10 questions to test your understanding of infection control requirements
Take our pop quiz to find out where you stand when it comes to infection control efforts in the dental industry.
The most dreaded words any student can hear are “pop quiz.” While those words can strike fear and anxiety into students’ hearts, there’s a good reason for their use. It’s a quick assessment to evaluate students’ knowledge level.

Read more: Should you be concerned about measles?
The same tool can be used by professionals to find out what they know and where they might need a little help. Over their careers, dental healthcare personnel (DHCP) are exposed to a lot of information about infection prevention. And while all of it is important, there may be facts that have been mistaken, misunderstood or forgotten.
Click through the slides to see the questions.

Question 1: True or false: Gloves protect your hands 100 percent of the time.
A: False.
“People think gloves protect their hands 100 percent of the time, but that’s actually not true,” says consultant and speaker Leslie Canham, CDA, RDA. “Gloves have micro perforations and pinholes that are actually allowed. The Food and Drug Administration (FDA) oversees exam gloves because they are medical devices. The FDA allows a 2.5 percent defect rate in gloves. That means the gloves don’t have the integrity that people think they have. Sometimes, when you put your gloves on, you pull, and those micro perforations and pinholes get a little larger than they were in the box. It reinforces the need for handwashing after you remove your gloves every single time.”



Question 2: Can sterilized items that are wrapped or in peel pouches be removed from the sterilizer when damp?
A: No.
“All sterile items that are to be removed, after the cycle is complete, should be completely dry,” says Joyce Moore, RDH, an infection control consultant and clinical instructor at Bristol Community College in Fall River, Mass. “If items are touched when damp, bacteria can be wicked and enter the packages, thus rendering them contaminated.”



Question 3: Which side of an autoclave bag faces up? The plastic or the paper side?
A: It depends.
“It is whatever the manufacturer’s directions say to do,” Canham says. “Of course, there are many different sterilizers in many different dental offices, so you can’t just say, automatically, ‘Well, you put it paper-side up.’ It really depends on the manufacturer of the unit. Probably, the real answer is, ‘Where does the steam get withdrawn from the unit?’ Is it out of the bottom or out of the top? The manufacturer can very easily describe how their sterilizer operates. The answer is that it depends on the manufacturer’s directions. If the manufacturer hasn’t given clear, written directions in their operating manual, it’s worth a phone call to the manufacturer to find out.”
“Don't let this answer be based on a someone else's advice,” Moore adds. “Many times, I've seen clinicians get this dead wrong. The best advice I can give is to refer to the manufacturer's instructions for use for the sterilizer. Some specify paper-side up and others state plastic-side up. There might even be a better option that is listed in that manual, like the use of a pouch rack, that will allow you to stand pouches on edge to facilitate better drying.”


Question 4: Do DHCP need hepatitis B booster shots?
A: No.
“The Centers for Disease Control and Prevention (CDC) says that boosters are no longer required,” Canham says. “Once you achieve immunity, you have immunity for life or 37 years (the hepatitis B vaccine was first available in 1982). You can’t go 38 years because that hep B vaccine wasn’t born yet.
“We had thought that our immunity disappeared because our antibody levels were low,” she continues. “So, in the past, we thought that we were losing our immunity. The fact of the matter was we never really lost immunity because the actual terminology is ‘Cellular immunity persists even though antibody levels are low.’ People still think they need those boosters for hepatitis B, and, really, if you go to the CDC website, you can get the information about hepatitis B vaccination for providers.”
Don’t let the advice on the website supersede that of a health care professional.
“Of course, a person should follow their healthcare professional’s recommendations,” Canham notes. “If someone’s been told by their physician that they need boosters for hepatitis B, they may have other health issues. Right now, it’s the CDC’s recommendations, generally, that boosters are not needed. But, there are going to be exceptions. Of course, your healthcare provider is the one that guides you on making that decision.”


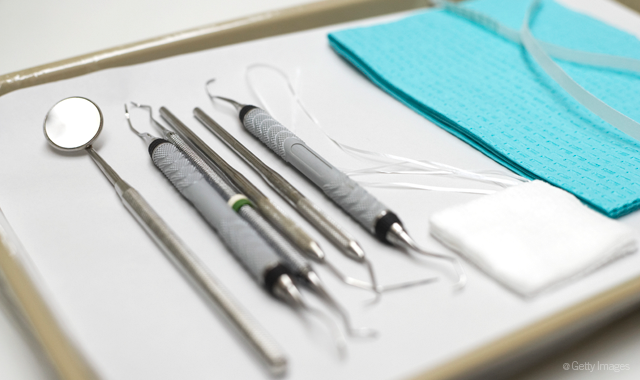
Question 5: What’s the most important step in instrument processing: cleaning, disinfection or sterilization?
A: Cleaning,
Proper instrument processing involves a number of steps, but instruments can’t be disinfected or sterilized unless they’ve been properly cleaned first.
“If any debris, body fluids or blood are left behind, complete cleaning will not be achieved,” Moore says. “The best cleaning methods involve the use of instrument washers and ultrasonic cleaners. Manual hand scrubbing is generally less effective and puts the worker at risk.”


Question 6: Do we unknowingly touch things causing cross-contamination?
A: It depends.
“That’s a question only you could ask yourself because only you would know what the answer is,” Canham says. “When you’re done working with a patient or if you need to go get an item that is out of your location, reach in a drawer and touch something, the gloves should come off and not be having a chance to cross-contaminate with whatever’s on the glove and another surface. If you’re wearing gloves and you touched something besides the clinical contact surface, are you causing cross-contamination unknowingly?”



Question 7: Can extracted teeth be disposed of in the regular trash?
A: No.
“Extracted teeth are considered potentially infectious and, unless local or state laws permit it, they should be returned to the patient upon request or disposed of in a medical waste container,” Moore says. “Extracted teeth containing amalgam should not be sterilized for educational purposes or put in medical waste that will be incinerated.”


Question 8: Can employees take contaminated personal protective attire home for laundering?
A: No.
“If employees take contaminated personal protective attire home, it’s an OSHA violation,” Canham says. “Employers are required to maintain and launder PPE.”



Question 9: Should surfaces contaminated with visible blood be cleaned and disinfected with a hospital disinfectant?
A: Yes.
There are different types and levels of disinfectants that can be used within the dental practice. Standard disinfectants, such as those found in household cleaning products, are able to kill common bacteria, but their use would be limited to nonclinical areas.
Hospital disinfectants are EPA-registered for use in hospitals, clinics, dental offices and other medical facilities, and they should be used in all clinical areas.
“Any clinical contact surface that is contaminated with visible blood should be cleaned and disinfected with an intermediate-level disinfectant that carries a tuberculocidal claim,” Moore says.



Question 10: True or false: Nonclinical areas don’t need any special consideration.
A: False.
“It seemed to come to the surface around 10 years ago, when swine flu was a big scare in the United States,” Canham says. “Do you have a box of tissues and a wastebasket in your reception room, and perhaps an alcohol hand sanitizer? It’s something so that visitors to your reception room have something to sanitize their hands with if they’re coughing or sneezing, and then they have a place to dispose of that tissue that they sneezed into. I do find a lot of dental offices are sensitive to that and provide tissues, hand sanitizer and a waste receptacle in their reception room. People are embarrassed to ask for a tissue, or it’s too late by the time they’ve sneezed into their hand. Infection control extends to the reception area, and it’s the little creature comforts that show your commitment to infection prevention.”
