How to avoid restorative Class II blues
Three clinicians give their suggestions on how to avoid Class II restoration complications and failures when working with composite resins.
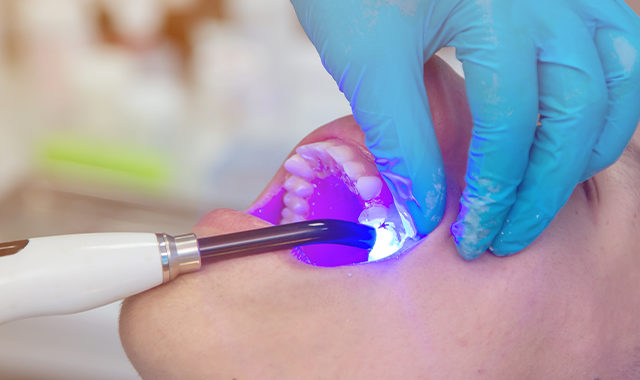
Class II restorations are a significant part of any clinician’s day. Dentists are looking for processes that make it easier for the patient, more efficient for themselves, and contribute to a better patient and doctor experience.
However, Class II composite restorations are also a vital contributor to a dentist’s bottom line. Therefore, many clinicians want to avoid complications that can contribute to restoration failures as well as productivity squelchers, otherwise known as the Class II blues.
“When you are doing something day after day, multiple times per day, you want to know how to make it quick and easy for everybody with predictable results every single time, “ Jason Goodchild, DMD, director of clinical affairs for Premier Dental Products Company, says. “That’s the holy grail; everybody’s happy, and both patient and doctor feel like it was a win-win.”
Everything in dentistry starts with a suitable treatment plan, Dr. Goodchild says. However, once the need for a Class II resin restoration is established, what adds up to an excellent Class II composite restoration is proper completion of all the procedural steps-preparation, isolation, adhesion, material placement, light curing and finishing and polishing.
Related reading: Total-etch or self-etch: which forms the best bond?
Also, each step is essential because they build upon each other. Per Dr. Goodchild, problems can occur if you fall short on any one of the steps in the Class II restoration process.
For example, if you don't prepare or fill the tooth correctly, if you leave caries behind or fail to place the bonding system right, you could possibly fail to create a marginal seal, have postoperative sensitivity, or worst case, the filling could de-bond or fall out. If you have voids in the composite, you might have postoperative sensitivity. If you don’t cure the material properly, the composite may not develop its full physical properties, which could mean micro-leakage.
“It's like this cascade effect,” Dr. Goodchild says. “If you do all these things correctly, then you have a chance for this to work, but if you mess up any of these procedures, well, it's hard to troubleshoot.”
We spoke to three clinicians to discover some of the ways to do all these small steps correctly when working with composite for Class II Restorations. Here’s what they had to say.

Read the directions
When it comes to Class II composite restorations, Dr. Goodchild says the most significant of the Class II blues is postoperative sensitivity. To avoid it and all the other complications with restorations, Dr. Goodchild says first and foremost, it is essential to read the directions on the materials. Although it sounds basic, reading the instructions is vital to the success of your restorations because not all bonding, composite, isolation or finishing and polishing systems are the same.
“They're not apples to apples. They all don't work the same way.” Dr. Goodchild explains. “The manufacturer’s directions are set up so you can learn how to use them, obviously, but also to get the best results. They’ve tested them, and they're going to report on how they should be used.”
Trending: The virtues of beautiful design
Set up bonding surface for success
Nathaniel Lawson DMD, PhD, assistant professor and director of the division of biomaterials for the UAB School of Dentistry likes to sandblast his preps with a PrepStart H2O, which is a particle abrasion performed with simultaneous water spray.
“I am not using this to increase my bond,” Dr. Lawson explains, “only to clean unwanted stains and artifacts from my preparation.”
Dr. Jennifer Sanders, a private practice general dentist in rural Frenchtown, Montana, cautions clinicians to isolate properly with a Class II, especially when replacing a subgingival amalgam filling. Unlike amalgam, you have to keep it 100 percent dry and keep the gingival crevicular fluid and blood out of the prep.
“If you don't keep it perfectly dry, you're not getting a good bond in there,” Dr. Sanders says.
Continue reading on page two...
Mind your matrix
Dr. Sanders says one of the main challenges is shaping the Class II properly down the side to avoid a catch or overhang so patients will not trap bacteria there, which could lead to periodontal complications. To avoid this problem, Dr. Sanders is careful about placing her matrix band. Also, she likes to use the sectional matrix systems because the bands, rings and wedges work together.
“Whichever brand you pick, be sure you know how to use the system you've chosen, and you're taking the time to put it in properly,” Dr. Sanders says. “ That makes a world of difference on getting a properly contoured side to the Class II.”
Dr. Lawson also uses sectional matrices and rings. “I have found 50-micron thick sectional matrices on the internet are easier to place when contact hasn't been completely broken,” he says.
Dr. Lawson then uses polishing discs to shape interproximal contacts. The polishing makes the embrasures smooth, reduces plaque traps, and makes it easier for my patients to floss.
Dr. Goodchild says the new matrixes made it easier to create improved interproximal contacts. However, he cautions clinicians to be sure they understand how to use the matrix correctly to create an appropriate interproximal contact. For some clinicians that don’t mind their matrix, or who use an older system that doesn’t simplify contact creation as the newer ones do, it can create another one of the Class II blues.
“If you haven’t developed the shape, you may not get a good fit with the tooth next to it, and then you get food trapped between the teeth every single time the patient eats,” Dr. Goodchild explains.
Related reading: How to polish composite restorations with Footsie
Don’t forget about resin-modified glass ionomers (RMGIs)
Another factor as you get deeper into the tooth, you run out of enamel and are at the cementum level. In these situations, Dr. Sanders uses what she calls an “open sandwich technique.”
“I place down a layer of RMGI material first at the bottom of the box, so I'm not fighting that little bit of moisture because it is slightly moisture tolerant. It will seal in better against that layer of cementum,” Dr. Sanders says.
Another problem the RMGI protects against is the expansion and contraction that can occur when curing composites, which can lead to shrinkage that creates micro gaps in your restoration. When you seal the box with RMGI, the gap would be between the layer of glass ionomer and composite, not between the composite and the tooth.
“I like to do it that way. A lot of people will do their layer of glass ionomer, then a layer of flowable, and then their packable. I usually go right for the packable, but that's a preference as well,” Dr. Sanders says.
Dr. Sanders uses a conditioner as a silanating agent before she puts down her RMGI. In her experience, it improves the bond with the RMGI and the tooth.
“The other thing I do is if the patient is worried about the filling being sensitive, I will put down some Gluma,” she says.
More by the author: Putting curing lights in the spotlight
Know your hodgepodge
Dr. Goodchild says most dentists use a Class II solution that is a “hodgepodge” of different restorative products. They use one manufacturer’s bonding system, and a different company’s isolation system and another’s light, and so on, because of brand loyalty or they think that product performs best in their hands.
However, he says if you do mix your restorative materials, you have to know how to use them correctly. Every bonding system, for example, is not the same; they have unique instructions. Therefore, if you have different manufacturer’s materials working together on your restoration, you should know what makes each one different.
“If you use a hodgepodge system, then know your hodgepodge,” Dr. Goodchild says. “It’s a back-to-basics approach. Know everything about those materials that makes them special and how to use them to their fullest potential.”
Dr. Goodchild says knowing these details contributes to efficiency. You should know when you can and cannot use the materials correctly. Also, he thinks you should be prepared to adapt when necessary-or when a new product comes out you want to try.
Continue reading on page three...
“You want to be able to adapt to some ‘new kids on the block,’ so to speak. You have to know how to integrate the latest and greatest and shiniest tool into the mix and how it works best with the other players,” Dr. Goodchild says.
For example, if you are trying a new bio-active composite, you need to know if they can work with the light. When you are testing a new bonding system, will it adhere with your composite? You need to know if the materials in your mix can work together and the nuances of them working well together.
Dr. Sanders also uses different products from different manufacturers. Her matrix and wedge system are one brand, her RMGI from another, her composite from another and her bonding agent from yet another brand.
“I don't think those make too much of a difference how they go together because they're all the same chemical,” she says. “It comes down to understanding the base properties of materials you're using so you know how they interact together. But generally, the ones we are using should be pretty good together.”
If you have questions about how the systems interact, Dr. Sanders said the product reps are a good source of information. However, she feels if the chemicals involved are the same, the interaction between products should also be the same.
Some manufacturers moved to a complete system for direct composite restorations. They know the materials will all work together because they were tested together.
“Their efficiency proposition is everything from us works well with every other player in the system. Some dentists like that story and some dentists like their hodgepodge,” Dr. Goodchild says.
Remember the particulars of your composite type
Another thing Dr. Sanders says you have to be conscious of is what type of composite you are using. Notably, she thinks you should be careful not to put composite in layers that are too thick for your version of the composite.
“Yes, there are some bulk fill composites that in theory can cure up to four millimeters. But with normal composites, you don't want more than two millimeters, which you need to layer in to avoid shrinkage and having gaps. All of that can lead to sensitivity afterward, which is a huge problem,” Dr. Sanders explains.
Trending: Top innovations announced at CDA Presents Anaheim 2019
Use a consistent approach to optimize your team effort
When it comes to productivity and efficiency for Class II restorations, Dr. Sanders says having an excellent assistant is critical, particularly when your assistant knows what your next step is in the process. Dr. Sanders says her assistant is familiar with her process, so the assistant has everything set up and ready to go.
“Most of the time, I don't even have to say anything. She just automatically knows what to do next, and she's got it ready to go. That makes it efficient,” Dr. Sanders says. “It is all about teamwork.”
Dr. Goodchild believes most dentists who use a mix of materials tend to be brand loyal. It translates into each dentist’s customized system, which is great for the assistant, too.
“When they do a Class II, it's always those materials in the same order and the same way, and there's efficiency there not only for the dentist but also for the team member that's helping that dentist because they know what's coming next,” Dr. Goodchild says.
Optimize every step for efficiency
Dr. Goodchild encourages dentists to build up their efficiencies in their process at each step, no matter how small.. Every step is critical and technique sensitive, so you need to do them all properly to get the best results.
Some dentists set aside 35 to 45 minutes for a Class II restoration, which includes getting the patient numb. The revenue for the practice could be $200 or even 40 percent less for an insurance-based practice. When you factor in the cost of materials, it is clear margins in dentistry are small.
“This is a tight rope dentists walk,” Dr. Goodchild says. “We have to build better efficiency in taking the many small steps needed to achieve good results and to do our jobs well.”