Should you be concerned about measles?
Find out what steps to take if a measles outbreak has occurred in your community.
It seems almost unfathomable that a disease such as measles is still a concern. The measles vaccine was first licensed in 1963 and was declared eradicated in 2000. However, cases still occur-and are even on the rise. For instance, in 2010, the Centers for Disease Control and Prevention (CDC) reported 63 cases. In 2014, that number spiked to 667 cases. But 2019 has already left that number the dust. By May 24, there were 940 cases of measles reported.
The fall and rise of measles
By the 1960s, measles was a serious health concern infecting thousands and killing hundreds each year.
“In the decade before the live measles vaccine was licensed in 1963, an average of 549,000 measles cases and 495 measles deaths were reported annually in the United States,” reads the CDC’s website.
After the vaccine, infections steadily declined, virtually wiping out all instances within four decades. But since the turn of the century, the disease has achieved a foothold and continues to rise.
Related reading: Infection control tips for nonclinical areas of the practice
Since 2000, when measles was declared eliminated from the U.S., the annual number of cases has ranged from a low of 37 in 2004 to a high of 667 in 2014,” the CDC website states. “The 2019 case count exceeded 2014 levels as of April 26, 2019, and continues to climb.”

The cause seems to be a lack of immunizations coupled with infections being brought in from other countries.
“The majority of cases have been among people who are not vaccinated against measles,” the CDC says. “Measles cases in the United States occur as a result of importations by people who were infected while in other countries and from transmission that may occur from those importations. Measles is more likely to spread and cause outbreaks in U.S. communities where groups of people are unvaccinated.”
Like any infectious disease, healthcare workers are especially at risk, given their proximity to patients, especially those who may carry a disease.
“Measles spread through very small particles or droplet nuclei that remain suspended in the air for long periods of time,” says Karen Daw, “The OSHA Lady,” a speaker and consultant. “It’s a concern when a susceptible person inhales the virus. Only a small number of diseases are transmitted this way, including tuberculosis and measles. In fact, measles virus can remain active for up to three hours after the infected person has left the area.”
A need for concern?
For all the warning signs about measles’ resurgence, the numbers are clearly what they were in the 1960s. Do healthcare workers really need to be all that concerned? The answer is yes.
“Everyone in the United States should be concerned about outbreaks of measles, which is something that’s a completely preventable infectious disease through immunization,” says Kathy Eklund, RDH, director of occupational health and safety at The Forsyth Institute. “Dental healthcare workers can actually play a role by following CDC-recommended immunizations and screenings for healthcare personnel. That is one of the first lines of protection. Secondly, have patient information in your dental practice setting about recommended immunizations, including measles, for adults and children.”
More from the author: The virtues of beautiful design
“Measles is highly contagious,” Daw adds. “I asked an audience last month their concerns around Ebola and the flu. Almost everyone who had gone to their primary care doctor recently recalls being asked some interesting questions related to possible Ebola exposure, like whether they’ve traveled outside the country in the past few months and if they’ve had any of the symptoms on the list. They also recall at least one person who contracted the flu. In epidemiology, the basic reproduction number, denoted R0 or ‘r nought’ is the number of secondary cases that can occur in a susceptible population. For flu and Ebola, it is two. For measles, it’s a whopping 12 to 18.”
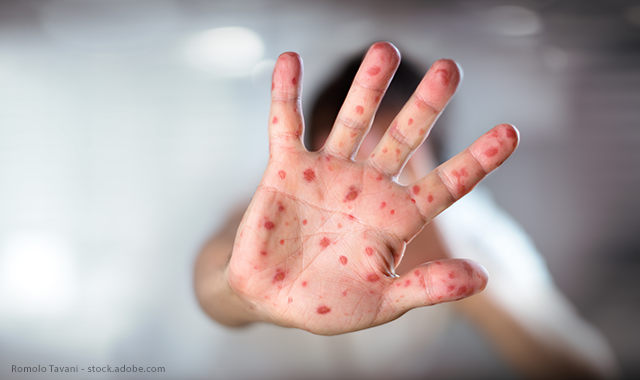
The most common symptom associated with measles is a distinctive rash, but measles can be so much more dangerous, if not deadly.
“Complications related to contracting measles include ear infections, which can result in hearing loss, pneumonia, which is a common cause of death among children with measles, brain damage and even death,” Daw says. “But most are familiar with the characteristic rash associated with measles. What few people realize is that the rash actually starts from the head and in the mouth before spreading to the rest of the body. Therefore, dental professionals are sometimes the first to diagnose measles in an individual. But by that point, they’ve most likely been exposed.”
Failing to immunize one’s self or children is easy to blame on a trend toward anti-vaccination. And while that may be the case for some, the fact remains others simply may not be able to get the vaccination.
“Clearly, if parents are making decisions about themselves or their children to not have them immunized, that’s a real challenge,” Eklund says. “They may have misinformation or a lack of understanding of current evidence-based information and CDC guidance. There are children and adults who can’t be immunized for health reasons, such as a compromised immune system. These individuals are at risk of becoming infected if exposed to measles, mumps, or chickenpox. That is why it is so important for everyone who can be immunized to be immunized, to protect those who cannot be immunized. This is referred to as ‘herd immunity,’ also called ‘community immunity.’”
Continue reading on page two...
Measles mitigation
The most obvious way for dental healthcare personnel (DHCP) to avoid measles and prevent its transmission is by ensuring that they’re immunized.
“Both OSHA and CDC mention the MMR vaccine, or ‘measles, mumps, rubeola’ vaccine,” Daw says. “Dental professionals should ensure they’ve received the proper immunizations or have documentation of previous exposure. This is to protect themselves, their colleagues, family and patients.”
DHCP, like other healthcare personnel, are in particularly susceptible positions, so it’s especially important that they’re mindful of infection prevention.
Trending article: Tackling the taboo topic of mental health in dentistry
“That’s why there are recommended immunizations and screenings for healthcare personnel,” Eklund says. “Dental healthcare personnel should know their antibody status to the vaccine-preventable diseases. I think this is important, not only from the standpoint of personal protection, but also to prevent healthcare-associated infection. Infectious diseases such as chickenpox and measles are highly contagious and someone can be contagious before they have overt clinical symptoms. The best preventative measure is immunization. “A non-immunized dental healthcare worker is at risk of being exposed and in turn exposing other nonimmunized staff and patients,” she continues. “The primary goal of an infection prevention and control program is to prevent healthcare-associated illnesses in patients and injuries and illnesses in personnel.”
Infection prevention is so important that governing bodies have rules in place to mitigate the spread of disease.
“OSHA also has standards and directives regarding protecting employees from the transmission of infectious agents,” Daw says. “The most well-known are the Bloodborne Pathogens, Personal Protective and Respiratory Protection Standards. The latter provides information on protecting the team from exposure to airborne transmissible diseases, which includes measles. An additional document to consider is the CDC’s ‘2007 Guideline for Isolation Precautions: Preventing Transmission of Infectious Agents in Healthcare Settings.’”
The worst-case scenario
What if the practice operates in a community where a measles outbreak has occurred? Should anything extra be done?
“The first line of defense is having people understand that if they’re at risk for measles, if they have children at risk for measles, it is very important to closely monitor their signs and symptoms and to get them immunized as soon as possible,” Eklund says. “Dental practices in a community where measles have been identified can have messaging when they’re doing appointment reminders, for instance, reminding individuals if they have any signs or symptoms of measles, such as fever, rash, etc., to contact their primary healthcare provider immediately.”
In the event a measles exposure has occurred within the practice, contact the local health department for guidance.
More from the author: Dental care in paradise
“Practices should have an immunization record for all personnel and follow the CDC-recommended immunizations and screenings for healthcare personnel,” Eklund says. “In the event of an exposure, review the personnel immunization records to determine if there are staff who have not been adequately immunized or who have a history of measles infection. Anyone who doesn’t know their antibody status, hasn’t had the vaccine, or doesn’t know if they have had measles should refrain from patient care; they should contact their primary healthcare provider; and they should probably go in and be screened, which is just a simple blood draw for antibodies to measles. And if they’re not protected, they should get the measles vaccine.”
How the practice responds in the event of a measles occurrence-or any contagious infectious disease, for that matter-can help prevent the disease’s spread as well as alleviate patient concerns.
“The dental practice should have written policies and operating procedures regarding what steps to take to prevent infectious agents from arriving in the practice, especially for respiratory infections.” Daw says. “It’s helpful to know that three to five days before the characteristic rash appears, the exposed individual will have cold-like symptoms. So, it would benefit the practice to remind patients that if they are experiencing common symptoms associated with a respiratory infection, they should call as far in advance as possible to reschedule. Also, ask questions like whether they have new symptoms since their last appointment.
“Signage can also help to educate patients that if they feel unwell, they should reschedule,” she adds. “Some offices offer the patient a mask to don if they arrive with cold or flu symptoms, but the goal is to prevent the patient from coming in to begin with if they are contagious.”
Like some unwelcome fad, measles seems to be making a comeback, but DHCP can do its part to make sure that it doesn’t come back any faster-or any stronger-than it has to.