Study finds technology allows remote diagnosis of cleft palate patients
The study determined that readily available technology can make clinics more efficient and reliable while providing remote care.
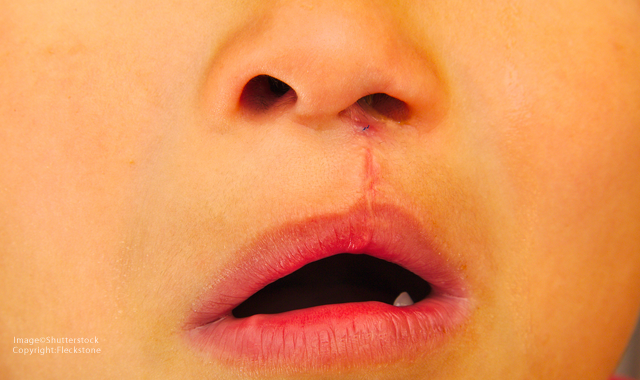
In today’s connected world, surgeons and anesthesiologists have the ability to use widely available technology, such as GoPro cameras, Skype, WebEx, and Google Chat to remotely care for patients in distant countries.
This readily available technology has the ability to make clinics more efficient and reliable. A recent study examines the possibilities these tools create, and how they can assist in the diagnosing of patients in remote areas.
In the current issue of The Cleft Palate–Craniofacial Journal, researchers asked whether remote videos could be used to reliably diagnose a cleft lip or palate. Due to lack of funding in developing countries, citizens’ access to medication, medical devices, and surgeons is limited. Through Hands Across the World, a nonprofit that provides reconstructive surgery for patients with congenital conditions, the researchers reviewed digital video evaluations of patients with oral clefts.
At a hospital in rural Ecuador, 27 patients were evaluated for oral clefts. Researchers compared in-person and remote video assessments made by two separate craniofacial surgeons. The video was taken with an iPhone, without special lighting or camera enhancements. The surgeons who made in-person and remote evaluations nearly always agreed on how patients with a cleft lip or cleft palate should be treated. Those who assessed patients with an alveolar cleft agreed only about half of the time, likely because of the challenges of performing an oral exam via video.
Ultimately, more than 80 percent of the patients examined underwent oral cleft surgery. The researchers speculated that using remote video in diagnosing oral clefts among Ecuadorians could have an economic impact of roughly $7.9 million over 20 years. Worldwide, nearly 5 billion people do not have access to essential surgical care, and almost a third of all deaths and disabilities result from surgically treatable conditions.
“We are well positioned to invent new ways to work with technology to improve surgical outcomes,” said researcher Christopher Hughes. Among potential improvements, he listed fewer redundancies, less lost time, and more patients seen in the clinic, as well as speedier and more affordable care for patients. “If we can scale our model,” he said, “then we can change the way that children with cleft and craniofacial disorders are treated in their own country.”
The researchers concluded that digital technology could be used to reliably diagnose cleft lips and palates, and reduce the cost to patients with oral clefts. They argue that, most importantly, digital evaluations let surgeons provide high-quality care even in remote, rural locations.
Full text of the article “Remote Digital Preoperative Assessments for Cleft Lip and Palate May Improve Clinical and Economic Impact in Global Plastic Surgery,” The Cleft Palate–Craniofacial Journal, Vol. 54, No. 5, 2017, is now available at http://www.cpcjournal.org/doi/full/10.1597/15-305.