Is this newer anesthetic injection technique better for patients?
Taking a look at the Anterior Middle Superior Alveolar injection and the impact it has on patient care.In the world of oral anesthesia, this injection is fairly new. If you have been practicing for more than five years, you may not have been introduced to it in your pain management course. It is gaining popularity particularly for its potential uses in cosmetic dentistry.
In the world of oral anesthesia, this injection is fairly new. If you have been practicing for more than five years, you may not have been introduced to it in your pain management course. It is gaining popularity particularly for its potential uses in cosmetic dentistry.
The Anterior Middle Superior Alveolar (AMSA) injection is a palatal injection that anesthetizes pulpal tissue of incisors from the midline thru premolars, including the facial periodontium and the palatal tissue from the midline to molars. This affects the Anterior Superior Alveolar (ASA) and the Middle Superior Alveolar (MSA) nerves. It was introduced to the dental field around 1997 when the Computer-Controlled Local Anesthesia Delivery system (CCLAD) emerged.
Related article: How to make anesthesia less of a pain
The AMSA can be described as a field block. It effects the terminal branches of the ASA nerve and the MSA nerve when present (approximately 30 to 50 percent of individuals lack this nerve). Because the anesthetic is deposited on the palate, the nerves innervating the upper lip are not affected, therefore allowing for normal lip function, which is ideal for when the patient needs to maintain upper lip function.
How do you administer?
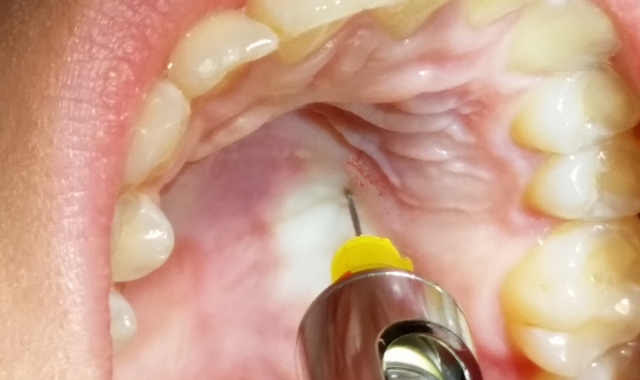
This injection can be done manually or with a computer-controlled delivery device. Using a 27 or 30 gauge short needle is best. The point of insertion is halfway between the gingival margin of the maxillary premolars and the palatal midline raphe (this is where the horizontal and vertical portions of the maxilla join), and between the first and second premolars. Insert the needle until bone has been contacted, after a negative aspiration deposit desired amount of local anesthetic typically 2/3 to a full cartridge (1.4-1.8 ml). As the anesthetic is deposited the palatal tissue will begin to blanch, allowing the clinician to see the extent of the tissues affected. The delivery time is rather slow when performed manually due to the nature of the palatal tissue. The use of a computer-aided delivery device is usually recommended due to clinician fatigue because of the duration of deposit time. However, this author has successfully used manual deposition for this injection with great success.
Pros and cons
There are several pros with this injection. Because of the wide field of tissue anesthetized, few injections are needed for quadrant anesthesia. A traditional approach to anesthetizing the entire quadrant would require four to five injections. The posterior superior alveolar (PSA), MSA and ASA, nasopalatine (NP) and greater palatine (GP) injections would be required. If using the AMSA, the clinician may only need to perform two injections: the PSA and the AMSA. Another benefit is the patient’s upper lip will retain normal sensation and function, making it easier for restorative esthetic dentistry and for the patient’s ease of life after the procedure. Perhaps the patient has a meeting he or she needs to attend after the dental appointment. Now, he or she can continue on with the day with normal lip function. Due to fewer injections, the potential to use less anesthetic is a great bonus.
In my opinion, the use of 4% Articaine with 1:100,000 mg of epinephrine and the AMSA are a match made in oral anesthesia heaven. Due to the potency of this anesthetic, the clinician can achieve profound anesthesia with less anesthetic than 2% Lidocaine with 1:100,000 mg of epinephrine.
More from the author: Should you become a dental hygiene educator?
The drawbacks to this approach are important to consider as well. Due to the dense palatal tissue, manual deposition can take longer than expected and the clinician may develop hand fatigue. Also, incomplete anesthesia with the central incisors due to cross-over innervation are of concern. Depositing more anesthetic using the infiltration technique easily remedies this problem.
Something for the clinician to keep in mind is for patients who have a history of poor healing, palatal injections given with anesthetics containing vasoconstrictors could develop a post-operative ulcer. This has been seen in patients whom are severely immunocompromised.
When you first begin to use this injection, you may not have success with it right away. Be patient as you progress. You will find that this injection is very forgiving regarding deposit site unlike many of the other injections we administer.
Reference: Bassett, K.B., DiMarco, A.C., Naughton, D.K., 'Local Anesthesia for Dental Professionals,' 2nd ed.
Photo Credit: Taken by Tina Clarke RDH MEd. Clinician: Erik Rojas, Senior DH Student (Oregon Tech) Patient: Kelsey Leon Senior DH Student (Oregon Tech)