The best clinical x-ray products and practices for your dental practice
DPR presents the first in a two part series examining the latest and greatest in digital radiography, including must-have products and the best practices for your practice.
DPR presents the first in a two part series examining the latest and greatest in digital radiography, including must-have products and the best practices for your practice. When it comes to digital sensors, there's always more than meets eye. Information provided by Suni If you have ever been in the market for a new digital intraoral x-ray sensor, you are probably familiar with the term “line pairs per millimeter.” Sensor companies love to toss this term around. It is an easy way to convey the purported imaging capabilities of a sensor, and it is represented conveniently by a number. The higher the number, the better the image quality, right? RELATED: New SuniRay2 intraoral digital sensor boasts low radiation, high image quality The truth is, a digital sensor’s image quality is an essential aspect of its diagnostic capabilities. A sensor that captures high-quality digital X-rays makes it a lot easier to detect small, difficult-to-discern cavities than a sensor that captures low-quality images. But line pairs per millimeter is an inadequate measure of a sensor’s imaging capabilities. It just doesn’t tell the whole story. And for dentists looking to purchase a new digital intraoral sensor, line pairs per millimeter can actually draw attention away from the other important specs and measures that will provide them with a more complete sense of a sensor’s ability to capture diagnostic images. According to a recent survey of dentists and dental radiologists, contrast resolution is the most desired characteristic for a new sensor-not line pairs per millimeter. Contrast resolution is a measure of the subtle gradations of gray levels in an image; LP/mm is a measure of the fine detail that can be distinguished in an image. Contrast resolution is important for caries detection, spotting subtle changes in the density of enamel, etc., and LP/mm is important for being able to see small items on a radiograph. Simply put, contrast resolution is a greater measure of a sensor’s diagnostic capabilities. Most diagnostic tasks in dentistry require contrast perception and detectability, not necessarily the detection of fine detail.
Review Suni products, view videos or request a quote
Another thing to consider is how efficiently a digital sensor captures its X-rays. All sensors require a radiation dose to capture an image, but quite often sensors with high LP/mm counts require a much larger dose of radiation. This is a problem for patients and practitioners: for patients because unnecessary radiation exposure can pose health risks, and for practitioners because images that have higher LP/mm counts and require higher radiation doses can often, after image processing and filter applications, come out “noisy” or grainy. Because of the ALARA principle (As Low As Reasonably Achievable), doctors should aim to capture diagnostic-quality X-rays using the minimal amount of radiation.
RELATED: How to determine the ROI of digital radiography equipment
That is why optimal exposure is another important measure of a sensor’s diagnostic capabilities. Optimal exposure is the lowest radiation exposure at which the maximal LP/mm and contrast resolution are achieved. The lower the optimal exposure level, the more efficiently a sensor captures diagnostic-quality images. Suni Medical Imaging’s SuniRay2 digital intraoral sensor, for instance, was recently shown in a University of Texas Health Center study to have the lowest optimal exposure levels among 20 digital intraoral sensor brands. Ultimately, the truest measure of a sensor’s image quality is always going to be your own eyes. If a sensor facilitates accurate diagnosis, whether it boasts 20 LP/mm or 10 makes little difference to the user. What you can usually be sure of, however, is there is more to consider when comparing sensors than the mere number of line pairs sensor manufacturers love to talk about. It’s easy to market a number. What is not so easy is to convey, comprehensively yet concisely, the full measure of a sensor’s diagnostic capabilities.
Spec Check
by Dr. John Flucke
- Bring each system in for an in-office demo. Digital radiography sales reps are mobile and can bring sensors and a laptop to you. If you're already computerized, have them connect their laptop to one of your treatment area monitors and take some images of the doctor and the staff. Then you can see how the images will appear on your monitor using your x-ray heads.
- Have each clinical staff member take turns placing the sensor in a patient's mouth as well as switching places and being the patient. This allows everyone to see how easy or difficult the sensor is to place while also being able to determine the way the sensor will feel to a patient. Also, this will help them explain to patients about the sensor after you make the jump to digital.
- Expect some minor hiccups. Any time you try something new there will be one or two unforeseen problems that present themselves. The learning curve for digital sensors is extremely short, but anticipating minor problems helps you and your staff deal with them in a more positive, productive manner. Remember, the benefits of digital radiography far outweigh any minor problems that may present themselves as you familiarize yourself with the new systems.
- Consult with your staff to get their opinions on which systems they prefer and why. Also have an "all hands" staff meeting to discuss the plan to move to digital, as well as to identify any potential problems that you or the staff foresee during implementation.
- If you're still using film, making the transition to digital can seem intimidating. But with the proper planning in place for the transition, things can go quite smoothly. Your sales representative can provide an incredible amount of knowledge about the dos and don'ts of going digital. I can assure you that the shopping, planning, training and integration is all worth it! Digital radiography offers immense benefits for patients and the dental team. I know you will find the technology to be all you expected and much, much more.
Featured Products
DEXIS® Platinum

The award-winning DEXIS Platinum’s physical attributes lead to patient comfort, remarkable image quality with lowered radiation and overall efficient use. Plus, the TrueComfort™ design of DEXIS Platinum offers beveled corners and a smoothly rounded casing that allows the clinician to more efficiently move the sensor about the mouth, even in tough areas like the upper molars and lower premolars. Also, the sensor offers greater image quality and consistency across both high and low radiation dose, while post-capture images can be displayed at ultra-large sizes.
DEXIS
888-883-3947 |
dexis.com
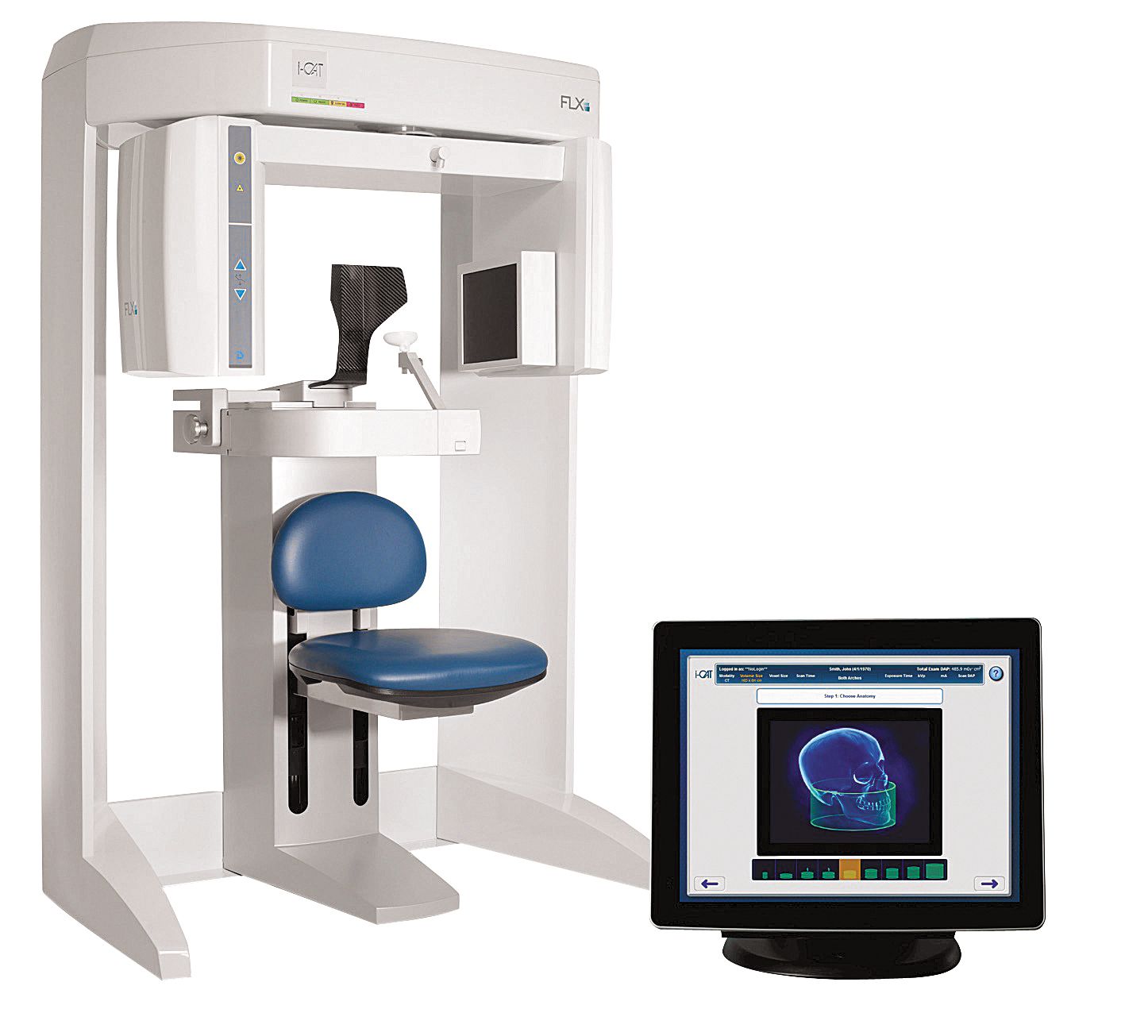
i-CAT 3D imaging solutions are said to help clinicians quickly diagnose complex problems with less radiation and develop treatment plans more easily and accurately. It features 3D planning and treatment tools for implants and restorations, oral and maxillofacial surgery, orthodontics, and TMD and airway disorders. Other features include Visual iQuity™ that provides clear 2D and 3D images; QuickScan+ technology that offers a lower dose when high resolution is not needed, at a dose comparable to 2D pan; TxSTUDIO™ treatment tools for implant and restoration planning, surgical guides and other CAD/CAM applications; as well as an easy-to-use SmartScan STUDIO™ touchscreen that allows for selection of the appropriate scan for each patient.
i-CAT
800-205-3570 |
i-cat.com
The ProMax 3D imaging unit features a broad range of imaging views that make it well-suited for diagnosis, planning and treatments including oral surgery, orthodontics and implants. Its three imaging planes make it easier to locate and trace the mandibular nerve canal, providing the dentist with more confidence when planning dental implants.
Planmeca
630-529-2300 |
planmeca.com
What's your imaging IQ?
1.
All digital sensors are created equal.
The only real difference is price and the customer service a company offers.
False.
The image a sensor produces is an important factor in deciding which sensor to purchase. And while the major brands’ sensors are coming very close to one another in terms of image quality, there is still a slew of other factors to consider, such as warranty details and compatibility with your practice’s existing technologies, or the technological knowledge of your dental team. 2.
Cone beam technology is far too advanced for a general dentist.
False.
On the contrary, cone beam systems are a valuable asset to general dentists in all disciplines: teeth crowding and eruption for orthodontics; canals, morphology, underobturated canals and fractured roots in endodontics; periodontal defects for possible grafting, in addition to nerve location for impacted extractions or implant placements. 3.
If I invest in a specific pan/ceph technology, I’m locked into that equipment for the next 10 years.
False.
New technology doesn’t automatically render obsolete that which you currently use. Like all expensive equipment, practitioners must define what they want it to do and how it will provide what they need. 4.
Digital photography offers significant value to general practice beyond showing professional-looking before and after photos of a successful esthetic transformation.
True.
Merely showing patients a transformation is just the tip of the iceberg with respect to digital photography. Other uses like “co-diganosis” often offer the shortest path to gaining treatment acceptance, making your digital camera an indispensable tool that’s no less important than your digital X-ray system. 5.
To be a digital dentist, you need to hire a server specialist.
True.
The advice and support of professionals is required when properly running any business that depends on computers. Doing it improperly wastes more money every month than the cost of the computers themselves, while properly maintained and smoothly running systems provide a solid ROI and give your practice a cutting-edge image. 6.
You must tell your patients how much radiation they’re being exposed to in a given procedure.
False.
Changing “must” to “should” would make this true. Informing before performing is a must for all treatments, not excepting the digital X-ray process. It’s not required, but a reassurance of low radiation in comparison to traditional dental X-rays helps with treatment acceptance, as many patients may have concerns they are afraid to voice. 7.
I have too many film hard files to go digital.
False.
While not a decision to be made lightly, moving from analog to digital shouldn’t depend on the number of hard films you currently have. Solid technologies like the VIDAR Film Digitizer exist that allow you to easily convert hard copy films to digital in just seconds. Simply put, a small investment lets your old information move into the future along with the rest of your practice. 8.
Once I take a scan, I can just attach it to an email and send it to an insurance provider or specialist.
False
. It is almost that easy, but not quite. Sharing in this manner requires attachment capabilities offered by services like NEA FastAttach.