Bacteria Responsible for Periodontal Disease Might Also Cause Rheumatoid Arthritis
The study was carried out by investigators at Johns Hopkins University after other findings implied that mucosal surfaces are the sites where diseases like rheumatoid arthritis typically begin.
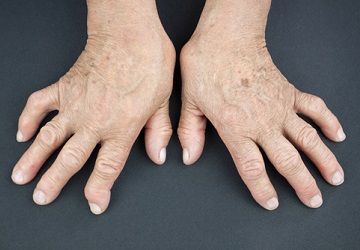
The evidence supporting the importance of good dental practices continues to grow as more research shows just how critical oral health is to the rest of the body. A new study published in Science Translational Medicine has shown that bacteria commonly connected with periodontal infections might also be responsible for more serious autoimmune diseases like rheumatoid arthritis (RA).
The study was carried out by investigators at Johns Hopkins University after other findings implied that mucosal surfaces are the sites where diseases like rheumatoid arthritis typically begin. Since many RA patients also have periodontal dysbiosis, or an imbalance in the bacterial flora in the mouth, the investigative team hypothesized that this imbalance might trigger the production of disease-specific autoantibodies and arthritis in those individuals that are already susceptible.
For the study, the team used mass spectrometry to identify the bacterial composition of gingival crevicular fluid in two groups of patients — one with preexisting periodontal disease and another, healthy control group. A certain type of autoantigen was present in the periodontitis samples that has also been identified as the primary immune target in cases of RA.
The link was further strengthened after the team found this autoantigen in rheumatic joints, leading to the conclusion that the gingiva is the site of initiation in RA pathogenesis. Additionally, the investigators were able to identify a certain bacterial species, Aggregatibacter actinomycetemcomitans (Aa), as a common pathogen in the periodontitis samples. This bacterium induces hypercitrullination in neutrophils, mimicking the pathways by which inflammation and damage occurs in RA joints.
Exposure to Aa was confirmed in RA patients included in the study. However, not all of the study participants with RA were exposed to Aa, indicating that there may be other bacteria located elsewhere in the body that could be responsible for inducing this type of inflammation.
As of 2005, the Centers for Disease Control and Prevention estimated that there were 1.5 million individuals living with RA in the United States. Typical treatments include antirheumatic drugs, steroids, and treatments such as physical therapy. However, evidence such as this could lead to the development of new, more effective treatments targeting the bacterial factors causing diseases like RA.