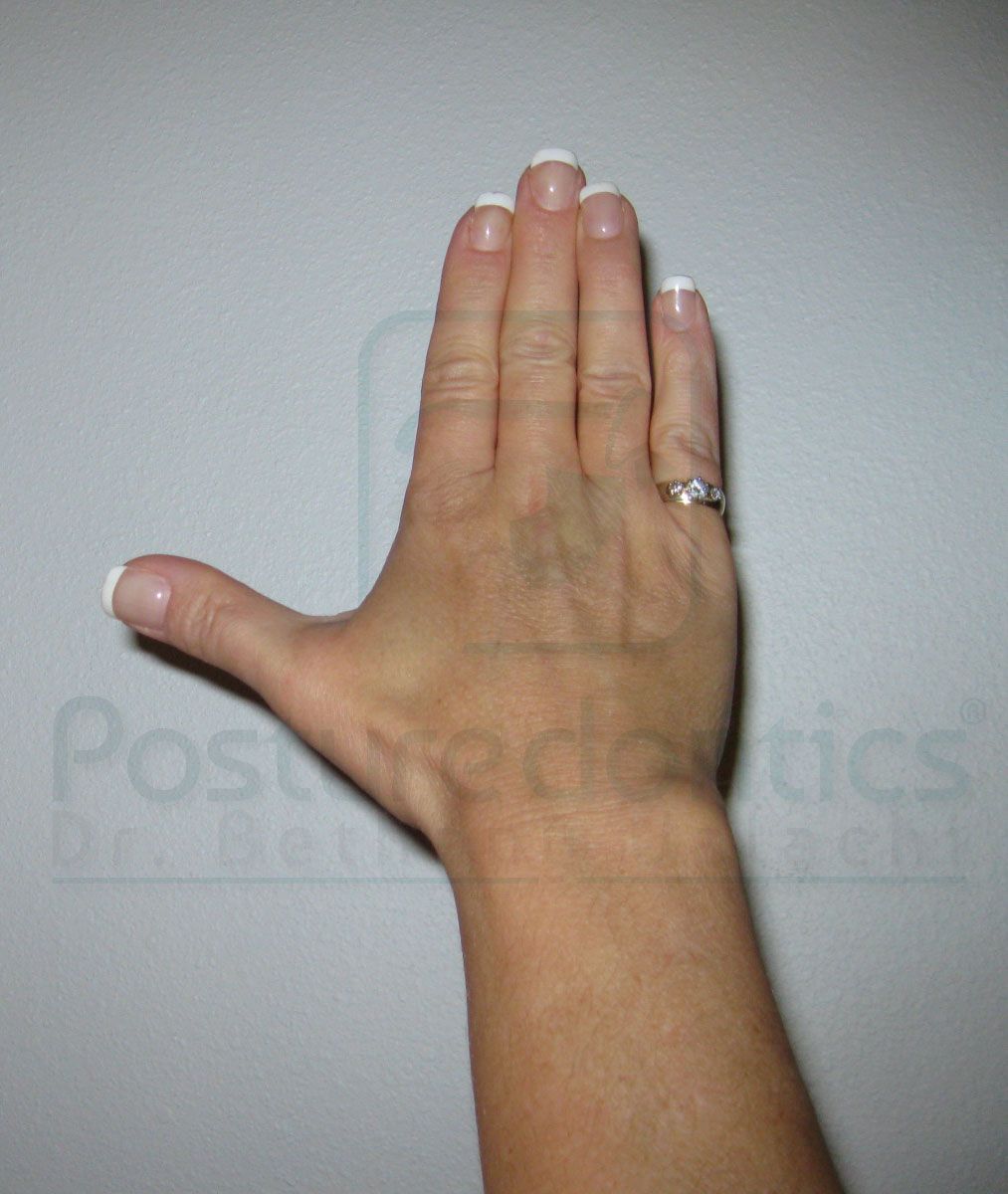
Fig. 4a Fig. 4b
Medical interventions usually involve splinting, hot or cold therapy (cold is usually more effective when pain is due to repetitive use), and, after pain is resolved, specific strengthening exercises. If conservative management fails, surgery may be indicated.
Ensuring a long and healthy career in dentistry requires a multifaceted approach, including optimizing ergonomics in your hygiene operatory, differentiating between loupes that will improve your neck health and those that will make it worse, identifying the unique muscle imbalances to which dentists are predisposed, and implementing the correct exercises, knowing which exercises can worsen your health, requesting a referral (from your primary care doctor) to the correct healthcare practitioner, effectively treating your own trigger points and more.
This and much more is in Dr. Valachi’s “Well Body System for Dental Professionals,” available at www.posturedontics.com. DPR readers can receive a discount by entering the code “DPRDisc.”