How to Create More Esthetic Restorations
When it comes to restorations, practice, a little know-how and the right materials make perfect.
Placing direct restoratives on patients is a very common procedure in most general dental practices. While esthetics are important when utilizing composite restoratives, practitioners are also concerned about post-op sensitivity and longevity of the restorations.
Dentists can review the results of their techniques in radiographs taken at recare appointments and consult with patients about post-op sensitivity and esthetic results. Dentists can use techniques to improve the Class II posterior direct composite procedure. While many of us received minimal training in dental school on clinical placement of posterior composite restorations, it’s important to keep current on improved restorative materials and treatment modalities to ensure more consistent results.
Fig. 1
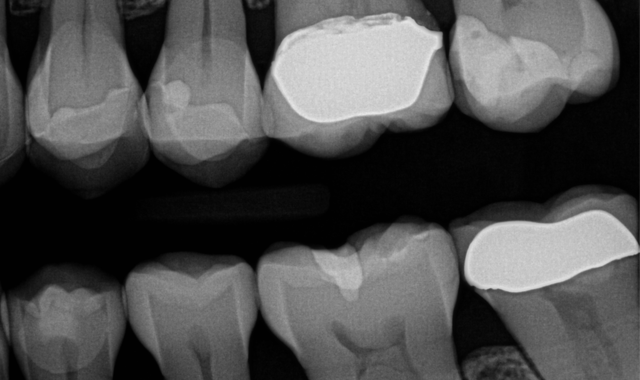
Fig. 2
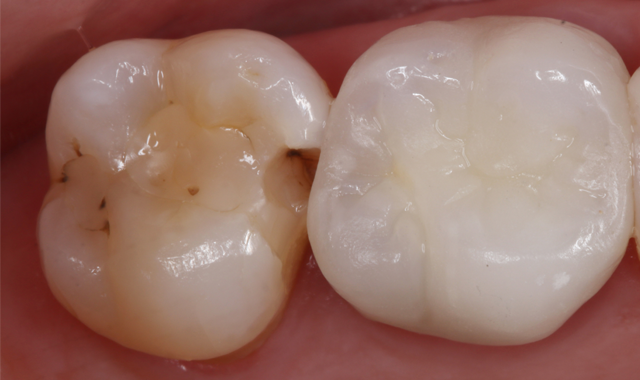
A 50-year-old female patient presented for replacement of a fracture and decay in an existing composite restoration (Figs. 1-2). While crowns or onlays would be the typical treatment of choice in our office, the patient will need to put off receiving indirect restorations for a couple years. It was decided that due to the depth of the existing restorations and the recurrent caries present, it would be wisest to perform caries control for the teeth.
Click through to see how this practitioner created great-looking restorations
The direct composite restorative of choice in my office is Tetric EvoFlow® Bulk Fill and Tetric EvoCeram® Bulk Fill. When treating cavities of this size, the composite material makes placement much more efficient and predictable while still offering a high level of esthetics.
The patient was anesthetized and a latex-free dental dam was placed with an NW clamp on the second molar (Fig. 3). Utilizing a Brasseler 6845KR.31.018 diamond, the old composite restoration was removed in its entirety. The deeper portions of the box were beveled with a 6856.018 diamond and the cavosurface margins were beveled to increase enamel bonding area and for esthetics.
Fig. 3
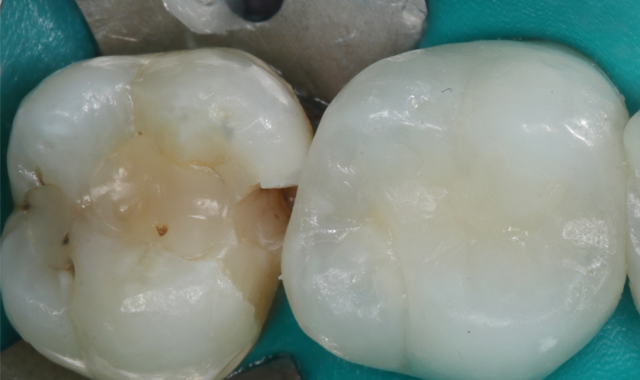
Fig. 4
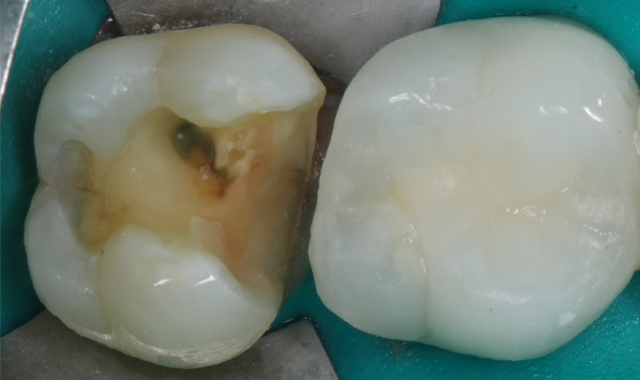
Once the preparation was complete, the preparation was micro-abraded with an air abrasion unit (PrepStart™, Danville) with a 90-degree .015 tip and 27-micron aluminum oxide powder. This step results in micro-retentive surface increases, surface area that potentially further increases dentin bonding and reduces post-op sensitivity (Fig. 4).
Fig. 5
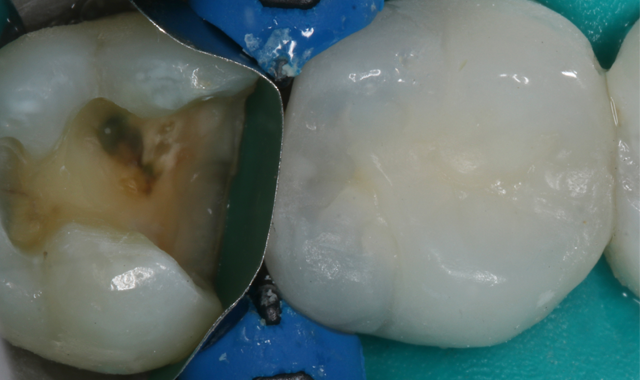
Fig. 6
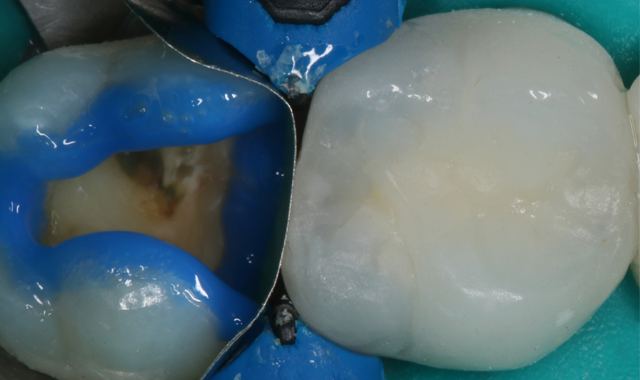
A Compsi-Tight™ 3D Ring with a SlickBand™ and WedgeWand® (Garrison) were used to replace the missing tooth surface and form the adaptive layer of composite restoration. It is very important in this step to have a tight interface between the band and tooth to allow for ultimate adaptation of the direct restoration to the margins (Fig. 5).
Fig. 7
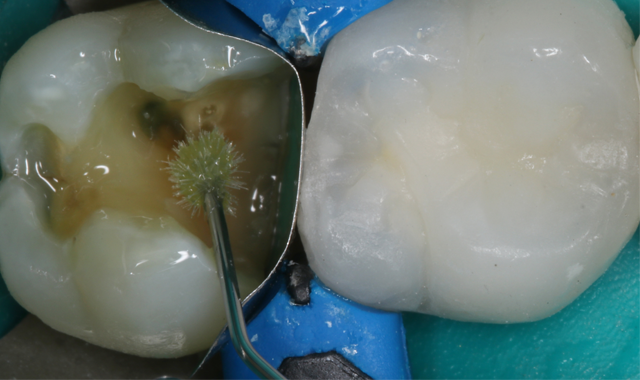
The next step was the selective etching technique, utilizing 35% phosphoric acid (Ultra-Etch®, Ultradent) on enamel only. The etch was applied on the enamel for 15 seconds and rinsed thoroughly (Fig. 6).
A universal adhesive was scrubbed on the selectively etched tooth per manufacturer’s instructions using Adhese® Universal in the VivaPen® delivery (Ivoclar Vivadent) (Fig. 7).
The adhesive was air-thinned with an A-dec air dryer to deliver oil- and moisture-free air and was light-cured for 10 seconds with a Bluephase® Style (Ivoclar Vivadent).
Tetric EvoFlow Bulk Fill Shade IVA was placed as a first increment. While traditional flowable materials need to be placed as a thin increment to minimize shrinkage stresses and allow for complete curing, Tetric EvoFlow Bulk Fill can be placed in increments of up to 4 mm without worrying about shrinkage stresses or incomplete curing. Taking advantage of Ivocerin® and its self-adapting and opacifying technologies means that practitioners get void-free restorations in the deepest of boxes, and the dark underlying tooth structure is blocked out with a similar dentin-like opacity. Figures 8 and 9 show before and after curing.
Fig. 8
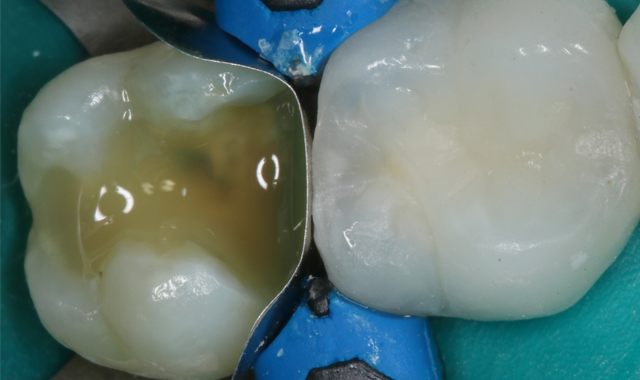
Fig. 9
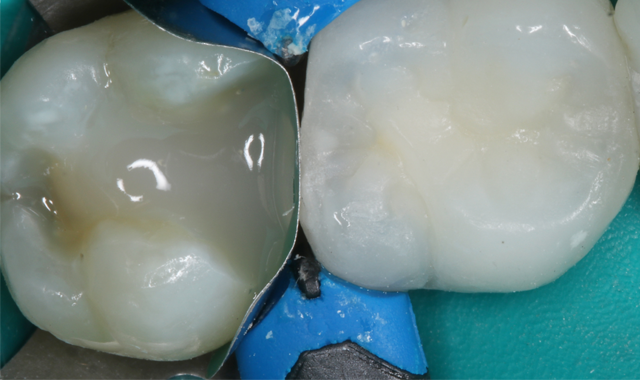
The final layer is a single increment of Tetric EvoCeram Bulk Fill Shade IVA (IVA is a universal “A-range” shade). The material was placed from a Cavifil, injecting directly into the preparation. The material was condensed gently with an OptraSculpt® composite instrument (Ivoclar Vivadent) and shaped with primary and secondary anatomy (Figs. 10-11).
Fig. 10
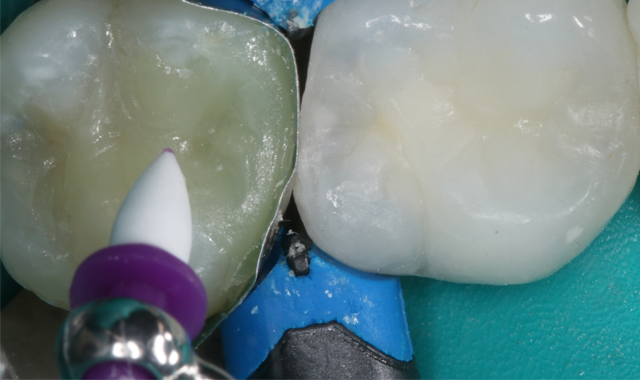
Fig. 11
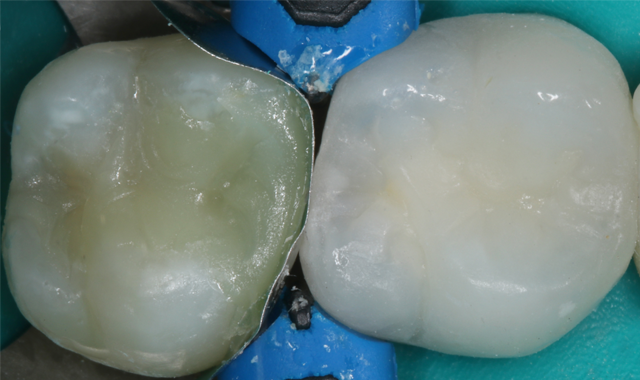
The composite was light-cured with the Bluephase Style for 10 seconds from the occlusal surface, then the band was removed and the restoration was light-cured again from the proximal surfaces for an additional 10 seconds to ensure complete curing (Fig. 12).
The composite was contoured with a Brasseler flame 8274.31.016 and the margins were contoured and defined with discs (Cosmedent FlexiDisc® Medium Grit) (Fig. 13).
Fig. 12
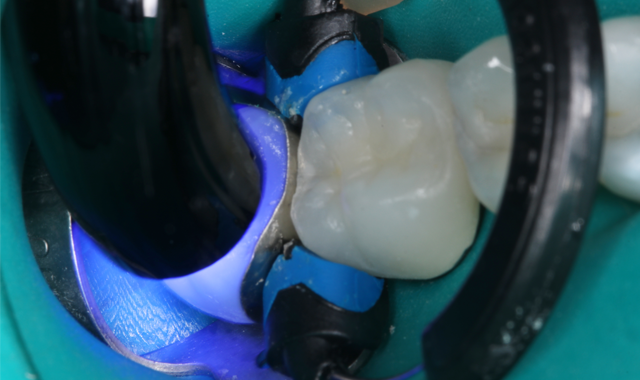
Fig. 13
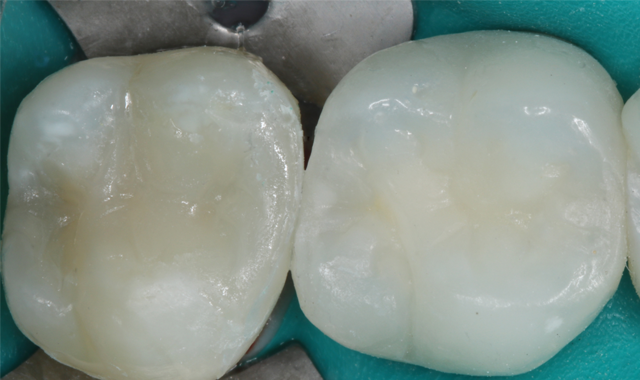
The restorations were adjusted for occlusion and polished with Astropol polishing points and finished with Enamelize polishing paste (Cosmedent).
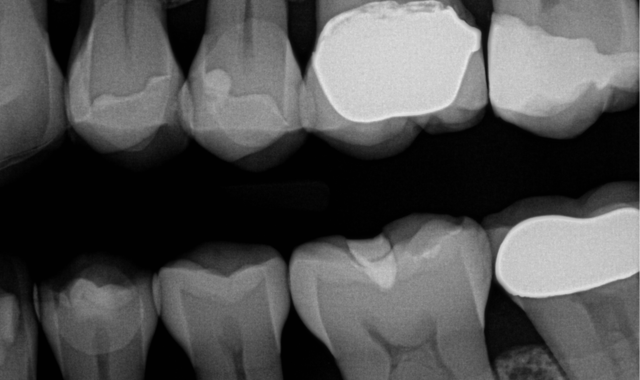
A post-operative picture and radiograph were taken to confirm ideal restoration placement with sealed proximal margins and a void-free restoration (Figs. 14-15).
Fig. 14
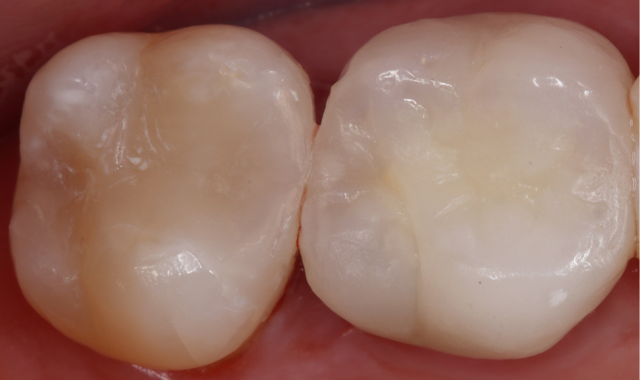
Fig. 15
Direct restorations can be challenging to complete with ideal results. The procedure begins with ideal isolation and is completed with regard to proper band placements and utilization of materials that facilitate ideal outcomes. Even larger restorations are completed with efficiency utilizing bulk fill restoratives that can provide not just shorter chair times for patients but also esthetics that exceed patient expectations.