Exploring an innovative model for specialty dental care delivery
How the Pediatric Dental Initiative of the North Coast is changing the way the industry addresses pediatric dental care in underserved populations.
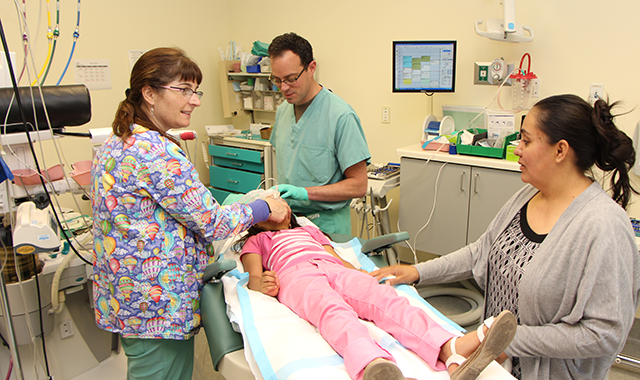
Dental disease is the nation’s number-one preventable childhood disease, and there is a serious lack of resources providing dental care for children, especially those on Medicaid.
The Pediatric Dental Initiative of the North Coast (“PDI Surgery Center” or “PDI”) model is one that could be followed by others throughout the nation to provide greater access to care for underserved children.
A national epidemic
Severe tooth decay is national epidemic. According to the Kaiser Commission, “Oral disease has been linked to ear and sinus infection and a weakened immune system, as well as diabetes, and heart and lung disease.” Poor dental health disproportionately affects children from low-income families and leads to a lifetime of health problems that cost many billions to address.
Related reading: 9 of the scariest medical conditions with links to oral health
“When money's tight, dental care is something people put off to the very end, failing to realize it's crucial to overall health”, Dr. Michael McCunniff, chairman of the University of Missouri-Kansas City Department of Public Health and Behavioral Science, says. “Thirty-one percent of our nation’s seniors have no teeth. In 2017, dental pain alone accounted for more than one million emergency room admissions in adults and children costing more than a billion dollars.”
Because of low Medicaid reimbursement rates and sporadic payments many dentists are unwilling to treat patients on Medicaid. In California, 25 perce t of children start kindergarten with tooth decay, and in Sonoma County California, where 47 percent of PDI patients live, there are only 1.5 pediatric dentists (three part-time positions) providing treatment for 46,711 children on MediCal. Nationally, children on Medicaid and patients with special needs (autism, Down syndrome and cerebral palsy, or severe anxiety) face similar challenges leading to severe, untreated tooth decay.
Trending article: Why prevention is cheaper than restoration when it comes to gum disease
By law, hospital emergency rooms have to see patients even if they can't pay. These visits cost more than three times as much as a routine dental visit, costing the U.S. health care system $1.6 billion a year. A Children Now policy brief states, “For every dollar spent on preventative dental services for children, $8 to $50 is saved in restorative and emergency treatments later in life.” By providing safe, low-cost dental treatment and comprehensive preventative services, the PDI model reduces the number of visits to hospital emergency rooms and missed school days and lowers costs for tax payers.
The model
PDI’s innovative model addresses this national problem. A nonprofit, stand-alone AAAHC- and CMS-licensed Ambulatory Surgery Center, PDI treats children from underserved families who are suffering from such severe dental decay that they require surgery under anesthesia.
Two operating rooms are staffed with a dentist, medical anesthesiologist and registered dental assistant, and two registered nurses monitor patients’ recovery in the post-op room. Because these are the only surgeries performed at PDI, specialization and volume allow for shorter turnover times with patient-centered care provided in a sustainable manner. PDI dentists and anesthesiologists work two to three times a month, allowing them to continue working in their own practices, hospitals or anesthesia groups.
Trending article: Does early preventive dental care for kids lead to more long-term care?
Dentists in private practice, federally qualified health centers, community clinics or tribal health clinics attempt treatment in their own facilities. If they are unable to complete it, they refer the patient to PDI. Patients are only treated at PDI if their tooth decay is severe or the patient has special needs that make sitting in a dental chair for treatment impossible. The average patient age is three and on average have 12 teeth requiring treatment. A post-op report is sent to the referring dentist.
Since opening in 2008, more than 22,000 children have received treatment for severe tooth decay. PDI also serves as the permanent home for another 200 special-needs patients aged up to 25 whose families have been unable to find a dentist to treat them.
Continue to page two to learn more about PDI's prevention education...
Prevention education
In 2018 alone PDI’s prevention education programs reached 21,305 people, through a dual approach of in-house and community based outreach activities.
On-site prevention education: While their child is in surgery, PDI's in-house oral health educator meets one on one with parents/guardians to explain the causes and dangers of tooth decay, the importance of a healthy diet and good oral-health habits. She stresses the danger of sugary beverages and high-carb foods.
According to a 2018 UCLA Health Policy fact sheet written by Susan H. Babey and Joelle Weinstein, “Consumption of beverages that have added caloric sweeteners such as sucrose or high fructose corn syrup, is associated with overweight and obesity, increased risk of type 2 diabetes, metabolic syndrome, liver disease and dental decay, as well as decreased consumption of more nutritious foods such as fruits and vegetables.”
When parents leave PDI, they are given a dental health kit (toothbrush with timer, toothpaste, floss, tooth brushing chart) and written instructions in their native language, as well as a bag of produce and groceries together with simple healthy recipes.
Trending article: 5 ways to get your patients to brush their teeth
Community-based prevention education: Recognizing the need to reach families before their child is in pain, the Promotores (lay health worker) Program was created to provide culturally and linguistically appropriate oral health prevention education to families in their own communities explaining how to maintain good overall health, and helping them to access health insurance, find a permanent dental home and obtain services and advice as needed.
PDI’s three bilingual and bicultural promotores provide culturally appropriate services and serve as patient advocate, educator, mentor, outreach worker and translator. They are the bridge between the diverse populations PDI serves and the healthcare system.
Promotores participate in community events such as resource fairs/ health fairs, schools and outreach events; provide rides to and from the surgery center for families who may live in rural areas and have difficulty accessing transportation; make home visits to families whom clinical staff consider to be “at risk”; and train staff at other nonprofit agencies to become promotores through PDI’s “train the trainer” program. The promotores’ goals are to:
- Provide oral education to families
- Ensure that children with dental decay receive prompt treatment
- Provide parents with the necessary tools and information to maintain healthy teeth
- Ensure that families have good overall health through healthy diet
- Assist families to find a permanent dental home
- Help families to access social services available in their communities
To quote Dr. Ruchi Sahota, a California dentist and consumer adviser for the ADA, "Prevention is priceless." Dentists at PDI treat all four quadrants of a child’s mouth so when children leave the surgery center, they have healthy mouths, and the oral health educator has given parents the knowledge to maintain their family’s dental health.
The value of PDI’s dual approach to dental disease is clear. Providing treatment, prevention education, and general support to low-income children and their families helps them overcome cultural and economic barriers to care and builds the foundation for a healthy future.
Trending article: 8 easy ways to educate your dental patients on the oral-systemic link
Replication
By providing safe, low-cost dental treatment and comprehensive preventative services, the PDI model reduces the number of visits to hospital emergency rooms and missed school days, and also lowers costs for tax payers. PDI effectively serves 33 counties in Northern California. Funding for building or leasing and equipping a surgery center, prevention education and transportation-cost assistance, as well as billing methods and appropriate staffing, must all be considered before going forward.
The model would be challenging for Federally Qualified Health Centers that are typically reimbursed on a per patient visit but would work well for other health-related related nonprofits. PDI is reimbursed on a per tooth basis and relies on funding from foundations, government agencies, corporations and private donors to support prevention education and other programs. The PDI model is easily replicable and could be implemented throughout the nation. Doing so would provide an invaluable service to some of the most vulnerable in our society.
For more information go to www.pdisurgerycenter.org or http://pdisurgerycenter.org/contact