5 ways to ensure effective dental instrument processing
Strict attention to detail encompasses the entirety of a dental professional's work – from training, to product handling and treatment. Attention to detail is important in any job – if a chef doesn’t pay attention to the recipe, a meal can taste awful; if a lawyer puts a comma in the wrong place, a contract becomes unenforceable; if a mechanic doesn’t tighten all the bolts, a wheel can fall off a car.
Attention to detail is important in any job – if a chef doesn’t pay attention to the recipe, a meal can taste awful; if a lawyer puts a comma in the wrong place, a contract becomes unenforceable; if a mechanic doesn’t tighten all the bolts, a wheel can fall off a car. So, too, is its importance in the dental practice, especially as infection prevention is concerned.
Instrument processing requires such attention to ensure that patients – and team members – are properly protected.
Read more: The dangers of microbial resistance in the dental practice
Click through the slides to learn five ways to ensure effective instrument processing.


Training
Proper instrument processing begins with the appropriate training. Unfortunately, not everyone gets that guidance. And while the end result can be catastrophic for patients, the attitudes of some professionals are disappointing.
“In 2013, an infection control breach at an oral surgeon’s office made national headlines,” says Karen Daw of Karen Daw Consulting and former clinic health and safety director for The Ohio State University College of Dentistry. “According to the compliant, assistants performed procedures only a dentist should, and sterilization processes were subpar. In fact, the executive director for the board of dentistry stated, ‘I will tell you that when ... we left, we were just physically kind of sick. I mean, that’s how bad [it was], and I’ve seen a lot of bad stuff over the years.’ When the dentist was asked about this area in his practice he replied, ‘My staff takes care of that, I don’t.’”
More from the author: The 3 common infections dental professionals should be worried about
Proper training on infection control issues should be of critical importance.
“Like the adage for realtors, ‘Location! Location! Location!’ a great way to ensure effective instrument processing is through ‘Training! Training! Training!’” Daw says. “It’s not really fair to expect this area is going to do well if we haven’t set up the team member for success. This starts with the doctor setting the expectation, leading by example and assessing for competencies after training. And yet, many dentists themselves have received little to no professional instruction or guidance. In fact, ask the average dentist when was the last time they cleaned an instrument and they’ll respond with: 'They haven’t,' or 'Do it once in a blue moon.' This is why I applaud schools like University of the Pacific and The Ohio State University for including an instrument processing rotation as part of the dental student curriculum.”
There’s a lot at stake when it comes to infection prevention, including patient and staff health, but also the dentist’s reputation.
“Training the dentist and the team members makes sense,” Daw says. “After all, it’s the dentist that is responsible … and it’s the dentist’s name that ends up on the front page when there’s been a breach.”



Check your work
Sterilizers are somewhat analogous to household dishwashers: one simply loads dishes/instruments into the machine and then starts the cycle. In the case of the sterilizer, the process is supposed to get everything germ-free. But, like our dishwasher comparison, one can’t put in items that are too messy for the machine to handle.
“Does staff really look at the instruments, to see if they got them clean?” consultant and speaker Leslie Canham, CDA, RDA, asks. “That’s where sometimes we fall short. You’re in such a hurry to get those instruments dried and packaged, or wrapped and put into the sterilizer, that not examining the instruments is a misstep that allows missing debris to stay on the instruments.
“When I visit a dental practice and I do a mock OSHA or infection control inspection, I’ll go to their sterile instruments, and I’ll open up some of the bags or cassettes, and I’ll look for instruments that have debris on them. I always find something. It’s a crucial part of the process, if instruments aren’t cleaned first, they might not get sterilized.”
Related reading: 5 do's and don'ts of sterilization in the dental practice
For the sterilizer to do its job, it can be hindered if debris gets in the way.
“I like to tell the teams that I consult with that instruments that have debris are not going to get sterile,because the debris creates a coating or a covering over oral microorganisms that can allow them to survive the heat, the chemical vapor, or the steam of the sterilizer. There’s evidence that shows that there can still be microorganisms present in debris, even though they’ve been processed through a sterilizer,” she says.
Care especially needs to be taken with small, precision instruments.
“This is the case with dental burs and endodontic files in that they have such small nooks and crannies that you can’t really clean them effectively,” Canham says. “And when there’s debris present, the oral microorganisms can survive that sterilization cycle. To me, the cleaning is a critical part of patient safety.”


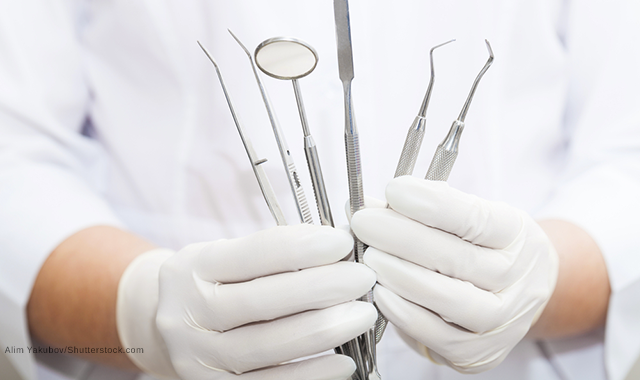
Handling
How and where instruments are handled matters. If the steri-center is not suitable for the task, instruments won’t be properly processed, and staff can put themselves at risk.
“Have we planned this space for safety and peak performance?” Daw asks. “Few people take into consideration just how important this area is. Yet, I’ll watch instruments being processed at a rapid pace in a room no larger than a broom closet. In addition, there’s no clear direction for the flow of instruments leading to potential safety concerns and decreased efficiency. It just might be time to reassess central sterilization and treat it with the consideration and respect it deserves. Fortunately, there are plenty of resources to assist with this.”
How instruments are sterilized is critical. If the manufacturer’s instructions are not followed, it is unlikely that instruments will be properly processed.
More from the author: 10 major infection control risks
“Frequently, when I visit dental practices, I see that they have overloaded their sterilizer, Canham says. “They have placed so many instrument pouches or cassettes or combinations thereof together in the sterilizer, that the sterilant cannot do its job of circulating around all the instruments, actually penetrating the wraps... Some states don’t require wrapping of instruments; however CDC recommends that instruments be packaged or wrapped prior to sterilization. If you overload, not everything is going to achieve the benefit of the sterilant, which is usually steam.
“What I sometimes see is, because they’ve overloaded the sterilizer, the wetness hasn’t dried off of the instrument bags or cassettes,” Canham says. “The wet material can wick bacteria from the environment to the inside of the sterile pouch or cassette, and it can compromise the integrity of the wrap or pouch. You could pick up the package and all the instruments fall out because it’s so wet.”
Further, how the instruments are stored is another critical factor.
“The instruments need to be distributed and stored in a manner that they’re not going to become contaminated again,” Canham says. “Something else I find when I do my inspections is when I look at instrument pouches that are displayed for use for the next patient, or the next day’s patients, sometimes I’ll find a package where the chemical indicator has not changed color. It tells me that package did not go through the sterilizer. You should having a system of making sure that you double check all of the instruments that come out of that sterilizer. Every time you set up for a patient, you should double check to make sure that color change has occurred on the packaging. If everybody’s done their job correctly, whether it’s one person or multiple people that handle the sterilization in dental practice, then that color change should have occurred and instruments should be clean and sterile.”



Be careful
It's not just patients who need to be protected from unsafe instrument handling practices. Carelessly handling instruments can pose a risk to dental team members. Transporting contaminated instruments from treatment room to sterilization should be done safely. Never carry sharp, contaminated instruments by hand.
An easy way to avoid trouble, she recommends, is by using a treatment tray with a locking lid.
“It’s very common practice to see people, carrying an open treatment tray,” Canham says. “My preference is to see them transporting instruments in a container that has a closed or locking lid. There are treatment trays that have this feature or you could buy a shoe container at Walmart with clips that hold the lid on, so that if you drop it all the instruments don’t fall out. I like to see people wearing utility gloves when they transport and reprocess contaminated instruments.”
Read more: How to create a culture of safety at your practice
Most practices have automated cleaning systems, like ultrasonic or instrument washers.
“Automated systems reduce accidents. Let the automated system do its job. And if there’s still debris on the instruments, hand scrubbing is warranted,” Canham advises.



Verification
Dental team members don’t need to just rely on their senses and quick wits to ferret out problems. There are tools in place to help ensure proper instrument maintenance.
For instance, practices should spore test their sterilizers at least weekly – or more often.
“It’s the only indicator that your sterilizer is doing its job and making instruments safe for patients,” Canham says.
Chemical indicators are easy and obvious ways to ensure that instruments have been sterilized. But, it is still up to the team members to check those indicators – surprisingly, not everybody does.
Trending article: Digital impressions: Ready for their close-up?
“It’s important to look for because we assume that it’s been done. Routinely, we grab the sterile instruments and prepare for the patient, but do we always look to see if the color change has occurred?” Canham asks. “If you interviewed 50 dental assistants they probably would say, ‘I just assumed, it came out of the sterilizer. I’m grabbing it from the sterile drawer or the cupboard or from the tray. I’m not actually looking at that. The only time I really look at that is if I can’t determine whether somebody has run the cycle or not run the cycle, then I’ll look to see if the color change occurred.’
“Every now and then, something escapes that quality control,” she continues. “So that’s why I say, when you’re getting ready to bring your instruments to a patient or you’re setting up your treatment tray, do you really double-check? Remember, only spore testing guarantees sterilization, but this is one quick way to know, immediately, if there’s a problem either with your machine or if there’s a problem in the process of getting a sterile package from your sterilization area.”
Not having paid proper attention to detail can result in a ruined a meal, an unenforceable contract or a roadside disaster. In the dental practice, it can mean harm to patients or staff members. In short, attention to detail should matter to everyone.
“When it comes to sterilization, this is the heart of patient protection," Canham says.
