Total-etch or self-etch: which forms the best bond?
Since the invention of self-etching bonding systems in the ‘90s, the question has lingered surrounding adhesive dentistry: which is better for bonding, total-etch or self-etch?
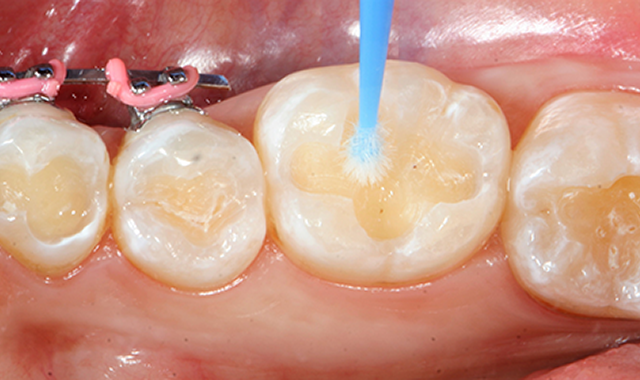
Adhesive dentistry has changed the profession. Per the Journal of the American Dental Association, it revolutionized restorative dentistry.1 The addition of bonding systems to natural teeth improved resin-based composite dentistry, creating restorations that were both predictable and durable.2 However, some debate exists about what type of system produces the best possible bond with natural teeth: total-etch (i.e., etch and rinse), or self-etching systems.
Different benefits exist for each type of bonding system, and they also have some drawbacks. Per Nathaniel Lawson DMD, Ph.D., assistant professor and director of the division of biomaterials for the UAB School of Dentistry, the advantages and disadvantages of both are the following:
- Total-etch: The benefit of total-etch is that it involves the application of phosphoric acid, with a pH well below one, to the entire preparation-both enamel and dentin. This application ensures a thorough etch pattern on the surface of the enamel and the removal of the smear layer on dentin. The disadvantage of a total-etch technique is it has more technique variability, particularly when bonding to dentin because the amount of time to etch dentin and the residual wetness of the dentin after rinsing can have a significant effect on the bond.
- Self-etch: The benefit of self-etch is it takes away some of the technique sensitivity of etching dentin with phosphoric acid. However, the disadvantage is some self-etch adhesives, which perform better for bonding to dentin than total-etch systems, are not acidic enough to create surface texture on enamel.
Since the late 1960s, dentists have known that creating an etched surface of a tooth creates tiny pores that allow the resin to adhere to the tooth. They used phosphoric acid to create these micropores in enamel to form bonds that last and don’t lead to any postoperative sensitivity.
Related reading: 3 cosmetic procedures you can complete with composite resin bonding
However, when using phosphoric acid to etch dentin, they didn’t have the same success. In fact, Michael Buonocore, DDS, the pioneer of adhesive dentistry, described the process of adhering restorative materials to dentin as “elusive."3
It wasn’t until the 1990s in the fifth generation of bonding systems that self-etching adhesive systems first entered the market. The Self-Etching Primer used a solution of 20 percent phenyl-P in 30 percent HEMA and was touted to bond to enamel and dentin at the same time.4 These early systems had some shortcomings, however, including clinical studies that proved they were less successful at bonding to enamel than the previous generations of adhesives that used a total-etch technique-and phosphoric acid on the enamel.
Now, nearly 30 years later, the question remains: which creates a better bond? The fact is, they both do. It all depends on the indication.
Jason Goodchild, DMD, director of clinical affairs for Premier Dental Products Company, subscribes to the concept of lining up the “rights”- the right material, right patient, right procedure, and right clinical situation-to choose the most appropriate bonding approach for that particular patient and procedure.

Some preps have enamel and dentin in equal amounts, while other preparations are all dentin. Some preps are so small and minimal that they’re all in enamel. Dr. Goodchild explains you should be flexible when it comes to etching teeth for a bond. In other words, whether you use a total-etch or a self-etch system depends on the size and shape of the prep.
“At the end of the day, we have to know that if we have enamel, we'd like to etch it, and when we have a lot of dentin, we’d like to be judicious with etching. So, having systems that allow for that is where we are now,” Dr. Goodchild says.
The first bonding systems were total-etch. Dentists had to apply etchant to remove the smear layer. Then, by removing the smear layer, the dentist exposed collagen and could create a hybrid layer.
“In those instances, total-etch works great,” Dr. Goodchild says.
More from the author: Break out of your restorative rut
However, as bonding systems evolved, dentists learned phosphoric acid on dentin could cause postoperative sensitivity, or matrix metalloproteinase (MMP) creation, which can degrade the bond from within. Per Dr. Goodchild, bonding systems began to use acidic monomers that didn’t require phosphoric acid to eliminate the etching step and make it easier for the dentist, also known as the self-etch bonding systems.
The next evolution of bonding systems looked for a middle ground, which is to say a bonding agent that could either have total-etch or self-etch. Dr. Goodchild explains with these types of “middle-ground” systems, you can also enjoy the benefits of etching enamel without worrying about a little getting on the dentin because it won’t cause a problem.
“We now understand that etching enamel when you can creates the best bond,” Dr. Goodchild says. “And keeping phosphoric acid off of dentin is probably a good idea. So, that's why we have to pick the right stuff for the right indication because some preparations have a nice mix of enamel and dentin."
“The ideal combinations of these two modes is selective-etch,” Dr. Lawson agrees. “In other words, employ phosphoric acid application on the enamel and self-etch application on the dentin."
Continue reading on page two...
Are we asking the wrong question?
It turns out we might be asking the wrong question pertaining to materials that perform best in adhesive dentistry. Dr. Lawson says the literature doesn’t show the type of etching mode improves a bond universally; instead , it’s how many bottles the system uses.
“A lot of dentists want to know which is better: total-etch or self-etch? If you take a look at the clinical trials that have compared these bonding modes, what you will find is that both modes can have excellent clinical performance when two-bottle systems are used,” Dr. Lawson says.
Trending article: Should you be concerned about measles?
Dr. Lawson says two of the materials with the longest standing track records are Clearfil SE Bond (Kuraray Dental), a self-etch adhesive, and OptiBond™ FL (Kerr Dental), a total-etch adhesive. Both materials are two-bottle systems. Furthermore, according to Dr. Lawson, the two systematic reviews performed by Peumans confirmed two-bottle adhesives outperform single-bottle systems.
However, Dr. Lawson says a recent exception to this rule seems to be the performance of universal adhesives, which are mildly acidic, single-bottle systems. When these adhesives are used in a total-etch or selective-etch (etching enamel only), they seem to perform on par with some two-bottle systems.
Aside from clinical longevity, the other questions surrounding the debate between total-etch and self-etch is the incidence of postoperative sensitivity. Dr. Lawson says there have been several recent reviews of clinical trials that showed no difference in postoperative sensitivity between self-etch and total-etch adhesives.
“One concession is that clinical trials often compare ideal clinical situations with shallow- to medium-sized restorations. A real-world practice-based research network study determined that there was a slightly lower incidence of postoperative sensitivity with self-etch adhesives,” Dr. Lawson says.
Selective-etch is the future-for now
Of course, dental materials manufacturers would like to introduce a bonding agent that could work for anything. Dr. Goodchild says that’s where the next generation of bonding materials is heading.
“These universal eighth-generation bonding systems allow for the etchant to be applied or no etchant to be applied. You could do it either way,” Dr. Goodchild says. “Historically, that hasn’t been the case. It's only recently that we've been able to get that product robustness."
Related reading: Why dentists should take a fresh new look at restorative innovations
Not everyone is using universal bonding systems today. Dr. Goodchild knows doctors who consider the fourth generation of bonding systems the gold standard. They etch the whole preparation, and then apply a primer and a separate adhesive.
“People still use those old-school bonding systems because they work,” Dr. Goodchild says. “However, when you get into those older bonding systems, there can be some technique sensitivity, meaning you have to know how to use them very precisely. But, when you use them precisely, they can be extremely successful."
Dr. Goodchild says the same is true with self-etch. For example, he says Clearfil SE, a significant player in the self-etch category, has a wonderful product. The doctor’s preference can come down to brand loyalty.
“You can stick with ‘what works well in my hands’ and get fantastic results. But, you need to read directions and be able to use these things correctly because bonding is one of those great examples where every single step of every single product has different directions, and there are nuances that you have to follow,” Dr. Goodchild says.
References:
1. "THE SCIENCE OF BONDING: FROM FIRST TO SIXTH GENERATION," Kugel, Gerard et al. The Journal of the American Dental Association, Volume 131, 20S - 25S. Accessed via Web. 11 June 2019. < https://jada.ada.org/action/showCitFormats?pii=S0002-8177%2814%2965275-2&doi=10.14219%2Fjada.archive.2000.0398>.
2. Ibid.
3. Ibid.
4. Ibid.