How technology is changing the game for implants
Breaking down how technology and digital tools are changing what dental laboratories and practices are able to provide for patients.
There’s no doubt: Implant dentistry is booming. Thanks to advancements in technologies, materials and procedures, the restorations are more popular than ever. According to the American Association of Implant Dentistry (AAID), three million people have dental implants, and that number grows by 500,000 every year. Further, the AAID estimates the dental implant and prosthetic market in the U.S will reach $6.4 billion by 2018.
Labs are able to deliver more for their doctors. Doctors are able to perform the surgeries quickly, more easily and less expensively than ever. And, as a result, more patients want the restorations, leading to more work for the entire dental workflow.
Advances are happening on many fronts: from the doctor to the manufacturers, but nowhere more so than what the lab is able to deliver.
How CAD/CAM shapes the implant workflow
Any discussion of improved workflows would be incomplete without recognizing the role of CAD/CAM. Like so many other restorations, implant creation has benefitted from a digital workflow.
“I’ve been around the implant business and digital for a long, long time,” says Dr. Robert Gottlander, VP, Global Prosthetic Solutions at Henry Schein. “The whole thing started out with machined titanium abutments, then you got to cast gold abutments, and what CAD/CAM really has done is that it has made it possible to use ceramic materials. When we talk about digital and CAD/CAM, we are usually focused on the technology and the equipment. But in some ways, what is really driving the technology is that you can use ceramic materials. You can use zirconia, you can use lithium disilicate, and you can actually design these materials in a way so they can be used for abutments, for crowns and for bridges. And that means that you will get a much better esthetic outcome.”
Dr. Gottlander compares crafting implants to building cars.
“If you have a really good person that’s doing it handcrafted, you get a phenomenal product,” Dr. Gottlander says. “It’s like [an] automobile. It’s not bad if the person who’s [building] it knows what they’re doing. But if you want to have a really good, predictable quality for a larger number of people, then it’s good if you have robots doing it. It’s a little bit the same with abutment production. I would never say that digital is better than handcrafted, but since we all know that handcraft[ed restorations have] more fluctuations in quality than something you design in 3D and produce on a milling machine, I think the design of the abutments in the production of the implants is very good and that will also lead to better esthetics.”
Ultimately, CAD/CAM is a tool-a revolutionary tool, but a tool nonetheless-and lab technicians and dentists can use it to produce quality restorations.
“CAD/CAM just improves all the little details,” says Marina Caponigro, MDT, EFDA and in-house lab technician for Dr. Neal Patel, DDS at Infinite Smiles in Powell, Ohio. “They’re little details but they’re very important. It cannot be done sloppily. It should be scientifically driven and you should think about the end result. You don’t have to spend time on routine steps that are a waste of time. CAD/CAM makes it very easy on the doctor and the technician.”
How software helps
Innovation has occurred in every part of implantology, especially where CAD/CAM is involved. The software used to design implants has not only made the restorations better, but has also made the work easier.
“It’s more intuitive,” observes Dr. Gary Severance, DDS, Planmeca University. “In the early generations, the software may have given you a good proposal or it gave you something the computer thought was a tooth in the right location, but the more information that we, as dental professionals, can provide the system, whether scanning more, detailing some areas, marking the margins of the tissue, then the computer has information and can present an ‘educated’ proposal. We see the computer becoming more intuitive and learning from past patterns-learning the clinician/technician’s preferences. There’s going to be artificial intelligence in the design process [to] give you a better proposal, saving time, and that’s a big thing when you’re in the mouth or you have a patient waiting. If that computer can have an educated/learned proposal for what you really want, then the whole design process of the CAD becomes much easier for everybody and less time-consuming.”
Implants have come a long way, and innovation continues to revolutionize what can be done.
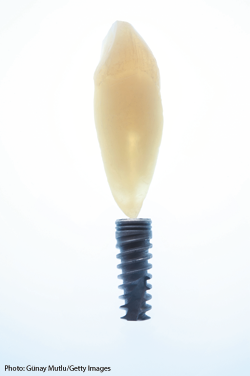
As a result of the technology’s precision and intelligence, implants are improved and prices lowered.
“Certainly the accuracy has improved dramatically, and it’s getting even better every day,” says Mark Ferguson, General Manager, Vulcan Custom Dental in Birmingham, Alabama. “Here at Vulcan, when we’re printing models, we’re no longer using a metal lab analog. We’re actually printing the implant interface and screw threading in the printed model, which is keeping prices down as well. It’s more accurate, because there are fewer things to rotate. Fewer parts always makes things more accurate.”
CAD is also able to help labs objectively quantify formerly subjective information.
“One big thing is the ability to measure things,” Ferguson says. “We’re not guessing anymore. We know precisely where a margin’s being placed. We know precisely how much tissue displacement there is. If a doctor has trained the tissue, we can digitally set the implant right on that trained tissue, so there’s some really amazing features, digitally.
“None of it is actually new, it’s just being used in a different way now,” Ferguson adds. “One of things that got me excited about digital 10 years ago was the fact that I can make my model translucent and then measure exactly how far something is from something else. It’s the ability to quantify what we’re doing, instead of saying, ‘Yeah, that’s about the tissue compression that we want,’ based off of a feel.”
While these innovations make implant creation easier, more accurate, and less expensive, in the end, patients see the benefit.
“All of this technology can speed up treatment times while also resulting in higher-quality outcomes,” Dr. Gottlander says. “You can take digital impressions with an intraoral scanner, design the position of the teeth, and then take that design file from the cone beam and to do the implant planning. There are so many things that you can do today that you could not do five or 10 years ago.”
Breakthroughs in esthetics
Patients want durable, quality implants. But when they smile-and see their investment reflected back in the mirror-they aren’t seeing durability. They want to see something that looks like a real tooth. Happily, esthetics continue to improve and evolve.
“The potential for ideal esthetics has always been there; it’s more a question of how skilled does someone have to be to achieve the ultimate results,” Dr. Severance notes. “In previous years and decades, a technician would layer many layers of ceramic and fire it and layer it again and fire it to get those layered looks. And now blocks are coming out with that layered translucency and are multi-chromatic, so it’s just made it easier for the masses to achieve and predictable. Techniques have been simplified so there’s less chance of errors, and so whenever anybody has fewer choices to make, they have a better chance of success.
“It’s like when you do MapQuest and you get 11 different turns. You have a pretty good chance of getting lost,” he compares. “But if we reduce that to one or two, and the computer or the intelligence takes care of the rest, you have less chance of an error. One of the misnomers of CAD/CAM or digital dentistry is that it makes a bad dentist/technician/assistant good. No; it just makes a good team better. Because there are still fundamentals you can’t compromise on, but it makes it easier to get up to that better dentistry level consistently by eliminating variables.”
Great esthetics are the lab’s responsibility. Not only must they make the restoration as natural looking as possible, but they also must be skilled enough so that implants can be accurately placed and properly fitted.
“Esthetics really come from the lab, but the quickest way to kill esthetics is by having the doctor grind them all away, and trying to get something to fit in the mouth,” Ferguson observes.
Manufacturers continue to improve their designs, resulting in better quality esthetics. For example, Dr. Patel looks to TiBases, from Dentsply Sirona.
“We’re getting phenomenal results because there are newer concepts in the restorative process for implants,” Dr. Patel says. “The TiBase is very low in profile and sub-gingival, so we can really customize the emergence of the restoration from the gum tissue. There is a lot of ceramic material, as opposed to titanium, which allows us to then have a more predictable esthetic result near the gum line and certainly the top of the tooth itself. The ceramics are now at the point where we can mimic existing teeth, regardless of their characteristics and color. They’ve come so far, I would say we are close to the edge of where we’re getting perfect results, esthetically where they’re not detectable by the untrained eye.”
New materials make implants better-but there’s room to grow
The components used to create implants continue to advance, providing better esthetics, greater precision and overall superior quality.
“We went from the cast frameworks, which we all know could be really good, but they were often not optimal,” Dr. Gottlander says. “Digital technology means that you can actually mill something that is absolutely precise and fits well, but what we’ve also seen is that you can do that and go from metal to ceramic.”
Though materials for digital workflows are improving, there are not as many options for digital dentistry as there are for traditional workflows.
“There are fewer materials to use than with the analog workflow,” Ferguson notes. “Traditionally, if you look at the UCLA abutments, labs had a wide variety of materials to choose from to then create porcelain-fused-to-metal, screw-retained. Right now, you’re kind of limited to either non-precious or titanium, titanium being harder to stack porcelain to, non-precious not necessarily being the ideal material for the implant-to-abutment connection. There’s still a little bit of work to do in terms of materials, but what we have is great.”
And while materials are improving, Ferguson notes that nothing is-yet-poised to take the implant world by storm.
“They’re not game-changing,” Ferguson says. “Hopefully they are stop-gaps to some really improved materials in the future. If we look at these materials, hopefully they are going to turn into kind of what zirconia has turned into, where, in the beginning, you’re given this one flavor, but through use, more shades come out and different processing methods come out, with the zirconia and painted on coloring and things like that hopefully something like that can happen with these high-strength ceramics.”
A new revenue source for labs that can improve patient outcomes
In some cases, doctors are able to drill holes into patients’ mouths-freehand-to place the implant. However, in more complex cases, surgical guides aid doctors. These plastic pieces fit over the patient’s gums and show the doctor precisely where, at what angle, and how deep to drill.
“If the case is ideal and just seems super easy, I will freehand it,” says Dr. Kaveh Ghaboussi, DDS, of Madison Smile Solutions in Madison, Wisconsin. “But if there is any kind of tricky part to it or angulation or the access is difficult, we just go ahead and have a surgical guide made.The cost of a surgical guide has come down significantly, so it just makes the workflow so much easier and cuts down on wasted time. The surgical guides can really simplify the case.”
In the past, creating surgical guides was a time-consuming process and were only made for the most difficult cases. Now, CAD/CAM and 3D printing has streamlined the process, making guide creation faster and easier than ever.
“It used to take me about three hours to go through all the steps, plus I’d have to wait for the gypsum to set up and acrylics to set up, so it was a long process,” Caponigro says. “Now, with CAD/CAM, it’s so much easier. The doctor does his work, then I get my file, open it in the software, make it look nice, and it gets sent to a milling unit where it mills out while I’m drinking coffee and eating cookies.”
Creating surgical guides takes a lot of stress off of everyone involved in the case.
“[Dentists] don’t need to sweat,” Caponigro says. “They don’t need to not sleep during the night thinking about how difficult the implant is going to be, because the implant is very predictable. The doctor has everything he needs to have with CAD/CAM technology and surgical guidance. There are no doubts. All he needs to do is pick up his drill, drill the hole, screw in the implant and he is done. It takes 10 minutes. It’s not bleeding. The patient has no pain and swelling. The lab technician’s life is easy, the doctor’s life is easy, the patient’s life is easy.”
The key to every implant case
It is incumbent on doctors and their laboratories to communicate and collaborate on their cases. Happily, digital dentistry has made that collaboration much easier and more effective.
“Successful laboratories have very often been successful because they have a close collaboration with the dentist,” Dr. Gottlander says. “In many situations, laboratories have supported the dentist with knowledge, and I think that will continue. What the technology is doing is that you can actually communicate much faster and more directly between the dentist and laboratory. Let’s say if I do a scan and I send it to my lab and the lab has designed an abutment, the lab can send that design back to me so I can check it on the screen in my office. I can approve it or ask for changes. I also think that communication between the dentist and the laboratories, when it comes to implants, is OK, but it can be taken one step further with new technology, that’s for sure.”
Digital tools, while great, are not perfect. The idiosyncrasies between the doctor’s and the lab’s systems necessitates communication.
“Hopefully there’s more back and forth now, and there certainly needs to be,” Ferguson notes. “Dentists have-if you’re going all-digital-maybe five-to-seven different scanners that they can use in the mouth. Not all labs can accept files from all those scanners. They’re all going to be slightly different, and depending on the technology in the lab, they may or may not be able to work with certain files. So a doctor can take a scan with the intraoral scanner and then all of a sudden have nowhere to send it-at least nowhere he’s been working with. And then the other side of that is on the clinical side; what scan body the doctor uses becomes very important as to the workflow that would follow as well, unlike traditional impressions, where the doctor can buy his impression coping, send it to the lab, and then the lab has free reign. The doctor’s making choices for the lab before the lab ever gets the case. My biggest advice I can give anybody is, don’t just do your first case. Communicate with your clinicians. For clinicians, communicate with your lab. Hopefully they’re communicating with their labs before they even purchase a scanner.”
It’s time to embrace tech
Dental professionals that may not embrace CAD/CAM implant creation should consider adding it to their repertoire. The proposition may seem like a prohibitively expensive addition, but it can be added in smaller, easier, more affordable phases.
“I like to advise [labs] to kind of dip their toe in the water before they jump into the deep end, the same way I tell doctors to reach out to their labs before they buy an intraoral scanner,” Ferguson says. “If you’re a lab technician and you’re going to start doing these bigger and more complex cases, or even if it’s the smaller cases and you’re not fully comfortable exactly with how the workflow is, get some information ahead of time. The information’s there. Any company that’s doing this type of work is absolutely there to help you, and they would find it much easier to help you before the case is under way than when it’s midstream.”
Caponigro advises accepting that CAD/CAM is the future and jumping on board.
“Labs that are trying to avoid CAD/CAM technology and sticking to the old ways, they really need to get exposed to CAD/CAM, because it is our future,” she advises. “It does take some investment to make, but you have to invest money before you make money. People who are resistant shouldn’t be afraid. I see a lot of people who say, ‘Fixed bridges on implants, it’s such a complicated thing,’ but before you start doing it, you don’t know how to do it. Just don’t be afraid. Accept that you can make mistakes and things can break. But we learn from our mistakes and our experiences. There’s no point to be afraid and resist. Get your educational level up on the implantology and CAD/CAM technology, and just strive for better results. I see a lot of people who are very skeptical about it, and they shouldn’t be. Of course they’re going to sweat a little bit, but they’re going to get great results with less effort.”
Dr. Gottlander notes that labs must understand how CAD/CAM will fit in with their implant services and existing clients.
“I think everyone can benefit from it, but they have to figure out how much they’re going to use it,” he says. “They have to figure out, should they get involved with the dentist. If my dentist is using an intraoral scanner, I also have to learn about the scan technology, because I, as a laboratory, should provide support services to my customer. If the laboratory does not know about the procedure the dentist is doing, there will be a disconnect. Then, based upon how much volume the laboratory does, they can decide if they want a scanner only. If you go to the big implant labs today, they have machine after machine after machine working 24/7. If you go to a small laboratory, they might have a scanner only and outsource to someone else for production. There’s a solution for everyone, but they have to assess it and base it on where they fit in.”
And while CAD/CAM is changing how some restorations can be delivered-even allowing crowns to be created chairside in the dentist’s office-it affords new opportunities to the entire workflow.
“Dentistry has to embrace digital in all areas,” Dr. Severance says. “Don’t treat it like competition to conventional methods. The times are changing. We know that some dentists can do a lot of the work in their office, which used to go to a laboratory, but that just opens up other avenues for the laboratory to pursue. There’s nobody better at designing a smile or looking at the overall [complexity] of designing teeth than dental technicians, but if the profession rejects the opportunity or if they say, ‘I’m not going to get into digital,’ that’s not going to last very long. It’s really the opportunity for the dental profession to embrace technologies that make you a better dental professional, whether it’s dentists or technicians, so it’s just having an open mind. It’s the same thing when we were taking conventional film for cameras or X-rays and now nearly everything is digital. There are always some that will hesitate, but the ease of use, the advantages to the patient and the dentist and the dental technician are so numerous, you just have to be open to the new opportunities.”
Dental implants are expanding and changing. Whether it’s new software, new systems or new sources of revenue, there are plenty of opportunities to grow along with this exciting trend for every part of the dental team.