5 fascinating questions hygienists asked Kara RDH in June
Kara Vavrosky shares five more interesting questions she's been asked by hygienists recently, along with her answers.
As a well-known and accomplished dental hygienist, Kara Vavrosky often gets asked for advice.

She runs the popular Facebook page Dental Hygiene with Kara RDH and is also the founder of dentalhygieneanswers.com, a question-and-answer platform for dental hygienists.
Here, Vavrosky shares five more interesting questions she's been asked recently, along with her answers.
Continue to the next page to view our slideshow of these questions and answers.


Are you a quiet hygienist or a talkative one?
I'm just curious if you have non-dental related conversations during the appointment. I usually do most the talking before/after scaling unless it's related to homecare, but keep pretty quiet during the actual appointment. I even had one patient tell me "thank you for not talking when you're in my mouth, I really appreciated it." Is it normal to be a quiet hygienist?
Overall I am a quiet hygienist. Just like you, I have had people tell me they appreciate not being "talked at." I've also had patients say they appreciate being seen on time and being dismissed on time because the appointment's focus was on their oral health instead of with talk about the weather (patient's words paraphrased, not mine!). I tend to catch up with my patient's lives before medical history. Then throughout the appointment, when I'm out of their mouth switching instruments or something, I will continue the conversation from before medical history. It's a fine balance. You really have to feel the patients out to see what they are comfortable with and get cues from them. The conversation adjusts accordingly.



Receptionist trouble
Recently my employer has been out on medical leave. Over the past few weeks the receptionist has been late returning from lunch twice by one to two hours, and on three other occasions she has come to work "impaired" to the point she can barely do her job. Yesterday she called in sick after lunch and left me in the lurch alone with patients. She said she is on a new medication. My boss doesn't know what to do. I am not comfortable working alone in the office.
I don't blame you for feeling uncomfortable as this is a valid concern! Whether your boss is out on leave or not, this is a serious situation that he or she needs to deal with immediately. It's also a liability, especially if you are being left alone. Your boss really needs to step up and be the boss. "Not knowing what to do" is not an excuse here. If your boss knows what is going on and the receptionist happens to get in a car accident on the way home from work or has an accident at work-even though "impaired," the liability may fall on your employer. I actually called OSHA (anonymously) about this because per OSHA, "Every organization must provide a safe working environment for its employees and follow all applicable laws and regulations governing workplace safety and health." They told me you should call and speak with an OSHA enforcement officer, which you can do anonymously. You should feel safe at work at all times and your boss should provide a safe work environment at all times.


ADVERTISEMENT
Sponsored content: How MI Paste Plus reverses and prevents white spots



Periodontal concerns and pregnancy
I had a 30-year-old patient who hadn't had her teeth cleaned in a year and a half. Prior to that cleaning, it had been about five or six years. She was in my office a few weeks back for pain in her upper left quad. My doctor probed the area and 4mm pockets were present on DB of #14 and MB of #15. Today when probing that area in those exact same locations there were 6mm pockets. Between teeth 30-31 there were 5mm pockets present. She is also 31 weeks pregnant. I did not perform a cleaning and referred her to a periodontist for an evaluation due to risk of bacteria entering blood stream during pregnancy. Did I do the right thing? What would you have done in this situation?
First, I would have gotten a release from her OB/GYN specifically asking if the patient and baby is healthy enough for non-surgical periodontal therapy/SRP's (or even localized SRPs) and which anesthetic is recommended (2% Lido w/epi or 3% mepivicaine is generally okay). Then I would have proceeded. Here's why: more and more studies are showing a positive correlation between untreated moderate-severe periodontal disease and preterm and low birth weight babies. More studies need to be done to establish association however.
If she follows through with the periodontist referral all is great. But if she doesn't, I'd hate to see her swallowing bacterial endotoxins every day, them entering her blood stream, then crossing the placenta barrier to baby. Arguably, this constant exposure to endotoxins would be worse than the exposure during scaling. I think the benefits would outweigh the risks.
It's also worth mentioning, she could also have pregnancy gingivitis and have inflammation due to hormones. Was there bone loss? Recession? Bleeding? Subgingival calculus? It's definitely worth assessing more than just probe depths to get a comprehensive picture of the patient's condition.
That's just what I would do. It's not that you did anything wrong, just a different way of looking at it!


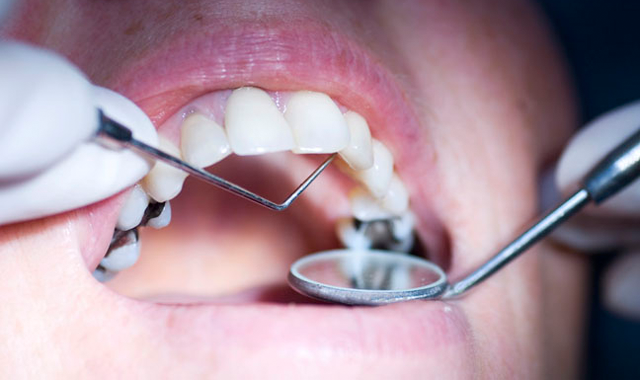
New hygienist probes and finds deeper pockets than other RDH. SRP?
A patient has been coming in for years for his six-month recall prophy. His probe readings have been 1-3mm with localized BOP. You come in as a new hygienist and do a full mouth probe and your readings are different. You are probing 1-3mm with localized 4-5mm BOP. Do you recommend SRP in those localized areas? From an insurance standpoint, can you go from a prophy to localized SRP? Or would you have to do a debridement first?
I would recommend localized non-surgical periodontal therapy/SRP in those areas if there is active bone loss on his radiographs or any clinical attachment loss change. You treat what you are presented with at the time because it's a fine line of if the hygienist wasn't as thorough with scaling or probing or if it truly is a lapse in homecare on the patient's part. It could even be a change in the patient's health history increasing risk factors for perio.
If there's no clinical attachment loss (including active bone loss) and leaning toward gingivitis, non-surgical periodontal therapy isn't warranted. Instead, you would want to educate heavily on home care, demonstrating proper brushing and flossing technique (or proxy brushes or water flosser – whatever is best for the particular patient). I would link the need for homecare to the periodontal disease process, to really make the patient understand how homecare (if that's the issue) makes a difference. Then at the next appointment, reassess the patient's periodontal condition and go from there.
You don't have to do a debridement before non-surgical periodontal therapy. A debridement is for a patient that has too much plaque/calculus/material alba that the doctor cannot do a proper exam. It is scaling above the gumline. Debridements get tricky because to a patient, it "looks" like their teeth are clean, but subgingivally (where it really matters) they are not. I only do debridements when absolutely necessary because if the tissue closes up around any calculus it can cause a perio abscess. Whether you need to do a debridement is based on need and clinical judgement.



Patients who wince during cleaning
I have been a hygienist about five years now and am generally confident in my skills. Once in a while I will have patients who wince in a few areas while I'm cleaning them and I always worry it's something I'm doing wrong with the instrumentation, rather than their own gingivitis or something. If I know their mouth is full of gingivitis its one thing; but when it doesn't seem bad I worry it's something I'm doing wrong, though generally I don't have an issue when cleaning patients. Am I doing something wrong? How do I stop worrying about it?
If you generally don't have an issue with people wincing and it only happens once in a while, I doubt it's something you are doing wrong. I say this because some people are more reactionary than others and wince even if it doesn't "hurt" per se, but they wince simply because they "felt" something. When people do this I like to ask them what they are feeling. There's a differentiation between feeling pressure, to tenderness from infection, to sensitivity due to recession (even the smallest amount of recession can cause sensitivity).
Depending on what they feel, it may not be you at all, but infection, recession, etc. Don't be afraid to grab a probe to check for infection if a patient winces when you are treating an area. You can also use an intraoral camera or have a patient use a hand mirror and you can show them recession (or whatever the reason for the discomfort) to ensure not only yourself, but the patient why they feel what they feel.
If nothing obvious is causing their discomfort, and you are using the ultrasonic, you may need to turn it down a touch or use more water. I have found that patients who brux (clinchers and grinders) tend to be more sensitive to the ultrasonic, this includes myself. If the patient says pressure (from instrumentation) is causing discomfort, double check the pressure you are using with your working strokes, it may be caused by poor fulcruming. However, the biggie here is to make sure your instruments are sharp. Dull instruments make you work harder (and can cause injury to you) and the pressure you must use to remove deposits effectively (without burnishing) can be uncomfortable to a patient.
Like I mentioned above, I don't think you are necessarily doing something wrong. I think finding the cause of the discomfort will give you some answers and help with the worrying. Above all, be confident in your skills. Questioning your ability and pushing to be the best clinician you can be is awesome-but don't let it stress you out or cause worry; look at it as challenge. Scalers up!

Resources
Teo, B.K., Lim, L.P., Paquette, D.W., Williams, R.C. (2005). Periodontal Disease – The Emergence of a Risk for Systemic Conditions: Pre-term Low Birth Weight. Annals Academy of Medicine, 34(1), 111-116. Retrieved from http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.494.4019&rep=rep1&type=pdf
