How guided implant surgery can deliver better patient care
How digital tools and communication come together to deliver safer, more dependable implant results.
As dentistry has moved to a digital platform, more clinicians and labs have started taking advantage of enhanced communication tools in order to provide greater patient care.
The accuracy currently achievable with digital dentistry is unparalleled. This accuracy, along with teamwork within the surgical and restorative team, is creating workflows where the final outcome can be visualized before a case is started.
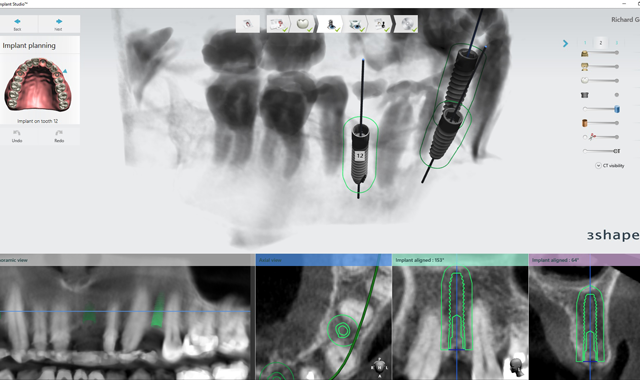
Implant dentistry is no different. Using 3Shape software (Implant Studio and Dental Designer), the entire restorative team (lab, restoring doctor and surgeon) can plan the surgery and restorative options based on the planned implant placement. Benchtop testing is showing fully guided implant surgery places the implant within .1 mm in all directions of planned placement. This certainly allows for the ability to place better temporary restorations or healing abutments than what has been used in the past.
Trending article: 7 ways 3D printing is changing everything
Case study
1. In Figure 1, we have an intraoral photograph of the patient with existing metal reinforced temporary bridge, which is planned for replacement with three implants and individual crowns. In Figure 2, we see another intraoral photograph after removing a PFM bridge, to reduce scatter in the DICOM image of the bone.
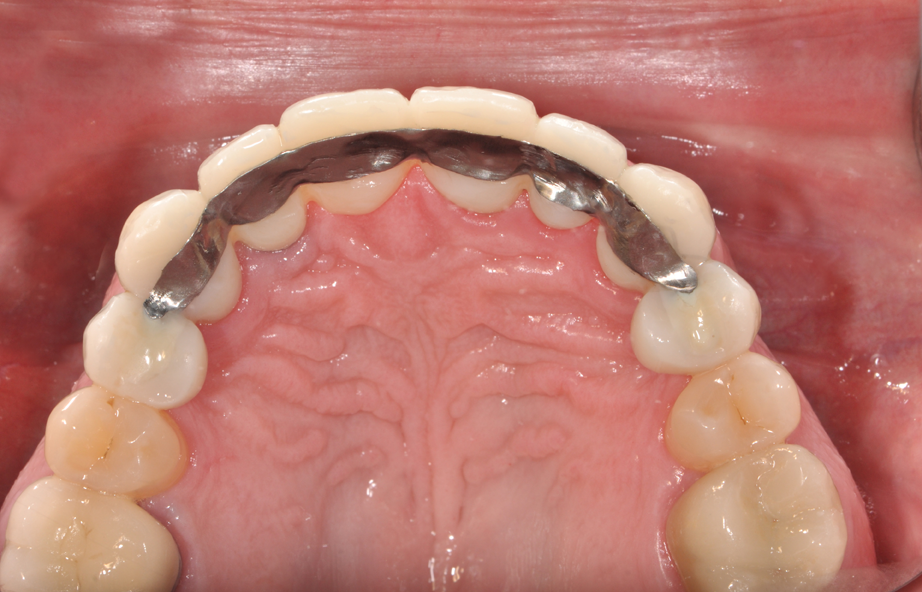
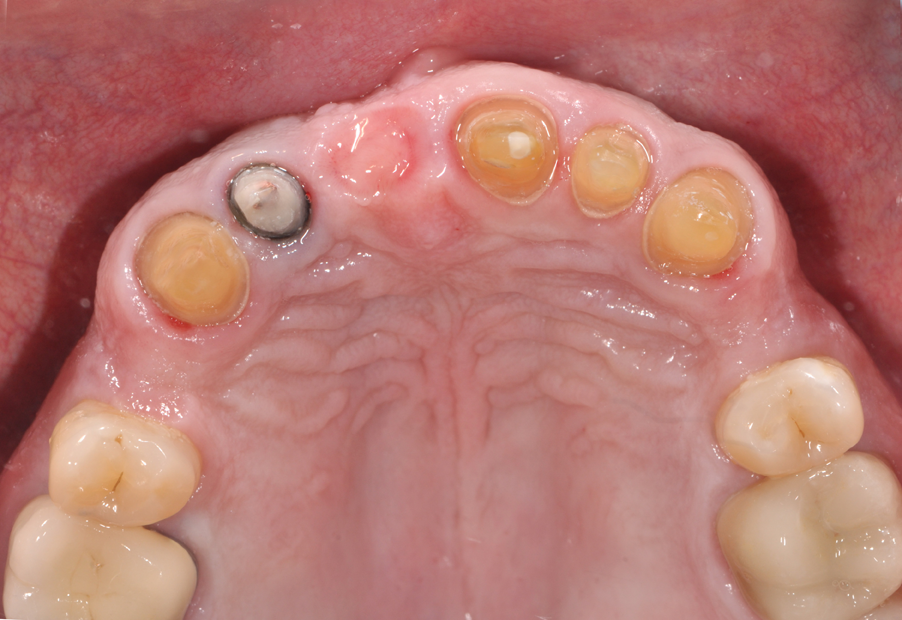
Fig. 1 Fig. 2
2. This patient was then scanned with a 3Shape TRIOS intraoral scanner. The resulting color scan is shown in Figure 3. This scan was then pulled into 3Shape Implant Studio and aligned with the DICOM data, and placement of three BioHorizons Implants was planned. Tooth position #12 was planned with a 3.0 mm x 15.0 mm implant. In Figure 4 you can see the root formations for teeth 11 and 13 created a limited space situation.
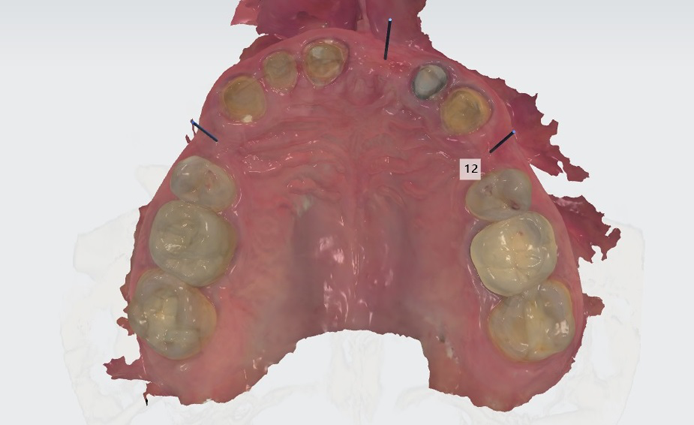
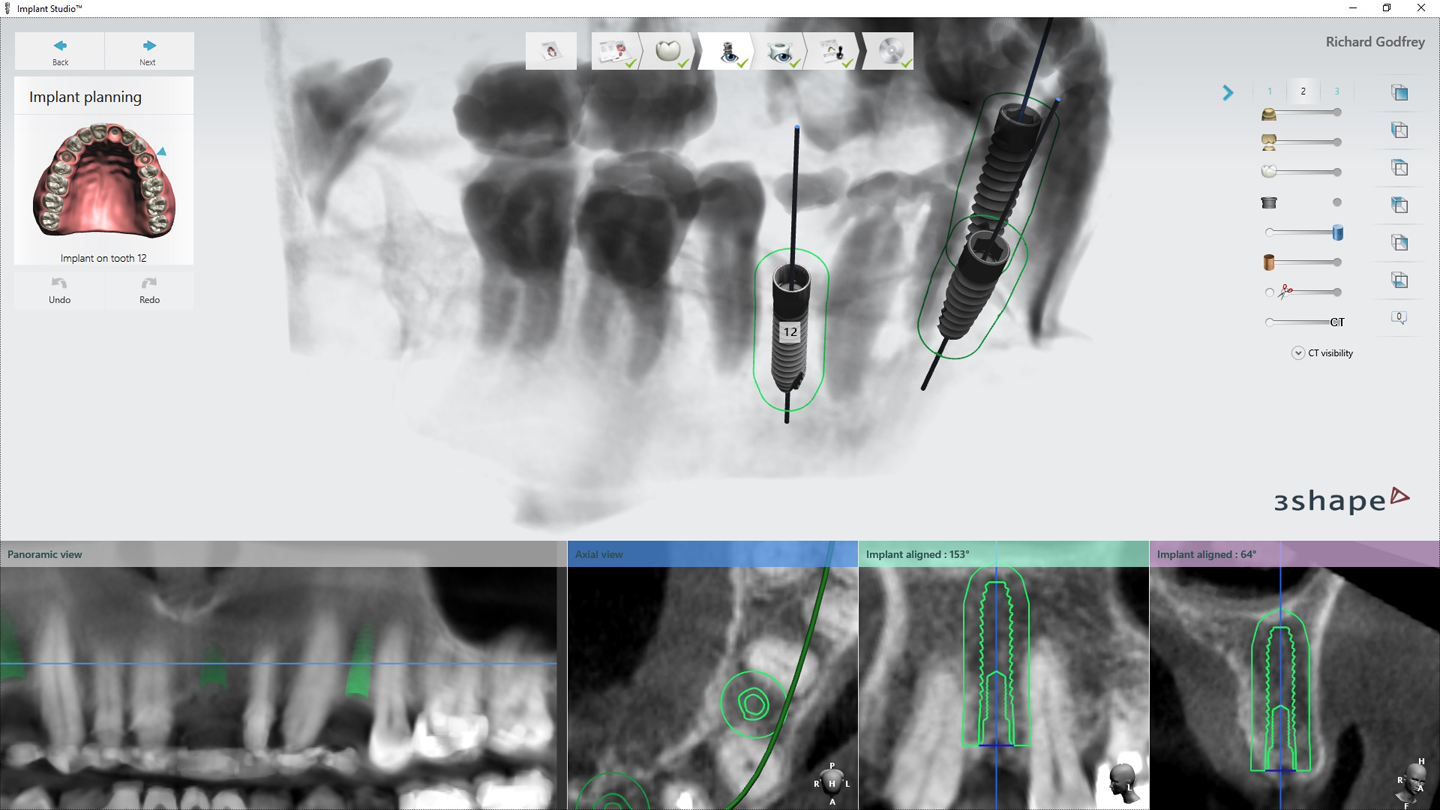
Fig. 3 Fig. 4
3. Implant placement was planned during a conference call between the surgeon, the restoring doctor and the lab. In this instance, the restoring doctor wanted to place screw-retained crowns for each of the implant sites. Thus, angulation of implant for tooth #8 was critical as well as the safe placement of tooth #12. Once the placement was agreed upon by all involved with the case, a surgical guide was created. Figure 5 shows the printed guide. Figure 6 shows the guide during try-in.
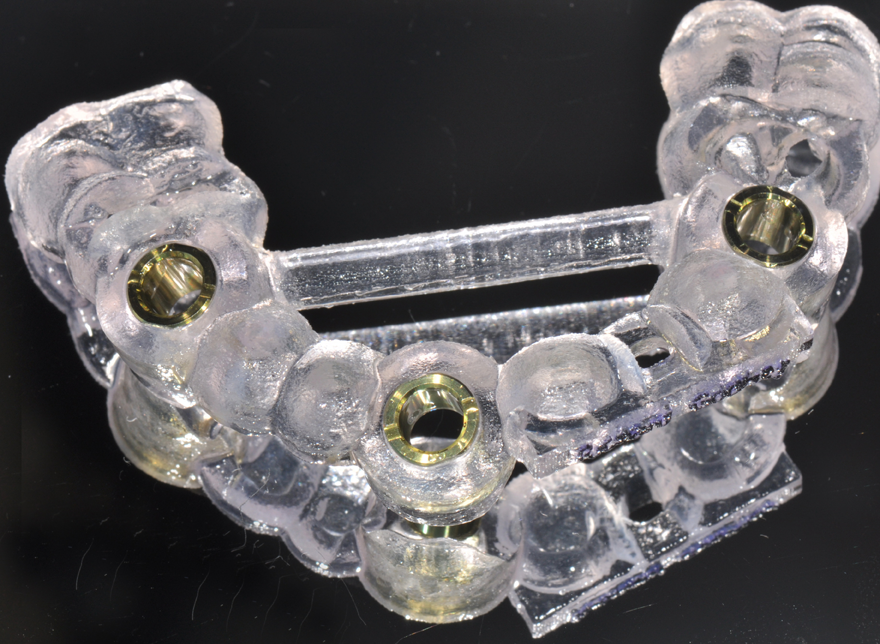
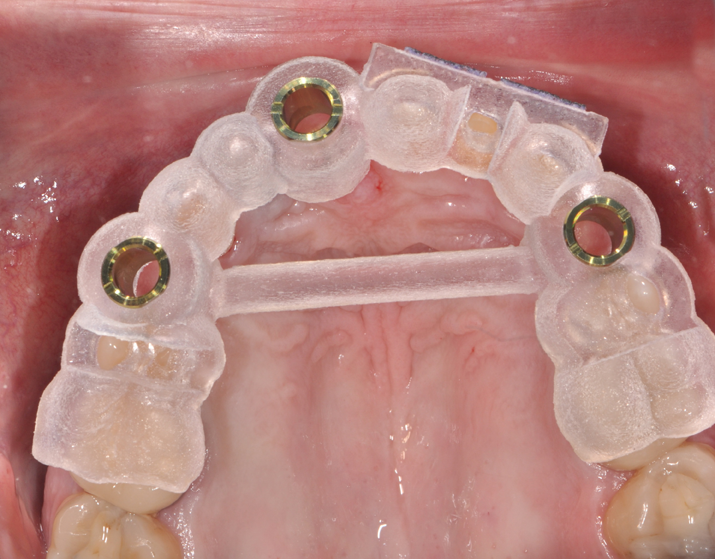
Fig. 5 Fig. 6
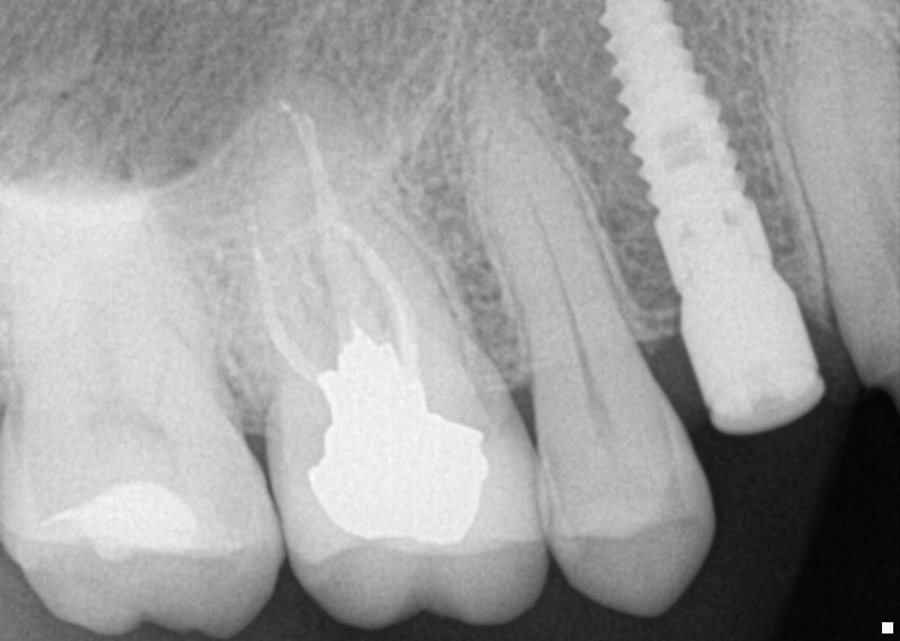
4. After surgery, several X-rays were taken to verify implant placement. Figure 7 shows accuracy to the guided placement for the implant in tooth #12 position (which mirrors the planning stage of Figure 4). Figure 8 shows the implant in tooth #8 position with healing abutment. Figure 9 shows the placement of the implant for tooth #5.
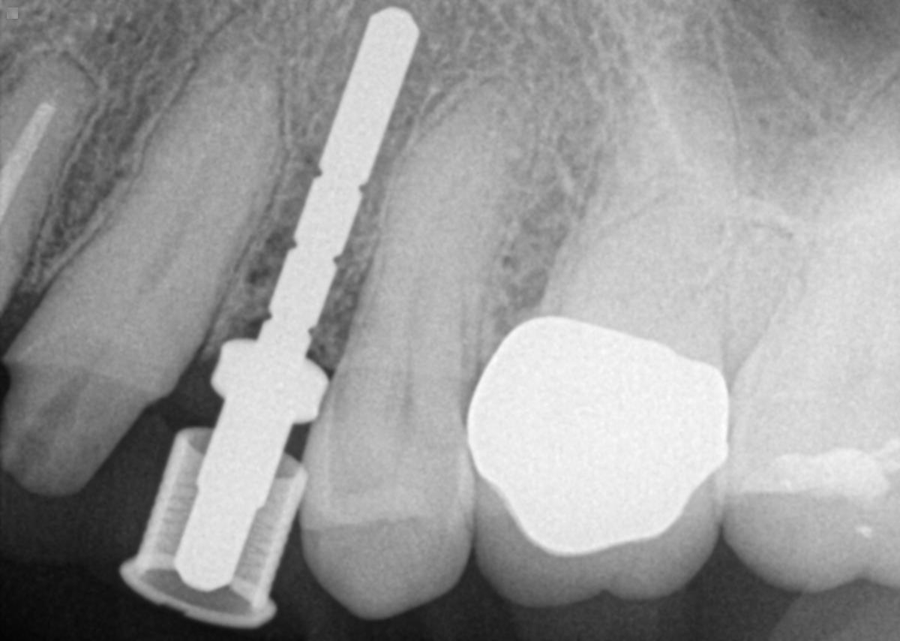
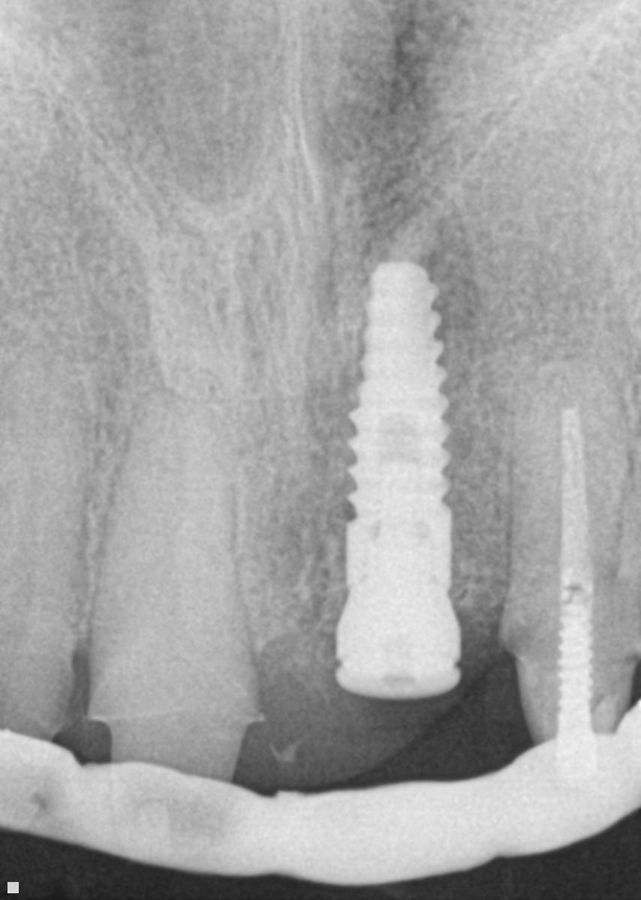
Fig. 7 Fig. 8
More from the author: Why it's time to embrace the digital workflow
Conclusion
Fig. 9
Through the use of guided surgery software, this case was preplanned based on a particular restorative selection. In this case, the choice was screw-retained crowns and single unit restorations for the anterior eight units. By using technology, the entire restorative team was able to discuss the case and see potential difficulties each member would face. The implant for tooth #12 was difficult based on limited space between the adjacent roots. Tooth #8 was carefully planned in order to allow for a screw-retained crown with the access hole coming through the lingual.
By using a guide and preplanning the case, the implant surgeon felt confident he would be able to place the implants optimally, and the restoring doctor and lab knew the implant restorations would be able to blend nicely with the final crowns on natural teeth.