How to Get New Dental Practice Staff Up to Speed with Infection Control
Every dental practice has specific infection control protocol that needs to be followed. It’s vital that new staff receive adequate training for best infection control practices.
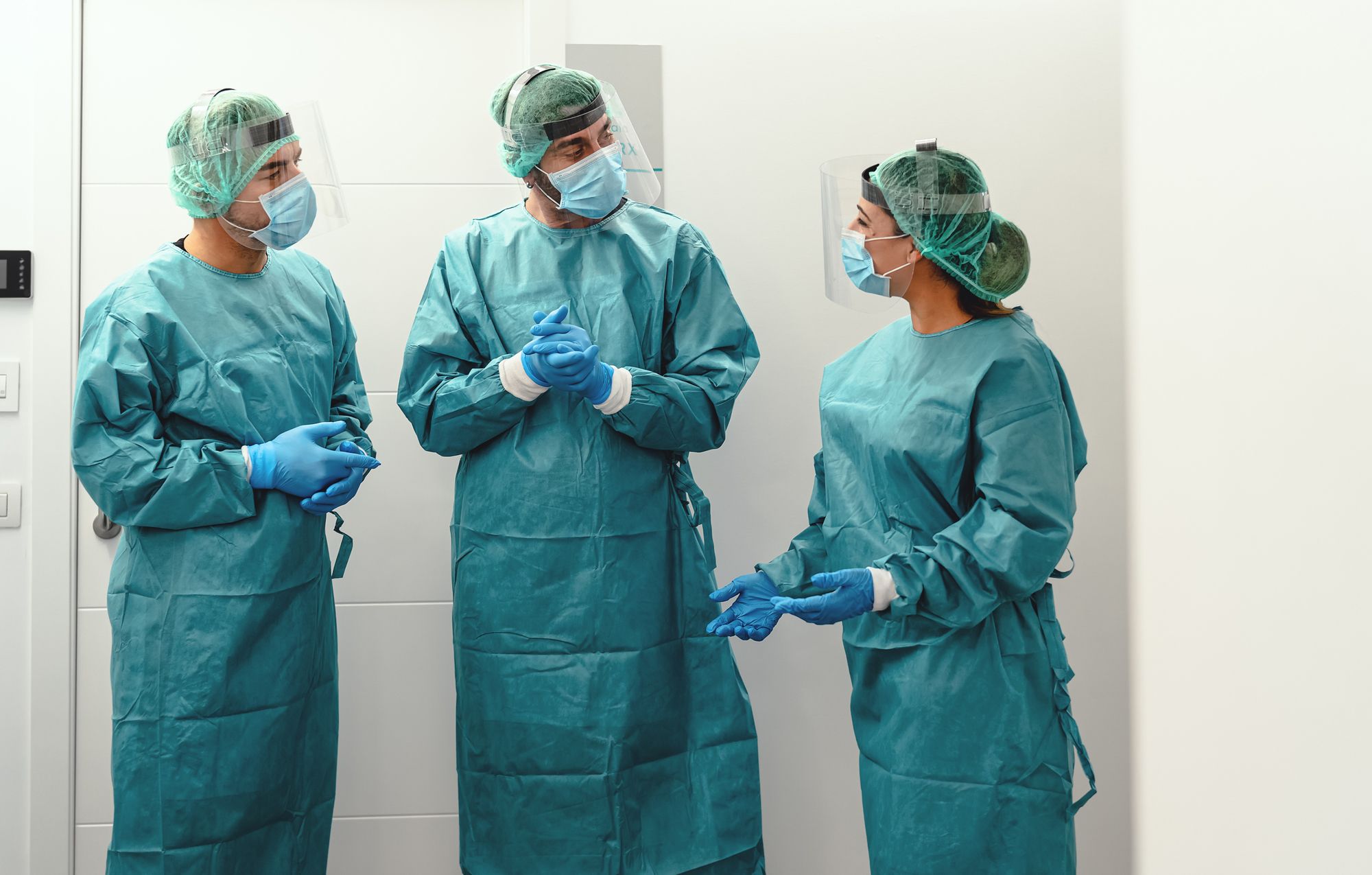
How to Get New Dental Practice Staff Up to Speed with Infection Control. Photo courtesy of Alessandro Biascio/stock.adobe.com.
While best infection control processes might seem universal, there are differences from state to state and practice to practice. Because there can be such variability, onboarding new staff – whether they are temporary employees, new hires fresh out of dental school, or veteran dental professional coming to a practice – on the infection control rules at a new practice is a necessary part of orientation.
“There is the potential for conflict when a new team member comes into the office, because of misunderstandings, and that’s where clear guidance lets everyone know what’s expected of them and what the procedures are,” Jackie Dorst, RDH, BS observes. Dorst is an infection prevention consultant and speaker. “An excellent way to introduce new team members is to share a copy of those written infection control standards that every office should have. They should share those with the new employee prior to the first day, so that they can read through them and anticipate new or different infection control protocols. Infection Control standard operating procedures (SOPs) ensure consistency and checklists ensure no steps are overlooked. I liken the infection control checklists and logs to what management gurus, like Robert Crawford, have put out there: ‘What gets measured, gets done. And what gets recognized gets done again, and even better’.”
The Same (But Different)
Infection control standards and mandates differon a state-by-state basis, and while every practice within a given state hasthe same requirements, each practice may get there in its own way.
“The requirements may differ depending upon which state you’re in, but everyone should be following the Centers for Disease Control (CDC) guidelines and Occupational Safety and Health Administration’s (OSHA’s) Bloodborne Pathogens Standard,” Lisa Kane, DMD, says. Dr Kane is a speaker and infection control consultant at Dental Office Compliance of New England. “That’s just standard of care. Every office might do things differently. Some offices might have a lot of barriers; some offices might disinfect surfaces. Regardless, when you get into a new office, you’re required – within 10 days – to have OSHA training for the new employee. So, it should be based on your policies. Yes, there are best practices. Things are very generic, but each office has its own standard operating procedures and ways to do them. So, it’s really important that when you onboard a new person, anyone can review all of your specific plans, policies, and protocols; how you set up a room; how you break down a room; how you do everything.”
A lot of variability comes down to what sort of products that the practice uses. No 2 practices are likely to be the same.
“Infection control protocols in the office encompass everything from hand hygiene to surface disinfection to personal protective equipment (PPE) and sterile instrument management,” Dorst says. “Those can vary greatly from office to office. Yes, the principles are the same, but the variations may be such as which disinfectant brand the practice uses and what is the wet contact time? That depends on the brand of disinfectant that the office is using. And every office – for contaminated surfaces – has the choice of using a barrier or cleaning and disinfecting potentially contaminated surface after treating a patient. So, a new employee would need – on their initial introduction to the infection control protocols – specific directions on the disinfectant that they use, the wet contact time, how many wipes are used in the operatory, and on which surfaces are barriers placed. PPE use can vary from office to office such as brands, reusable or disposable and disinfection or cleaning.
“The new employee needs to know when they would wear an N95 respirator in this office,” she continues. “It should be with aerosol-generating procedures at this time during the pandemic. When would they wear a procedure mask? And if they’re going to wear an N95 respirator – before they could even start work in the office, caring for patients – they should have a medical evaluation and fit test with that brand N95 respirator. And then there are isolation gowns. Which type are they going to wear – disposable or launderable? Where are clean and dirty gowns stored? Does the office have the right size and type for the new employee? Let’s say a new employee comes in and they happen to be a very petite person with a very small face and small hands. Does the office have the extra small sizes of PPE to accommodate the new employee?”
Office variability, also, extends to the sterilization center.
“The sterilization rooms can vary greatly,” Dorst says. “For example, handpieces are costly pieces of equipment in the office, and yet the cleaning and sterilization process is specific for each handpiece. Employees must follow instrument and equipment manufacturer’s disinfection, cleaning and sterilization directions. Employees must be aware of what the manufacturer’s instructions for use (MIFU) are. The MIFU’s should be stored in the sterilization room. If the employee has a question or thinks, ‘Wow, I don’t remember quite what the procedure was for this item, the employee can review the directions for reprocessing the item.’”
In the end, however,those differences shouldn’t be overall obstacles.
“It depends on what kind of practice they were in before,” Dr Kane says. “Ideally, if you’re organized and you have written procedures and you have a standard way of doing things, it should be an easy thing to do.”
Training is Key
Training the new staff is a necessary step toward ensuring that everyone follows the same processes. Dorst says that a good way to ensure proper, effective onboarding is to have a dedicated person in charge of training.
“We’re busy in the office and often training is sacrificed because of our busyness,” Dorst says. “That’s when it opens the practice up to breaches in infection control and sterilization and lapses in training. Unfortunately, if an employee starts doing 1 specific step incorrectly, that can persist and be continued, if it’s not evaluated. That evaluation by the mentor employee or the lead clinical assistant or lead clinical dental hygienist is so important to maintaining the standard of infection prevention and preventing breaches.”
The practice should already have an infection prevention coordinator, and the trainer could either be this person or someone else, entirely.
“That clinical lead or the mentor for the new employee is, ideally, the infection preventionist for the clinical team,” Dorst observes. “However, they may be busy or have so many responsibilities that it would serve better to have a proficient, experienced clinical team member who has good training and teaching skills. Remember the good teachers that you had through school? Subjects might vary, but basic teaching techniques and an encouraging attitude get results. Having a mentor who inspires and motivates is valuable in getting an employee started off on the right foot within infection prevention. I highly encourage offices with a new team member to have at least a 30-day new employee mentoring with that clinical mentor. At the end of each day, for that first 30 days, the mentor and the mentee meet together for 5, 10, or 15 minutes, and there’s an interchange of, ‘What issues did you encounter today?’ ‘What questions do you have?’ The mentor verifies that the employee – through observation and verbal information exchange – is doing each of the infection control procedures correctly each day, because unfortunately, even in an experienced longstanding team, there can be some inconsistencies. We might bring bad habits with us from a previous dental office that we worked in, or someone misunderstood newer techniques for infection prevention.”
Everyone Has Something to Offer
Ultimately, having consistent training for new hires ensures overall patient and workplace safety.
“Everything has to come from the top,” Dr Kane observes. “Everyone should value infection control and safety. I think initially having the explanation about the importance of it and why you’re doing this, that it’s best for you as a team member and it’s best for your patients, is important. If everybody is doing things the right way, then you’re going to be safe. Making a checklist is a good way to do it. I would have the infection control coordinator own it. I would have them go over everything. Yes, there should be something written so that they don’t have to know procedures for everything, then they can understand it.”
How long will it take for a new hire to learn the practice’s way of doing things? It depends.
“It depends on how long they’ve been doing it,” Dr Kane says. “I think when we go in offices and people are doing things that they’ve been doing forever, educating is the most important thing. Obviously, not shaming people, not telling them that they’re bad or doing things wrong. You can talk about the guidelines, new research, new things, and it kind of explains why you’re having them change what they were doing before and how that’s beneficial to everyone.”
Infection control education can be a 2-way street. That new employee may bring something unique to the practice, so it’s a good idea to keep an open mind.
“A big thing is to not have an ego in dentistry,” Dr Kane says. “Make sure your team understands that your ultimate goal is to do right by patients and give patients the best care that they need. So, if somebody comes in fresh out of school and they have some more efficient way of doing something, listen to them and don’t think that, ‘Oh, they’re a kid and I know better.’ Really listen to what they say. And it may not be what’s right for your practice, but I think being open and understanding that any infection control, OSHA-related thing is for everyone’s safety.”
Starting any new job can be somewhat overwhelming and there’s a lot involved in onboarding new team members, but with methodical, consistent education and training, learning the practice’s infection control ropes need not be daunting.