3 major challenges when creating dentures
From choosing the right materials to ensuring proper fit, there are any number of factors that can go wrong.
Many challenges exist when creating dentures. From taking proper impressions to choosing the right materials to fabrication issues to fit, there are any number of places where making dentures can go wrong.
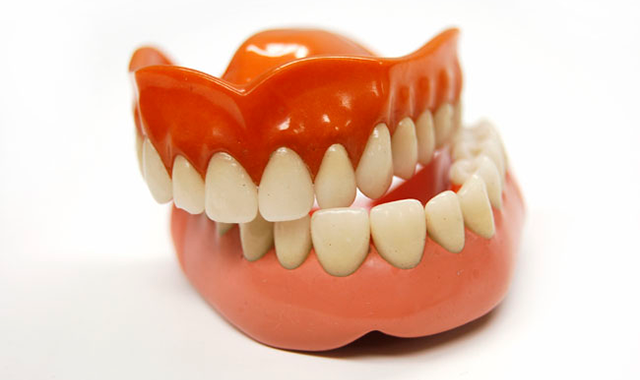
Moreover, fewer dental technicians are going into conventional denture fabrication, and the experienced denturists are beginning to head into retirement. Soon, it could be that the most significant challenge when creating dentures is finding someone to create the dentures.
Trending article: The biggest evolution in dentures is almost here
We talked to four denture experts to discuss the three most significant problems you could encounter when fabricating dentures. What they had to say might surprise you!
Click through the slides to read more.

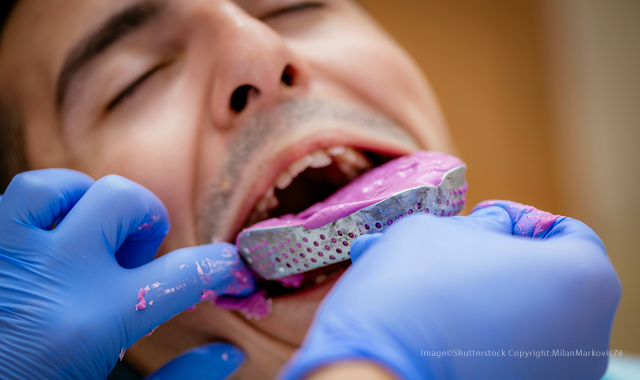
Challenge #1: Not getting a proper impression
All of our experts agree that having an adequate impression is the most significant challenge for creating dentures. When the impression isn’t accurate, it can result in dentures that don’t fit or function well for the patient.
Dan Elfring, CDT, an in-house lab technician for Pickle Prosthodontics, says it’s understandable why impressions can be a challenge. However, he also believes that getting proper training and having the right attitude will make a significant difference in the quality of the impressions a clinician takes.
“If a provider cares, they will try to improve. If they don’t care, I don’t care what you do; they won’t improve. It’s wanting to serve the patient better and just doing your best,” Elfring says.
More from the author: 5 biggest patient complaints about dentures - and how to solve them
Elfring doesn’t work a lot with digital impressions. However, he thinks it will be easier for some dentists, particularly young doctors, to take great scans. However, he believes that experienced clinicians might continue their bad habits in digital impressions.
“If they took a poor impression before, then they probably are going to take a poor scan,” Elfring says. “If it isn’t a good impression, it isn’t going to fit.”
Dr. Paresh Patel, who’s in private practice in North Carolina, agrees that inadequate impressions result in poor fit and function in dentures. Dr. Patel says the best way to avoid these complications is to take a suitable impression for the lab to build a proper fit.
“It’s garbage in, garbage out,” Dr. Patel says. “It depends what the laboratory has to begin with. If they don’t have, for example, the retromolar pad or the buccal shelf correctly marked, then we’re already starting with a sub-acceptable impression. From there, if the laboratory doesn’t have the correct vertical dimension or the teeth are not set to help stabilize the denture and the function, then we have another set of parameters that are not met.”
Elfring thinks a contributing factor to sub-optimal impressions is how time-consuming they are to do correctly. First, the doctor would want to do a diagnostic cast in a custom tray. Then, at a second appointment, the doctor would get a border-molded impression around all of the moving tissues and attachments. Elfring says that this moving tissue impression is key to getting an accurate fit.
“When you smile and kiss, that kind of movement will dislodge a denture if it hasn’t been accommodated for those movements,” Elfring explains. “So, getting a proper, good impression is the No. 1 issue.”


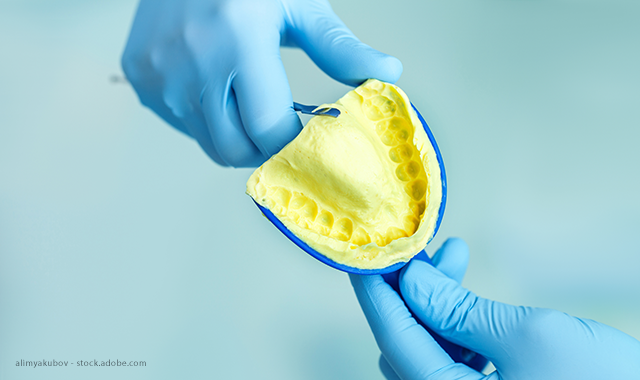
Challenge #2: Inadequate or inaccurate bite registration
From his perspective as a lab owner, Justin Marks, CDT, founder and CEO of Arfona, says the main reason he has to remake a denture or reset the teeth either in wax or digitally is the result of improper bite registration. Poor bite registration far outweighs the number of times Marks has had to remake or reset due to poor impressions.
Marks says many times dentists aren’t familiar with the standard operating procedures for taking an accurate bite registration. He says it’s better to have too much information than not enough when you’re a dental technician.
“The more measurements and records you can send initially, the less adjusting you have to do later,” he says.
Trending article: The most common OSHA violations in the dental lab
Elfring agrees, adding that often edentulous patients have forgotten where the centric position is and can’t repeat their bite, which adds to the difficulties of capturing it. However, capturing the proper bite relation is crucial to their oral health.
“If their bite is not registered accurately, then when they are biting, they can cause more harm to their temporomandibular joint,” Elfring says.
Elfring explains that recording where the lower jaw is on the hinged access and in the proper position to bite and speak is essential. It becomes a pinpoint stop, like a bullseye.
It’s difficult for a moveable jaw to hit the “biting bullseye” every time. Then, if the bite hits the side of the optimal spot, it could dislodge the denture. For these reasons, Elfring says the denture needs to be able to accommodate a bite that isn’t on target every time.
However, many dentists don’t know how to obtain that data accurately. Marc Wagenseil, CDT, DD, is a denturist in Alberta, Canada, and an international lecturer for VITA North America and VITA Zahnfabrik in Germany. He recommends understanding the individual patient’s chewing style, much like you would if you were assessing their gait.
“Some people walk heavier on one side than the other, more on the left side than the right. It depends on their bone and muscle structure,” Wagenseil explains. “Well, some people chew more left or when they talk, they swing their jaw and favor one side or another. Typically, we don’t check for those things in the treatment room.”
More from the author: Increasing FDA involvement in CAD/CAM dental restorations
Wagenseil says that we don’t chew with our natural teeth in a movement like a hinge, but rather more like a tear-drop. The dentures need to function in that movement style so that they don’t bind against each other and rock the denture when the patient chews. He suggests dentists analyze how that person’s jaw is moving for that person by watching him or her say the days of the week and the months of the year, not only in English but also his or her mother language, if applicable. This will identify jaw movement, posturing and how the denture teeth function within.
Marks says the inadequacies in bite registration go hand-in-hand with the fact that removable prosthodontics aren’t addressed in dental school as much as they once were. Dentures and removable prosthodontics have taken a back seat to some of the more exciting things, like implantology.
“They have more things to teach these days,” Marks says. “They have the same amount of time in dental school but more things that have to be taught.”


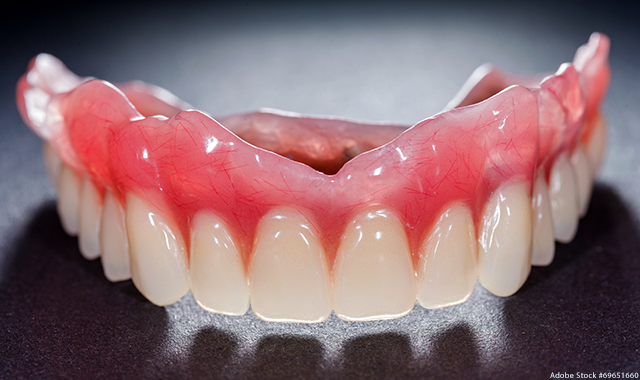
Challenge #3: Remembering that patients are individuals with unique needs and challenges
When you look at dentistry in general, a patient comes in with a problem with a tooth. Dentists then come up with a treatment plan that fixes that problem, precisely for that patient in his or her mouth.
However, when a patient needs a denture or walks in with a denture already, Wagenseil says dentists take more of a process approach rather than an individualized treatment plan. There’s not much customization to it.
“If you have a specific problem with a natural tooth, the treatment is customized to you. We seem to have forgotten that as it pertains to dentures,” Wagenseil says.
Related reading: What you need to know about the evolution of dentures
Wagenseil recommends dentists consider the patient more in the process. The denture will integrate into the human body, fitting inside their mouth. Dentists should consider not only the patient’s gum structure and gum shape but also their overall health. Details like their age, medication and even their skin condition can make a difference in the denture design.
“Does the patient bruise easily? A denture sits inside the body. It compresses the tissue and as such creates hydraulics,” Wagenseil says. “So, if I think the patient bruises easily and thus has a sensitivity to hydraulic pressure, it is reasonable they should have a hydraulically sensitive denture in the mouth. That helps me build the denture more specifically to the patient.
“One of the challenges is for us to remember that you are treating an individual,” Wagenseil adds. “You have to look at the individual and make decisions as to what do you think they can accept and tolerate in their mouth at that snapshot of time when they are in your office. You have to look at whom you are doing it for and not just do things because the textbook told you to do it. You have to look at the individual.”
Wagenseil says dentures can be very successful for people when you take some of these critical points into consideration when you design and build them for patients. Moreover, he says you can have great success as a practitioner treating patients.
“Remember that you are building a denture to a person and you have to look at the whole person holistically,” Wagenseil says.
Dr. Paresh adds that dentures can be challenging to systemize because people have individual ability to adapt to the appliance. Just going by the book won’t make them happy.
Read more: How digital dentistry and 3D printing are changing dentures
“We were taught a myth that if you followed the biostatic design principle - which is to give landmarks that don’t move for the denture to sit on, border mold and add correct extensions to our denture - and do a laboratory clinical remount and grinding the occlusion to where it’s balanced on both sides, you will have well-constructed dentures and people will appreciate your efforts and will skip out of the office singing your praises,” Dr. Paresh says. “That is just simply not true.”
Dr. Paresh says that it comes down to whether the individual can accept the denture. Some patients can, while others can’t.
“Consider your favorite pair of shoes. Let’s say they are Nikes. You may love them and think everybody should get this particular brand of Nike because it’s the most comfortable shoe you ever wore. Well, you might give it to 10 other people, and seven of them might say it is a completely worthless shoe,” Dr. Paresh explains. “That’s how dentures are. We just don’t know. Even if we do the best job we can do, we don’t know if it’s going to work for a patient or not.”


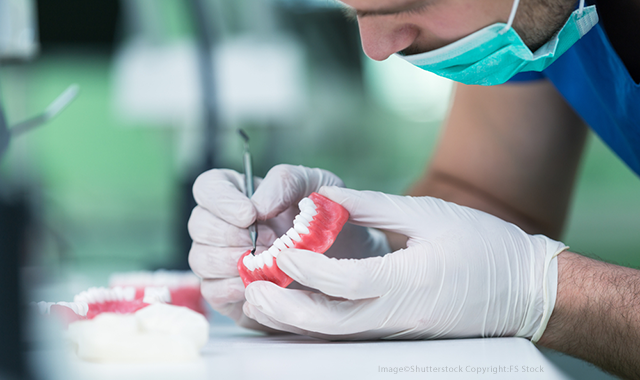
A future challenge when creating dentures: The shrinking of the denturist talent pool
One additional challenge faces the dental industry regarding dentures: the labor pool for denture technicians is running dry. Marks says laboratories face difficulty hiring denture technicians.
“The two skill sets that require the most experience and knowledge - arranging dentures and designing partial dentures - are the two areas that the dental technician talent pool is getting smaller and smaller,” Marks says.
Elfring echoes that sentiment adding that well-trained denturists are getting to be quite a commodity. Many experienced denturists are approaching retirement, and the new technicians gravitate toward digital dentistry.
“It’s much easier for them to learn digitally then all of the hands-on and conventional ways. Young technicians and doctors are picking it up easily and readily. That’s just how they learn. To design a denture digitally is much easier for them,” Elfring says.
Trending article: The 5 craziest denture tips on the internet
Marks estimates that many experienced denture technicians are retiring in the next five to 10 years. Dentistry will have to look for alternative methods of denture fabrication.
“We need to make more dentures with fewer technicians and digital can do that,” Marks says.
Marks recommends that clinicians attend continuing education courses on digital dentures. With the impending launch of digital technology for fabricating dentures and partial dentures, the continuing education opportunities are likely to rise.
“Now is a great opportunity to learn as much as possible about the new technology and dentures in general because we are going to see a lot of focus on that category,” Marks says.
