Oral Health in the Heart of Opioid Country and Beyond
There is no doubt that drug addiction, particularly addiction to opiates, is a public health crisis that crosses regional, racial and class boundaries in the United States today. While it is expected that less-urgent matters take a backseat as doctors, researchers, police and governments on every level scramble to address sky-rocketing overdose deaths, less trendy issues, both new and old, are becoming worse. In Appalachia, long-neglected dental health affects people of all ages, and while the region may be infamous for its poor oral hygiene, it is hardly the only one suffering from this health care emergency.
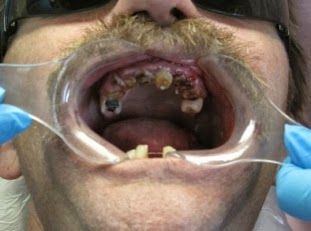
A plethora of contributing factors, namely addiction and lack of access to medical care, are creating a generation of abysmally poor oral health.
Appalachia is often the butt of jokes about missing teeth, but few truly understand the grim reality that the region, and many others across the U.S., live with. According to the Center for Oral Health Research in Appalachia (COHRA), the population of this rural landscape bears the brunt of the nation’s oral health problems with the largest per capita rate of disease, infection and decay.
Like any isolated area with high rates of poverty, discrepancies in general and oral health abound. COHRA, a continuing research project at West Virginia University and the University of Pittsburgh, is one of the only programs attempting to understand the multiple causes of oral health disparities in Northern Appalachian populations. Now in its second phase, researchers follow women during pregnancy and beyond after its phase-one findings indicated that caries begin in early childhood.
RELATED: More Coverage on
- How to Choose a Financial Planner
- The Unwavering Passion of DDS Greg Vigoren
- Deciphering your Long-term Care Insurance Policy in Advance
Dr. Dan McNeil, principal investigator for COHRA at WVU, says on top of having some of the poorest oral health, his state boasts the highest rate of overdose deaths in the U.S. West Virginia’s environmental and economic issues have drastically changed the fabric of the state, leaving many unable to provide for themselves or secure adequate health care. The state’s large senior population, according to McNeil, is also a propellant of general health problems like chronic pain. Availability of opiate medications as the solution for pain has helped pave the way for the staggering overdose death rates.
“We have a unique population and a unique set of environmental and economic circumstances right now. Unfortunately, all that is coming together to make the opioid crisis as bad as it is in our state,” McNeil said.
The painful and unsightly tooth decay that plagues the region often begins in children as young as one, and nearly half of Appalachia’s most high-risk population is completely toothless before the age of 70. Children suffer the most physical and emotional pain from inflamed gums, cavities and rot. School absences are a common side effect, as is dental fear associated with excruciating visits to address early childhood oral ailments. These factors, combined with lack of Medicaid coverage for adults up to 55, establish a pattern of avoiding dental care.
“If you have missing dentition, it’s a huge social issue. We have also done with work with orthodontics, and one of the problems we’ve seen is that children who get care through Medicaid have an increased rate of not completing that care,” McNeil added. “That leaves [young patients] with less-than-functional and less-than-aesthetic dentition, which has social and employment implications later in life.”
With no dental insurance or even a dentist nearby, many are left with no choice but to pull out their own teeth using pliers or other make-shift tools. West Virginia in particular has a lower rate of insured patients, thus decreasing dental utilization. McNeil said this lack of comprehensive oral health care creates huge problems, as people are dealt with on an emergent basis rather than a preventative one.
“It was probably six to seven years ago they really just started breaking off — some of them even below the gum line. Worst pain of my life,” Bobby Horn, a Grundy, Virginia, resident, told PBS Newshour in 2011.
Social and general health is hurt by these realities. People with visible extractions are less employable, further perpetuating stereotyping and misunderstanding of the Appalachian population. While West Virginians do face serious problems with addiction and oral health, McNeil says there are many positives about the state and its people that often go ignored in favor of stigmatization.
“There is a strong sense of self-reliance. People want to stand on their own two feet and get themselves out of problems,” McNeil said. “There is a strong sense of patriotism and sense of devotion to community, and unfortunately, that is one of the things the opioid crisis has caused problems for. There is also a real devotion to young people and to the future. They want life to be better for their kids than it was for them in terms of health issues, including oral health.”
COHRA, Continued
While oral ailments have persisted in Appalachia for decades, comprehensive efforts to reveal their causes and remedy them have only been underway since 2000. Most families residing in Northern Appalachia rely on well water, which Mary Marazita, principal COHRA investigator at PITT, says contains little to no fluoride.
“Like much of Appalachia, the counties are fairly mountainous, remote and struggle economically,” Marazita told the National Institute of Dental and Craniofacial Research. “A lot of people still live out of town on farms or family land. We ask our participants to bring in water samples from their homes, and that allows us to test fluoride levels.”
But lack of fluoride is hardly the primary cause of decay, periodontal disease and the array of other oral conditions impacting the Appalachian region. Given the generational endurance of these issues, considering patients within the context of their family situations is crucial, as is education on oral health for new parents.
“One of our most striking findings to date is that the oral health disparity begins very early in life,” Marazita continued. “The overall increase in decay that is seen in our study population, compared to the rest of the nation, typically remains steady throughout childhood into adulthood.”
Educating these rural communities, however, is not as simple as reminding them to brush and floss twice a day. In places where families struggle to provide the basics and often suffer from more life-threatening issues like addiction, heart disease and lung cancer, oral hygiene is low priority. Other illnesses, especially addiction to meth and opioids, join forces with poor diet and sugary drinks to accelerate the already nightmarish levels of decay and disease.
Lack of access to dentists, along with the U.S. health care system’s treatment of dental health as non-essential, further exacerbates these disparities. And it does not end with Appalachia.
Beyond the Mountains
In an increasingly divided nation that struggles to provide basic health care to the poor, having a full set of healthy teeth is a privilege few can afford. Though an ailing mouth affects the rest of the body — potentially leading to heart disease, diabetes and even cancer — alternet.org writer Anna Sanford reports that in the eyes of insurers and even government-subsidized programs, dental benefits are optional.
Across the U.S., Sanford writes, more than 50 million people live in Dental Health Professional Shortage Areas and are forced to go to emergency rooms for treatment. New federal requirements are improving coverage for children, but individuals over 19 often go years without receiving dental care.
“Emergency room visits for dental-related issues among adults over 65 rose from 1 million in 199-2000 to 2.3 million in 2009-2010,” the Center for Medicare Advocacy (CMA) reports. “As overall health care system reforms aim to emphasize primary and preventive care and deter costly emergency care, dental care remains neglected by policymakers at a time when the need for attention is greater than ever.”
Going Forward
Combatting the lack of dental care on this scale — particularly in this era of mounting public health crises and uncertainty about the future of Medicaid, Medicare and the Affordable Care Act — is no easy feat. But according to CMA’s report, solutions are available.
Advocating specifically for policy changes to improve public health, the group encourages strengthening community education and outreach, as well as addressing provider payment and shortage issues. COHRA’s research in their target area can be applied on a larger scale to educate affected communities with consideration to income levels, literacy and recruitment of families and dental professionals.
“Access to dental care is another community issue that can contribute to the disparity. It can be extremely difficult for rural communities to recruit dentist,” Marazita said. “Without a dentist in town, people must go out of their way to find treatment.”
McNeil, who specializes in psychology, emphasized the importance of a strong inter-disciplinary approach that allows dentists, hygienists, physicians, psychologists and pharmacists to work together.
“We need to ensure that [oral health] is brought to the table as an issue. We need to impact both national and state policies, even local community policies and school system policies [to promote] tooth brushing and things like that in their curriculum,” he said.
The economic factors in place, however, stand as one of the most profound causes of health disparities, and states must work to provide incentives and opportunities for young people. Increased outflow from places like West Virginia and Northern Pennsylvania, which relied primarily on the coal and oil industries, is creating a deficit of wage-earning people.
“That leaves greater problems for the state budget, but at the same time the state continues to maintain a program to provide tuition for students going to college in the state,” McNeil continued. “Part of the effort is to keep young people in the state so they will hopefully settle here, become tax payers and contribute to the well-being of the state.”