Fundamentally, our clinical goal for restoring a dental implant is to make the restoration appear, feel, and function as if the tooth had never been removed. The final esthetic outcome can be influenced by a variety of factors to include implant size for the anatomical site, position of the implant platform vis-a-vis the bone crest, buccal-lingual implant position, and soft tissue thickness.
Some of these variables are not easy to control or require some level of compromise (eg, selecting an implant that fits the available bone). One other important contributor to the implant’s esthetic and functional outcome is the emergence profile created in the soft tissue and how the clinician and dental laboratory partner manage it.
Gingival Cuff Links™
• Fully customizable healing cuffs
• Maintains and sculpts gingival soft tissue
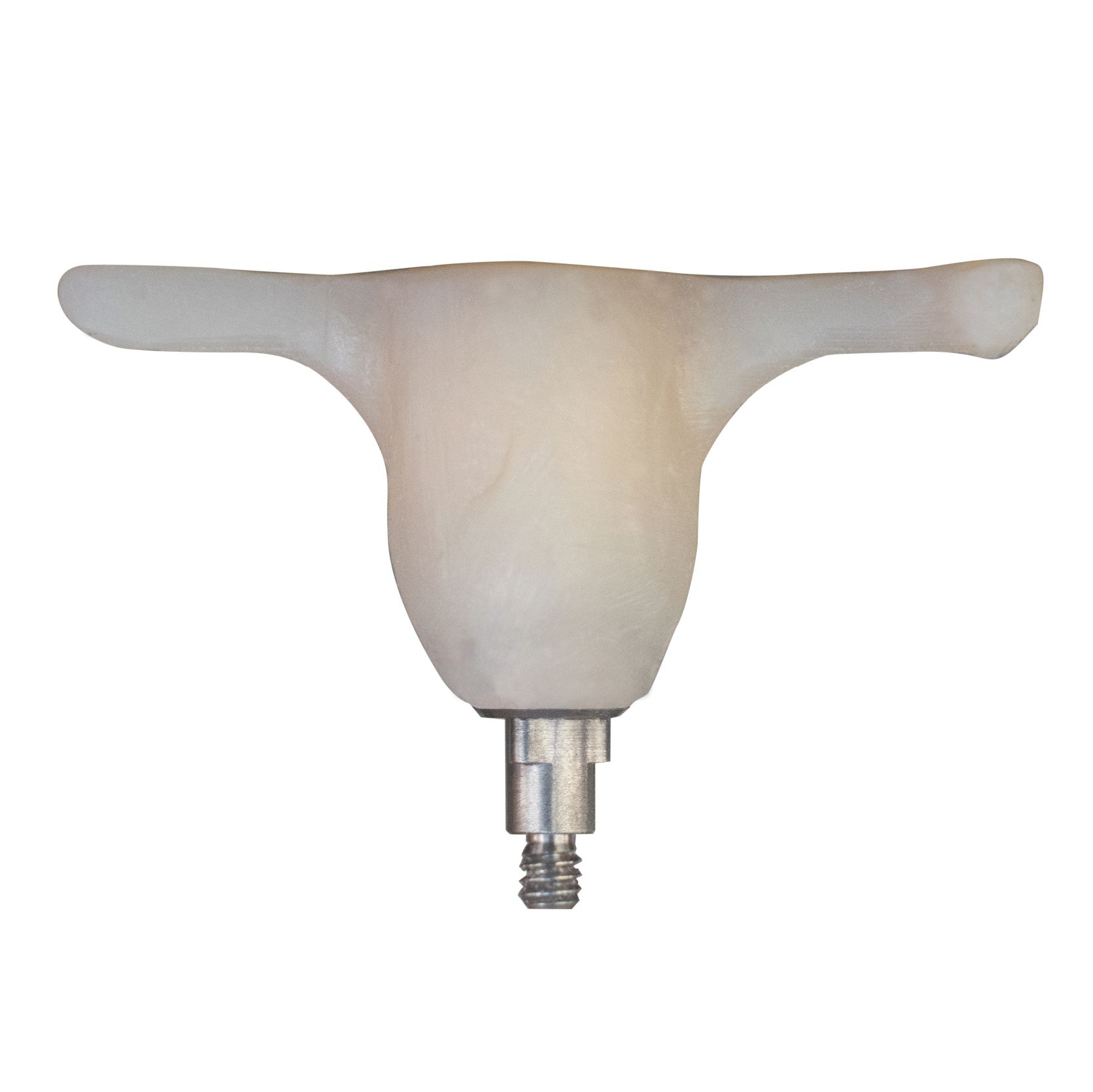
• T-handle design assists doctors in aligning the implant in the correct position
• Compatible with most implant systems
GCL Systems
833-425-4346 | gclsystems.com
Dental implant manufacturers offer metallic healing abutments fabricated from titanium/titanium alloy (Figure 1 shows a sample titanium healing abutment in vivo.) Some of these systems provide multiple flare angles to create some options for emergence. However, these abutments all have a circular profile that does not match the three-dimensional morphology of the natural tooth being replaced.
A mismatch can put the laboratory technician in a tough position—generate a restoration with a natural emergence that might not fit the soft tissue envelope, or match the soft tissue profile created by the healing abutment resulting in an unnatural emergence profile.
In many cases where a small healing abutment was used for a larger tooth site, this can result in the infamous popsicle on a stick restoration. (A crown with an exaggerated emergence is illustrated in Figure 2.) Every patient who has received this type of restoration will complain of food impaction all the time. By creating the proper emergence profile, the doctor can avoid these problems patients suffer with daily.
Start with the Proper Anatomy
Logically, it would make the most sense to create healing abutments that are site-specific and produce the ideal emergence profile for the anatomical tooth location. Given the variables described above, we want to maintain some flexibility to make minor modifications as necessary. An anatomical solution also must be positioned correctly, so the solution must engage the antirotational interface of the respective implant system.
Related reading: How To Create the perfect emergence profile for dental implant restorations
The Hybrid Solution
The Gingival Cuff Links™ product solution from GCL Systems starts with a titanium alloy core to provide an exacting and antirotational connection to the dental implant. Using a patented approach, bis-acryl material is over-molded around the titanium core using silicone molds that mimic the morphology of natural teeth as taken from the literature (Figure 3 shows a sample of a GCL Healing Cuff.)
There are a total of 11 different configurations to ensure the gamut of tooth morphologies are sufficiently covered. Bis-acryl is flexible, allowing for subtractive modification with burs or augmentation and/or shade change with flowable composite materials that bond to the native abutment.
The GCL Healing Cuff can even be converted into a provisional abutment through this additive technique or with the incorporation of a crown shell. A “T” handle incorporated into the design not only assists in handling the GCL Healing Cuff during modification, but it also allows the clinician to ensure proper placement as the “T” handle is always placed perpendicular to the facial position allowing for the correct rotational placement of the implant. The “T” handle is removed prior to final placement of the GCL Healing Cuff.
The Outcome
Using the GCL Healing Cuffs, the ideal emergence profile is created in the soft tissue at the onset (Figure 4). Note the soft tissue healing. There is no guesswork for the laboratory technician on how to emerge the restoration from the implant platform; they can simply mimic the soft tissue envelope created by the GCL Healing Cuff. (Figure 5 shows the final crown in place.)
The seal between GCL Healing Cuffs and the gingival margin is designed to eliminate the loss of particulate bone graft and minimizes pain for the patient.
Given the nice adaptation of the gingival tissue to the GCL Healing Cuff in these types of procedures, there is oftenno loss of the particulate bone graft and bone volume is maintained. An implant level impression can then be taken allowing the dental laboratory to fabricate a final crown with a matched emergence profile to what was created with the GCL Healing Cuff.
While there are other techniques that can be employed to create a custom healing abutment (eg, modification of a titanium or PEEK temporary abutment, lab-milled custom healing abutment), the GCL Healing Cuff is an off-the-shelf, user-friendly solution that is predicated on the morphology of the natural teeth being replaced with implant therapy. ●