Tackling the taboo topic of mental health in dentistry
Very few people go through life without any chronic health challenges. Cancer, heart disease, chronic pain, diabetes, mental illnesses and more touch every family at some point, in some way. Physical health conditions and mental illnesses are often paired. People with cancer often have depression; people with schizophrenia often have diabetes; and people with chronic pain, including orofacial conditions like temporomandibular joint disorders (TMD), often suffer from both physical and emotional health challenges. Even more specifically, people with type 2 diabetes, for example, are doubly at risk for developing depression and vice-versa.
Many factors play a role in mental health and since May is Mental Health Month-the 70th year of the awareness month-it’s a good time to take a closer look at what dental practice leaders, doctors and teams can do to improve the overall well-being of those suffering from mental health challenges.
Why dentists may have poor mental health?
In healthcare, most of the conversations surrounding the impact of mental health on caregivers is about physicians. Dentists, likewise, seem to be as or more susceptible to the effects of poor mental health when the two professions are compared. A query of the CDC's National Occupational Mortality Surveillance for the years 1999 through 2010 found that dentists were more than two-and-a-half times as likely to die by suicide as members of the general population. Farmers, fishers and forest workers were only 0.9 times more likely than the rest of the population.
Read more: How to handle mental health issues in the dental practice
Researchers suggest that more than half of people who died by suicide did not have a known diagnosed mental health condition at the time of death. Suicide is rarely caused by a single factor.
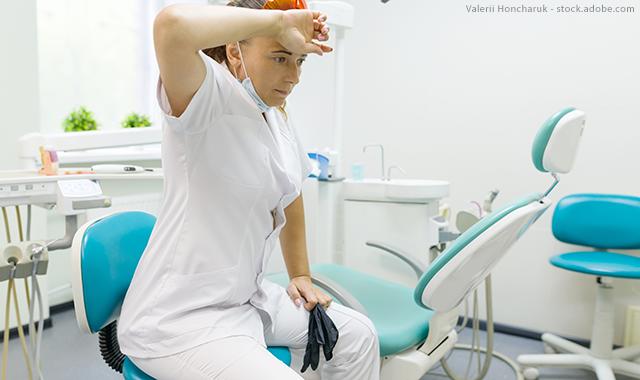
Dentists are in a unique position, literally. They spend their day bent over a patient in an awkward position, their necks often bent or crimped, their backs strained while trying to peer into the depths of their patient’s mouths and holding tools for long periods of time.
Steven Stack, a criminal justice professor at Wayne State University, is one of the few researchers to study the specific correlation between dentistry and suicide. His study cited decades of previous research on suicide rates among dentists and showed that being a dentist increased one's risk of suicide by 564 percent. Dentists practice under significant stress: financial needs, physical and emotional stress, potential isolation, and even unfavorable public perception are cited as negatives of the profession.

The American Dental Association also found 11 percent of dentists were diagnosed with depression, and 6 percent of dentists surveyed had an anxiety disorder, while only 3.1 percent of the general population did. Four percent of dentists reported panic disorder, while only 2.7 percent of the general population reported the same. Generally, some of this results from people not liking experiences with their dentists; dentists are in a career where “nobody wants to see them” or their office is the “last place they want to come back to.” For dental professionals, that perception can be depressing.
By and large, dentists operate in rather confined, small spaces, which can lead to isolation. Repetitive patient conversations including statements such as, “Are you a real doctor?” and, “I wish I didn’t have to be here to see you,” are also blamed for creating insecurities in dentists. A recent piece about the most hated professions in America listed dentists at the top, followed by politicians, lawyers, used car salesmen and even stock traders.
Trending article: Break out of your restorative rut
Although mental health and suicide prevention efforts largely focus on identifying and providing treatment for people with mental health conditions, there are many additional opportunities for prevention.
Creating healthy mental health environments
In essence, poor mental health can lead to poor overall health. Healthy work environments are key to job satisfaction. The happiest employees-and business leaders-engage in interpersonal relationships, and possess a sense of meaning or purpose among the parts of their job with which they are most satisfied. Those who leave their jobs tend to cite lack of respect, teamwork and growth among their top reasons for quitting. A healthy workplace, even in a field perceived poorly as dentistry, is where individuals feel valued and supported, and where other aspects of a person’s life are respected.
This is no truer than it is for dentists. Yet, not enough employers are taking steps to prevent poor mental health in their workplace, Willis Towers Watson’s 2019 Emerging Trends in Healthcare Survey shows. Only 22 percent of employers currently have or plan to implement programs to address suicide prevention in 2019; 15 percent of organizations are considering programs to prevent suicide over the same time frame. Employers can take action by partnering with outside vendors, providing access to employee assistance programs (EAPs), offering education programs or sponsoring worksite campaigns. Offering programs to help combat mental stress and advance the emotional intelligence in your dental practice is highly beneficial to the overall health of everyone in practice, Dr. Rahul N. Mehra, M.D., a neuropsychiatrist, founder and chief physician executive at National Center for Performance Health says. In fact, Mehra has developed an educational session targeted to dental practices that addresses this challenge head on.
“How Your Team's Mental Hygiene Affects Practice Performance” is an educational session being offered by NEA Powered by Vyne and the National Center for Performance Health. In this first-of-its-kind session, Dr. Mehra discusses how practice leaders can improve their own emotional intelligence and that of their employees.
Continue reading on page two...
Signs of depression: What to look for
Per the ADA’s Dentist Health and Wellness Survey, of those surveyed, 28 percent of dentists sought help for their mental health disorder, but 44 percent of the dentists interviewed said they believed they could solve their own problems and did not seek professional help. Obviously, this is not the best course of action. Dentists often are reluctant to seek formal help because of the possible stigma related to it.
One of the best approaches to address this may be by adding an employee assistance program (EAP) to the benefits offered by the practice. Making use of the benefit through such a program is confidential and free to employees. These programs provide incentive, because they are free and confidential, for those in the practice to seek professional mental health support. For practice leaders, such programs are often inexpensive additions to the benefit plans offered and help boost the “emotional intelligence” of the organization.
According to a recent report, 92 percent of employers are planning to offer wellness programs focused on mental and emotional health, encouraging because physical and mental health are inextricably linked. Employees experiencing these stressors miss an average of nine work days each year. The top objectives for wellness programs are improving employee engagement and performance.
Related reading: The biggest mistakes dentists make: Never taking a vacation
The best way to support a colleague suffering from depression or poor mental health is to encourage them to seek professional help. The ADA actually has prepared a resource guide that identifies signs and symptoms a person battling with depression may present.
Those signs and symptoms may include:
- The individual doesn’t seem to care about anything anymore
- He or she is uncharacteristically sad, irritable, short-tempered, critical or moody
- They become absent in their work, and become less productive
- He or she has lost interest in work, hobbies and other pleasurable activities
- The individual talks about feeling “helpless” or “hopeless”
- He or she expresses a negative outlook on life
- They frequently complain of aches and pains, such as headaches, stomach problems and back pain
- They also complain of feeling tired and drained all the time
- He or she withdraws from friends, family and other social activities
- They sleep less than usual or oversleep
- They eat more or less than usual, and have recently gained or lost weight
- He or she has become indecisive, forgetful or disorganized
- They drink more or abuse drugs, including prescription medications
Based on Dr. Mehra’s experience, recognizing and managing potential mental health challenges among peers and practice leaders is key to keeping one’s mental bill of health clean. Dental practice leaders face unique concerns in that they need to be aware of mental illnesses that can cause other health concerns, up to and including drug abuse/misuse and suicide. Because of this, practices and their leaders must be proactively involved in maintaining the health and well-being of their teams, and they should be trained to recognize when someone needs further assistance.
Getting professional mental health help
While there is no substitute for professional treatment and advice, one simple first step a practice can take toward learning more about mental health and wellness is reviewing a recent educational session by Dr. Mehra. In it, Mehra speaks about recognizing and managing potential mental health challenges with peers and physicians; understanding how to handle emotion-driven situations in the practice; coping with stressors of everyday life to attain a good work/life balance; and evaluating overall team performance and well-being. The event (you can listen here https://attendee.gotowebinar.com/register/1234063659758104321) may be a good place to start.
Ultimately, if you or someone you know is struggling with depression or has had thoughts of harming themselves or taking their own life, get help. The National Suicide Prevention Lifeline (1-800-273-8255) provides 24/7 free, confidential support for people in distress as well as best practices for professionals and resources to aid in prevention and crisis situations.