5 phrases hygienists need to stop saying to patients
Is sugarcoating decaying your clinical practice?
It happens to the best of us: As we become comfortable in our clinical practice, we forget the ways in which our verbiage can dramatically alter the way our patients understand our recommendations.

When I was in grade school, we used to play the Telephone Game on days when our music teacher didn’t have a voice and instead chose to play games during class. She would whisper a saying into someone’s ear, and we would patiently watch as the message got passed between us. Finally, the last person in the back of the class would shout out what they “heard,” and we would giggle at recognizing that a message that started as “Don’t forget to tie your shoes today” turned into “The cafeteria is handing out espresso shots and kittens all week long."
It makes me wonder: Perhaps it isn't how we are saying it but rather what we are saying to our patients that causes important message to become lost. Moreover, are our words being misinterpreted by our patients because we're being too nice?
More from the author: A day in the life of a dental hygienist
Are you sugarcoating your verbiage and, in turn, encouraging patients to take their dental needs with a grain of salt? Here are some common phrases you may want to avoid using in the future.
Click through the slides to read more.

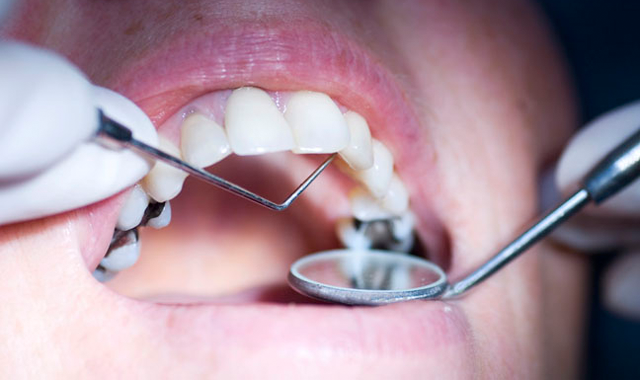
1. “…a little bit…”
During my time as a dental hygiene faculty member, I was required to listen to my students deliver treatment plans to their patients based on their level of disease. My students spent the better part of their dental appointments educating their patients on the presence of disease, the pathogenicity of bacteria, the risk of losing teeth or function and the like.
Despite the incredible education they were providing to their patients, the term “a little bit” slipped its way into their vocabulary right about the time when they felt uncomfortable or nervous in explaining the presence or severity of a disease process. The verbiage “a little bit” or “some” provides an excellent opportunity to diminish the severity of a disease process.
Let’s try this in a sentence: “You have a little bit of bone loss” or “You have some bleeding.”
Related reading: The secret to great customer service
Afterward we start telling our patients about how important it is to improve their oral hygiene or begin discussing the presence of periodontitis, a chronic and irreversible disease process that we know is directly linked to upper respiratory tract infections, stroke, heart disease and various types of cancers, to name a few.
For your consideration: Is it possible that using verbiage such as “a little bit” is giving patients the wrong message about their disease process?
Let’s try this with other chronic diseases: “You have a little bit of cancer,” “You have some heart disease” or perhaps “There’s a little bit of cirrhosis of your liver.”
Sounds weird, right?
The reality is that the medical community has sophisticated verbiage that indicates activity and severity of disease without using such basic terminology. In conjunction with this, the American Academy of Periodontology has developed far more inflammatory (see what I did there) verbiage that better aligns with the medical community. Previous case types ranging from mild to severe are now classified as stages.
Let’s try this in a sentence: “Mrs. Jones, you have Stage I periodontal disease.”
Now that has a different ring to it, doesn’t it? It advises Mrs. Jones that she has bleeding 4 mm pockets that, without careful implementation, could easily advance to further stages of periodontitis.



2. “Dr. Smith is going to stop in for a check…”
This is a STANDARD in most dental practices. We become so comfortable with our patients, we’re casual within our operatories and we establish such friendly relationships with our doctors that we effortlessly diminish the value of the periodic oral evaluations our doctors are performing.
Trending article: The top 10 things that scare your patients the most
Let’s consider the work our doctors are doing while performing a periodic oral evaluation. First and foremost, they’re usually leaving their crown prep, fillings, extraction or endo patient due to the “hurry up” stare down from us. As they walk down the hallway, they’re reframing their minds while we blurt out information like “He still doesn’t want to do that crown” or “She refused X-rays today.” Our doctor walks into the operatory, half slathering on hand sanitizer, half trying to casually draw up a conversation with the patient. After having a handful of seconds to scroll through radiographs, intraoral photos and periodontal charting, the doctor has to become completely versed in the patient’s history while performing a caries examination, verifying our periodontal findings, completing an oral cancer screening, evaluating occlusion, and screening for sleep disorders, parafunctional occlusion and opportunities for treatment.
Most hygienists have established such a strong working relationship with their doctors that the periodic examination has evolved into a meeting in front of the patient in which the doctor is verifying and supporting the findings of the hygienist. Nevertheless, the doctor is responsible for all assessments, diagnosis and treatment of patients entrusted to their care, and verbiage such as “The doctor will pop in for an exam” or “Let’s see if we can get Dr. Smith to stop by” easily diminishes the value of the doctor’s examination.
If we’re already diminishing the value of the examination prior to the doctor walking into the operatory, how well will patients listen, understand and act on the findings during the examination?


3. "Let's keep an eye on this..."
I've said it before: Watching the advancement of a disease process has become a spectator sport in dentistry.
While our noble efforts may mean we're informing our patient of an area of concern before it becomes a greater problem, our patients certainly can interpret this in a different way.
Watching a disease process tells the patient two things: 1. There's something going on and 2. It's not that big of a deal because if it were, we'd be doing something about it right now.
I completely respect that depending on the clientele, dental needs and access to care considerations, the "healthy patient" model is truly a spectrum across dental practices. While I may be using the diode laser and recommending CloSYS for a handful of bleeding 4 mm pockets in my North Scottdale spa-like office, I'm lucky if I'm allotted enough time to thoroughly gross debride and slather on some fluoride varnish for my Medicare/Medicaid patients in a busy Central Phoenix office. Despite this, I do believe we have an opportunity - no, a responsibility - to provide our patients with the minimum standard of care based on their unique needs.
More from the author: Are you suffering from burnout?
I love to tell my fellow RDHs that THIS is our moment to shine! As preventive specialists, this is the moment when you make your recommendation. "Watching" an incipient carious lesion? Get some remineralization going. "Watching" an early sign of gingival disease? Beef up the oral hygiene instructions, put your patients on a medicated rinse, fire up the laser or shorten that recall interval.
Dental professionals have evolved from the word "watch" and are now calling the same act "actively monitoring." Semantics aside, it's important for dental professionals to understand the imeprative role they play in the prevention and therapeutic intervention of chronic disease.


4. "You're due for a hygiene visit..."
Picture this: A day within your schedule where you ONLY scale and polish teeth. You don't collect vitals, you don't perform a medical and dental history interview, no radiographs, no periodontal charting, no adjunctive services, you don't conversate over oral hygiene instruction, nutrition or tobacco cessation, no head and neck examinations, no oral cancer screenings, no collection of a chief complaint, no evaluation of the airway, no risk assessment evaluation, no "goodie bags" - just scaling and polishing.
First, this would make for an incredibly boring day.
Second, we know that we wouldn't be providing our patients with anywhere near the standard of care if that was the only therapy we were providing.
Are you devaluing your own appointment by calling it a "hygiene" visit? Are you making it easier for patients to understand that your visits are "just a cleaning"? Are you, in turn, making it more challenging to be able to present adjunctive services during your appointment?
Trending research: Study finds more than 60 percent of people suffer from dental fear
Here's my theory: For 11 years, I drove the same Chevy SUV that I bought the day before my graduation from undergrad. Like clockwork, I would bring in my car for its oil change and would of course expect the conversation surrounding adding additional services such as the air filter or transmission flush of whatever. I was annoyed and consistenly felt like services were just being added on to fill their production quota for the day.
In contrast, I finally hit a major professional goal this year and bought myself a BMW. I take "fast car" (that's what I named her) for maintenance visits where the BMW dealership does a complete assessment of my car, tops off all fluids, fills my tires with air, checks alignment and, of course, completes an oil change while I enjoy premium coffee and Wi-Fi.
There's truly no difference between the two experiences except that I value fast car's maintenance visits because I'm prepared for what they are - visits to ensure she keeps running smoothly.
Many offices are gaining success with integrating verbiage such as "dental maintenance visit" or "preventive visit," as these terms better outline the objective for the visit, which is to completely evaluate, diagnose, treat and reevaluate your patient's oral conditions.



5. "Cleaning"
I'm raising my hand: guilty.
I was working in private practice the other day when my friend, colleague and source of inspiration, Sarah Cottingham, asked me an interesting question. She had listened to my case presentation of a patient who needed scaling and root planing. With a smile, she asked me, "Why do you call SRP a cleaning?"
Now it doesn't happen often, but every once in a while I'm truly speechless. Sarah tends to pull the best out of me, and she knew I was processing this.
Related article: Hygiene instrumentation shortcuts: are they wise?
I had spent the better part of 11 years of my career explaning the chronic nature of periodontal disease. A true microbiology nerd, I would discuss the gram-negative anaerobic bacteria living at the base of the pocket. I'd talk about how they release enzymes like hyaluronidase to help attack the body. I enjoyed the wildly overdramatic ways in which I could describe the sequelae of disease if untreated. I would delicately discuss the link to oral-systemic diseases and share my concern for my patients' well-being. I would remind my patients that our collective goal is to save their teeth and keep their smile healthy for a lifetime. Like a perfectly rehearsed Oscar acceptance speech, I would eloquently bring my patients to understand the irreversible nature of periodontitis and the severity of this disease. Then, like clockwork, I would say, "So let's do that cleaning!"
Now perhaps my patients didn't think much of it. Maybe they were so overwhelmed with words like "P. Gingivalis" and "crestal lamina dura" to even know what was happening. And perhaps, despite everything, my patients simply understood my concern for their well-being. But the fact remains: I literally referred to active periodontal therapy to arrest and stabilize an irreversible disease as a "cleaning."
I perform a cleaning on my house when I want to tidy up for guests. I clean my dogs when they're stinky and need a bath. I clean my car so that I'm not driving around in a pig sty. But cleaning my house doesn't prevent chronic inflammation, giving my dogs a bath doesn't reduce bleeding, and cleaning my car doesn't address a disease linked to diabetes, heart disease, stroke and cancer. Even the ADA's CDT codes discuss the removal or debridement or root planing of calculus and plaque but nowhere do they mention "cleaning." So why then do we relate our therapeutic services to a cleaning?
My challenge to you is to try going one week without using the word "cleaning." Don't "clean" your prophy patients; instead, provide a preventive hygiene service. Don't "clean" your periodontal maintenance patients; rather, provide a therapeutic maintenance service. Don't "clean" your "deep cleaning" patients; instead, provide active therapy to address the bacterial load located below the gum line. Heck, don't even "clean your operatory; sanitize it. Challenge accepted!



Conclusion
While we always aim to be sweet to our patients, our sugarcoating can devalue and, in turn, decay our practices.
More from the author: The medical history mistake every dental provider makes
Hopefully I’ve provided you with “a little bit” of information on how to improve your verbiage. I encourage you to print out this article and be sure that you “stop in for a check” to make sure you’re “keeping an eye” on your verbiage. Remember: your “hygiene visits” are more than just a “cleaning,” your skills are valuable, and you have an immense ability to improve lives with your knowledge.
So WHEN you seat your next patient, consider HOW you'll adopt this revised verbiage so that WHAT you say doesn't decay.
