The economics of ergonomics
In part three of Dental Product Report's three-part series on ergonomics, Garrett Ludwig, president of Diversified Design Technologies, explains how ergonomics can increase a practice's efficiency and productivity-all while saving money. Check out Part 1 and Part 2 of the series for more insight into ergonomic practices and benefits.
In part three of Dental Product Report's three-part series on ergonomics, Garrett Ludwig, president of Diversified Design Technologies, explains how ergonomics can increase a practice's efficiency and productivity-all while saving money.
Check out Part 1 and Part 2 of the series for more insight into ergonomic practices and benefits.
Although the nature of our work as designers obligates us to understand the bio-mechanics of ergonomic function, I will reserve commentary regarding healthy practices and prevention of occupational injury to experts like Bethany Valachi. Rather, I will focus on the economics of
ergonomics
.
The Epiphany
We humans are an odd lot. We can absorb, intellectualize and proselytize about all of the things that are good for us. But, more often than not, we don’t practice what we preach- until we have an “Aha” moment. Although there are many more factors to consider, it is my hope that, what follows will inspire such a revelation, resulting in change.
Related reading: Part two: The biggest ergonomic mistakes dental professionals make
Consistency
As remarkable as it may seem, the number one cause of reduced efficiency and productivity [that I have witnessed in clinical practice] is lack of consistency in the orientation of clinical adjuncts. Perhaps it is a result of incremental practice growth and like-product availability.
But, I constantly see practices with profound variations in everything from patient chairs, doctor’s/assistant’s stools, to dynamic and hand instrument delivery. That includes adjuncts like, intra-oral lights, trituators, curing lights and impression materials.
Beyond the stresses associated with the dysfunction that results from these inconsistencies, these conditions rob you of valuable production time. Gross movement aside, the uniform orientation of instruments and adjuncts will shave calculable amounts of time off of production.
Besides the evident increase in revenue, achievement of this goal will be truly realized when the only distinguishing factor between rooms is the view out the window.
Gross Movement
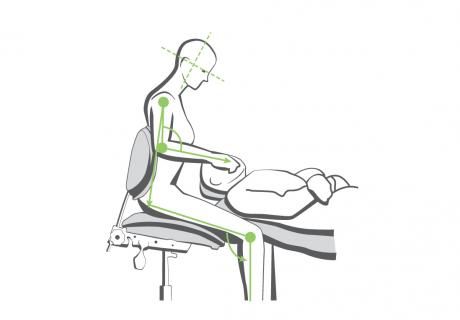
I attended a Four-Handed Dentistry training program during its early development in the late 70’s. At that time, the prescribed recommendation for movement* by the clinician was limited to Class II. Correlatively, trans-thoracic handpiece delivery was the “rule” and the passing of instruments and handpie
ces, left the clinician’s hands in a perpetual carpal-tunnel-provoking position; bi-lateral to the oral cavity. Ergonomic research has resulted in advancements in clinical practice, which are now more user-friendly. To wit the recommendations regarding range-of-motion include Class III and occasional Class IV movements [such as adjusting an intra-oral light] for clinician and assistant.
Related reading: How to handle daily pain in the dental office before it becomes chronic [VIDEO]
I believe that most dentists follow those principles. However, I often observe chair-side assistants, whose range-of-motion pushes the limits of Class IV movement, and often extends to Class V movement; including having to stand and/or bend to access equipment and supplies. Not only do these movements consume time and retard function due to superfluous motion, there is a loss of visual access to the oral cavity and the reasonable ability to suction, retract and irrigate during a procedure. As a result, efficiency and productivity are compromised.
Space Consumption
For the sake of discussion, please assume the following:
1. The average space consumed by patient and exam chair is approximately 24 inches.
2. A comfortable distance between the patient chair and lateral work surfaces for both clinician and assistant is approximately 30 inches.
3. Based on the postulate that form follows function, and the axiom that the human anatomy will perform most efficiently in a defined field of movement, an ideal space accommodation of seven feet should suffice between support surfaces. To reach beyond this work zone would defeat the goal of ergonomic adjacency.
As a result, the determination of total treatment room width will ultimately be defined by the lateral work surfaces themselves; call them “power-wall” systems or simply cabinets and counters.
Theoretically, if a 15” deep counter would adequately accommodate a sink and work surface, then a room width of 9 feet, 6 inches should suffice. Why then would any design professional propose treatment rooms that are ten feet or ten-and-one-half feet wide? Effective use of that redundant space would equate to a savings of three feet to six feet of that could be valuably utilized by other clinical or administrative areas. Waste not, want not.
I. Fingers
II. Fingers and wrist
III. Fingers, wrist and elbow
IV. Arm and shoulder
V. Torso