Study finds possible link between P. gingivalis, Alzheimer's Disease
Cortexyme, Inc., a clinical-stage biopharmaceutical company, announced the publication of research further documenting the ability of the pathogen Porphyromonas gingivalis to invade neurons and trigger Alzheimer’s-like neuropathology.
Cortexyme, Inc., a clinical-stage biopharmaceutical company, announced the publication of research further documenting the ability of the pathogen Porphyromonas gingivalis to invade neurons and trigger Alzheimer’s-like neuropathology. These findings are set to be published in the June 2020 issue of the Journal of Alzheimer’s Disease, while an early online version is available now.
P. gingivalis is primarily known for its role in causing periodontitis in the oral cavity, said Dr. Stephen Dominy, Cortexyme’s chief scientific officer and co-founder, and co-author on the paper.
“Researchers at Cortexyme and independent labs around the world have assembled a compelling body of data on [P. gingivalis’] ability to infiltrate the brain and cause pathology characteristic of Alzheimer’s disease. This latest research strengthens the connection between P. gingivalis and Alzheimer’s, and underscores the importance both of studying the pathogen and targeting it with potential therapeutics, such as COR388,” Dr. Dominy said.
P. gingivalis is a Gram-negative, asaccharolytic bacterium, meaning it breaks down proteins for its primary source of energy by utilizing toxic virulence factor proteases known as gingipains. The team at Cortexyme has previously demonstrated the presence of gingipains in more than 90 percent of post-mortem brains of patients with Alzheimer’s Disease. Cortexyme and others have also shown that P. gingivalis results in brain infection and classic Alzheimer’s Disease pathology, including neurodegeneration, inflammation, beta-amyloid, and tau pathology.
In the JAD paper, researchers demonstrate for the first time in vitro that P. gingivalis can invade and persist in mature human neurons expressing active gingipains, and that these P. gingivalis-infected neurons display signs of Alzheimer’s-like neuropathology, including:
- Disruption of the cytoskeleton, which is critical for proper cellular function
- Degradation of tau protein and increased tau phosphorylation, a key regulator of axonal transport mechanisms
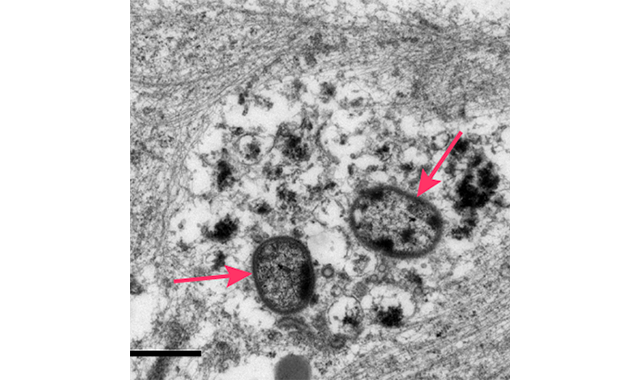
- Accumulations of intraneural autophagic vacuoles and multivesicular bodies, suggestive of disruption of normal lysosomal function
- Synapse loss, one of the earliest pathological events in the onset of Alzheimer’s Disease
“This research sheds new light on the ability of P. gingivalis to persistently infect and trigger Alzheimer’s-like pathology in human neurons, providing additional evidence for the gingipain hypothesis of Alzheimer’s causation that Cortexyme and our fellow researchers are aggressively pursuing,” said Casey Lynch, chief executive officer, chair, and co-founder of Cortexyme. “We believe gingipain inhibition has the potential to be an important, differentiated mechanism of action against AD, and are committed to fully evaluating its potential in the GAIN Trial, the ongoing Phase 2/3 clinical study of COR388, our lead investigational medicine, in mild to moderate Alzheimer’s disease.”
For more information on this research, view the early online version of the paper here. The final publication is scheduled for Volume 75, issue 4 of JAD, June 2020.
Cortexyme is pioneering a novel, disease-modifying therapeutic approach to treat what it believes to be a key underlying cause of Alzheimer’s and other degenerative diseases. Cortexyme is targeting a specific, infectious pathogen found in the brain of Alzheimer’s patients and tied to neurodegeneration and neuroinflammation in animal models. To learn more about Cortexyme, visit cortexyme.com.