How to perform closed crown lengthening with an all-tissue CO2 laser
A demonstration of how to remove both soft tissue and bone using a Solea® dental laser.
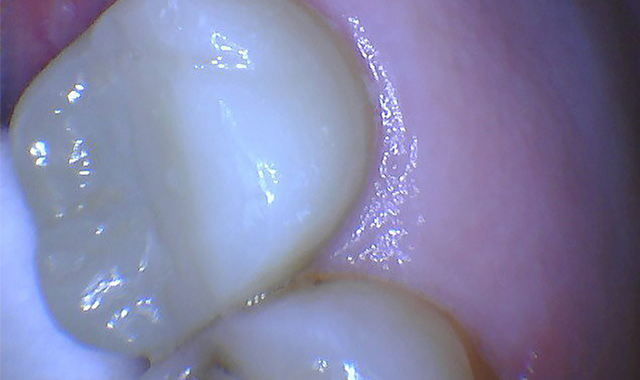
A 63-year-old female patient presented for an emergency visit having fractured off the palatal cusp of tooth #15. She experienced cold sensitivity and discomfort in that area. The patient was very apprehensive about dental surgery because she was undergoing chemotherapy and had a session scheduled for the next day.
A pre-operative diagnostic radiograph showed no endodontic pathology. She is in excellent periodontal health (Fig. 1). Oral evaluation of the patient indicated that the palatal cusp of #15 fractured subgingivally to the level of the alveolar crest (Fig. 2).
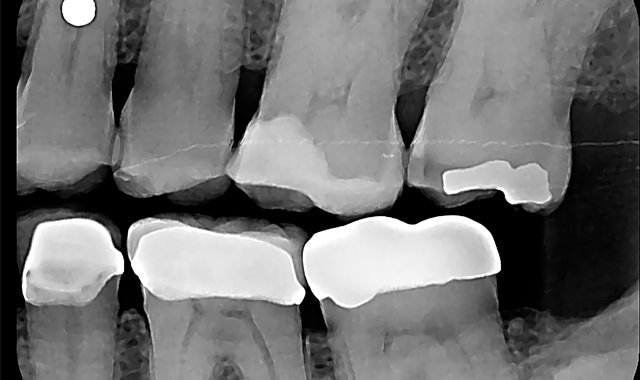
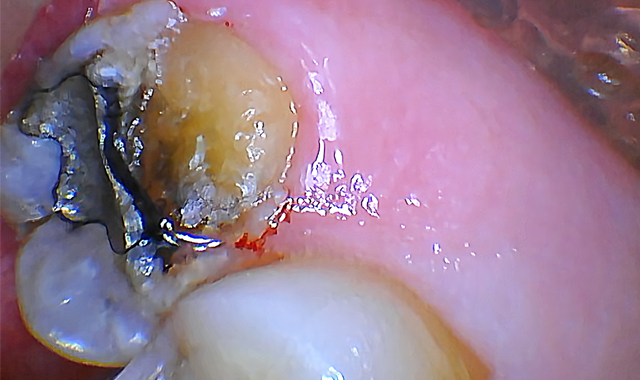
Fig. 1 Fig. 2
Case study
A crown lengthening was required in order to expose sufficient tooth structure for a further restoration and to establish biologic width. As no interproximal bone needed to be removed, a flapless (closed) crown lengthening was to be performed using Solea®.
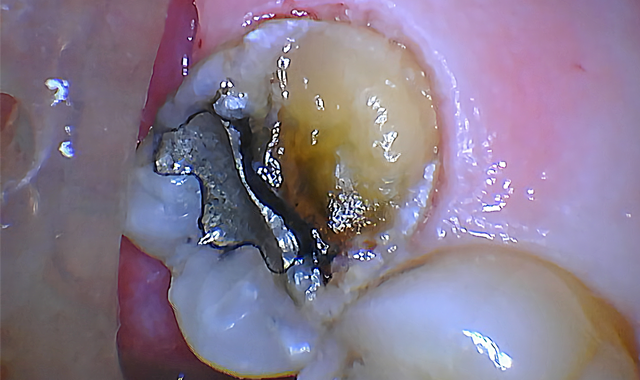
Fig. 3
Due to the patient’s medical history and her dental anxiety, crown lengthening via traditional instruments and technique would have been problematic.
The patient was anesthetized with a minimal amount of anesthetic (¼ carpule of 4 percent articaine with epi 1:100,000) injected to the palatal of tooth #15. This procedure is often performed without injection, but she was too worried about sensation and preferred to receive an injection.
Using the 1 mm spot size with cutting speed between 30-50 percent and 20 percent mist, the gingival tissue was ablated until the planned restorative margin could be seen (Fig. 3).
I then proceeded to remove bone using the 0.75 mm spot size with 80 percent cutting speed and 50 percent mist.
The laser was aimed down the long axis of the tooth to remove bone between the tooth and soft tissue.
The bone was ablated until the osseous crest was 2 mm apical to restorative margins (Fig. 4). Both steps were completed with virtually no bleeding.
To finish, a piezoelectric scaler was used to smooth the surgical site and a temporary restoration (Scotchbond™ Universal Adhesive, 3M and Beautifil Flow Plus, Shofu) was placed to prevent gingiva from growing back over the tooth structure. (Fig. 5).
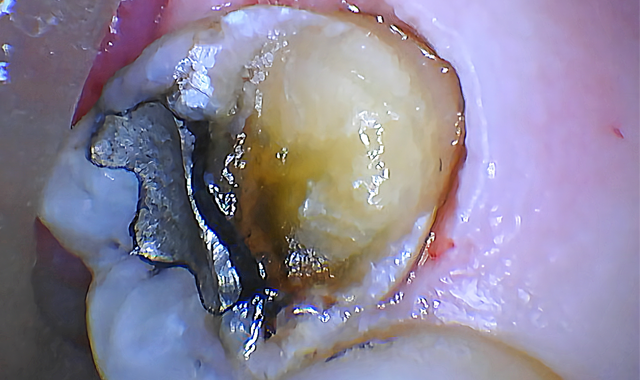
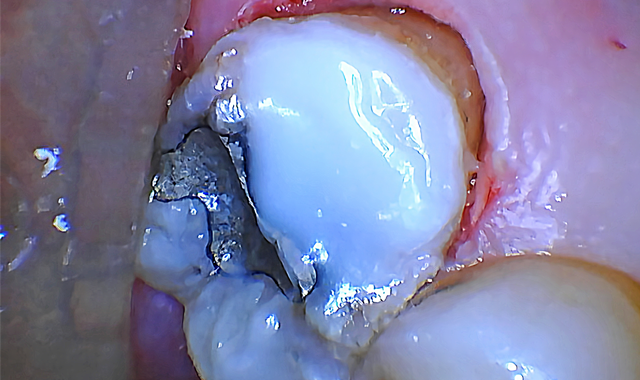
Fig. 4 Fig. 5
Note the excellent healing and tissue appearance at one week post-op when the tooth was prepped for a zirconia crown (Fig. 6). The patient was thrilled to report no post-operative pain or discomfort. Amazingly, rapid healing was observed with excellent tissue tone and appearance. She was grateful that the surgery went smoothly, was stress-free and much faster than she expected.
Conclusion
Solea made this challenging procedure amazingly simple. I was able to easily treat a patient who normally would have had to be referred to a specialist. I was able to perform a procedure easily that I would not be comfortable performing with traditional instruments due to risk of iatrogenic damage, etc.
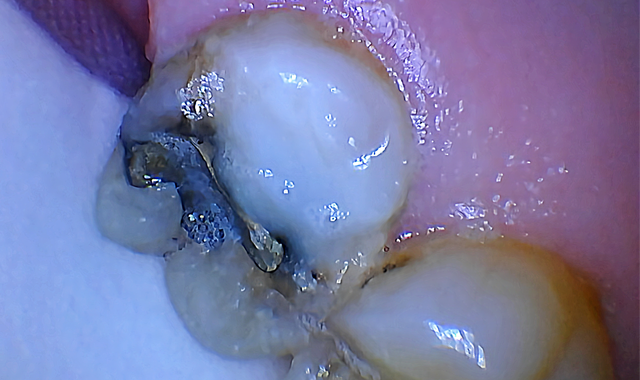
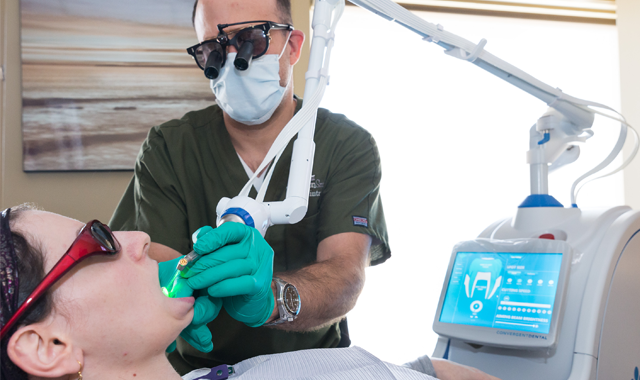
Fig. 6 Fig. 7
The total appointment time was less than 15 minutes, whereas utilizing traditional techniques, crown lengthening surgery typically takes at least an hour (Fig. 7).