How to efficiently remove fixed restorations with crown cutters
Why crown cutters from Komet USA LLC are ideal for working with different restorative materials.
The removal of all-ceramic and porcelain-fused-to-metal (PFM) crowns is routine in modern dental practices where fixed-prosthetic restorations are among the most commonly used treatments. The specific properties of different restorative materials, however, require special crown cutters to ensure effective, efficient removal. This is especially important when dealing with the new generation of high-performance ceramics, which have considerably improved the long-term clinical prognoses of these restorations.
Restoration longevity
Recent studies have shown comparable five-year survival rates for the following anterior crowns: PFM crowns (94.7 percent), all-ceramic crowns made of lithium silicate (96.6 percent) or zirconium oxide (92.1 percent)6. Similar survival rates of 94.4 percent to 95.6 percent were established for tooth- or implant-supported PFM bridges3,4. The failure of a fixed restoration can be due to biological (e.g., secondary caries or endodontic complications) or technical reasons (e.g., material fracture)2,7,8. The failure of tooth-supported PFM crowns and bridges is primarily related to biological complications3,6, whereas implant-supported PFM restorations frequently fail due to technical problems such as fracture of the ceramic veneer1,3-6.
Tooth- and implant-supported all-ceramic bridges and crowns on molars and premolars also exhibit an increased rate of technical complications due to ceramic-veneer fracture2,3,4. To reduce the incidence of such complications, the use of monolithic bridges made of high-strength glass ceramics or translucent zirconium-oxide ceramics is recommended3,6. Common reasons for the biological failure of tooth-supported crowns and bridges include secondary caries and endodontic complications7. In some cases, an anterior fixed prosthetic restoration might be removed because of undesirable esthetics1-6 (Fig. 1).
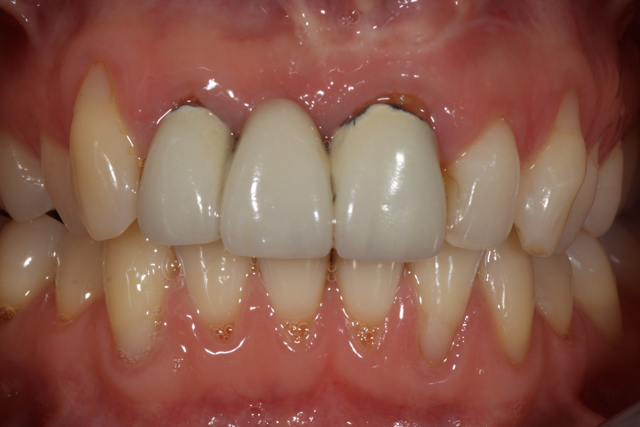
Fig. 1
In summary, clinical data suggest an annual loss risk of approximately 1 percent in cases of fixed crowns and bridges, meaning that one in 100 integrated restorations are expected to be lost per year1-4,6. The removal of all-ceramic or PFM crowns is, therefore, an essential treatment carried out regularly in any dental practice.
Aside from various techniques for the nondestructive removal of crowns and bridges with mechanical or compressed-air powered devices, the most common method for removing a restoration is opening it and then manipulating or breaking it8. Due to the specific properties of the different restorative materials, the removal of PFM and all-ceramic crowns places special demands on the clinical procedure.
Komet USA has created a line of highly efficient instruments to cut through any crown quickly and easily: the H35L crown cutter features a special blade geometry for use on non-precious metal and gold; the H4MC®L cutter for metal and ceramic is ideal for PFM and hard-metal crowns, efficiently cutting through ceramic veneers and any underlying metal structure without requiring instrument changes; and the 4ZR and 4ZRS Jackie™ crown cutters meet the challenges of removing all-ceramic crowns and are especially effective on those made of extremely hard ceramic materials such as zirconia.
The following guidelines present the steps necessary for removing PFM and high-strength all-ceramic restorations using the Komet® H4MCL and 4ZRS Jackie crown cutters.
PFM restorations
Because they contain two different materials that must be separated, PFM restorations present a special challenge for removal. While diamonds are the best option for separating the ceramic portion, the metallic frame is generally best cut with tungsten carbide. Consequently, the removal of PFM restorations traditionally requires a change of rotary instruments during the procedure. Another decisive factor regarding the removal of metallic or PFM restorations is the type of material used in the metal framework. Alloys containing precious metals can be separated fairly quickly and easily. Non-precious metal alloys, however, are considerably harder, so removal takes more time and leads to increased instrument wear.
The Komet H4MCL specialized tungsten-carbide cutter has been developed in response to this challenge. Featuring specially adapted blade geometry, the instrument quickly and easily cuts through alloys with or without precious metal content, and it is equally suitable for removing ceramic veneers. As a result, all-metal and PFM restorations now can be removed with a single instrument.
Removal of PFM restorations
The following points should be observed during PFM removal:
- Operate at an optimum speed of 160,000 rpm and work with minimum pressure. Take care to cool the site with plenty of water (50 mL/min.).
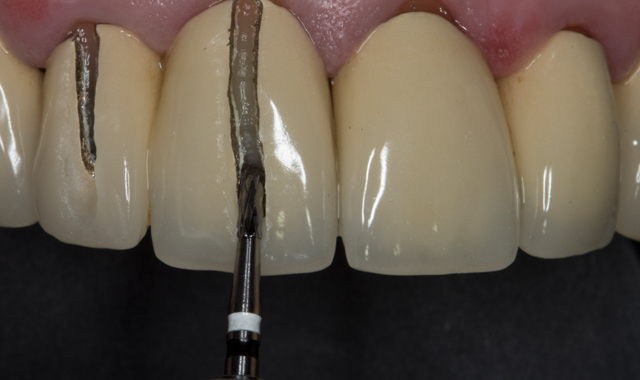
- Use the entire circumference of the instrument to ensure outstanding cutting performance, apply the H4MCL instrument to the crown surface at a 45° angle (Fig. 2).
A two-step crown-separation technique enables the cutting depth to be precisely controlled, and more substance can be preserved as compared to separating both the ceramic and metallic layers in a single step. First, the ceramic veneer is cut open until the underlying metal frame is completely exposed. Next, the frame is opened to expose just the tooth stump surface. When opening PFM restorations, it is generally sufficient to separate the vestibular surface up to the incisal edge or up to the occlusal surface (Fig. 3). The crown then can be bent upward and removed.
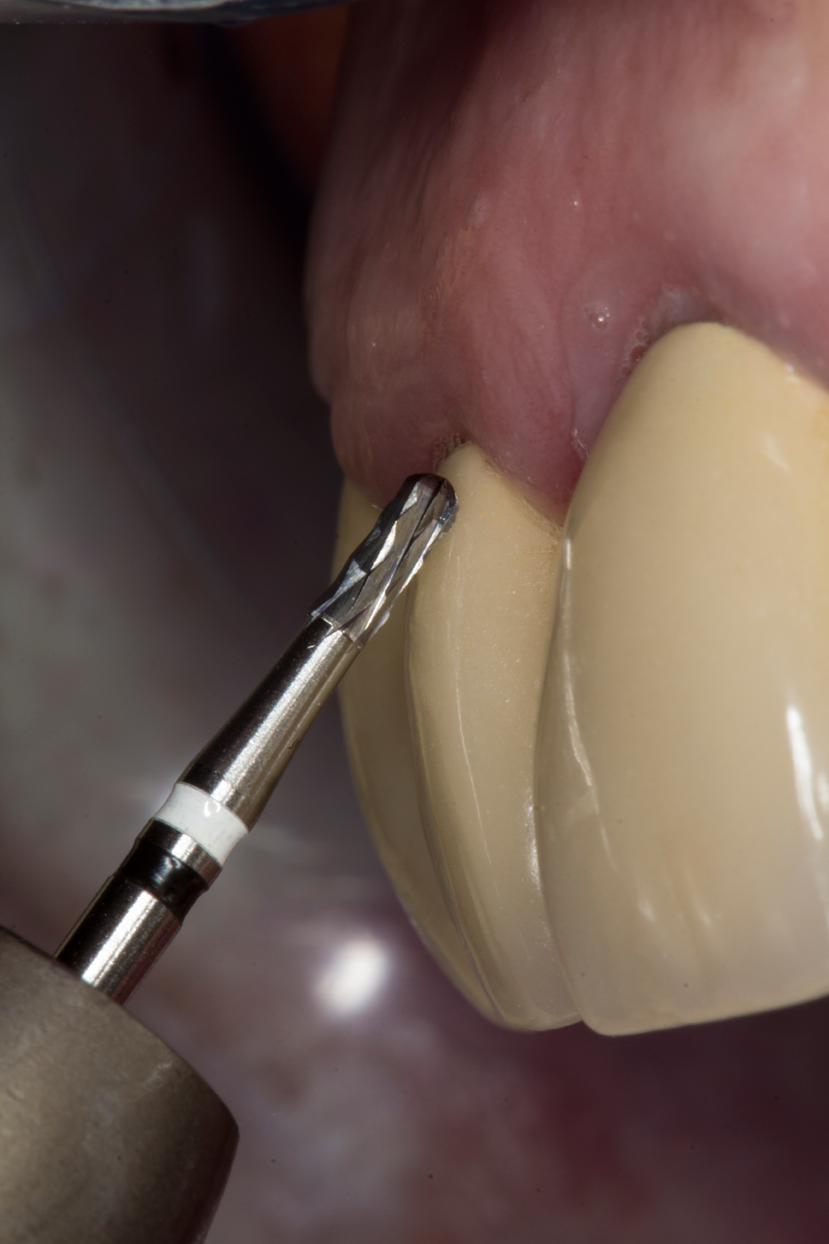
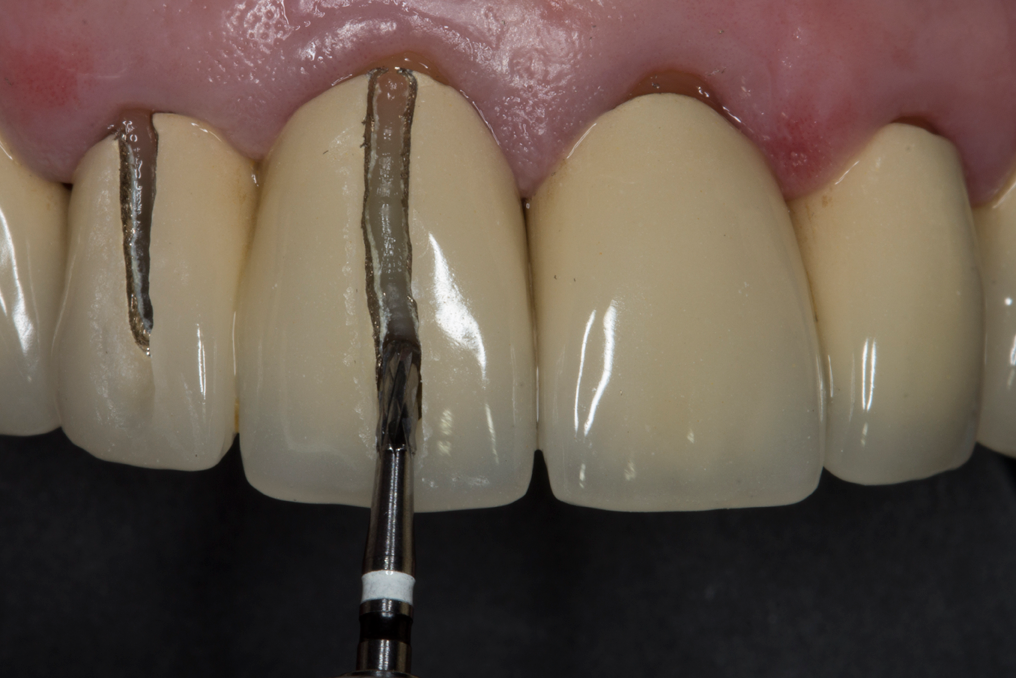
Fig. 2 Fig. 3
Although in principle the crown can be opened with suitable levers, specialized crown-spreading pliers or crown-dilating forceps are safer options. The pliers are introduced into the gap to remove the restorations and the forceps work on the principle of two counter-rotating discs, each provided with four retention claws. When the forceps are pressed together, the two discs rotate and the retention claws push the two halves of the restoration apart. The generated pressure causes the metal frame to open, and the crown can then be removed (Figs. 4a & 4b).
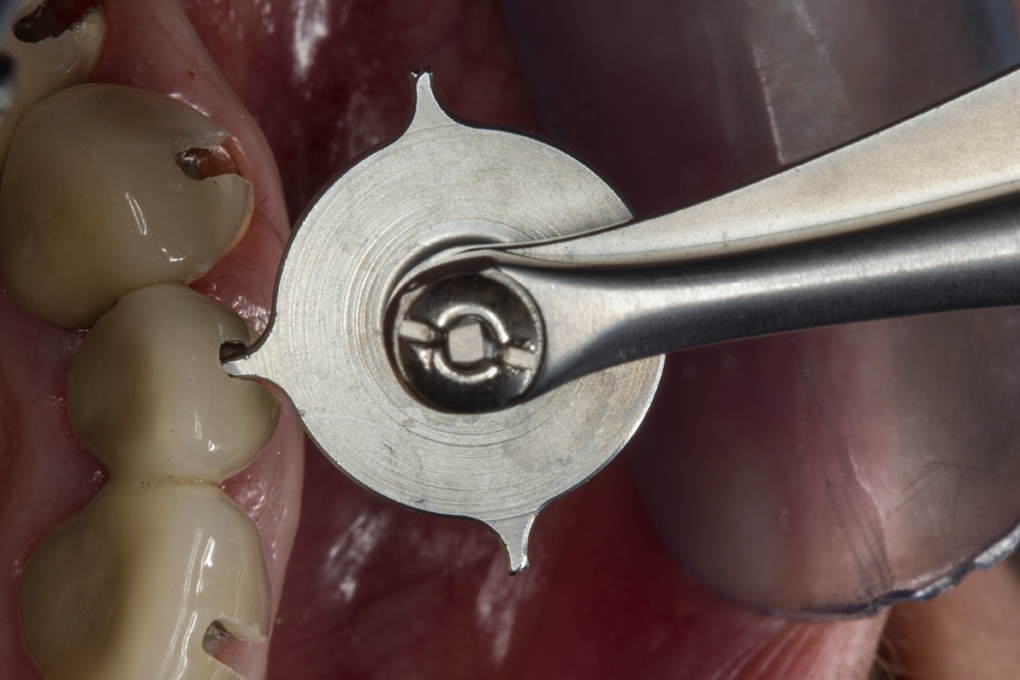
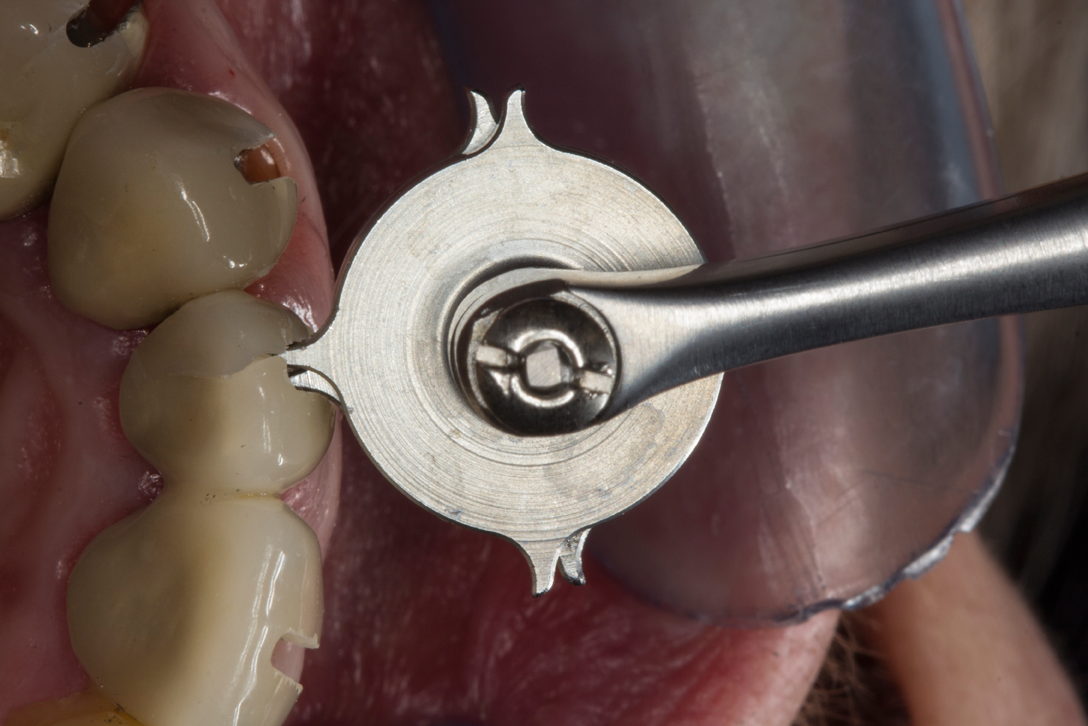
Fig. 4a Fig. 4b
Compared to a simple lever, the pliers offer distinct advantages when opening the restoration:
- Thanks to the special operating principle of these pliers, the tooth is not subjected to bending forces when the crown is opened. This minimizes the risk of accidental tooth fracture.
- The instruments used for leverage can slip and cause damage to hard and soft tissues during use. The crown-spreading pliers work without pressure, significantly reducing the risk of iatrogenic injury.
Removal of all-ceramic restorations
Today’s generation of adhesively bonded, all-ceramic restorations can be extremely difficult to remove. Although traditional ceramic veneers can be cut quite effectively with coarse diamonds, these diamonds are of limited use for modern high-performance ceramics (high-strength glass ceramics and zirconia). Traditional diamond instruments wear down quickly when used on these materials and, as a result, several instruments are needed for the treatment, particularly when cutting monolithic restorations or bridge connectors. This greatly increases the costs and the time required for the treatment. Furthermore, the rapid wear of the instruments leads to increased heat generation and, when working on zirconia, can lead to sparks, even if the site is constantly cooled with plenty of water.
Komet ZR-Diamonds™ are specially designed for use on zirconia and other high-strength ceramic materials. They feature permanently bonded, high-quality diamond particles arranged in a densely packed diamond layer, making them considerably more durable and capable of removing far more substance than traditional diamonds. A new addition to the ZR line, the 4ZRS Jackie crown cutter, is tailor-made for removing all types of ceramic restorations; it is uniquely engineered to slit crowns and bridges to simplify final fracture and removal with a hand instrument. Thanks to a short (4 mm), tapered working end, the cutter is perfectly suited for separating restorations on both anterior and posterior teeth. In addition, it is less prone to fracture than instruments featuring longer working ends.
The following general recommendations should be observed during the clinical use of these instruments:
- The optimum speed is approximately 160,000 rpm. Use with a red contra angle is recommended because the higher torque of the contra angle - as compared to dental turbines - allows more effective work on ceramic.
- To avoid excessive heat generation while opening the ceramic restoration, take care to cool the site with plenty of water (> 50 mL/min.). Work with gentle pressure.
- For best cutting results, apply the instrument at a 45° angle (Fig. 5).
To remove the high-strength ceramic restoration, open it along an axial surface, minimally exposing the hard dental substance underneath. For crowns on anterior teeth, the cutting point is extended beyond the incisal edge, thereby leaving the palatal or lingual wall intact (Fig. 6).
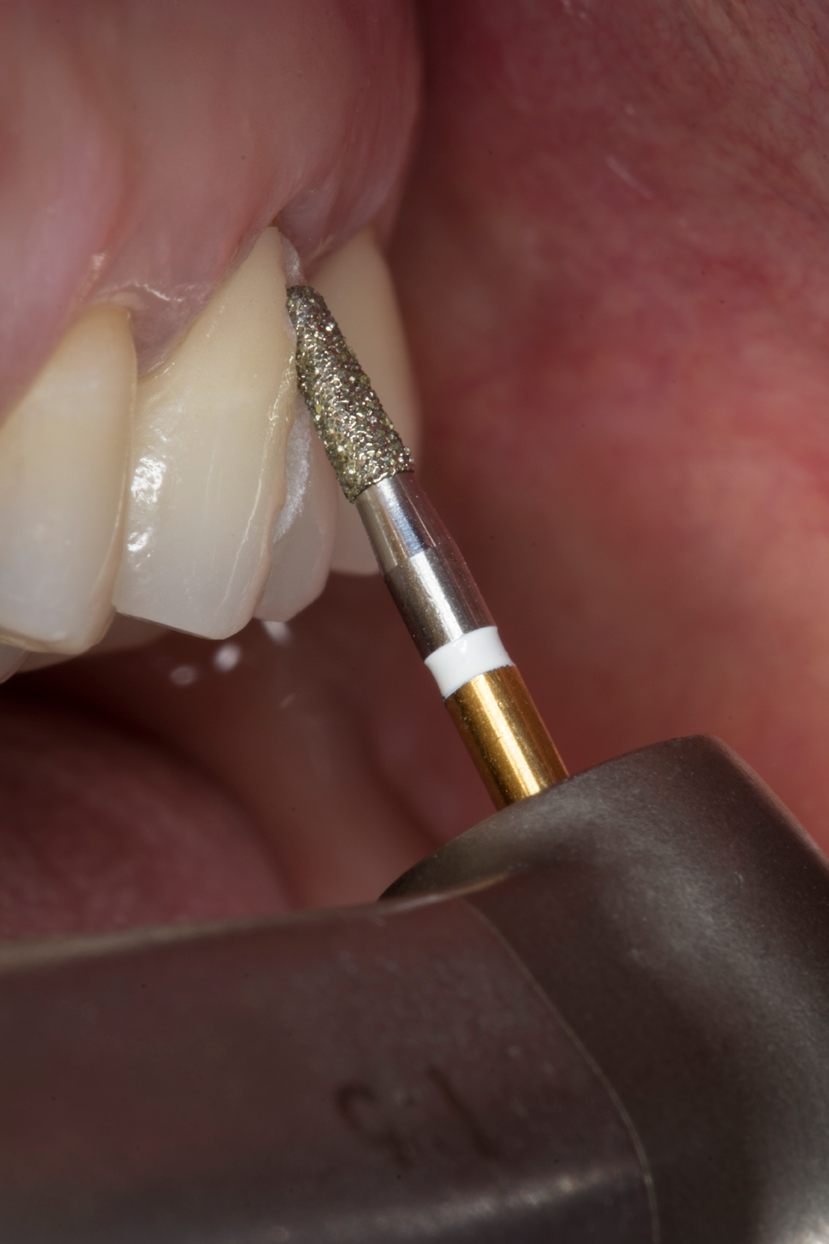
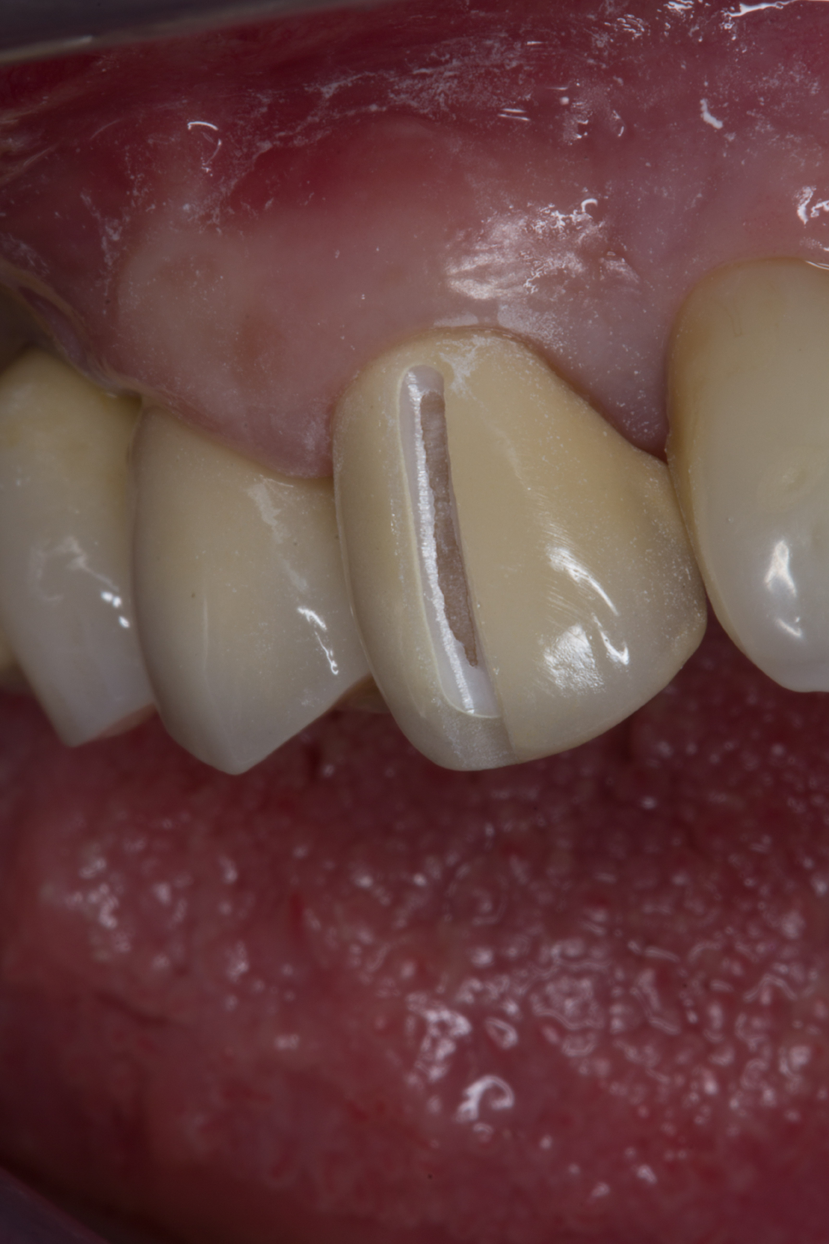
Fig. 5 Fig. 6
In case of traditional, cemented zirconia crowns, the crown-dilating forceps should be used only once following the opening of the restoration; this facilitates the fracture and removal of the entire restoration in the region of the remaining axial wall. For posterior crowns, both the axial wall and the occlusal surface should be opened to ensure that the restoration can be fractured with ease. Thanks to the short working end of the crown-cutter, the ideal angle can be achieved even in the posterior region (Fig. 7).
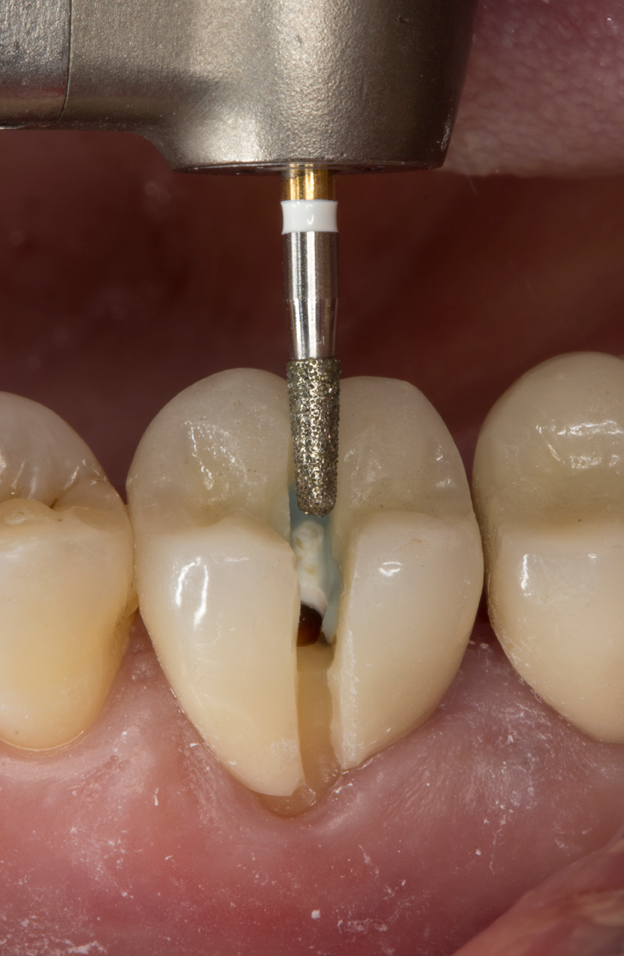
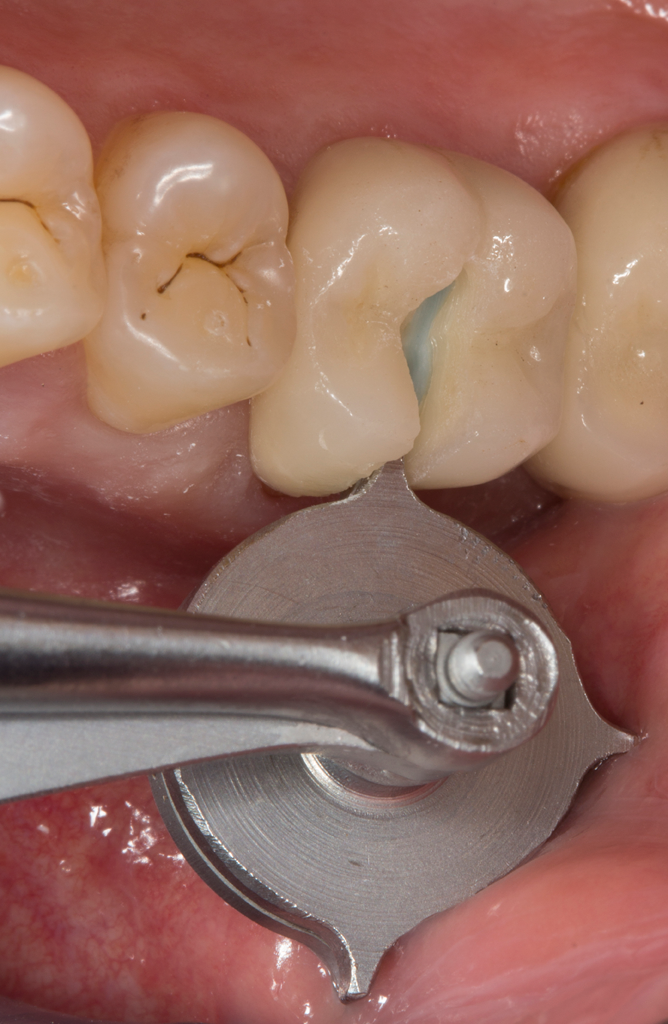
Fig. 7 Fig. 8
For a traditional, cemented zirconia crown, special forceps can be used to open the restoration until it breaks (Fig. 8). The fragments then can be removed with relative ease. If the restoration is adhesively fixed, the forceps should be applied as far as possible in a cervical direction so the restoration does not fracture completely but can be removed in segments. Once the first few segments have been removed, the forceps are applied again at the separating slit - this time further in an incisal/occlusal direction - to remove the remaining segments one by one.
If the remaining intact lingual or palatal crown surface fails to come off, a separating slit should be cut in this area and the forceps can be used once again. Any remaining fragments can then be removed with sonic tips (SF979.000.014, Komet USA) or with an 8mm-long crown cutter for all-ceramic crowns (4ZR.FG.014, Komet USA).
Conclusion
The removal of prosthetic restorations is a routine treatment in today’s dental practice. All restorative materials require tools and treatment concepts that are specially adapted to their specific properties. Metallic and PFM restorations can be efficiently separated with suitable tungsten-carbide instruments, while all-ceramic restorations can be universally removed with diamond instruments specially developed for work on high-performance ceramics. For the dental practice, this means that two types of instruments are sufficient to remove both PFM and all-ceramic restorations (Fig. 9).

Fig. 9
For more information on the full line of specialized crown cutters from Komet USA LLC, call 888-KOMET-USA (566-3887) or visit www.kometusa.com.
This article was originally published in the Dental Magazin, published by Deutscher Ärzteverlag. This translated version is reprinted here by permission.
References:
1: Jung RE, Zembic A, Pjetursson BE, Zwahlen M, Thoma DS. Systematic review of the survival rate and the incidence of biological, technical, and aesthetic complications of single crowns on implants reported in longitudinal studies with a mean follow-up of 5 years. Clin Oral Implants Res. 2012 Oct;23 Suppl 6:2-21.
2: Minguez C, Lyons K. Failure of crowns and bridges--a review of the literature. N Z Dent J. 2007 Mar;103(1):7-13.
3: Pjetursson BE, Sailer I, Makarov NA, Zwahlen M, Thoma DS. All-ceramic or metal-ceramic tooth-supported fixed dental prostheses (FDPs)? A systematic review of the survival and complication rates. Part II: Multiple-unit FDPs. Dent Mater. 2015 Jun;31(6):624-39.
4: Pjetursson BE, Thoma D, Jung R, Zwahlen M, Zembic A. A systematic review of the survival and complication rates of implant-supported fixed dental prostheses (FDPs) after a mean observation period of at least 5 years. Clin Oral Implants Res. 2012 Oct;23 Suppl 6:22-38.
5: Sadid-Zadeh R, Kutkut A, Kim H. Prosthetic failure in implant dentistry. Dent Clin North Am. 2015 Jan;59(1):195-214.
6: Sailer I, Makarov NA, Thoma DS, Zwahlen M, Pjetursson BE. All-ceramic or metal-ceramic tooth-supported fixed dental prostheses (FDPs)? A systematic review of the survival and complication rates. Part I: Single crowns (SCs). Dent Mater. 2015 Jun;31(6):603-23.
7: Schwass DR, Lyons KM, Purton DG. How long will it last? The expected longevity of prosthodontic and restorative treatment. N Z Dent J. 2013 Sep;109(3):98-105.
8: Sharma A, Rahul GR, Poduval ST, Shetty K. Removal of failed crown and bridge. J Clin Exp Dent. 2012 Jul 1;4(3):e167-72.